|

|
 |
|
Case Report
| ||||||
| Primary leiomyosarcoma of the nipple-areola complex with an unusual clinical presentation: A case report | ||||||
| Xavier Guedes1, Meritxell Medarde2, Tamara Parra3, MJ Martinez3, Enric de Caralt4, Constanti Serra5 | ||||||
|
1MD, Member of Staff of the Department of General Surgery, Consorci Hospitalari de Vic, Barcelona, Spain.
2MD, Member of Staff of the Department of General Surgery and Breast Surgery, Consorci Hospitalari de Vic, Barcelona, Spain. 3MD, Member of Staff of the Department of Pathology, Consorci Hospitalari de Vic, Barcelona, Spain. 4MD, Chief of Staff of the Department of General Surgery, Consorci Hospitalari de Vic, Barcelona, Spain. 3MD, Member of Staff of the Department of General Surgery and Chief of Breast Surgery Consorci Hospitalari de Vic, Barcelona, Spain. | ||||||
| ||||||
|
[HTML Abstract]
[PDF Full Text]
[Print This Article]
[Similar article in Pumed] [Similar article in Google Scholar] 
|
| How to cite this article: |
| Guedes X, Medarde M, Parra T, Martinez MJ, de Caralt E, Serra C. Primary leiomyosarcoma of the nipple-areola complex with an unusual clinical presentation: A case report. International Journal of Case Reports and Images 2014;5(1):66–70. |
|
Abstract
|
|
Introduction:
Primary leiomyosarcoma of the nipple is a rare disease that accounts for less than 0.1% of all malignant tumors of the breast. About 35 cases have been described in English literature.
Case Report: We report a case of a 46-year-old female presenting with a two-year suppurative squamous plaque-type lesion of the right nipple at first considered as an unusual Paget’s disease presentation. No adenopathies or associated lesions were identified. Core biopsy was informed as a possible leiomyosarcoma. It was decided to remove the lesion surgically by wide excision of the nipple-areola complex with adequate surgical margins with no lymph node dissection or adjuvant radiochemotherapy. Histopathology and immunohistochemistry confirmed the diagnosis of leiomyosarcoma. One year after the surgery there are no recurrences or distant metastasis. Conclusion: More data and long-term follow-up is necessary to understand prognosis and develop an adequate treatment protocol for this type of neoplasms. | |
|
Keywords:
Leiomyosarcoma, Breast, Sarcoma, Nipple-areola complex
| |
|
Introduction
| ||||||
|
Since it was first described in 1968 by Waterworth, [1] primary leiomyosarcoma of the breast has been discussed in about 35 reported cases in English literature. This entity is rare considering that it accounts for 5–10% of breast sarcomas, that only account for 0.1% of all malignant tumors of the breast. [2] From the reported cases, less than a third are located on the nipple-areola complex. [3] We describe the unusual clinical presentation, diagnosis and treatment of a 46-year-old female with a leiomyosarcoma of the nipple-areola complex and a review of the existing literature. | ||||||
|
Case Report
| ||||||
|
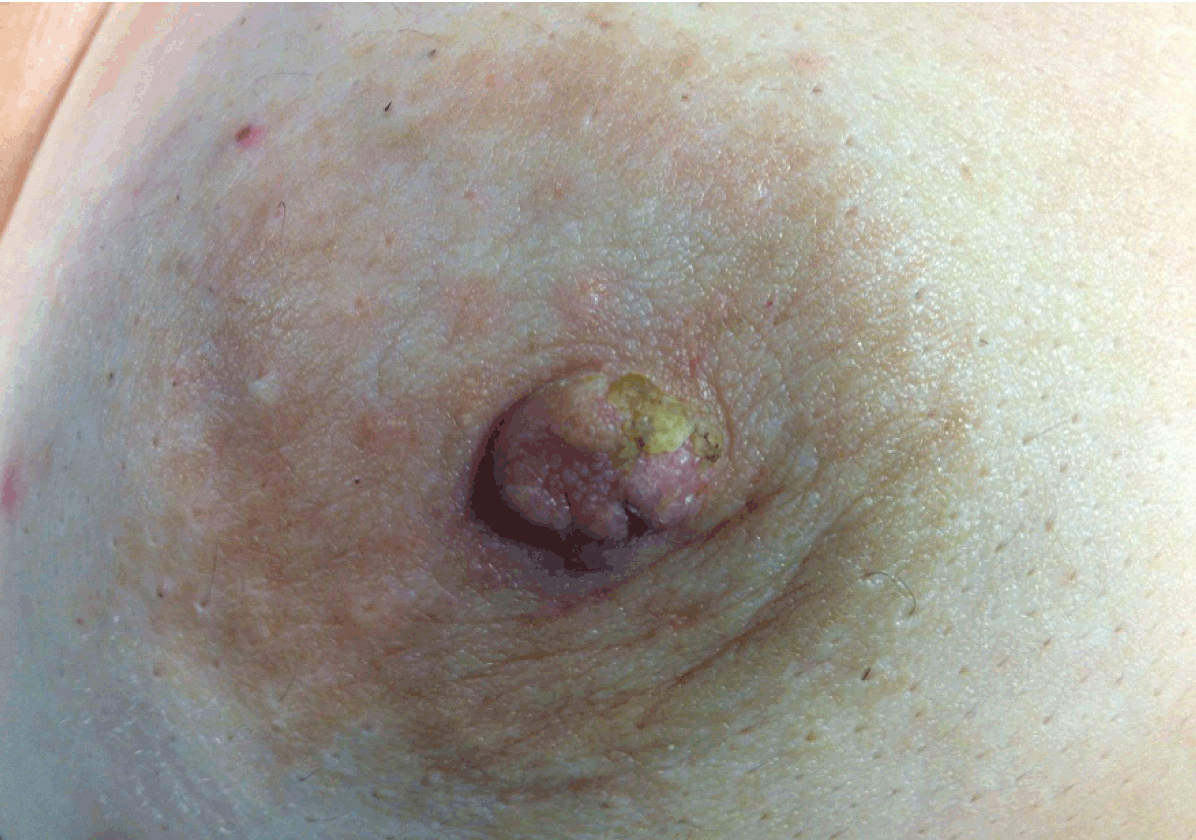
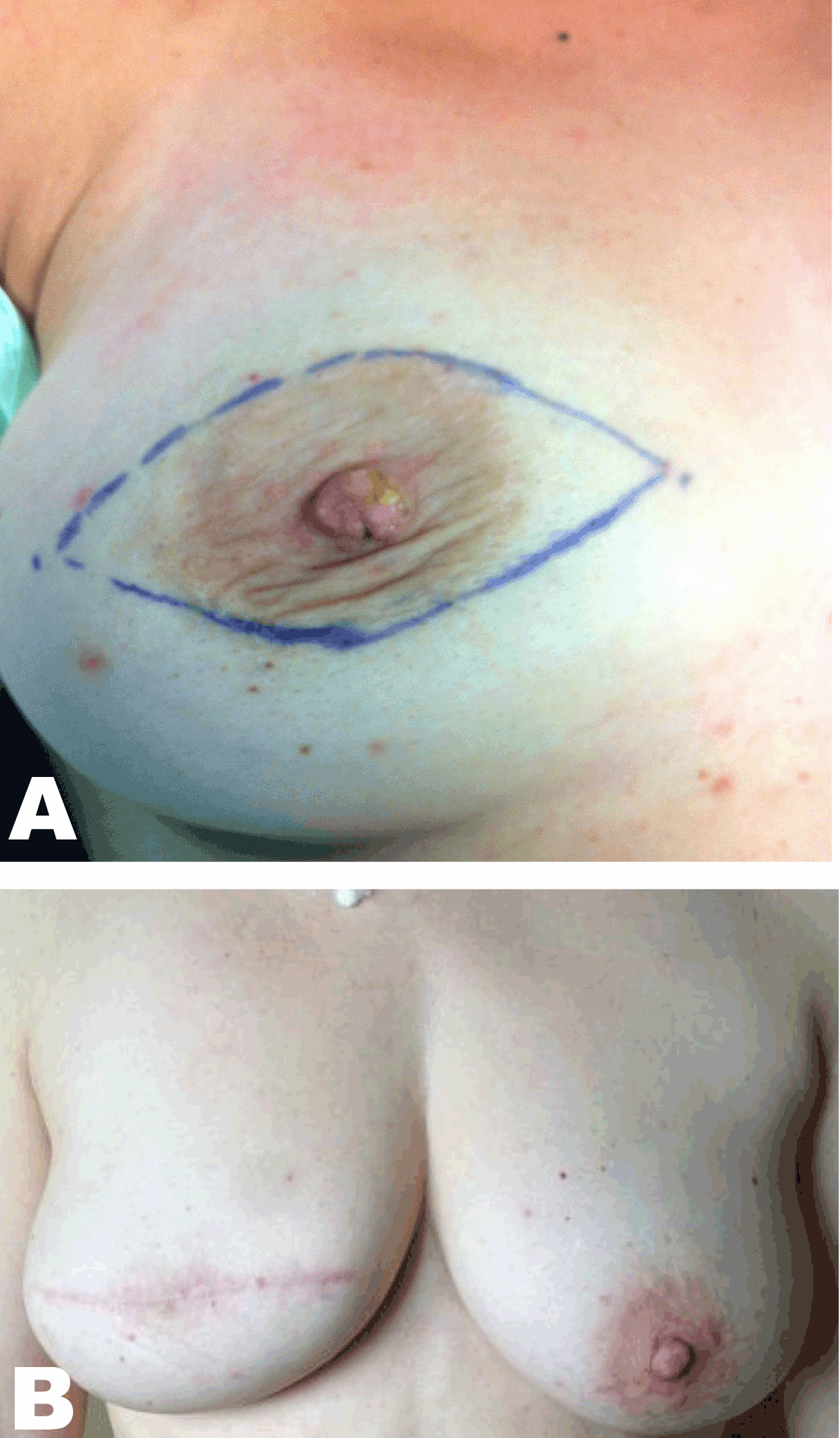
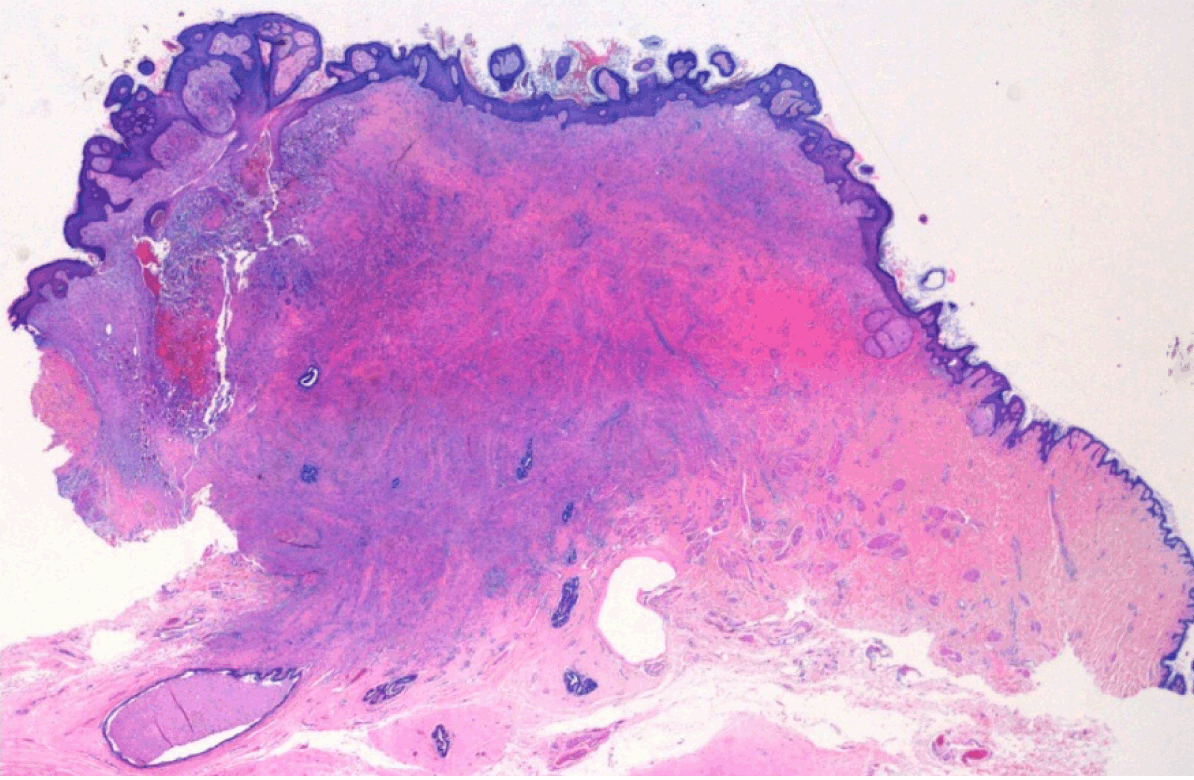
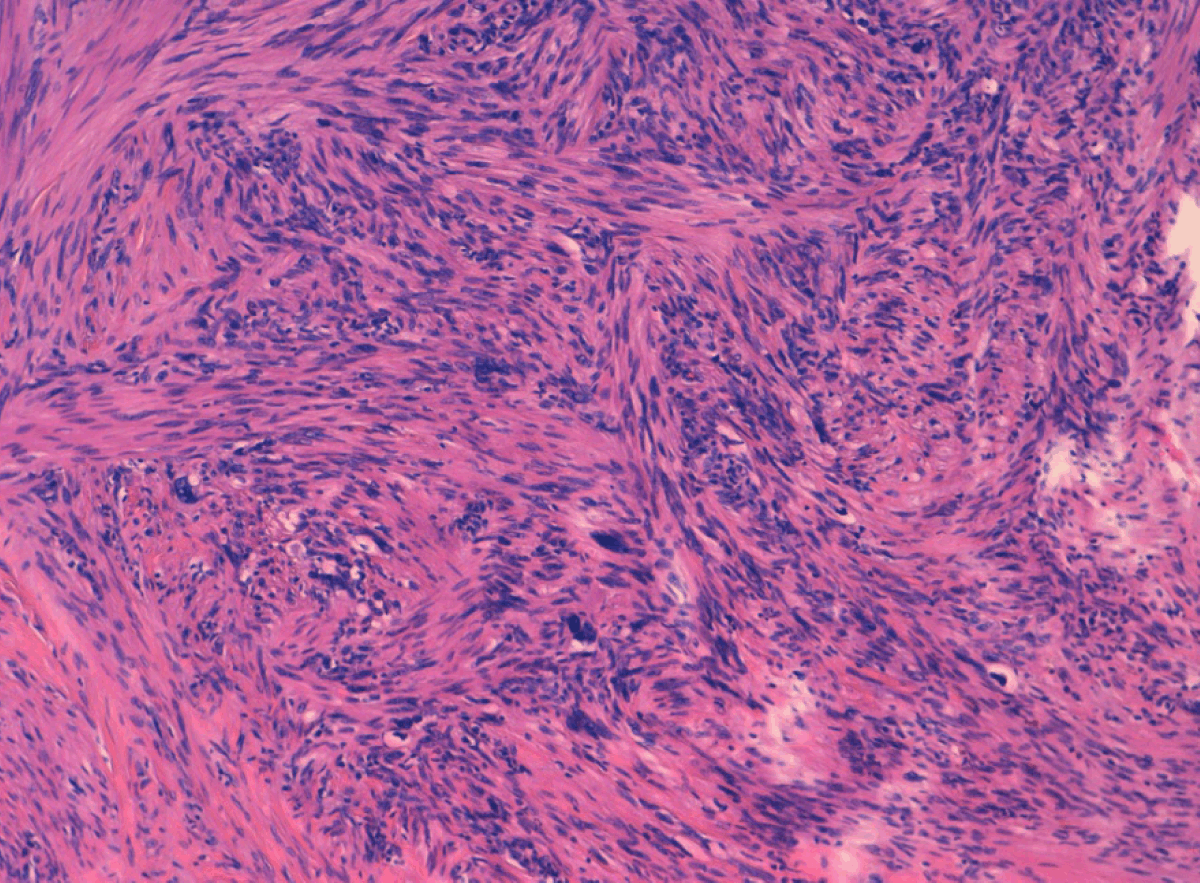
A 46-year-old female came to our clinic presenting with an induration of the right nipple after more than two years experiencing several episodes of suppuration of a punctate lesion in the left margin of the right nipple. The past medical history of the patient was without pathological findings and had no family history of malignancies in any first-degree relatives. She had a routine mammography performed four years before with no pathological findings. Physical examination only revealed induration of the right nipple with increased sensitivity and a squamous plaque-type lesion. (Figure 1) No axillar, supraclavicular or cervical lymph nodes were palpable. Ultrasonography did not find any suspicious lesions and assessed a BIRADS 1 category (Breast Imaging-Reporting and Data System of the breast 1: no images suggest breast malignant patologies). A preoperative core biopsy of the indurated lesion was performed, and was described by the pathologist as a smooth muscle neoplasm with atypia that suggested a leiomyosarcoma with affected margins. Immunohistochemistry revealed actin (Dako- Clon 1A4, Denmark) and desmin (Dako-Clon D33, Denmark) positivity. The patient underwent a second surgical procedure for a wide excision of the nipple-areola complex with 4–5 cm safe margins (breast parenchyma) and without axillary lymph node dissection. (Figure 2) Macroscopically, the tumor measured 1.6x1 cm located on the left margin of the nipple with superficial pale desquamative white patches. Histological examination revealed a leiomyosarcoma of the nipple, 1.6 cm in diameter, with hyper cellular areas composed of round cells, bundles of spindle cells with focal pleomorphic cells and 3 mitosis per 10 high-power fields (HPF) without necrosis and no affected margins. (Figure 3) (Figure 4) (Figure 5) Immunohistochemistry confirmed actin and desmin positivity and the cell proliferation marker Ki-67 (Dako-Clon MIB-1, Denmark) showed an index of 15. After surgery, a computed tomography (CT) scan of the chest and abdomen were performed discarding distant metastasis. After one year, the patient is in good health with no evidence of local recurrence. | ||||||
| ||||||
| ||||||
| ||||||
| ||||||
| ||||||
|
Discussion
| ||||||
|
We report a case of a primary leiomyosarcoma of the nipple which only accounts for less than 0.1% of all malignant neoplasms of the breast. Most patients are female, though there are at least four reported cases of male subjects with primary leiomyosarcoma of the breast. [4] It usually appears in postmenopausal women between the ages of fifty to eighty years and in some rare cases it can appear in young girls. [5] Most cases describe a painless slow-growing nodular mass. In our case the patient described a punctate lesion that underwent several episodes of suppuration that gradually turned into a plaque-type lesion. No reports of this type of clinical presentation where found on previous literature. At first it was thought to be a rare case of Paget’s disease because of the similarity to the eczema that appears on the nipple on this disease. The importance of describing these rare cases is to avoid the risk of not including this neoplasm in the differential diagnosis of neoplasms of the breast, specially sharing similarities with a wide range of benign and malignant neoplasms such as leiomyomas, peripheral nerve sheath tumors, malignant phyllodes tumors, malignant fibrous histiocytoma, dermatofibrosarcomas, spindle cell malignant melanoma and other sarcomatoid carcinomas. [6] Mammography and ultrasonography can often lead to misdiagnosis of these tumors because of the difficulty in differentiating them from benign lesions such as fibroadenomas, phyllodes tumors or intracystic papillomas. Even fine-needle aspiration cytology (FNAC), core-needle or surgical biopsies are not enough to make a definitive diagnosis of leiomyosarcoma. A complete excision of the tumor, immunohistochemistry, and detailed histologic examination is needed for correct diagnosis. [3] Most cases are not diagnosed preoperatively for these reasons. Microscopically, the tumors are composed of atypical and hyperchromatic spindle-shaped cells arranged in interdigitating fascicles and the cytological characteristics are hyperchromasia in the nuclei, pleomorphism, and mitosis. [7] The key to discern leiomyomas from leiomyosarcomas is the presence of mitosis, and in previous literature the mitosis of these tumors ranged from 2 to 21 per 10 HPF. [8] [9] Immunohistochemical profile of smooth muscle actin, vimentin and desmin positivity can be helpful but not pathognomonic of the tumor. [5] There is still controversy on the origin of this tumor. In the nipple-areolar complex it might originate from the smooth muscle bundles that surround the lactiferous ducts and the arrector pili muscle at the periphery of the areola. Outside this region it is believed to originate from the smooth muscle cells of the vascular walls in the mammary parenchyma. [3] [6] As for any unusual or infrequent type of tumor, there is no clear consensus on the best treatment modality. Since 1968, it has been treated surgically either by simple excision, modified radical or radical mastectomy. Some cases included axillary dissection and others preferred the use of adjuvant radiochemotherapy. Though there were cases that reported metastasis or local recurrences, most authors agree that there is not enough evidence that supports the idea of lymphatic spread and nodal metastasis as features associated with these neoplasms, similarly to other breast sarcomas. [10] [11] [12] Usually, tumors of the nipple-areola region are treated as other skin sarcomas, with wide local excision leaving 3 to 5 cm safe margins, and those involving mammary parenchyma undergo simple or modified radical mastectomy with no lymph node dissection. Adjuvant radiochemotherapy is still an option considered by some authors. [6] Better prognosis has been associated with adequate surgical margins and with low cellular pleomorphism. [1] [13] Wong et al. review of previous cases suggests that leiomyosarcoma of the nipple-areola complex has less local recurrences or metastases compared to those located on mammary parenchyma, though most cases had no long-term follow up. In general, the prognosis of patients with leiomyosarcoma of the breast is better than that of other sarcomas of the breast. [14] | ||||||
|
Conclusion
| ||||||
|
Still there is not enough gathered data on this type of neoplasms. We describe a case with a different clinical presentation thus supporting the idea that we need more cases to develop a better understanding of this disease. Long-term follow-up is necessary to understand prognosis thus to find the need for less or more aggressive treatments such as wider surgical resections or the use of adjuvant radiochemotherapy, always considering the added risk of causing more damage or developing second malignancies. | ||||||
|
References
| ||||||
| ||||||
|
[HTML Abstract]
[PDF Full Text]
|
|
Author Contributions
Xavier Guedes – Substantial contributions to conception and design, Acquisition of data, Analysis and interpretation of data, Drafting the article, Revising it critically for important intellectual content, Final approval of the version to be published Meritxell Medarde – Substantial contributions to conception and design, Drafting the article, Revising it critically for important intellectual content, Final approval of the version to be published Tamara Parra – Substantial contributions to conception and design, Drafting the article, Revising it critically for important intellectual content, Final approval of the version to be published MJ Martinez – Substantial contributions to conception and design, Drafting the article, Revising it critically for important intellectual content, Final approval of the version to be published Enric de Caralt – Substantial contributions to conception and design, Drafting the article, Revising it critically for important intellectual content, Final approval of the version to be published Constanti Serra – Substantial contributions to conception and design, Drafting the article, Revising it critically for important intellectual content, Final approval of the version to be published |
|
Guarantor of submission
The corresponding author is the guarantor of submission. |
|
Source of support
None |
|
Conflict of interest
Authors declare no conflict of interest. |
|
Copyright
© Xavier Guedes et al. 2014; This article is distributed the terms of Creative Commons Attribution License which permits unrestricted use, distribution and reproduction in any means provided the original authors and original publisher are properly credited. (Please see Copyright Policy for more information.) |
|
|