|

|
 |
|
Case Series
| ||||||
| Guidewire technique: Removal of a doorknob in tourniquet syndrome | ||||||
| Phee-Kheng Cheah1, Xiang-Yun Yang2, Azlan Kamalludin3, Thian-Lian Soo4 | ||||||
|
1Emergency and Trauma Department, Sabah Women and Children´s Hospital, Kota Kinabalu, Sabah, Malaysia 2Emergency and Trauma Department, Sarawak General Hospital, Kuching, Sarawak, Malaysia 3Emergency and Trauma Department, Langkawi Hospital, Pulau Langkawi, Kedah, Malaysia 4Paediatric Department, Sabah Women and Children´s Hospital, Kota Kinabalu, Sabah, Malaysia | ||||||
| ||||||
|
[HTML Abstract]
[PDF Full Text]
[Print This Article]
[Similar article in Pumed] [Similar article in Google Scholar] 
|
| How to cite this article |
| Cheah PK, Yang XY, Kamalludin A, Soo TL. Guidewire technique: Removal of a doorknob in tourniquet syndrome. Int J Case Rep Images 2017;8(4):233–238. |
|
Abstract
| ||||||
|
Introduction: Tourniquet syndrome caused by a constricting band is common, and can be removed either by intact removal or by division. Finding a doorknob as the constrictor is rare and challenging to manage due to its bulky size, larger area of contact with the skin surface, and difficult access to the constricting site. The optimal removal technique has not yet been established. Keywords: Constricting band, Doorknob, Guidewire technique, Tourniquet syndrome | ||||||
|
Introduction
| ||||||
|
Constricting bands around body appendages is not an uncommon presentation to the emergency department. The constriction can produce a clinical condition known as the tourniquet syndrome, which causes neurovascular compromise to the tissues distally, leading to ischemia and necrosis. This will result in long-term loss of function and sensitivity, or worse, amputation of the affected appendage [1]. Hence, timely removal of the constricting band is of the utmost importance to prevent this complication. Generally, the methods available can be divided into intact removal, or removal by division [1] [2]. The former can further be classified into five distinct groups: the winding technique, compression technique, the caterpillar technique, twin-thread technique, and glove technique [3] [4][5][6] [7] [8]. Intact removal techniques work by first reducing the edema distal to the constricting band via different techniques of compression, then followed by distal advancement of the band over the affected area to remove it. On the other hand, removal by division uses cutting devices and will depend on the material and size of the constricting band [2]. Methods to remove a ring from the finger have been extensively described in literature [1][2][3] [4][5][6] [7] [8]. However, no literature is available with regards to methods of removing a doorknob from the finger. Indeed, finding a doorknob as a constricting band around the finger is quite rare. The point of insertion of the finger is into the doorknob hole and through the shank (Figure 1). Metal doorknobs are mostly made out of brass, which is an alloy composed of varying percentages of copper and zinc [9]. Brass is popularly used because of its strength, resistance to rust and formability, hence such durability poses a challenge in its removal. In this case series, we present two patients who came to emergency department with doorknobs as the constricting band around their fingers. | ||||||
|
Case Series
| ||||||
| Case 1 | ||||||
|
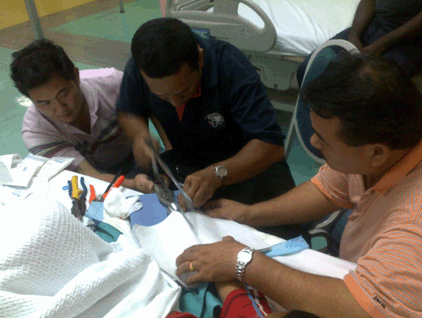
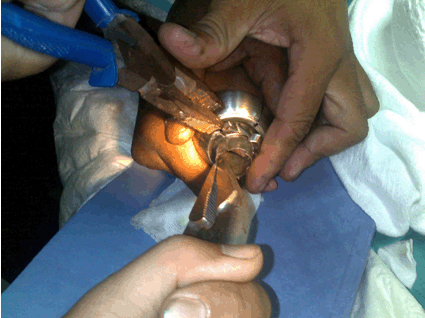
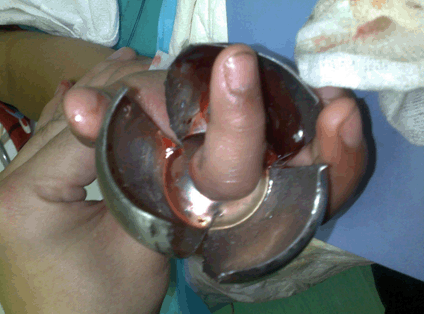
An eight-year-old boy presented with his right index finger stuck to a doorknob. The child was playing with an unused doorknob still attached to a door in a house undergoing renovation. Attempts to remove the doorknob by the family members at home had failed. The finger was swollen with the doorknob tightly stuck above the proximal interphalangeal joint. Capillary refill was less than two seconds. There was no cyanosis, pallor or necrotic tissue noted. The child could still move the finger and denied any altered sensation distally. A home improvement personnel was called in for assistance as we were not familiar with the structure of the doorknob. The patient was administered with a digital block over the right index finger, and removal was attempted using lubricant. It was unsuccessful. We decided to proceed with removal by division as the child was able to cooperate. No sedation was required. The doorknob structure had to be dismantled into components and had to be sawn into multiple segments, as the hard metal of the doorknob prevented bending of the structure to release the finger. The smooth and rounded surface of the doorknob also proved to be a challenge, particularly to balance the metal saw on it. A few assistants were needed to hold the doorknob steady during the sawing process (Figure 2). Three cuts were made on the knob, and the segments were bent to overlap each other to enable the release of the finger (Figure 3). The patient tolerated the procedure well and only sustained minimal swelling and a few superficial lacerations around the area due to the prior manipulation attempts to free the finger (Figure 4). There was no reduction in the range of movement. The patient was discharged with normal saline dressing and oral analgesia. | ||||||
| Case 2 | ||||||
|
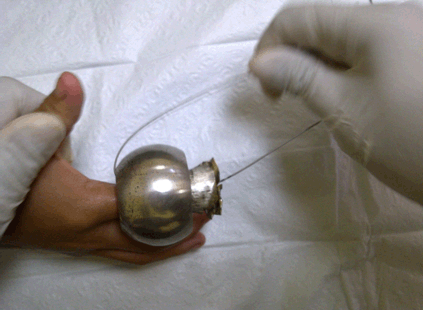
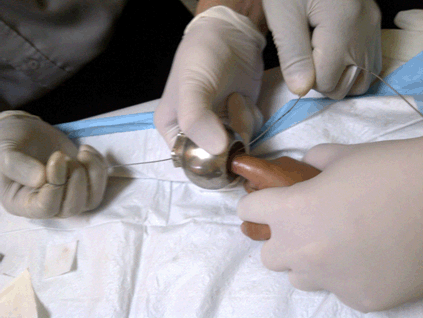
A 10-year-old boy was brought into emergency department with his right index finger stuck to a doorknob (Figure 1). The child was playing with a defective door at home. Multiple attempts by the family members to free the finger from the doorknob were unsuccessful. In the emergency department, the child complained of severe pain over the affected finger. He was apprehensive of any inspection or manipulation of the finger. The entire length of his finger was covered by the doorknob with minimal swelling noted distally. Capillary refill time was less than two seconds. The division method would be risky in this case as the child was unwilling to cooperate. It was also noted that the doorknob actually has sharp edges near the contact area, which can cause a string, suture or rubber band to snap or tear off during manipulation using the intact removal method. A string with higher tensile strength is more feasible to achieve removal, and therefore, a metal guidewire from a triple lumen central venous catheter was chosen as it is easily available in the emergency department (Figure 5). Wrist block was administered in this case. The child was also sedated with oral chloral hydrate prior to the procedure.from one end to the other in order to form a “hooking” mechanism through the doorknob (Figure 6). Both ends of the guidewire were held in one hand and constant gentle traction was maintained in order to pull the doorknob away from the affected finger, while the other hand stabilizes the spherical doorknob. The child´s hand was kept in position by an assistant (Figure 7). No lubricant was required. The doorknob was then successfully removed within three minutes. Evaluation post procedure revealed a mildly edematous finger with a circumferential abrasion wound at the site of entry. There was no reduction in finger movement, and no fracture was detected clinically. Simple wound dressing was done and the patient was discharged with oral analgesia. A follow-up via phone call a week later reported full functional recovery of his finger. | ||||||
| ||||||
| ||||||
| ||||||
| ||||||
| ||||||
| ||||||
| ||||||
|
Discussion
| ||||||
|
In this case series, both intact removal technique and removal by division were used in removing the constricting doorknob. Both techniques resulted in successful removal, with minimal soft tissue injury sustained from the previous removal attempts (Figure 8). The method employed in Case 1, which was removal by division using a metal saw, has several limitations which has to be addressed. Using a saw would require extra time in the preparation process, such as ensuring the availability of trained personnel in using it, and also the personal protective gears for the staff and the patient. This leads to a potential risk in causing a delay in the removal of the constrictor, which can lead to irreversible complications to the finger. The doorknob´s bulky and rounded physical structure overlies not only the narrowed area of the doorknob hole, but also a large portion of the finger. The wide, smoother and global surface of the doorknob is hard to stabilize especially if the cutting technique is employed. As a result, it is highly likely that the sawing equipment might slip off the cutting surface and cause injury to the patient and also the operator. This poses an extra hazard to the patient and personnel involved. Significant heat could also be generated while the patient´s skin is in contact with the constricting band, causing thermal injuries. Peay et al. found that significant heat was generated by just 5–10 seconds of grinding [10]. In our case, the doorknob is a relatively large sized constricting band as compared to a ring which is the usual mentioned in literature. A longer time would be required to cut the doorknob sufficiently for a finger release. The patient will also have to be cooperative and actively giving feedback regarding the sensation of the affected site, whether it is burning hot or if there is any worsening of the constriction felt. Therefore, this method might not be suitable in patients who are fretful and unable to obey commands, especially children who are already traumatized by the event. In Case 2, we used a guidewire from a triple lumen central venous catheter to maintain the force of pulling on the doorknob from the finger, which is a modified version of the string technique. Whilst maintaining a constant force of traction, the doorknob itself compresses the immediate point of contact, hence enabling it to progress further distally. In comparison to a string or a rubber band, a guidewire has higher tensile strength and does not snap easily, especially for a large constrictor such as in this case. The guidewire also provides a smooth surface that prevents excessive skin abrasion during manipulation of the constrictor, hence reducing the chances of iatrogenic injury. No lubrication or very minimal lubrication was required in this case, as the constant force maintained over the guidewire enabled the doorknob to surmount the main obstruction, which is the PIP joint. Such guidewires are also readily available in the emergency department where central vascular catheterization sets are available, as compared to looking for a suitable saw to cut the constricting band open. However, if the finger were to be more edematous, using multiple techniques simultaneously (compression),lubricate and traction) would often increase the chances of success. Wrist block was administered in this case. The child was apprehensive of any approach by the healthcare staff thus stabilization of the wrist joint would be easier and safer as compared to stabilizing the finger. The bulky size of the doorknob which has covered up most of the finger also leaves minimal surface area for digital block access. Digital block could increase the swelling over the affected site, worsening the tourniquet effect. In this patient, the wrist block is probably a better option of local analgesia as compared to digital block. Although both techniques successfully removed the doorknob, our guidewire technique using a metal guidewire is simpler and time-saving, with a lower-risk of manipulation-related injury. The guidewire used is a readily available in the most emergency departments, and the technique is easily mastered by novice operators, without the risk of injuring medical personnel themselves. With the absence of loud noises and the threatening appearance of cutting machines, this guidewire technique can be safely applied to most patients, especially the pediatric group. However, in both our cases, the patients only presented with mild edema distal to the constrictor with no open wound or fracture and no signs of ischemia. This technique may only be applicable to such patients. Kalkan et al. proposed an algorithm in removing a stuck ring in the emergency department [2]. This algorithm can serve as a guide in deciding whether the patient is suitable to undergo cutting or non-cutting technique. However, there is still no review or algorithm proposed for cases of a bulky constrictor, such as a doorknob. | ||||||
|
| ||||||
|
Conclusion
| ||||||
|
It is challenging using either the cutting or non-cutting technique when faced with a doorknob as a constricting band. We believe our guidewire technique will be useful in the removal of large constricting bands, as it is not only readily available in the emergency department, but also poses less hazard to the patient and health staff. This technique can be used as a first attempt before other more complicated methods are undertaken. | ||||||
|
Acknowledgements
| ||||||
|
We would like to thank the Director General of Health, Malaysia for the permission to publish this paper (NMRR-16-2188-33561). We would also like to thank Dr. Darlene F Ongkili for reviewing our paper. | ||||||
|
References
| ||||||
| ||||||
|
[HTML Abstract]
[PDF Full Text]
|
|
Author Contributions
Phee-Kheng Cheah – Substantial contributions to conception and design, Acquisition of data, Analysis and interpretation of data, Drafting the article, Revising it critically for important intellectual content, Final approval of the version to be published. Xiang-Yun Yang – Analysis and interpretation of data, Revising it critically for important intellectual content, Final approval of the version to be published. Azlan Kamalludin – Analysis and interpretation of data, Revising it critically for important intellectual content, Final approval of the version to be published. Thian-Lian Soo – Analysis and interpretation of data, Revising it critically for important intellectual content, Final approval of the version to be published. |
|
Guarantor
The corresponding author is the guarantor of submission. |
|
Source of support
None |
|
Conflict of interest
Authors declare no conflict of interest. |
|
Copyright
© 2017 Phee-Kheng Cheah et al. This article is distributed under the terms of Creative Commons Attribution License which permits unrestricted use, distribution and reproduction in any medium provided the original author(s) and original publisher are properly credited. Please see the copyright policy on the journal website for more information. |
|
|