|
Case Series
| ||||||
| Abdominal menstruation: A dilemma for the gynecologist | ||||||
| Seema Singhal1, Sunesh Kumar1, Yamini Kansal2, Deepika Gupta3, Mohit Joshi1 | ||||||
|
1Assistant Professor, Department of Obstetrics and Gynaecology, All India Institute of Medical Sciences New Delhi, India
2Professor, Department of Obstetrics and Gynaecology, All India Institute of Medical Sciences New Delhi, India 3Senior resident, Department of Obstetrics and Gynaecology, All India Institute of Medical Sciences New Delhi, India 4Assistant Professor, Department of Surgery, All India Institute of Medical Sciences New Delhi, India | ||||||
| ||||||
|
[HTML Abstract]
[PDF Full Text]
[Print This Article] [Similar article in Pumed] [Similar article in Google Scholar] 
|
| How to cite this article |
| Singhal S, Kumar S, Kansal Y, Joshi M, Gupta D. Abdominal menstruation: A dilemma for the gynecologist. Int J Case Rep Images 2017;8():370–375. |
|
ABSTRACT
| ||||||
|
Introduction:
Menstrual fistulae are rare. They have been reported after pelvic inflammatory disease, pelvic radiation therapy, trauma, pelvic surgery, endometriosis, tuberculosis, gossypiboma, Crohn’s disease, sepsis, migration of intrauterine contraceptive device and other pelvic pathologies. We report two rare cases of menstrual fistula. Keywords: Abdominal menstruation, Excision of fistulous tract, Menstrual fistula, Salpingocutaneous fistula, Uterocutaneous fistula | ||||||
|
INTRODUCTION
| ||||||
|
Gynecologists are familiar with vesicovaginal, ureterovaginal or rectovaginal fistula. Menstrual fistula is defined as communication between the reproductive organs and skin, is a rare condition and only few case reports are published [1]. They are characterized by periodic discharge of blood from laparotomy scar site that coincides with normal menstruation [1]. Various types of such fistula viz tubocutaneous, tuboenterocutaneous, uterocutaneous, cervicocutaneous and salpingo-ureteric fistula are described. This is a highly morbid condition as it usually affects young women and is a source of anxiety to patient as well as clinician because of persistence of symptoms despite treatment. It is essential to be aware of this entity because clinical suspicion is the key for successful management. Herein, we report two rare cases of menstrual fistula and discuss the management options of this condition. | ||||||
|
CASE SERIES
| ||||||
|
CASE 1 | ||||||
|
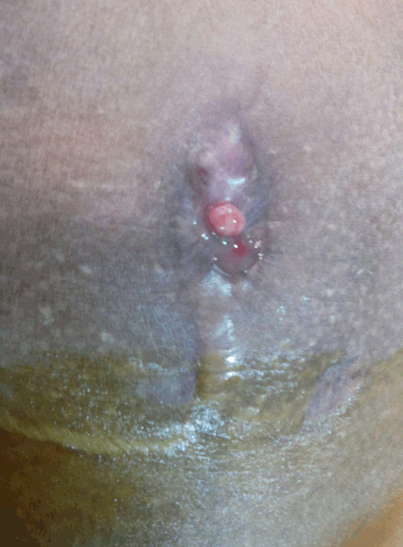
A 27-year-old nulliparous female with history of primary infertility presented with complaint of cyclical bleeding from the abdomen since three years. She had hypomenorrhea and cyclical abdominal pain since menarche. History of laparotomy five years back elsewhere because of mass in abdomen. However, intraoperatively no intervention could be done due to adhesions. After one year she underwent laparoscopy outside but again nothing was done except adhesiolysis. Few months after the second surgery, patient started having blood tinged purulent discharge from anterior abdominal wall scar site. Discharge coincided with menstruation. She had to use 1-2 pads per day at the abdominal site. On examination her built was average, breasts were Tanner stage IV, axillary hair were present and spine was normal. A midline vertical scar was present on her abdomen. Discharge was seen from a small pinkish area on the scar site along with mild induration (Figure 1). A tender cystic mass of 18 weeks size uterus, with restricted mobility was felt towards right.
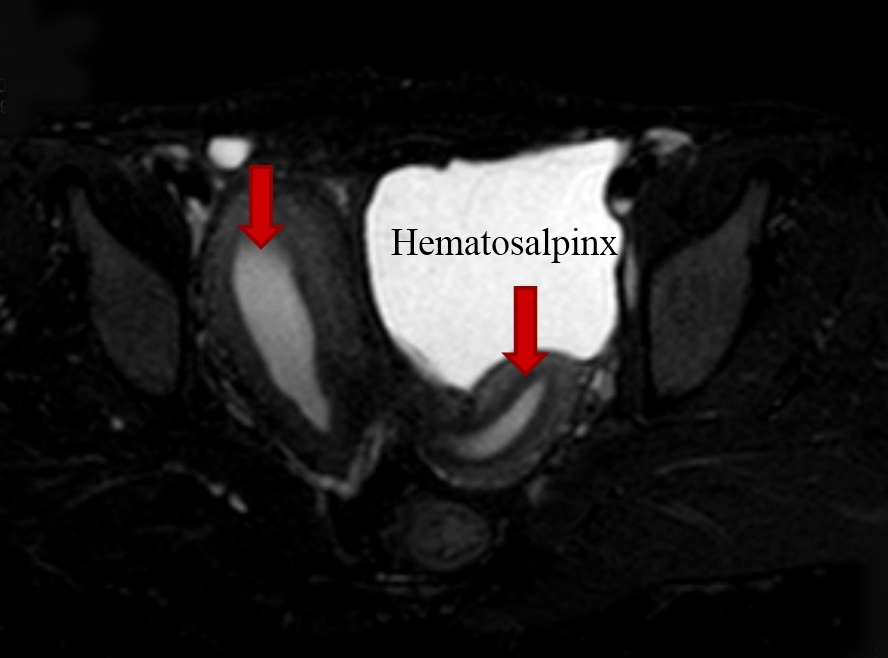
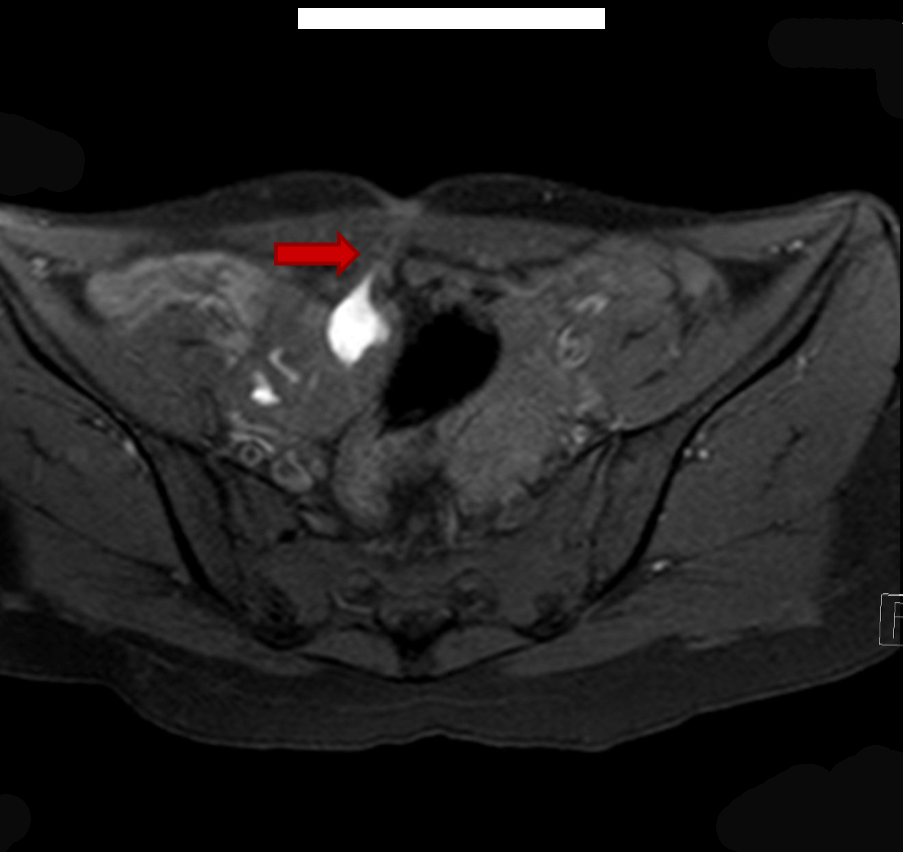
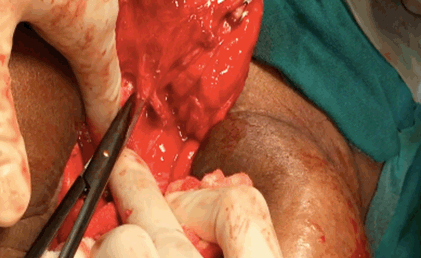
On local examination pubic hair were present, Tanner stage V. On speculum examination cervix was normal but deviated to left. On bimanual examination same mass was felt from right fornix and small size uterus from left fornix. Ultrasonography revealed bicornuate uterus with collection within endometrial cavity of right horn likely non-communicating. Bulky right ovary with a tract noted from it to the scar site on anterior abdominal wall likely scar endometriosis with solitary left kidney. Magnetic resonance imaging scan revealed two uterine cavities with a single cervix and vagina and a left communicating horn and a right non-communicating uterine horn with hematometra and right hematosalpinx (Figure 2). Blood filled tract was extending from the hematosalpinx to the skin opening on the anterior abdominal wall (Figure 3). Patient and her family were counseled and prognosticated about poor fertility potential. She was given the option of excision of the horn. Patient wished to retain her menstrual and child bearing function. She was taken up for laparotomy. Intra operatively fistulous tract was delineated with a probe (Figure 4) and a hypoplastic communicating uterine horn was identified. A right non-communicating normal sized uterus was present. Hysterotomy along with drainage of collection, excision of right hematosalpinx and creation of neovagina was done. A small left uterine horn communicating with the cervix was identified. A new opening was created in the vagina followed by stent insertion and previously non-communicating horn was connected with the vagina. Histopathology showed ulcerated fistulous tract with inflammatory granulation tissue with chronic salpingitis and foci of endometriosis. Patient received oral hormonal pills for three months. Later, there was resumption of normal menstruation with good flow postoperatively along with relief of pain. | ||||||
| CASE 2 | ||||||
|
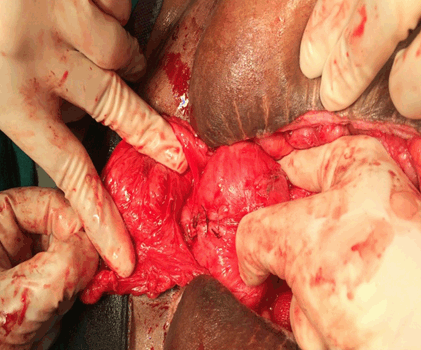
A 25-year-old P1L1 presented with complaint of bleeding from scar site during periods since six months. She had an LSCS one year back at some hospital, followed by burst abdomen. She was then referred to us and underwent a laparotomy. Intraoperatively an injury was detected in ileum and a loop ileostomy was done. Patient recovered well but subsequently she started having monthly bleeding from LSCS scar site for which she was using 1–2 pads per day. On per abdomen examination midline puckered scar with a small central defect was seen. On speculum examination cervix was not visualized and vaginal examination revealed six weeks size uterus with restricted mobility. Ultrasound showed bulky uterus with multiple fibroids, largest measuring 35 mm, bilateral ovaries were normal with ill-defined tissue (1 cm) at scar site anterior to uterine fundus. Contrast enhanced magnetic resonance imaging (MRI) showed divarication of recti with mid line defect. There was defect in the lower uterine segment communicating with anterior abdominal wall with endometrial fluid extending up to the anterior abdominal wall (Figure 5). There were two foci of T2 hyperintensity at superior and inferior margins of the mid line abdominal wall scar respectively. Retroverted distorted uterus with multiple uterine fibroids with adherent small bowel loop in right adnexal region. Patient was taken up for laparotomy. Intraoperatively bladder was adherent to previous cesarean scar on uterus, sinus tract extending from previous cesarean scar site to peritoneum, to rectus sheath and to subcutaneous tissue (Figure 6). Adhesiolysis (Figure 7) with excision of istulous tract (Figure 8) was done. A probe was inserted to confirm communication with uterine cavity (Figure 9) and closure of uterine defect was done (Figure 10) along with ileostomy closure. Postoperative period was uneventful. Both patients are under follow-up and are keeping well with no recurrence of symptoms. | ||||||
| ||||||
|
| ||||||
| ||||||
| ||||||
| ||||||
| ||||||
| ||||||
| ||||||
| ||||||
| ||||||
|
DISCUSSION
| ||||||
|
Menstrual fistula have been reported after pelvic surgery especially after incomplete removal of inflammatory tissue, pelvic inflammatory disease, trauma, endometriosis, tuberculosis, gossypiboma, pelvic radiation therapy, Crohn’s disease and other pelvic pathologies [2]. Most tubal fistulas arise as a result of inflammation of the fallopian tube, bowel or as a complication of gynecological surgery (cesarean section, salpingectomy or myomectomy) [2]. In most cases infection is an additional complicating factor. Salpingocutaneous fistula has been described in case of pelvic abscess as a result of induced septic abortion [3] . Yadav et al. described the utero-cutaneous fistula as a complication of laparotomy performed due to paraovarian cyst and intraperitoneal adhesions [4]. Alina et al. described a case of salpingocutaneous fistula in a case of peripartum hysterectomy where the fistula was formed during removal of the surgical drains when the fallopian tube moved under the skin [5]. Tubocutaneous fistula is a rare presentation of uterine malformations. In our first case patient had a vertical fusion defect (class U4aC0V0) with hematometra, hematosalpinx in non-communicating horn with abdominal menstruation and resultant adhesions [6] . With subsequent surgeries there was formation of fistulous tract between fallopian tube and skin. The diagnosis of menstrual fistula is based on high index of clinical suspicion. One should suspect this entity in a postoperative case if there is persistent discharge from scar site despite treatment, and later with regularization of periods cyclical discharge from the scar site corresponding to menstrual bleeding [1][2][3] [4][5]. Vellanki et al. reported a case where patient presented with groin sinus, recurrent painful swelling over edge of scar site after LSCS and was managed on lines of suture granuloma, scar endometrioma, underwent local drainage and excision but there was no relief in symptoms [7]. The diagnosis was made only after she was taken up for laparotomy. To confirm the diagnosis various bed side tests are available, methylene blue dye test after inserting Foley catheter into uterus has been used to confirm the diagnosis [8]. With wide spread availability of contrast MRI scan and hysteroscopy complete delineation of fistulous tract and demonstration of its opening in uterus is used to confirm the diagnosis [9]. However, other modalities such as fistulography, hysterosalpingography, CT scan have been used for confirming the diagnosis and delineating the fistulous tract [7] [8][9]. Due to rarity of this condition there is no recommended treatment modality. Medical, surgical or combined medical and surgical treatment have been tried [9][10][11][12][13]. Treatment depends on the age of the patient and the desire to retain fertility. There are case reports of successful medical management of uterocutaneous fistula with six months therapy of GnRH agonists [11][12]. The mechanisms of action of GnRH agonists in the management of fistula are not clear. However, cessation of menstruation, endometrial atrophy, and decreasing uterine size may cause cicatrization and contracture of the fistulous tract, leading to fibrosis and closure [11] [12]. Patients should be reviewed after six months for failure of medical management because of limitations of prolonged treatment with GnRH [9]. Surgery remains the mainstay of treatment. The actual demonstration of the fistulous tract and identification of its underlying cause is quite tedious and difficult. However, the type of resection should be individualized according to the needs of the patient [14]. For salpingocutaneous fistula one may advocate fistula resection and salpingectomy as the only feasible method of treating this rare disease to prevent the occurrence of ectopic pregnancy subsequently [13]. For uterocutaneous fistula, excision of fistulous tract with or without hysterectomy has been attempted. Maintaining the postoperative uterine drainage is essential to prevent recurrence. | ||||||
|
CONCLUSION
| ||||||
|
Adopting good surgical techniques and prevention of postoperative infection can prevent this highly morbid condition. High index of clinical suspicion and prompt excision of the tract along with maintenance of good drainage of uterus post operatively is the key to successful management. | ||||||
|
REFERENCES
| ||||||
| ||||||
|
[HTML Abstract]
[PDF Full Text]
|
|
Author Contributions
Seema Singhal – Substantial contributions to conception and design, Analysis and interpretation of data, Drafting the article, Revising it critically for important intellectual content, Final approval of the version to be published Sunesh Kumar – Analysis and interpretation of data, Critical revision of the article, Final approval of the version to be published Yamini Kansal – Substantial contributions to conception and design, Acquisition of data, Drafting the article, Final approval of the version to be published Deepika Gupta – Substantial contributions to conception and design, Acquisition of data, Drafting the article, Final approval of the version to be published Mohit Joshi – Analysis and interpretation of data, Critical revision of the article, Final approval of the version to be published |
|
Guarantor
The corresponding author is the guarantor of submission. |
|
Source of support
None |
|
Conflict of interest
Authors declare no conflict of interest. |
|
Copyright
© 2017 Seema Singhal et al. This article is distributed under the terms of Creative Commons Attribution License which permits unrestricted use, distribution and reproduction in any medium provided the original author(s) and original publisher are properly credited. Please see the copyright policy on the journal website for more information. |
|
|