| Table of Contents |  |
|
Case Report
|
| Metastatic retroperitoneal fibrosis as first sign of breast cancer |
| Neeraj Singh1, Arvinder Bhinder1 |
|
1Department of Internal Medicine, The Ohio State University Medical Center, Columbus, Ohio, USA.
|
|
doi:10.5348/ijcri-2012-06-132-CR-5
|
|
Address correspondence to: Dr. Neeraj Singh MBBS Assistant, Professor of Medicine, Division of Nephrology 395 W. 12th Avenue Ground Floor Columbus OH 43210 USA Phone: 614-293-4997 Fax: 614-293-3073 Email: neeraj.singh@osumc.edu |
|
[HTML Abstract]
[PDF Full Text]
|
| How to cite this article: |
| Singh N, Bhinder A. Metastatic retroperitoneal fibrosis as first sign of breast cancer. International Journal of Case Reports and Images 2012;3(6):23–25. |
|
Abstract
|
|
Introduction:
Malignancy is an uncommon cause of retroperitoneal fibrosis.
Case Report: We discuss the case of a 66-year-old female who presented with anuric acute renal failure due to obstructive uropathy from retroperitoneal soft tissue infiltration and entrapment of both ureters. Fine needle aspiration and special staining of the retroperitoneal mass confirmed the malignant retroperitoneal fibrosis with breast as the primary site. Renal failure improved temporarily with bilateral ureteral stent placement but patient died during the course of palliative chemotherapy. Conclusion: Patients with retroperitoneal fibrosis often presents a diagnostic challenge. It is important to distinguish malignant retroperitoneal fibrosis from non-malignant causes due to its poor prognosis. | |
|
Key Words:
Breast cancer, Retroperitoneal fibrosis, Acute renal failure
| |
|
Introduction
| ||||||
|
Retroperitoneal fibrosis (RPF) is a rare disorder characterized by the development of extensive fibrosis throughout the retroperitoneum. Most patients present with nonspecific symptoms like weight loss, malaise, anorexia, back pain etc., but more often than not, there can be entrapment of individual organs/structures like abdominal aorta, gonadal, celiac, superior mesenteric, iliac or renal arteries, inferior vena cava, ureters, spinal cord and even bowels with their attendant consequences. We report a case of a patient with obstructive uropathy from bilateral ueteral obstruction due to malignant RPF with no prior history of primary cancer. | ||||||
|
Case Report
| ||||||
|
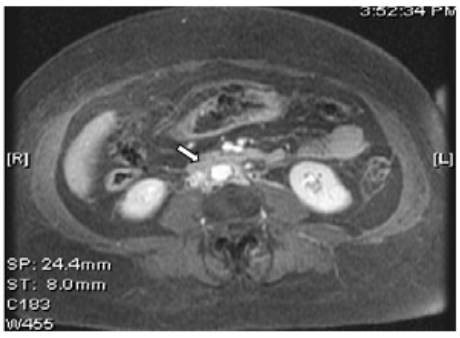
A 66-year-old African American female presented to the emergency department with a two months history of progressively decreasing urine output. She noticed no urine output for last one day. She had no history of chronic kidney disease, kidney stones or other significant medical illnesses in the past. She denied any abdominal pain, fever, chills or urinary tract symptoms. Her examination revealed blood pressure of 187/110 mmHg with 2+ pitting edema at ankles. A foley catheter was inserted in the emergency room but no urine output was recorded. Laboratory data showed serum creatinine of 9.2 mg/dl. Her serum creatinine was normal at 0.8 mg/dl, three months ago. A renal ultrasound showed normal sized kidneys with mild bilateral pelvicaliectasis. A non-contrast computed tomography (CT) scan of abdomen was unremarkable for stones but revealed mild hydronephrosis with indistinct periaortic fullness (Figure 1, arrow). Retrograde pyelogram revealed bilateral ureteral strictures. After placement of uretral stents, patient had brisk urine output and serum creatinine trended down back to the normal range. MRI with gadolinium done on day-3 of admission, showed an enhancing soft tissue infiltration encasing the abdominal aorta and IVC (Figure 2). No significant pelvic or retroperitoneal lymphadenopathy was identified. Fine needle aspiration biopsy of the retroperitoneal infiltration revealed metastatic adenocarcinoma in the background of dense fibrosis. The suspicion was raised for lungs, breast or uterus as the source of primary tumor. Patient's history was negative for any pulmonary, uterine or breast related symptoms. However, her breast examination that was deferred earlier on admission was suspicious for a left breast nodule. The mammogram revealed a 2x3 cm soft tissue density and an ultrasound guided fine needle aspiration biopsy confirmed the breast adenocarcinoma. The positive immunohistochemical staining of the malignant retroperitoneal tissue cells for estrogen, progesterone and herceptin-2 receptors, confirmed breast as the primary site. Patient was referred to oncology and she was initiated on palliative chemotherapy with weekly paclitaxel, carboplatin and herceptin. After six weeks of chemotherapy, patient was admitted with pneumonia, severe sepsis and respiratory failure. As per family and patient's prior wishes, she was made comfort care only and she expired two days after her hospitalization. | ||||||
| ||||||
| ||||||
|
Discussion
| ||||||
|
Retroperitoneal fibrosis, although uncommon, is an important cause of obstructive uropathy in patients presenting with anuric acute renal failure in the absence of discernible hydronephrosis. A careful interpretation of the imaging manifestations of retroperitoneal fibrosis is vital to ensure a correct diagnosis. [1] [2] Although, mostly idiopathic, [3] RPF can ensue secondary to inflammation, drugs, infection or malignancy. [4] The most common malignancies that can metastasize to retroperitoneum and incite fibroplastic reaction include, breast, lung, gastrointestinal, genitourinary, thyroid, lymphoma, sarcoma and carcinoid. [5] Prior reported cases of malignant RPF with breast cancer as the primary site, all mention either recent or remote history of a breast lesion, [6] [7] but our patient had no history of breast cancer or other malignancies in the past. | ||||||
|
Conclusion
| ||||||
|
Breast carcinoma should be strongly considered as the primary tumor in elderly females presenting with malignant RPF of unclear origin. | ||||||
|
References
| ||||||
| ||||||
|
[HTML Abstract]
[PDF Full Text]
|
|
Author Contributions:
Neeraj Singh - Substantial contributions to conception and design, Acquisition of data, or analysis and interpretation of data, Drafting the article or revising it critically for important intellectual content, Final approval of the version to be published Arvinder Bhinder - Substantial contributions to conception and design, Acquisition of data, or analysis and interpretation of data, Drafting the article or revising it critically for important intellectual content, Final approval of the version to be published |
|
Guarantor of submission:
The corresponding author is the guarantor of submission. |
|
Source of support:
None |
|
Conflict of interest:
Authors declare no conflict of interest. |
|
Copyright:
© Neeraj Singh et al. 2012; This article is distributed the terms of Creative Commons Attribution License which permits unrestricted use, distribution and reproduction in any means provided the original authors and original publisher are properly credited. (Please see Copyright Policy for more information.) |
|
|