| Table of Contents |  |
|
Case Report
|
| Iron pill induced bronchitis |
| Lisette Delgado-Sanchez1, Paramjeet Atwal1, Padmanabhan Krishnan2 |
|
1Fellow Pulmonary and Critical Care Medicine, SUNY Downstate Medical Center, Brooklyn, NY.
2Attending Pulmonary and Critical Care service, Coney Island Hospital, Brooklyn, NY. |
|
doi:10.5348/ijcri-2012-04-112-CR-9
|
|
Address correspondence to: Lisette Delgado-Sanchez MD Coney Island Hospital 2461 Ocean Parkway suite 9 Brooklyn NY 11235 USA Phone: 718-616-3171, 786-208-7182 Fax: 718-616-4071 Email: yilibet@yahoo.com |
|
[HTML Abstract]
[PDF Full Text]
|
| How to cite this article: |
| Delgado-Sanchez L, Atwal P, Krishnan P. Iron pill induced bronchitis. International Journal of Case Reports and Images 2012;3(4):34–36. |
|
Abstract
|
|
Introduction:
Pill induced esophagitis and gastritis is well described.
Case Report: We describe a patient who aspirated an iron pill and developed acute bronchitis with hemoptysis and localized airway obstruction. Conclusion: We report this case in order to heighten awareness of this entity. | |
|
Key Words:
Iron Pill bronchitis
| |
|
Introduction
| ||||||
|
Iron supplementation tablets are used in the daily routine of many patients with high risk for aspiration (elderly, pregnant and pediatric population). Iron tablets can cause particular damage if aspirated. We present a case of Iron pill induced bronchitis and describe literature future complications of this entity to highlight the knowledge of this potentially common encounter in the medical practice. | ||||||
|
Case Report
| ||||||
|
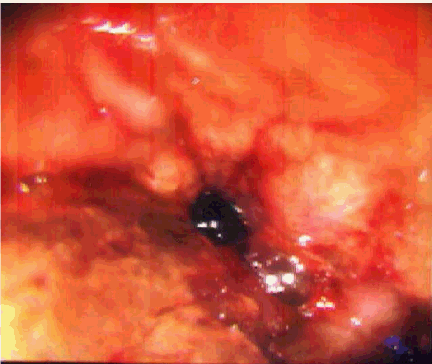
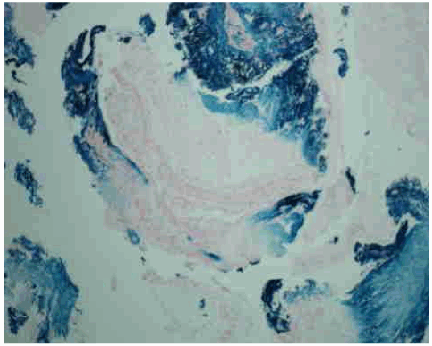
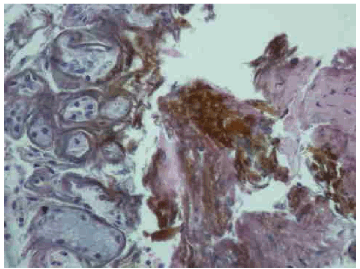
A 64-year-old woman presented with acute onset of cough with hemoptysis 20 minutes after ingestion of her daily iron tablets that she has been taking for the last three weeks. She also experienced wheezing and shortness of breath that lasted for 4-5 hours along with cough and dark brownish sputum which brought her to the hospital. Three weeks prior to this, she was diagnosed to have severe iron deficiency anemia and required blood transfusions. She was placed on oral iron therapy by her physician with ferrous sulfate 325 mg tds, PO. She experienced generalized weakness and dyspnea on exertion as a result of the anemia prior to the transfusions. Otherwise, she has been well. She was an ex-smoker (60 pack/year) who quit 20 years ago. She had traveled frequently to Mexico and the Caribbean in the last year. Examination was remarkable only for auscultatory wheeze over the right mid zone anteriorly and right base posteriorly. Hematologic investigations showed microcytic anemia with hemoglobin of 11.1 g/dL and mean corpuscular volume, (MCV) of 73 fL. Chest radiograph revealed a large left hiatal hernia but was otherwise unremarkable. A contrast chest computed tomography (CT) scan confirmed the hiatal hernia but was devoid of any other abnormality. Fiberoptic bronchoscopy done within 24 hours revealed that the tracheal and bronchial mucosa was erythematous and edematous. The mucosa at the bifurcation of the right middle and lower lobe and in the right lower lobe was most affected and appeared corrugated, ulcerated, friable and bled easily (Figure 1). The area was lavaged and thick brownish secretions were suctioned. Bronchial biopsy at the level of right middle and lower lobe carina and from the right lower lobe revealed features of mucosal burn with edema and inflammation and stained positive for iron with prussian blue stain (Figure 2, 3). The patient was assessed for adequacy of the swallowing mechanism which was found to be adequate. Following discharge she was scheduled to be seen over the next six months to reassess for evidence of local airway sequela however patient was lost to follow up. | ||||||
|
| ||||||
|
| ||||||
| ||||||
| ||||||
|
Discussion
| ||||||
|
Pill induced esophagitis and gastritis is a well known entity and a variety of medications have been implicated. [1] [2] Pill induced bronchitis, the result of aspiration, is far less common but well documented. Among these, iron pill aspiration stands out for the intensity of the bronchial injury in response to the oxidative effect of iron within a moist mucosa, in the form of a caustic chemical burns as seen in our patient. This inflammatory response can persist even months after aspiration and complications such bronchial necrosis and bronchial stenosis have been described with the formation of granulation tissue and ensuing fibrosis. [3] [4] [5] [6] [7] As iron is a common medication, used both in young and old, there is a potential for aspiration and bronchial injury in the form of acute or persistent bronchitis. Lee et al. proposed the term "Syndrome of iron pill aspiration" to include the sequence of aspiration, iron deposition in bronchial mucosa and the ensuing intense bronchial mucosal inflammation. [7] Our patient had symptoms and signs of airway obstruction, evidence of intense bronchial inflammation on bronchoscopy and presence of iron in bronchial mucosal tissue to justify the term "Iron pill bronchitis" with obstruction. Late reactions described after "Iron pill bronchitis" include bronchial necrosis, bronchial stenosis from granulation tissue formation and fibrosis. This needs treatment modalities such as lobectomy, balloon bronchial dilatation and bronchoplasty. [3] [5] [6] [7] [8] Topical Mytomycin C as has been used to attempt to prevent stricture formation in the involved bronchus. [7] Whether the early lavage performed in this patient would ameliorate the local reaction and its effects is not clear and therefore, close follow up is indicated for at least six months for signs of local complications. We describe this patient as a reminder that in patients on iron pill therapy, the development of acute bronchitis, hemoptysis, persistent bronchitis or bronchial stenosis should raise suspicion of this entity that we describe as "Iron pill bronchitis". Further damage can be prevented if it is recognized and treated early. As iron is caustic to the airway muscle, patients in whom iron pill aspiration is likely, prompt bronchoscopy will allow for early diagnosis and lavage. It is not clear whether a lavage for removal of as much of the caustic agent as possible will be beneficial. | ||||||
|
Conclusion
| ||||||
|
Iron pill can induce acute bronchitis, hemoptysis, persistent bronchitis and chronic stenosis if aspirated. Early suspicion and therapy could avoid further damage and close follow up is warranted. | ||||||
|
References
| ||||||
| ||||||
|
[HTML Abstract]
[PDF Full Text]
|
|
Author Contributions:
Lisette Delgado-Sanchez - Conception and design, Acquisition of data, Analysis and interpretation of data, Drafting the article, Critical revision of the article, Final approval of the version to be published Paramjeet Atwal - Analysis and interpretation of data, Critical revision of the article, Final approval of the version to be published Padmanabhan Krishnan - Analysis and interpretation of data, Drafting the article, Critical revision of the article, Final approval of the version to be published |
|
Guarantor of submission:
The corresponding author is the guarantor of submission. |
|
Source of support:
None |
|
Conflict of interest:
Authors declare no conflict of interest. |
|
Copyright:
© Lisette Delgado-Sanchez et. al. 2012; This article is distributed the terms of Creative Commons Attribution License which permits unrestricted use, distribution and reproduction in any means provided the original authors and original publisher are properly credited. (Please see Copyright Policy for more information.) |
|
|