|
 |
|
Clinical Image
| ||||||
| Successful treatment of pneumomediastinum in a patient with interstitial lung disease due to anti-synthetase syndrome: A case report | ||||||
| Roy Cho1, Erhan H. Dincer2, Rade Tomic2, Hyun Kim2 | ||||||
|
1Assistant Professor, University of Minnesota, Department of Pulmonary, Allergy, Critical Care and Sleep Medicine
2Associate Professor, University of Minnesota, Department of Pulmonary, Allergy, Critical Care and Sleep Medicine | ||||||
| ||||||
|
[HTML Abstract]
[PDF Full Text]
[Print This Article]
[Similar article in Pumed] [Similar article in Google Scholar] 
|
| How to cite this article |
| Cho R, Dincer EH, Tomic R, Kim H. Successful treatment of pneumomediastinum in a patient with interstitial lung disease due to anti-synthetase syndrome: A case report. Int J Case Rep Images 2017;8(8):564–566. |
|
CASE REPORT
|
|
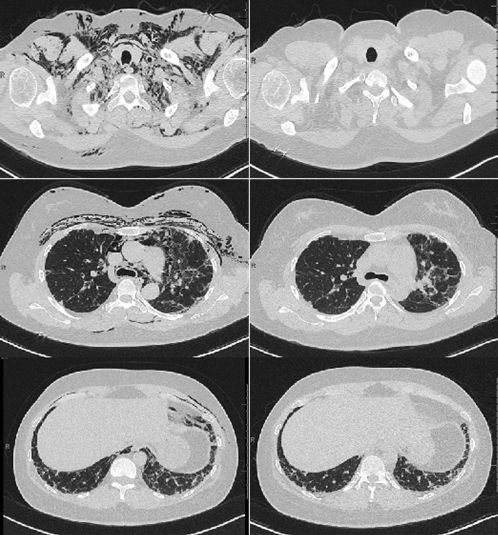
A 35-year-old female with interstitial lung disease due to anti-synthetase syndrome presented with cough, hoarseness and facial swelling. Chest computed tomography scan demonstrated significant pneumomediastinum (Figure 1). Bronchoscopy and esophagram were unremarkable. We began high-concentration oxygen (10 L/min with non-rebreather face mask for 12-hours/day), withheld mycophenolate mofetil, reduced prednisone and began dextromethorphan. After one-month, there was complete resolution of her symptoms and pneumomediastinum. |
|
|
|
DISCUSSION
|
|
Pneumomediastinum (PNM) is a rare complication of anti-synthetase syndrome with only three cases reported since 1986 [1][2][3] . The associated one-month mortality is 25%, which highlights the need for effective management [4]. The management of PNM in interstitial lung disease is based on case reports and experience forming expert opinion. However, the best management requires understanding the pathogenesis [5]. Several mechanisms of PNM in interstitial lung disease have been proposed including the Macklin effect, worsening vasculitis leading to airway rupture, and weakened alveolar walls from immunosuppression [6]. In this case, reducing immunosuppression suggested that weakened alveolar walls was a factor and using high-concentration oxygen and cough suppressant decidedly contributed to the full recovery. Notably, this is the second case in literature that has reported success using high-concentration oxygen for the treatment of PNM [7]. |
|
CONCLUSION
|
|
We report a case of pneumomediastinum in a patient with anti-synthetase syndrome who was successfully treated with reduction in immunosuppression, high-concentration oxygen, and cough suppression. Keywords: Anti-synthetase syndrome, Dermatomyositis, Interstitial lung disease, Pneumomediastinum |
|
REFERENCES
|
|
|
[HTML Abstract]
[PDF Full Text]
|
|
Author Contributions
Roy Cho – Substantial contributions to conception and design, Acquisition of data, Analysis and interpretation of data, Drafting the article, Revising it critically for important intellectual content, Final approval of the version to be published Erhan H. Dincer – Analysis and interpretation of data, Revising it critically for important intellectual content, Final approval of the version to be published Rade Tomic – Analysis and interpretation of data, Revising it critically for important intellectual content, Final approval of the version to be published Hyun Kim – Analysis and interpretation of data, Revising it critically for important intellectual content, Final approval of the version to be published |
|
Guarantor
The corresponding author is the guarantor of submission. |
|
Source of support
None |
|
Conflict of interest
Authors declare no conflict of interest. |
|
Copyright
© 2017 Roy Cho et al. This article is distributed under the terms of Creative Commons Attribution License which permits unrestricted use, distribution and reproduction in any medium provided the original author(s) and original publisher are properly credited. Please see the copyright policy on the journal website for more information. |
|
|