|
 |
|
Case Report
| ||||||
| Papillary carcinoma arising in thyroglossal duct cyst: A rare case presentation | ||||||
| Roopa Arora1, Fatima Al-Hashimi2 | ||||||
|
1MBBS, M.D Path, Senior Consultant, Pathology, Salmaniya Medical Complex, Manama, Manama, Kingdom of Bahrain
2MD, FRC Path, Specialist, Pathology, Salmaniya Medical complex, Manama, Manama, Kingdom of Bahrain | ||||||
| ||||||
|
[HTML Abstract]
[PDF Full Text]
[Print This Article] [Similar article in Pumed] [Similar article in Google Scholar] 
|
| How to cite this article |
| Arora R, Al-Hashimi F. Papillary carcinoma arising in thyroglossal duct cyst: A rare case presentation. Int J Case Rep Images 2017;8(11):721–724. |
|
ABSTRACT
| ||||||
|
Introduction: Thyroglossal duct cyst (TGDC) is a common congenital anomaly but carcinoma arising in thyroglossal duct cyst is rare, occurring in 1% of cases. Keywords: Diagnostic procedures, Management, Papillary carcinoma, Thyroglossal duct cyst | ||||||
|
INTRODUCTION
| ||||||
|
Thyroid gland develops as an endodermal diverticulum in floor of pharynx, at the level of foramen cecum and descends down as thyroglossal duct in front of neck, anterior to hyoid bone and laryngeal cartilages, between third and eighth weeks of gestation. Its distal end is enlarged to form thyroid gland. It obliterates completely by ninth week of gestation. Up to 60% cases of thyroglossal duct cyst (TGDC) show islands of functioning thyroid follicles in its wall [1]. However, parafollicular cells are absent. Incomplete involution of thyroglossal duct causes formation of thyroglossal cyst. Thyroglossal duct cysts are frequently seen in clinically practice in pediatric age group and 7% in adults. They present as slowly growing palpable anterior neck masses which move with swallowing [2]. Occurrence of thyroid carcinomas arising in a TGDC is rare [3]. Brentano in 1911 and Uchermann in 1915 were the first to describe a neoplasm in a remnant of thyroglossal duct [4]. Most common malignancy in TGDC is papillary carcinoma followed by others. However, medullary carcinoma is not seen owing to absence of parafollicular cells. Sistrunk operation is the treatment of choice but other treatment modalities like partial/total thyroidectomy are considered depending on status of thyroid gland (any cold nodules), cervical lymph node enlargement and neck irradiation [5]. | ||||||
|
CASE REPORT
| ||||||
|
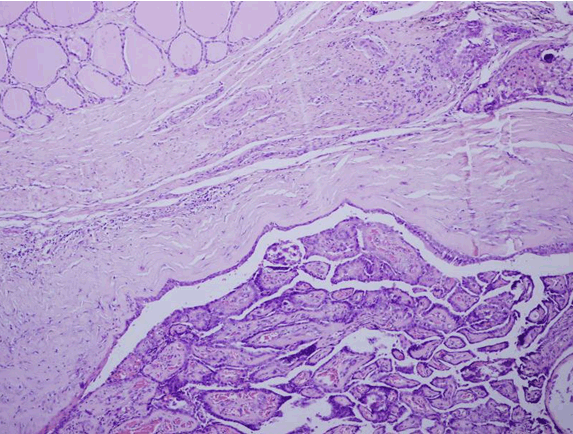
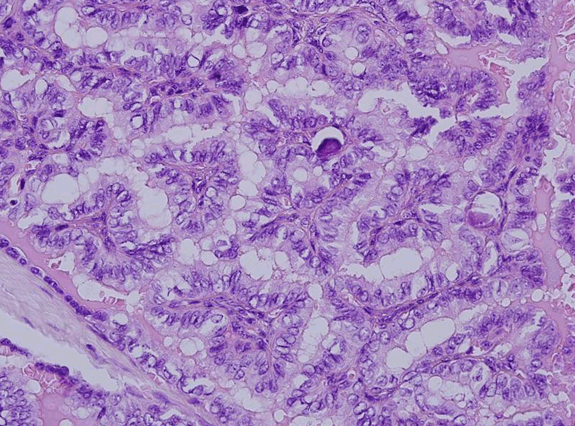
A 22-year-old female was referred to our hospital with a midline neck swelling for one year. There was no history of pain while swallowing. She did not give any history of shortness of breath, fever, weight loss or discharge from the lump. There was no change in bowel habits. Clinically, the thyroid was not enlarged and no cervical lymph node enlargement was palpable. Thyroid function tests were within normal range and other baseline blood investigations were also normal. Ultrasound of neck revealed a well-defined multi- loculated midline cystic lesion measuring 4.5x2 cm, with thin wall which was embedded in muscle and located in infrahyoid region with extension to both paramedian areas. The thyroid gland appeared normal. Also, there was no cervical lymphadenopathy. Based on clinical and ultrasound findings, a diagnosis of thyroglossal duct cyst was made. Fine needle aspiration cytology (FNAC) of the cyst revealed it to be a benign cystic lesion composed of lymphocytes, macrophages, few neutrophils and groups of bland follicular cells (Figure 1). A Sistrunk procedure was performed for removal of cyst and the surgical specimen was sent for histopathology. Grossly, the collapsed cystic mass measured 3.5x2.2x2 cm. A separate piece of hyoid bone was also received. Microscopic examination revealed a cyst lined by respiratory and squamous epithelium. Its lumen revealed a papillary carcinoma, composed of complex, branching randomly oriented papillae with fibrovascular cores and many psammoma bodies. The wall of cyst revealed islands of normal colloid-filled thyroid tissue as well as foci of papillary carcinoma (Figure 2) and (Figure 3). The papillae were lined by cuboidal cells with optically clear and overlapping nuclei, some showing intra-nuclear inclusions and nuclear grooves (Figure 4). The tumor measured 1.1 cm. Connective tissue surrounding the cyst showed many lymphoid aggregates and fibrosis. The tumor was very close to one resection margin. The hyoid bone did not show any tumor. Based on histopathological report, a post-surgery thyroid scan was performed which showed a normal sized thyroid gland with homogeneous radiotracer uptake. No cold or hot nodules were seen. Since the tumor invaded the wall of cyst and was close to one resection margin, a need for total thyroidectomy was discussed with the patient but the patient refused further surgical intervention. | ||||||
| ||||||
|
| ||||||
| ||||||
| ||||||
|
DISCUSSION
| ||||||
|
Thyroglossal duct cyst (TGDC) is a developmental abnormality of the thyroid gland. Due to embryological remnants of thyroid tissue located in the TGDC, the same malignant tumors that develop in the thyroid gland can also develop in the TGDC [6]. Most common are papillary carcinoma (75–80%), but other thyroid tumors such as follicular, Hürthle cell, and mixed papillary–follicular carcinomas also have been reported [7]. Anaplastic and squamous cell carcinoma can also occur but are very rare [8][9]. Thyroglossal duct carcinoma may be clinically indistinguishable from benign TGDC. It is an incidental finding on histopathology as was seen in our case. In such cases, diagnosis is usually made after histopathologic examination of a specimen obtained after a Sistrunk resection [6]. Ultrasound, computed tomography (CT), magnetic resonance imaging (MRI), and fine-needle aspiration biopsy (FNAB) can be useful techniques to differentiate TGDC carcinomas from simple TGDC before a surgical operation [5]. Fine needle aspiration cytology and intra-operative frozen section may help in a preoperative diagnosis of malignancy in TGDC. However, incidence of diagnosis of malignancy on histopathology after a benign diagnosis on FNAC is very rare [10][11]. Inadequate yield of aspirated material due to cystic degeneration in the tumor could have led to this error. However, in presence of adequate cellular material, presence of tridimensional fragments, anisonucleosis, nuclear grooves, pseudoinclusions and psammoma bodies are identified as the best indicators for a diagnostic resection of thyroid carcinoma. Strict criteria by Widstom et al. are followed for diagnosis of de novo TGDC carcinoma as opposed to metastasis from an occult primary in thyroid [12]. They are: histological identification of TGDC lined by columnar/squamous epithelium and normal thyroid tissue in its wall along with absence of carcinoma in thyroid gland [12][13]. The same were adhered to in this case. A cystic lymph node metastasis is also differentiated from TGDC carcinoma based on histological demonstration of epithelial lining in the latter. Similarly, cystic variant of papillary thyroid carcinoma would not have an epithelial lining of the cyst wall as opposed to TGDC carcinoma. As regards management of such a case, an algorithm has been proposed for treatment of papillary carcinoma in TGDC which involves a simple Sistrunk procedure in patients less than 45 years of age with tumors less than 1.0 cm that are confined to the cyst and which show an ultrasonographically normal thyroid gland and no suspicious lymph nodes [5][14]. There is a need of a total thyroidectomy followed by I131 ablation and thyroid-stimulating hormone suppression is considered [14]. If a tumor is more than 1 cm in size, multifocal or invades cyst wall. A similar treatment plan was recommended to the patient in the present case since the tumor extended outside cyst wall and was close to one resection margin but the patient refused another surgery. | ||||||
|
CONCLUSION
| ||||||
|
The diagnosis of thyroglossal duct cyst carcinoma can be missed due to its rarity. For rapidly growing midline neck masses, relevant investigations involving imaging of the neck and fine needle aspiration cytology are required before surgical operation for an accurate diagnosis. The Sistrunk operation alone is sufficient for small tumors confined to the cyst, but total thyroidectomy with neck dissection is recommended for larger tumors which have invaded the wall of cyst, associated thyroid nodules and enlarged cervical lymph nodes. | ||||||
|
REFERENCES
| ||||||
| ||||||
|
SUGGESTED READING
| ||||||
| ||||||
|
[HTML Abstract]
[PDF Full Text]
|
|
Author Contributions
Roopa Arora – Substantial contributions to conception and design, Acquisition of data, Analysis and interpretation of data, Drafting the article, Revising it critically for important intellectual content, Final approval of the version to be published Fatima Al-Hashimi – Analysis and interpretation of data, Revising it critically for important intellectual content, Final approval of the version to be published |
|
Guarantor
The corresponding author is the guarantor of submission. |
|
Source of support
None |
|
Conflict of interest
Authors declare no conflict of interest. |
|
Copyright
© 2017 Roopa Arora et al. This article is distributed under the terms of Creative Commons Attribution License which permits unrestricted use, distribution and reproduction in any medium provided the original author(s) and original publisher are properly credited. Please see the copyright policy on the journal website for more information. |
|
|