|
 |
|
Case Report
| ||||||
| Immunosuppression and infectious complications: A hemorrhagic dilemma | ||||||
| Isabelle Malhamé1, Amanda Farag2, Zu-hua Gao3, Alan Barkun2,4 | ||||||
|
1MD, Department of Internal Medicine, McGill University Health Center 2MD, Division of Gastroenterology, McGill University Health Center 3MD, Department of Pathology, McGill University Health Center 4MD, Clinical Epidemiology, McGill University Health Center | ||||||
| ||||||
|
[HTML Abstract]
[PDF Full Text]
[Print This Article] [Similar article in Pumed] [Similar article in Google Scholar] 
|
| How to cite this article |
| Malhamé I, Farag A, Gao Z, Barkun A. Immunosuppression and infectious complications: A hemorrhagic dilemma. Int J Case Rep Images 2017;8(8):541–544. |
|
ABSTRACT
| ||||||
|
Introduction:
Patients treated with immunosuppressive agents for autoimmune diseases are a unique patient population. Simultaneous management of an underlying autoimmune disease and of an opportunistic infection can present a therapeutic dilemma. Keywords: Cytomegalovirus, Immunosuppression, Vasculitis | ||||||
|
INTRODUCTION
| ||||||
|
Patients treated with immunosuppressive agents for autoimmune diseases affecting the gastrointestinal tract present a unique and complex challenge. When the symptoms of an opportunistic infection are similar to the underlying autoimmune disease, clinical management becomes even more difficult. We believe that our approach to this case may benefit physicians caring for such patients. | ||||||
|
CASE REPORT
| ||||||
|
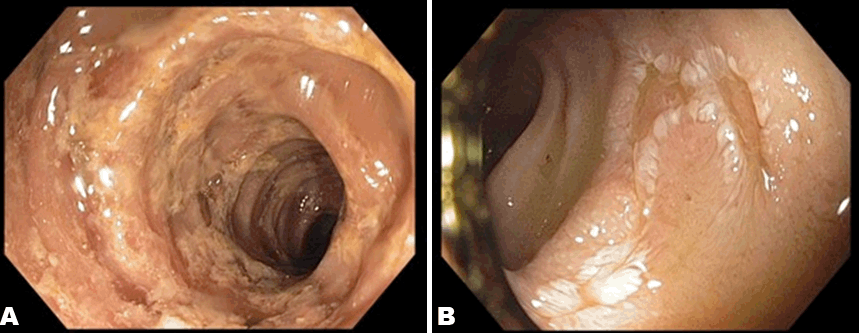
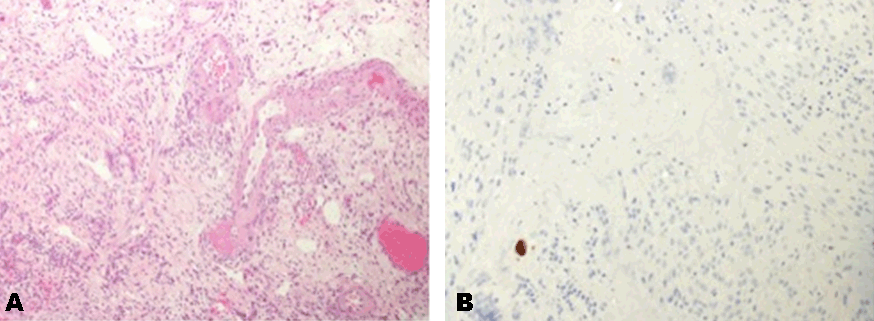
A 68-year-old female presented to the emergency department of a peripheral hospital for fatigue and palpable purpurae. Her past medical history included mild hypertension, hypothyroidism, and diabetes, for which she was taking calcium channel blockers, thyroxine, and an oral anti-hyperglycemic. One week after her initial visit, she developed polyarthritis, melena and bright red blood per rectum. Despite initiation of 60 mg of oral prednisone, her symptoms did not improve and she went on to develop hypoxic respiratory failure. In view of her clinical deterioration, she was transferred to a tertiary care hospital. Upon admission, she had both upper and lower gastrointestinal bleeding symptoms requiring volume resuscitation as well as transfusions. Given the constellation of polyarthritis, palpable purpurae, melena, and possible alveolar hemorrhage, we strongly suspected a vasculitic process with gastrointestinal involvement such as an eosinophilic granulomatosis with polyangiitis (EGPA), granulomatosis with polyangiitis (GPA), microscopic polyangiitis (MPA), polyarteritis nodosa (PAN), and rheumatoid arthritis associated vasculitis (RAAV) [1]. Pertinent laboratory examinations revealed normal platelet count, INR, eosinophil count, immunoglobulin profile, C3-4 levels, as well as negative C-anca, P-anca, anti-GBM, cryoglobulin, lupus anticoagulants, and rheumatoid factor. She also had negative HIV, hepatitis C and B screens. The patient’s bleeding originated from the distal ileum on capsule endoscopy, CT-scan with contrast, and colonoscopy. She also had diffuse mucosal ulcerations throughout the digestive tract (Figure 1). Given the strong suspicion of underlying vasculitis, the treating team initiated a three days course of 1 g of intravenous methylprednisolone daily. Despite the steroid treatment, and two attempts at arterial embolization, the patient continued to pass large amounts of bloody stools. On day-7 of her admission, given the growing risk of bowel ischemia and perforation associated with subsequent arterial embolization, the patient underwent urgent surgical exploration with resection of the involved bowel. Intra-operative endoscopy visualized the entire small bowel lumen with active arterial bleeding and ulcerations in the proximal and terminal ileum. She had a right hemi-colectomy and loop ileostomy with extended resection of the terminal ileum. The biopsy, which resulted on the second week of hospitalization, suggested a polyarteritis nodosa (PAN) involving the ileum and colon with superimposed cytomegalovirus infection (Figure 2). The patient was treated with ganciclovir for her infection and rituximab for PAN as a less aggressive treatment alternative to cyclophosphamide. The bleeding persisted from the ileostomy despite a decreasing cytomegalovirus viremia. Given the active PAN, which was thought to be responsible for the ongoing hemorrhage, a course of cyclophosphamide was initiated. The patient remained in the ICU for one month, during which she developed hospital-acquired infections including repeated bacteremiae with Staphylococcus aureus, and Candida dubliniensis. After a brief resolution of the intestinal hemorrhage, the patient had a recurrence of profuse bleeding through the ileostomy. While a repeat gastroscopy and ileoscopy demonstrated deep ulcerations compatible with ischemia of both duodenum and ileum, an explorative laparotomy did not demonstrate transmural necrosis; resection was therefore not carried out. In view of her overall deteriorating condition despite ongoing therapy, it was decided with the patient’s family to pursue a palliative approach and the patient died on day-70 day of admission. | ||||||
| ||||||
|
| ||||||
|
DISCUSSION
| ||||||
|
Polyarteritis nodosa is a necrotizing, focal segmental vasculitis of medium-sized arteries [1]. The outcome of patients treated for PAN has greatly improved in the last two decades [2]. In this cohort, 37.9% of patients diagnosed with PAN had gastrointestinal involvement, and gastrointestinal manifestations requiring surgery at diagnosis were independent predictors of mortality [2]. Traditionally, hepatitis B has been identified as a possible viral trigger, but infections with cytomegalovirus have also been reported [3][4][5]. In a multi-centric retrospective survey on cytomegalovirus infection among patients hospitalized with autoimmune diseases in Japan, oral prednisone, pulsed methylprednisolone, and cyclophosphamide were most associated with reactivation [6]. Reactivation of cytomegalovirus, whether previously documented or not, should therefore be considered to be a serious potential complication of the mainstay treatment of vasculitis. In the case of our patient, it is reasonable to believe that initial treatment of her vasculitis with prednisone and methylprednisolone precipitated the cytomegalovirus reactivation. Expert opinion on vasculitides in the context of viral infections suggests prompt intravenous antiviral treatment and discourages the use of corticosteroid and/or immune-suppressants for patients who are already immunosuppressed [3]. However, the combination of corticosteroids with cyclophosphamide remains the cornerstone of treatment, and herein lays the dilemma [7]. If we were to solely treat the cytomegalovirus we might be undertreating the vasculitis, which could worsen the patient’s prognosis. Similarly, only treating PAN could provoke more profound immunosuppression and lead to potentially fatal progression of the cytomegalovirus infection. In this context, we treated the PAN and the cytomegalovirus simultaneously and we monitored the clinical activity of the infection via serial measurements of the cytomegalovirus viral load. As the cytomegalovirus viremia was consistent with a resolution of the infection, we believe that uncontrolled PAN was the cause of the persistent hemorrhage. The clinical course of the patient we present is thus characteristic of the rare difficult clinical scenario in which patients with a vasculitis have active cytomegalovirus infection, requiring both antiviral and aggressive immunosuppressive therapies. To the best of our knowledge, there have only been a handful of cases in the literature of active cytomegalovirus infection in the presence of an acute PAN presentation. The four patients described in these reports were treated with corticosteroids and/or antiviral drugs in the absence of any additional immunosuppressant therapy. Mayer et al. describes the effectiveness of less aggressive treatment without immuno-suppressants for ANCA-associated vasculitis with a concomitant viral infection. Unfortunately, recommendations remain lacking in this rare group of patients [4][8]. | ||||||
|
CONCLUSION
| ||||||
|
In conclusion, the patient discussed highlights a unique diagnostic and therapeutic dilemma. The co-existence of active cytomegalovirus infection and severe polyarteritis nodosa resulted in having to choose between possible conflicting therapeutic aims. Clinicians should consider altering standard aggressive combination therapy for the vasculitis while administering antiviral treatment in such patients. | ||||||
|
REFERENCES
| ||||||
| ||||||
|
[HTML Abstract]
[PDF Full Text]
|
|
Author Contributions
Isabelle Malhamé – Substantial contributions to conception and design, Acquisition of data, Analysis and interpretation of data, Drafting the article, Revising it critically for important intellectual content, Final approval of the version to be published Amanda Farag – Substantial contribution to conception and design, Acquisition of data, Analysis and interpretation of data, Drafting the article, Revising it critically for important intellectual content, Final approval of the version to be published Zu-hua Gao – Substantial contribution to acquisition of data, Analysis and interpretation of data, Drafting the article, Revising it critically for important intellectual content, Final approval of the version to be published Alan Barkun – Substantial contribution to conception and design, Acquisition of data, Analysis and interpretation of data, Drafting the article, Revising it critically for important intellectual content, Final approval of the version to be published |
|
Guarantor
The corresponding author is the guarantor of submission. |
|
Source of support
None |
|
Conflict of interest
Authors declare no conflict of interest. |
|
Copyright
© 2017 Isabelle Malhamé et al. This article is distributed under the terms of Creative Commons Attribution License which permits unrestricted use, distribution and reproduction in any medium provided the original author(s) and original publisher are properly credited. Please see the copyright policy on the journal website for more information. |
|
|