|
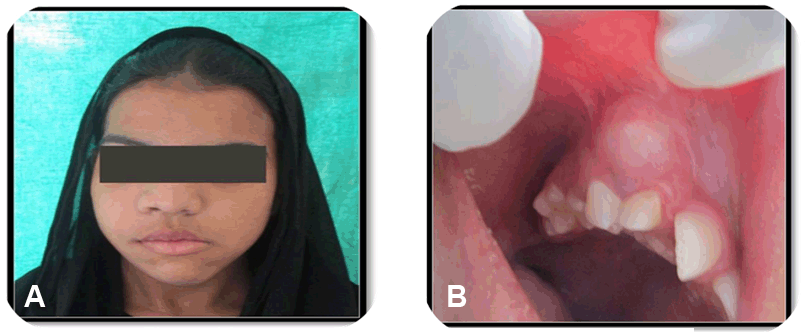
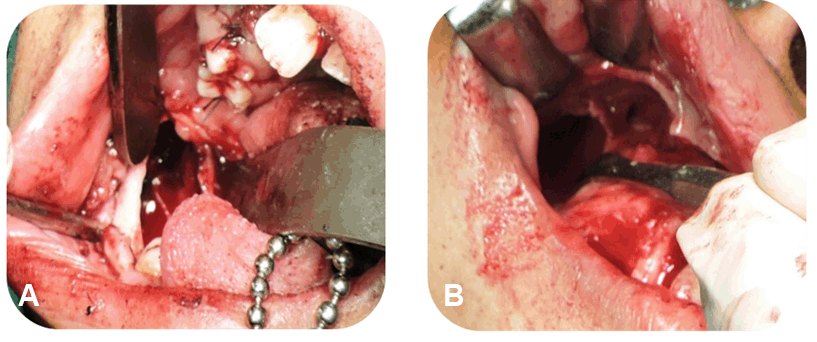
A 14-year-old female patient reported with a chief complaint of swelling in the right side of face (Figure 1A) since four months with a history of slowly progressing swelling.
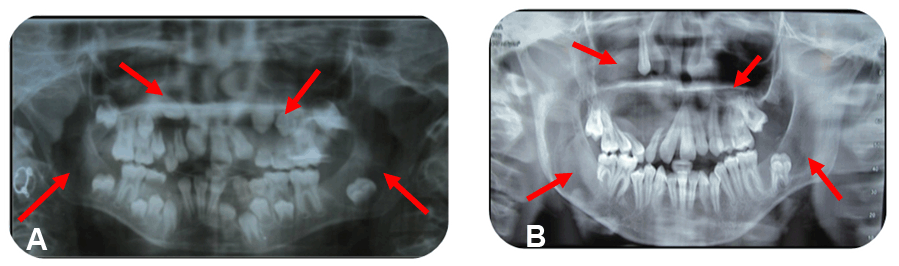
Her past history revealed that she was a diagnosed and surgically operated case of dentigerous cyst in relation to left deciduous maxillary teeth (C, D) at 6 years of age. At the age of 10 years, she was suspected for re-infection of the cyst with intra oral sinus opening and was advised an orthopantomogram (OPG) which revealed multiple radiolucencies involving maxilla and mandible (Figure 2A). Her personal history revealed mixed diet with no deleterious habits and family history was not contributory and there was no history of consanguineous marriage of her parents.
On extraoral examination, her face was asymmetrical due to diffuse swelling measuring 4x4 cm approximately in the right middle third of face with involvement of right ala of nose and upper lip associated with obliteration of nasolabial fold (Figure 1A) and it was non-tender, firm to hard in consistency with no local rise of temperature on palpation. Temporomandibular joint examination revealed tenderness on palpation on right side while opening with adequate mouth opening of 35 mm. Intraoral examination revealed missing 13, 25, 37 and an oval shaped swelling measuring 4x2 cm approximately in relation to right maxillary teeth (Figure 1B). It was soft in consistency, fluctuant, compressible, and tender. A panoramic radiograph was taken which revealed well defined unilocular multiple radiolucencies bilaterally in maxilla and mandible (Figure 2) and the radiolucencies are described in (Table 1).
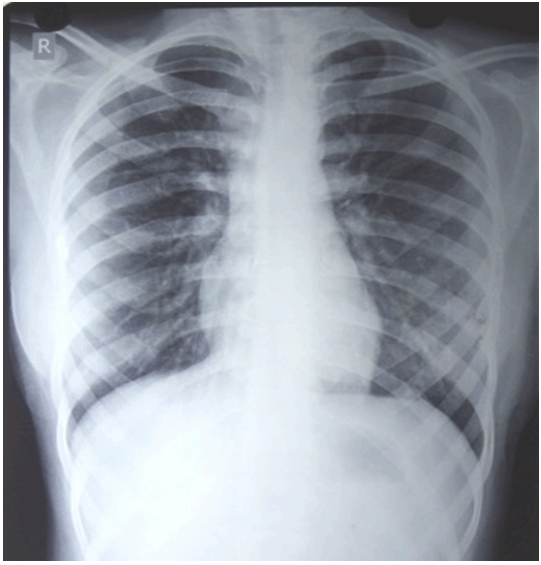
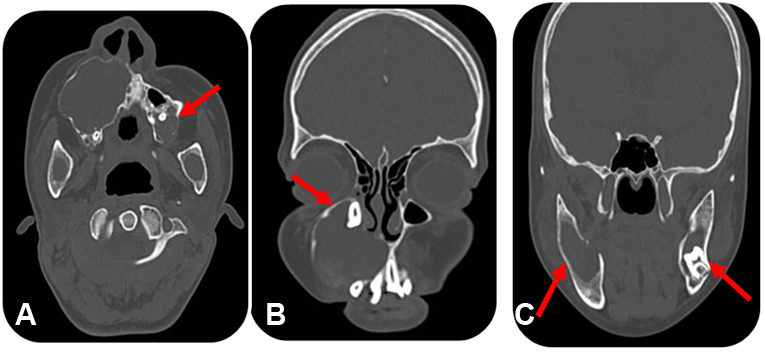
The patient was further evaluated to rule out any syndrome due to the presence of multiple cystic lesions. The patient's chest (Figure 3) and skull radiographs were unremarkable. Dermatological examination did not reveal any cutaneous abnormalities like palmar and plantar defects. Hematologic investigations were within normal limits. Computed tomography scan of maxillofacial region with axial (Figure 4A) and coronal (Figure 4B-C) sections revealed multiple hypodense lesions in the maxilla and mandible.
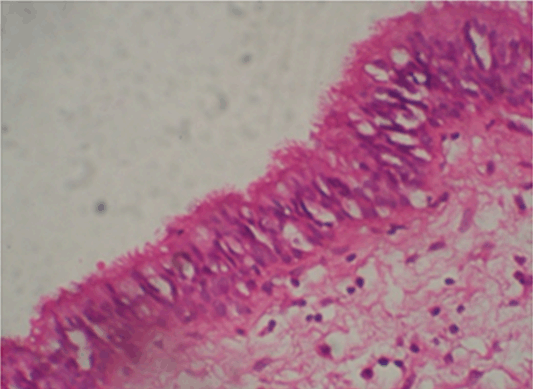
Aspiration of the cystic lesions showed white cheesy keratin like material. Incisional biopsy was done in relation to right and left maxilla and mandible and was subjected to histopathological examination which was suggestive of multiple KOTs. Under general anesthesia, four lesions were enucleated (Figure 5A-B) followed by chemical cauterization (Carnoy's solution) and tissue specimens were sent for histopathologic examination (Figure 6) which revealed "Parakeratinized Odontogenic Keratocyst" from all four quadrants which were of uniform epithelial lining 6–8 cells thick lacking rete ridges. The lumen was filled with keratin, cholesterol clefts and hyaline bodies and the connective tissue wall show 3–4 micro cysts, cholesterol clefts and inflammatory cells at few areas.
Follow-up was done on 1st, 2nd and 3rd months postoperatively. The postoperative period was uneventful without any complications. Patient is asymptomatic since then without any complaints.
|
|
The KOT is a common developmental odontogenic cyst and its biologic behavior is similar to a benign neoplasm [5]. It occurs at any age with peak incidence during the second and third decades, with a slight male predominance [6]. In 25–40% cases, involvement of unerupted tooth has been reported [5]. Brahnon in his analysis of clinical features of 312 cases of OKC found that, 5.8% of patients with multiple OKC had no other features of syndrome [7].The KOT is locally destructive and recurrence rate is very high where published recurrence rates for keratocystic odontogenic tumors range from 5% to about 70%. The recurrence rate of KOT associated with NBCC is about 82% whereas for solitary KOT is ranging between 2.5% and 62.5% [6].
PTCH (patched), a tumor suppressor gene involved in both syndrome associated and sporadic KOTs, occurs on chromosome 9q22.3 – q31. Syndromes associated with multiple KOTs are Gorlin–Goltz syndrome/NBCCS, oro-facial-digital syndrome, Noonan syndrome, Ehler danlos syndrome [5]. There is no specific laboratory test to diagnose NBCCS, although the diagnosis is made clinically using the criteria suggested by Evans et al. [6]
.
Evans et al. first published major and minor criteria for diagnosis of Gorlin–Goltz syndrome, later modified by Kimonis et al. and according to them the positive diagnosis of Gorlin–Goltz syndrome is when two major or one major and two minor criteria are satisfied [6] [7]
.
The major criteria are:
- Multiple Basal cell carcinomas (BCCs) or one occurring under the age of 20 years
- Histologically proven KOTs of the jaws
- Palmar or plantar pits (three or more)
- Bilamellar calcification of the falx cerebri
- Bifid, fused or markedly splayed ribs
- First degree relative with NBCCS
The minor criteria are:
- Macrocephaly (adjusted for height)
- Congenital malformation: Cleft lip or palate, frontal bossing, coarse face, moderate or severe hypertelorism
- Other skeletal abnormalities: Sprengel deformity, marked pectus deformity, marked syndactyly of the digits
- Radiological abnormalities: Bridging of the sella turcica, vertebral anomalies such as hemivertebrae, fusion or elongation of the vertebral bodies, modeling defects of the hands and feet or flame shaped hands or feet
- Ovarian fibroma
- Medulloblastoma
However, there may be variations in the major diagnostic criteria for NBCCS in some populations due to genetic and geographic differences [8]. Our patient was apparently healthy and did not meet any of these diagnostic criteria for NBCCS, such as pits on the palms of the hands or soles of the feet, multiple basal cell skin cancers, skeletal (bone) changes, calcium deposits in the brain and developmental disability.
Histopathological examination in our case revealed parakeratinized stratified squamous epithelium with absence of rete pegs and palisaded basal cell layer, giving an appearance of tombstone or picket fence. The connective tissue revealed multiple daughter cysts and cystic lumen revealed keratin, giving a picture of KOT.
Treatments are normally classified as conservative or aggressive. Conservative treatment modalities include simple enucleation, with or without curettage, or marsupialization [8]. Aggressive treatment modalities includes peripheral ostectomy, chemical curettage with carnoy's solution, cryotherapy, or electrocautery and resection [9]. The goal is to choose the treatment modality that Carries the lowest risk of recurrence and the least morbidity. Voorsmit et al. [9] (1981) have observed a reduction in recurrence rate if enucleation followed by application of Carnoy's solution (2.5%) when compared with enucleation alone (13.5%). Therefore, enucleation followed by application of Carnoy's solution can result in a reasonably low recurrence rate with less morbidity when compared to other treatment modalities. Kuroyanagi et al. suggested the presence of Ki-67 expression in OKC, which might be helpful for considering the alternative surgical procedure to avoid recurrence and might be used as a prognostic indicator. In recent studies, the hypothesis that suppression of sonic hedgehog (SHH) signaling pathway might be effective for the treatment of OKC [10]
.
|
-
Chuong R, Donoff RB, Guralnick W. The odontogenic keratocyst. J Oral Maxillofac Surg 1982 Dec;40(12):797–802.
[CrossRef]
[Pubmed]

-
Stoelinga PJ, Bronkhorst FB. The incidence, multiple presentation and recurrence of aggressive cysts of the jaws. J Craniomaxillofac Surg 1988 May;16(4):184–95.
[CrossRef]
[Pubmed]

-
Blanchard SB. Odontogenic keratocysts: review of the literature and report of a case. J Periodontol 1997 Mar;68(3):306–11.
[CrossRef]
[Pubmed]

-
Yucetas S, Cetiner S, Oygur T. Suspected familial odontogenic keratocysts related to Gorlin Goltz syndrome. Saudi Med J 2006 Feb;27(2):250–3.
[Pubmed]

-
Rajendran R, Sivapathasundharam B. Shafer's Textbook of Oral Pathology. In: Shafer WG, Hine MK, Levy BM eds. Cysts and Tumors of Odontogenic Origin. 7ed. New Delhi: Elsevier; 2012. p. 1099–110.

-
Evans DG, Ladusans EJ, Rimmer S, Burnell LD, Thakker N, Farndon PA. Complications of the naevoid basal cell carcinoma syndrome: results of a population based study. J Med Genet 1993 Jun;30(6):460–4.
[CrossRef]
[Pubmed]

-
Kimonis VE, Goldstein AM, Pastakia B, et al. Clinical manifestations in 105 persons with nevoid basal cell carcinoma syndrome. Am J Med Genet 1997 Mar 31;69(3):299–308.
[CrossRef]
[Pubmed]

-
Manfredi M, Vescovi P, Bonanini M, Porter S. Nevoid basal cell carcinoma syndrome: a review of the literature. Int J Oral Maxillofac Surg 2004 Mar;33(2):117–24.
[CrossRef]
[Pubmed]

-
Voorsmit RA, Stoelinga PJ, van Haelst UJ. The management of keratocysts. J Maxillofac Surg 1981 Nov;9(4):228–36.
[CrossRef]
[Pubmed]

-
Hammannavar R, Holikatti K, Bassappa S, Shinde N, Reddy M, Chidambaram YS. Multiple, multifocal odontogenic keratocysts in non-syndrome patient: a case-report. Oral Health Dent Manag 2014 Jun;13(2):189–93.
[Pubmed]

|