|
Case Report
Effort thrombosis: Paget–Schroetter syndrome in a 19-year-old female
1 Senior Associate Consultant, Hospital Internal Medicine Department, Mayo Clinic Health System, Eau Claire, Wisconsin, USA
2 Division of Immunology, Rheumatology Department, University of Iowa Hospitals and Clinics, Iowa, USA
Address correspondence to:
Omobolanle Adetimehin
Adetimehin, MD, Hospital Internal Medicine Department, Mayo Clinic Health System, 1221 Whipple St, Eau Claire, WI 54703,
USA
Message to Corresponding Author
Article ID: 101514Z01OA2025
Access full text article on other devices

Access PDF of article on other devices

How to cite this article
Adetimehin O, Oke I. Effort thrombosis: Paget– Schroetter syndrome in a 19-year-old female. Int J Case Rep Images 2025;16(2):10–13.ABSTRACT
Paget–Schroetter syndrome (PSS) is a form of effort thrombosis seen in young athletes and individuals with occupations involving repetitive upper limb movement. Arm swelling, distended veins, skin discoloration, and pain are characteristics of it. Diagnosis can be made with non-invasive investigations, such as Doppler ultrasound; however, a computed tomography venogram, magnetic resonance venogram, or traditional venogram may be required. Treatment involves anticoagulation, thrombolysis, and surgical decompression with removal of the first rib, and this is usually met with good outcomes. We present a young female diagnosed with PSS and requiring a staged multidisciplinary approach to treatment.
Keywords: Effort thrombosis, Paget–Schroetter syndrome, Venous thrombosis
Introduction
Paget–Schroetter syndrome (PSS) was named after James Paget and Von Schroetter, who first described and identified its etiology in the 1800s. Paget–Schroetter syndrome, also known as effort thrombosis, is a form of spontaneous thrombosis involving the axillary and subclavian veins, usually following a repetitive force on the vessel as it passes through the narrow space between the clavicle and the first rib in the anterior part of the thoracic outlet [1]. It has an incidence of 1–2 individuals/100,000/year and occurs more commonly in individuals in their 20s–30s. It is also more typical in males, with a male: female ratio 2:1 [2]. It is a venous variant of thoracic outlet syndrome [3],[4]. Other causes of upper extremity deep venous thrombosis include thrombophilia, the use of central venous catheters, trauma, and malignancy.
Case Report
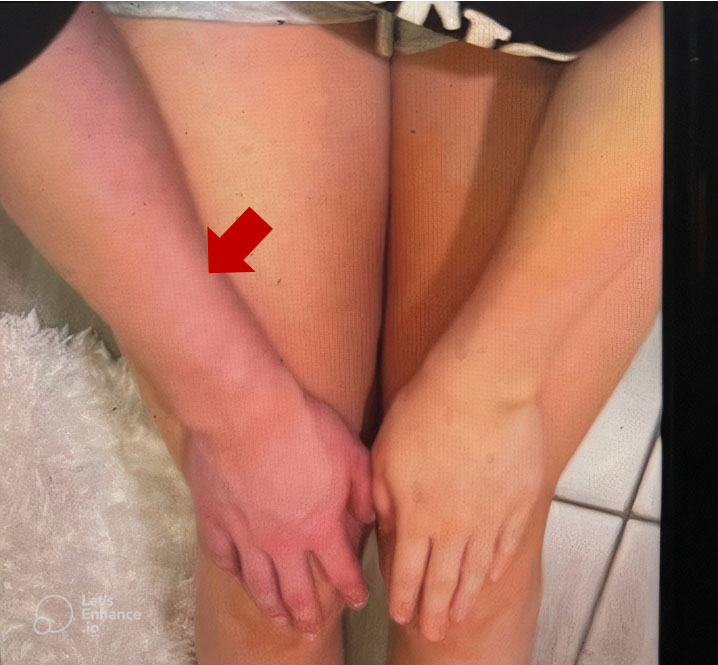
A 19-year-old right-handed female with a history of migraine presented to the Emergency Room with the acute onset of pain, swelling, and bluish discoloration of her right arm (Figure 1). Swelling and discoloration were present throughout the day. There was associated numbness and prominent distended veins in her right arm. There was no antecedent trauma and no personal or family history of venous thromboembolism. The patient works as an aesthetician and engages in repetitive activities such as waxing; she was also a cheerleader for ten years.
Her vital signs were heart rate (HR) 97 bpm, blood pressure (BP) 130/70 mmHg, respiratory rate 18 cpm, and temperature 36.1 °C. She had a positive Urschel’s sign (differential swelling with prominently distended veins and red discoloration of the skin) over the right upper extremity, but peripheral pulses were intact. Adson test, supraclavicular compression test, Wright test, and costoclavicular maneuvers were negative. Her labs were unremarkable.
Right upper extremity duplex ultrasound in the Emergency Room did not reveal deep vein thrombosis. Despite negative special tests for thoracic outlet syndrome (TOS), the patient’s symptoms were suspected to be due to TOS. She was seen by Vascular Surgery four weeks after the onset of her symptoms, and her repeat duplex ultrasound showed thrombosis in the right subclavian vein. A right upper extremity venogram showed thrombosis of the brachial vein in the upper arm near the confluence with the basilic vein, with multiple venous collaterals in the right arm at the shoulder level. There was also an appearance of chronic thrombosis of the right subclavian vein beneath the clavicle with collaterals, but the superior vena cava was patent. A thrombus was seen in the axillary vein at the level of the proximal humerus and in the subclavian vein beneath the clavicle on intravascular ultrasound (IVUS). She was admitted and underwent catheter-directed thrombolysis with tissue plasminogen activator (tPA), with improvement in the upper extremity collaterals but no significant improvement in her subclavian vein stenosis.
A repeat right upper extremity venogram showed a patent previously thrombosed basilic and axillary vein. The right subclavian vein’s patency was restored following suction thrombectomy and balloon angioplasty. The patient had a right first rib excision in that same admission and was discharged home on a three-month course of anticoagulation with rivaroxaban.
Discussion
Our patient presented with acute right upper extremity swelling, discoloration, and distended veins that were suspicious for thoracic outlet syndrome, but her examination findings were inconsistent with TOS. She had been a cheerleader for almost 10 years, and her current job as an aesthetician entailed several hours of waxing daily, an activity that involves repetitive hyperabduction of the shoulder.
Pathophysiology
A causal relationship has been reported between sporting activities leading to hyperabduction, retroversion, and PSS. These movements cause repetitive trauma to the venous intima as it passes through the tight thoracic outlet, leading to activation of the coagulation system and consequent thrombosis [4]. An abnormal congenital lateral insertion of the costoclavicular ligament on the first rib may cause venous occlusion and thrombosis in PSS [3],[5]. Some studies suggest a significant number of patients with PSS have underlying thrombophilia [6],[7],[8],[9], although it is not clear if this is a causal or casual relationship. Cassada et al. found an increased risk of postoperative complications in patients with concurrent PSS and thrombophilia [10]. These claims were later disputed.
Paget–Schroetter syndrome has a predilection for healthy young men, but it can also occur in females. The common denominator in both genders is “effort,” or activities that cause trauma to the subclavian vein.
Clinical features
Presenting symptoms include but are not limited to swelling and heaviness, red or bluish discoloration of the arm, and dilated, visible veins across the shoulder and upper arm (Urschel’s sign). The trigger may not be immediately apparent, but some patients will report an onset following a specific sporting activity. Clinical signs and symptoms are suggestive, but alone, they have poor specificity in diagnosing PSS [5].
Diagnosis
Doppler ultrasonography is the first-line diagnostic investigation, with a sensitivity of 56% to 100% and specificity of 77% to 100% in diagnosing upper extremity deep venous thrombosis [11]. The variability in sensitivity and specificity is hypothesized to be due to differences in patient selection, the ultrasonographic technique used, and the anatomical location of the subclavian vein under the clavicle. It is not surprising that our patient had a falsely negative study on her first Doppler ultrasound, which could be attributed to an early non-occlusive thrombus. Contrast venography is the gold standard for diagnosing Paget–Schroetter syndrome. Computed tomographic venography (CTV) and magnetic resonance venography (MRV) are being increasingly used, especially in patients with high clinical suspicion, because they are less invasive and have similar sensitivity to conventional venography [5]. Since the role of thrombophilia in PSS remains uncertain, selected patients should be screened for coagulation abnormalities, as this may influence the need for long-term anticoagulation [5]. Our patient underwent thrombophilia screening prior to the commencement of anticoagulation. Testing for proteins C and S, factor V Leiden, prothrombin gene mutation, and antiphospholipid antibodies returned negative.
Treatment
There are varying opinions on the ideal treatment. An aggressive treatment strategy that involves thoracic outlet decompression, thrombolysis, thrombectomy, percutaneous and surgical venoplasty, venous bypass, and stent placement has an almost 100% success rate. Catheter-directed thrombolysis was employed in this patient, offering a therapeutic effect similar to systemic thrombolysis without systemic side effects. This was followed by thoracic outlet decompression (TOD) surgery and oral anticoagulation. The higher incidence of post-thrombotic syndrome and recurrent upper extremity deep vein thrombosis (UEDVT) in patients who have delayed TOD surgery favors the current practice of routine and early surgery [12],[13],[14]. There is no consensus on the duration of anticoagulation in patients with PSS without underlying predisposing factors, such as thrombophilia, central venous catheters, or lines. Some authors suggest anticoagulation for 3–6 months; others recommend no anticoagulation in patients with good surgical outcomes [3],[14]. Anticoagulation without thrombolysis or first rib resection increases the risk of recurrent symptoms and residual deficits [15].
In a comprehensive study conducted by Spencer et al., 32 competitive athletes with effort thrombosis achieved a favorable outcome with a staged multidisciplinary approach [12]. The first stage is early diagnostic venography and thrombolysis. This is followed by thoracic outlet decompression and, lastly, temporary postoperative anticoagulation.
Like most cases of upper extremity deep venous thrombosis, PSS may be complicated by pulmonary embolism and post-thrombotic syndrome, the latter being more common in PSS [16]. Our patient did well after staged procedures; Physical Therapy cleared her for return to work. At her follow-up visit, she demonstrated significant improvement in swelling and skin discoloration.
Conclusion
Paget–Schroetter syndrome is relatively uncommon; it may be associated with a debilitating disability if misdiagnosed. Early diagnosis, prompt thrombus removal or dissolution, and resection of the 1st rib are crucial to achieving a good outcome following diagnosis. Despite a negative Doppler ultrasound, physicians should identify and proceed to venography, CTV, or MRV in patients with high clinical suspicion of the syndrome. A staged, structured treatment protocol ensures optimal outcomes while minimizing long-term complications in patients.
REFERENCES
1.
Illig KA, Doyle AJ. A comprehensive review of Paget-Schroetter syndrome. J Vasc Surg 2010;51(6):1538– 47. [CrossRef]
[Pubmed]

2.
Saleem T, Baril DT. Paget-Schroetter syndrome. In: StatPearls. Treasure Island (FL): StatPearls Publishing; 2025.
[Pubmed]

3.
Urschel HC Jr, Patel AN. Surgery remains the most effective treatment for Paget-Schroetter syndrome: 50 years’ experience. Ann Thorac Surg 2008;86(1):254–60. [CrossRef]
[Pubmed]

4.
Kommareddy A, Zaroukian MH, Hassouna HI. Upper extremity deep venous thrombosis. Semin Thromb Hemost 2002;28(1):89–99. [CrossRef]
[Pubmed]

5.
Alla VM, Natarajan N, Kaushik M, Warrier R, Nair CK. Paget-Schroetter syndrome: Review of pathogenesis and treatment of effort thrombosis. West J Emerg Med 2010;11(4):358–62.
[Pubmed]

6.
Zell L, Kindermann W, Marschall F, Scheffler P, Gross J, Buchter A. Paget-Schroetter syndrome in sports activities—Case study and literature review. Angiology 2001;52(5):337–42. [CrossRef]
[Pubmed]

7.
Hendler MF, Meschengieser SS, Blanco AN, Alberto MF, Salviú MJ, Gennari L, et al. Primary upper-extremity deep vein thrombosis: High prevalence of thrombophilic defects. Am J Hematol 2004;76(4):330–7. [CrossRef]
[Pubmed]

8.
Martinelli I, Battaglioli T, Bucciarelli P, Passamonti SM, Mannucci PM. Risk factors and recurrence rate of primary deep vein thrombosis of the upper extremities. Circulation 2004;110(5):566–70. [CrossRef]
[Pubmed]

9.
Vayá A, Mira Y, Mateo J, Falco C, Villa P, Estelles A, et al. Prothrombin G20210A mutation and oral contraceptive use increase upper-extremity deep vein thrombotic risk. Thromb Haemost 2003;89(3):452–7.
[Pubmed]

10.
Cassada DC, Lipscomb AL, Stevens SL, Freeman MB, Grandas OH, Goldman MH. The importance of thrombophilia in the treatment of Paget-Schroetter syndrome. Ann Vasc Surg 2006;20(5):596–601. [CrossRef]
[Pubmed]

11.
Mustafa BO, Rathbun SW, Whitsett TL, Raskob GE. Sensitivity and specificity of ultrasonography in the diagnosis of upper extremity deep vein thrombosis: A systematic review. Arch Intern Med 2002;162(4):401–4. [CrossRef]
[Pubmed]

12.
Melby SJ, Vedantham S, Narra VR, Paletta GA Jr, Khoo-Summers L, Driskill M, et al. Comprehensive surgical management of the competitive athlete with effort thrombosis of the subclavian vein (Paget-Schroetter syndrome). J Vasc Surg 2008;47(4):809–820; discussion 821. [CrossRef]
[Pubmed]

13.
Doyle A, Wolford HY, Davies MG, Adams JT, Singh MJ, Saad WE. Management of effort thrombosis of the subclavian vein: Today’s treatment. Ann Vasc Surg 2007;21(6):723–9. [CrossRef]
[Pubmed]

14.
Molina JE, Hunter DW, Dietz CA. Protocols for Paget-Schroetter syndrome and late treatment of chronic subclavian vein obstruction. Ann Thorac Surg 2009;87(2):416–22. [CrossRef]
[Pubmed]

15.
Urschel HC Jr, Razzuk MA. Paget-Schroetter syndrome: What is the best management? Ann Thorac Surg 2000;69(6):1663–8; discussion 1668–9. [CrossRef]
[Pubmed]

16.
Elman EE, Kahn SR. The post-thrombotic syndrome after upper extremity deep venous thrombosis in adults: A systematic review. Thromb Res 2006;117(6):609–14. [CrossRef]
[Pubmed]

SUPPORTING INFORMATION
Author Contributions
Omobolanle Adetimehin - Conception of the work, Design of the work, Acquisition of data, Analysis of data, Drafting the work, Revising the work critically for important intellectual content, Final approval of the version to be published, Agree to be accountable for all aspects of the work in ensuring that questions related to the accuracy or integrity of any part of the work are appropriately investigated and resolved.
Ibiyemi Oke - Conception of the work, Design of the work, Acquisition of data, Drafting the work, Final approval of the version to be published, Agree to be accountable for all aspects of the work in ensuring that questions related to the accuracy or integrity of any part of the work are appropriately investigated and resolved.
Guarantor of SubmissionThe corresponding author is the guarantor of submission.
Source of SupportNone
Consent StatementWritten informed consent was obtained from the patient for publication of this article.
Data AvailabilityAll relevant data are within the paper and its Supporting Information files.
Conflict of InterestAuthors declare no conflict of interest.
Copyright© 2025 Omobolanle Adetimehin et al. This article is distributed under the terms of Creative Commons Attribution License which permits unrestricted use, distribution and reproduction in any medium provided the original author(s) and original publisher are properly credited. Please see the copyright policy on the journal website for more information.