|
 |
|
Case Report
| ||||||
| Morel–Lavallée lesions: A rare cause of post-traumatic lower back and hip pain | ||||||
| Yuzeng Shen | ||||||
|
Associate Consultant, Department of Emergency Medicine, Singapore General Hospital, Singapore
| ||||||
| ||||||
|
[HTML Abstract]
[PDF Full Text]
[Print This Article] [Similar article in Pumed] [Similar article in Google Scholar] 
|
| How to cite this article |
| Shen Y. Morel–Lavallée lesions: A rare cause of post-traumatic lower back and hip pain. Int J Case Rep Images 2017;8(8):545–548. |
|
ABSTRACT
| ||||||
|
Introduction:
Lower back and hip pain after falling is one of the common presenting complaints at the emergency department. Keywords: Closed degloving injury, Morel–Lavallée lesion, Soft tissue injury, Trauma | ||||||
|
INTRODUCTION
| ||||||
|
Lower back and hip pain after falling is one of the common presenting complaints at the emergency department. The initial investigation of choice, depending on clinical history and physical examination findings, is the plain X-ray to rule out fractures and dislocations. Patients with unremarkable X-rays often have contusions or muscular-ligamentous sprains and strains, which respond well to analgesia and rest. In patients with persistently significant pain, advanced imaging is often performed to identify pathology not well seen on plain X-rays. Morel–Lavallée lesions are associated with trauma and shearing injury, leading to a closed degloving injury where the inter-fascial planes between subcutaneous tissue and underlying fascia is separated. The underlying pre-fascial space may subsequently be filled with blood, lymph or serous fluid [1][2]. We present a case of traumatic lower back and hip pain due to Morel–Lavallée lesions. | ||||||
|
CASE REPORT
| ||||||
|
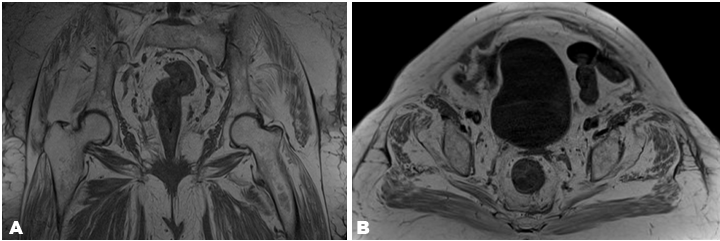
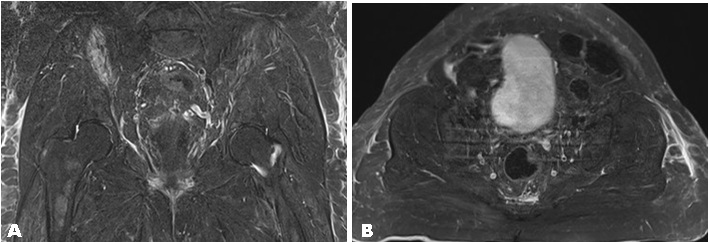
An 80-year-old female presented to the emergency department after sustaining a fall in the bathroom. The patient is currently taking an anti-platelet agent (clopidogrel) for presumptive ischemic heart disease. She slipped and fell off the toilet seat on the day prior to her emergency department visit, and landed on her hips. Since then, she complained of persistent lower back and right hip pain. Vital signs at the patient are as follows: temperature 36.2°C, pulse rate of 83 beats per minute, respiratory rate at 18 breaths per minute, blood pressure 120/57 mmHg, pulse oximetry 96% on room air, and pain score of 8/10. On physical examination, significant findings were that of midline tenderness over the lumbosacral spine, and pain on internal and external rotation of right hip. X-rays of the lumbar spine, pelvis and right hip did not show any obvious displaced fracture. Patient was admitted to the orthopedics department for further observation and workup in view of persistent lower back and right hip pain despite trial of observation and analgesia at the emergency department. Subsequently, inpatient magnetic resonance imaging of the pelvis and bilateral hips showed pre-fascial fluid at the lateral aspect of bilateral hips and posteriorly at the level of the lumbosacral junction, suggestive of Morel–Lavallée lesions. All identified Morel–Lavallée lesions were small (Figure 1) and (Figure 2). The right hip Morel–Lavallée lesion had a maximum width of 2.5 mm, and the left hip Morel–Lavallée lesion had a maximum width of 5 mm. Both collections above extend along the entire lateral aspect of the bilateral gluteus maximus. The third Morel–Lavallée lesion was superficial to the erector spinae muscles and extended from the level of the lumbosacral joint proximally with a maximum depth of 3.7 mm. The patient was managed conservatively with oral paracetamol and oral tramadol tablets for analgesia. She did not undergo surgery or aspiration for the Morel–Lavallée lesions and was discharged after symptoms improved during her stay in hospital. No intervention was performed due to minimal depth of the identified Morel–Lavallée lesions. The patient was a tourist who wished to return to her home country for further review. Due to her continuing management within her home country, further follow-up regarding her progress was not possible. | ||||||
| ||||||
| ||||||
|
DISCUSSION
| ||||||
|
Morel–Lavallée lesions, also known as closed degloving injury of the soft tissue, are rare and are usually due to shearing injury and disruption between subcutaneous tissue and the underlying fascia. Less commonly, it may present as a post-surgical complication, especially associated with liposuction. The space created when subcutaneous tissue separates from the underlying fascia may subsequently be filled with blood, lymph or serous fluid [1]. The patient being on an anti-platelet agent may have contributed to increased bleeding risk and hematoma formation within the resultant space. Common sites of injury include the greater trochanter and proximal thigh [3]. Possible mimics include hemorrhagic bursitis and soft tissue neoplasms. Advanced imaging with MRI is the investigation of choice for diagnosis [1]. Point of care ultrasound has been shown to be a useful and quick alternative in diagnosing Morel–Lavallée lesions [4]. Like this case, Morel–Lavallée lesions are commonly missed during initial evaluation [5], and may present with persistent pain and/or swelling despite rest and analgesia. They can be managed conservatively with compression therapy, physiotherapy, bed rest, or surgical aspiration, drainage or debridement [1][6][2]. Left untreated, complications include infection, expanding lesion and tissue necrosis due to mass effect. There are no large studies providing quality evidence with regards to the management of Morel–Lavallée lesions. In a systemic review of 21 articles detailing 153 patients with Morel–Lavallée lesions of the peripelvic region [7], it was found that surgical intervention was better than conservative management. However, most articles within the systemic review were deemed as Level IV studies. Nickerson et al. shared the creation of a practice management guideline for Morel–Lavallée lesions at the Mayo clinic [8], based on 79 patients with Morel–Lavallée lesions. The study recommended that aspiration of more than 50 ml of fluid from a Morel–Lavallée lesion would prompt surgical intervention, due to a higher rate of recurrence (83% vs 33% when less than 50 ml of fluid was aspirated). Patients can otherwise be conservatively managed with compression and observation. However, it was also mentioned that the study was limited to Level IV evidence, and would require further evaluation in the future. | ||||||
|
CONCLUSION
| ||||||
|
This case report highlights a rare cause of post traumatic lower back and hip pain. Ultrasound evaluation is a useful investigation at the emergency department to identify Morel–Lavallée lesions, which may respond well to conservative nonoperative management. It should be considered as a differential diagnosis for patients with persistent pain despite unremarkable plain X-rays done during initial evaluation at the emergency department. | ||||||
|
REFERENCES
| ||||||
| ||||||
|
[HTML Abstract]
[PDF Full Text]
|
|
Author Contributions
Yuzeng Shen – Substantial contributions to conception and design, Acquisition of data, Analysis and interpretation of data, Drafting the article, Revising it critically for important intellectual content, Final approval of the version to be published |
|
Guarantor
The corresponding author is the guarantor of submission. |
|
Source of support
None |
|
Conflict of interest
Authors declare no conflict of interest. |
|
Copyright
© 2017 Yuzeng Shen. This article is distributed under the terms of Creative Commons Attribution License which permits unrestricted use, distribution and reproduction in any medium provided the original author(s) and original publisher are properly credited. Please see the copyright policy on the journal website for more information. |
|
|