| Table of Contents |  |
|
CASE REPORT
|
| SAPHO syndrome may be treated effectively with combined drug regimens |
| Mehmet Özen1, Umut Kalyoncu1 |
|
1Hacettepe University Faculty of Medicine, Department of Internal Medicine and Rheumatology, Ankara
|
|
doi:10.5348/ijcri-2011-01-14-CR-2
|
|
Address correspondence to: Dr. Mehmet Özen Hacettepe University Faculty of Medicine Department of Internal Medicine E-mail: doktormehmet19@mynet.com |
|
[HTML Abstract]
[PDF Full Text]
|
| How to cite this article: |
| Mehmet Özen, Umut Kalyoncu. SAPHO syndrome may be treated effectively with combined drug regimens - A case report. International Journal of Case Reports and Images 2011;2(1):8-11. |
|
Abstract
|
|
Introduction: Because SAPHO is a rare syndrome, its treatment is controversial. We are presenting a case of a patient with SAPHO Syndrome, who was treated with combined drug regimen. Case Report: A 16-year-old man was admitted to our hospital with hip and back pain for one month. The patient was not able to move his thighs; therefore he could not walk because of pain. He had papullopustular acne on his back and face. Also, the patient had a mild pain on upper chest wall caused by sternoclavicular arthritis. The erytrocyte sedimentation rate was 69 mm/1hrhour and C-reactive protein was 2.8 mg/dl. HLA B27 was positive. Magnetic resonance imaging of the sacroiliac joint revealed a bilateral symmetrical sacroiliitis. Whole body Tc 99m-MDP bone scintigraphy detected bull's head sign. A diagnosis of SAPHO syndrome was made. The patient was treated with NASIDs, isotretinoin, sulphasalasine, methotrexate, hydroxy-chloroquine and methylprednisolone. Two weeks later, his pain was relieved. Two years later he is still on complete remission. Conclusion: SAPHO syndrome may be treated with combined drug regimen to obtain complete remission and relieve pain. | |
|
Key Words:
SAPHO, Remission, Sulphasalasine, Methotrexate, Hydroxychloroquine
| |
|
Introduction
| ||||||
|
SAPHO Syndrome, which has different skin changes and osteoarticular inflammation, is an acronym that stands for Synovitis, Acne, Pustulosis, Hyperostosis and Osteitis.[1] It was described by Chamot et. al. in 1987.[1] Etiopathogenesis of SAPHO is not clear.[2] Infectious and postinfectious theories were considered and it was reported that Propionobacterium Acne could be related with SAPHO Syndrome.[3] But investigations of most of the cases regarding Propionobacterium Acne were negative and generally patients do not respond to antibiotic therapy.[4] Diagnosis of SAPHO Syndrome is more often based of clinical findings. Although many diagnostic criteria for SAPHO Syndrome have been published, there are no acceptable diagnosis criteria. Diagnostic criteria for SAPHO syndrome were suggested for the first time by Benhamou et. al.[5] Kahn et. al. updated these criteria in 2003 at the 67th annual scientific meeting of American College of Rheumatology. Suggested inclusion criteria are; a) bone and/or joint involvement associated with palmoplantar pustulosis and pustular psoriasis, b) bone and/or joint involvement associated with severe acne, c) in adults isolated sterile hyperostosis/osteitis, d) in children chronic recurrent multifocal osteomyelitis and, e) bone and/or joint involvement associated with chronic bowel diseases. Exclusion criteria are: a) infectious osteitis, b) tumoral conditions of bone and, c) non-inflammatory condensing lesions of bone. [6] Natural history of disease includes multiple osteoarticular involvement and periodic exacerbations and remissions. Any pathogen/microorganism has not been isolated in the effected regions.[2] [5] Prevalence of SAPHO syndrome is not known completely because it is a new concept and has mixed clinical findings. It is estimated that its prevalence is not more than 1/10000. Published reports of SAPHO syndrome are generally from France, Germany, Japan, Australia and Scandinavian countries.[2] [5] SAPHO Syndrome can be seen in all ages, but it is more frequent in children and young adults.[5] We are presenting a case of a patient with hip pain and skin lesions who was diagnosed as SAPHO syndrome and treated with combined drug regimen. The time period from starting the treatment to relieving of pains was only two weeks and his remission has continued for two year. | ||||||
|
Case Report
| ||||||
|
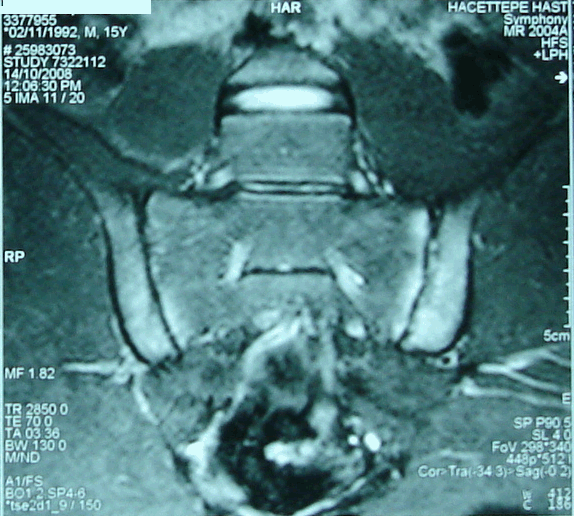
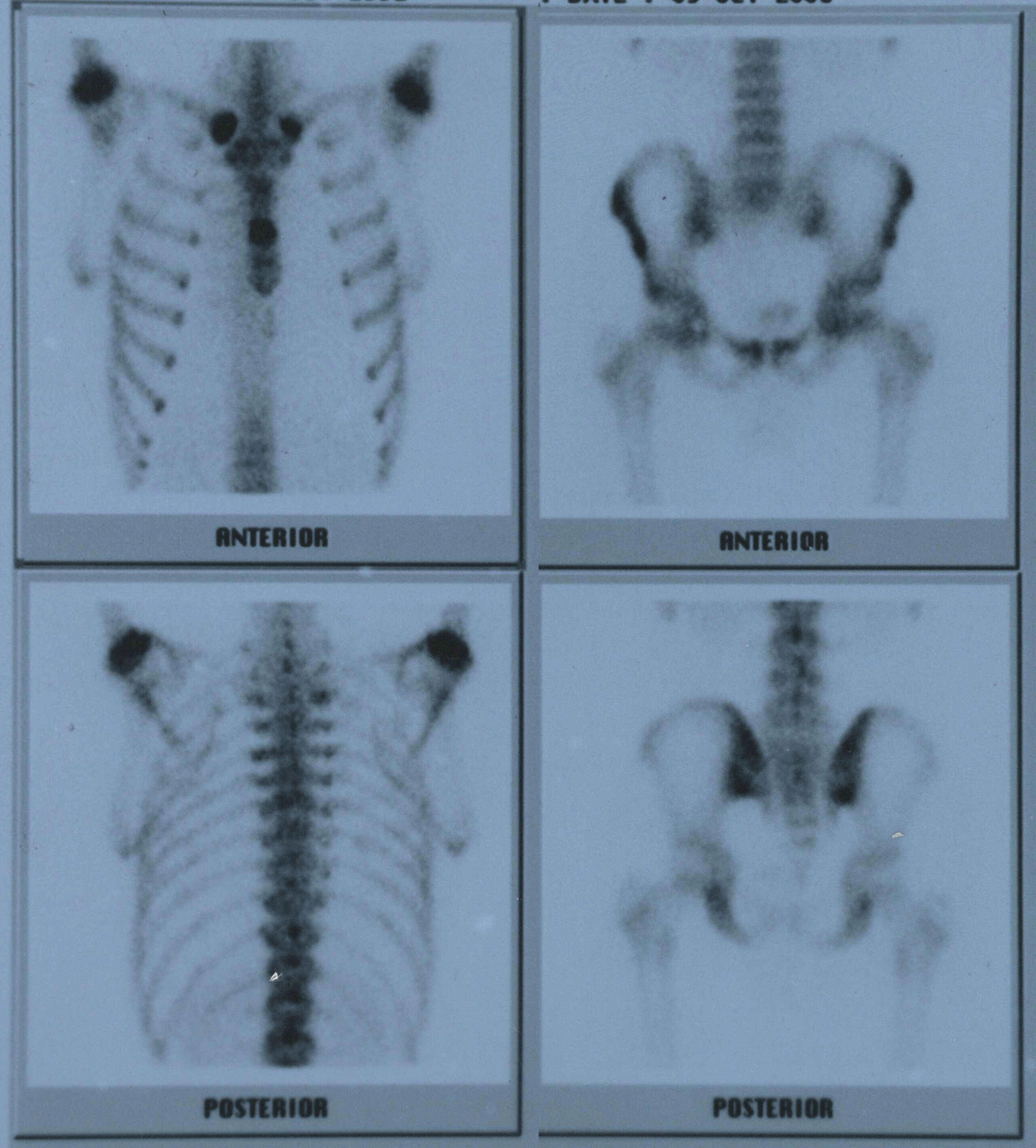
A previously healthy 16-years-old man, who was a student and not working in any job, was admitted to our hospital with bilateral hip and back pain, difficulty in walking and multiple acnes on his back, face and chest (Figure 1). His hip and back pain had started three months ago. Because of acne and pustule formations on his back, face and chest he had been treated with retinoic acid. However, his skin changes had not completely resolved with treatment. On physical examination bilateral painful hip joints and stiffness were present. Tenderness was seen in hip joints and costochondral joints. Pustule and acne in different size and shape were seen in his back. Other physical findings and vital signs including body temperature were normal. Liver and renal function tests were normal. The erythrocyte sedimentation rate (ESR) and C- reactive protein (CRP) were 69 mm/1sthour (range 0-20) and 2.8 mg/dl (range 0-0.8), respectively. HLA B27 level was positive. To exclude septic arthritis Magnetic Resonance Imaging (MRI) of the sacroiliac joint was performed which revealed bilateral, symmetrical sacroiliitis as a possible inflammatory arthritis but no findings associated with septic arthritis (Figure 2). So, SAPHO Syndrome was considered and to diagnose whole body Tc 99m-MDP bone scintigraphy was studied which showed increased uptake on chest wall, corpus sterni and bilateral sternoclavicular joints. This is known as "bull's head" or "bull-horn" sign and is characteristic for SAPHO [7] [8] (Figure 3). As a result, a diagnosis of SAPHO Syndrome was made. Nonsteroidal anti-inflammatory drugs (NSAIDs) were started for his pain relief. For skin lesions retinoic acid treatment was continued and 15mg/day methylprednisolone treatment was added. For the treatment of joint lesions the patient was treated with 2 gm/day sulphasalasine, 15 mg/week oral methotrexate and 200 mg/day hydroxychloroquine. Two weeks later NSAIDs and one month later slowly methylprednisolone were discontinued. Two weeks later, his pain was relieved. Retinoic acid and hydroxychloroquine were continued for one year and then stopped. At the end of two years follow-up he is still on completed remission and sulphasalasine and oral methotrexate treatments are being continued in decreased doses. | ||||||
| ||||||
| ||||||
| ||||||
|
Discussion | ||||||
|
In this case report, we presented a case with typical SAPHO syndrome, which was successfully treated with combined Disease-Modifying Anti-Rheumatic Drugs (DMARDs). Unfortunately, there are no validated diagnostic criteria designed specifically for SAPHO syndrome. Affected patients may fail to meet classification criteria for SpA or psoriatic arthritis. However, most of the authors have classified SAPHO syndrome as a spondylarthropathy (SpA), because of musculoskeletal manifestations in patients.[9] In fact, the treatment of SAPHO Syndrome is controversial because it is a new clinical entity with unclear etiopathogenesis and inadequate clinical studies. NSAIDs, antibiotics, steroids, sulfasalazine, methotrexate, ciclosporin, leflunomide, calcitonin, bisphosphonates, and other drugs are used in SAPHO syndrome treatment.[10] However, relapse or complete remission failure can be seen in some patient, so SAPHO's treatment still continues as a dilemma. Inspite; uncertain clinical efficacy of Tumor Necrosis Factor (TNF) alpha blockers, they are also considered as an alternative treatment modality for refractory SAPHO syndrome.[11] We consider that, TNF alfa blocker treatment can be accepted as an expensive regimen for SAPHO. Our patient was not a refractory case so we did not start this regimen. Over the last few years, intravenous pamidronate treatment is used with marked efficacy on chronic active osteitis. But, with bisphosphonates treatment, pain continues for more than three months.[12] Our aim in this patient was to relieve pain, prevent relapse and ensure complete remission. So, we started NSAIDs and methylprednisolone for his pain and it was relieved in two weeks. At this point, we want to state that, especially at the beginning of the treatment, to relieve pain, NSAIDs should be considered in the management of SAPHO Syndrome. Also, we know that sulfasalazine and methotrexate might be considered in management of SAPHO as these drugs improve remission in SAPHO.[10] [13] [14] [15] On the other hand combined DMARDs therapy are an alternative treatment and methotrexate, sulphasalazine and hydroxychloroquine combination therapy can be used effectively in SpA.[16] So, we treated the patient like a case, which has a SpA or a rheumatoid arthritis and to gain complete remission we added sulphasalasine, oral methotrexate and hydroxychloroquine to treatment. As a summary, the patient has been under observation for two years from diagnosis. Although, this follow-up time can be thought of as short, although doses decreased over this time, we observed complete remission and no relapse in this time period. | ||||||
|
Conclusion
| ||||||
|
SAPHO syndrome can be treated with combined drug regimes like rheumatoid arthritis. Our aim in the management of SAPHO Syndrome should be to obtain complete remission and relieve pain as soon as possible. To represent combined treatment's affectivity, adequacy and safety, more clinical studies should are needed. | ||||||
|
References
| ||||||
| ||||||
| [HTML Abstract] [PDF Full Text] |
|
Author Contributions:
Mehmet Özen - Conception and design, Acquisition of data, Analysis and interpretation of data, Drafting the article, Critical revision of the article, Final approval of the version to be published Umut Kalyoncu - Conception and design, Acquisition of data, Analysis and interpretation of data, Drafting the article, Critical revision of the article, Final approval of the version to be published |
|
Guarantor of submission:
The corresponding author is the guarantor of submission. |
|
Source of support:
None |
|
Conflict of interest:
The author(s) declare no conflict of interests. |
|
Copyright:
© Mehmet Özen et. al. 2011; This article is distributed the terms of Creative Commons Attribution License which permits unrestricted use, distribution and reproduction in any means provided the original authors and original publisher are properly credited. (Please see Copyright Policy for more information.) |
|
|