|
 |
|
Case Report
| ||||||
| Condylar osteoma unusual cause of facial asymmetry: A short surgical practice | ||||||
| Saman W. Boskani1, Shakhawan M. Ali2, Nazar A. Amin3, Ali H. Neamat4, Payman Kh. Mahmud5 | ||||||
|
1HDD FICMS, Lecturer, Maxillofacial Department, Sulaimany teaching hospital, Sulaimany, Kurdistan region, Iraq
2BDS HDD KBMS candidate, KBMS trainee, Maxillofacial Department, Sulaimany teaching hospital, Sulaimany, Kurdistan region, Iraq 3BDS MSC KBMS candidate Lecturer, Department of Oral Surgery College of Dentistry, University of Sulaimany, Sulaimany, Kurdistan region, Iraq 4BDS MSC, Implantologist in oral maxillofacial surgery department, Suilamany teaching hospital, Kurdistan region, Iraq 5BDS KBMS candidate, KBMS trainee, Oral medicine Department, Sulaimany teaching hospital, Sulaimany, Kurdistan region, Iraq | ||||||
| ||||||
|
[HTML Abstract]
[PDF Full Text]
[Print This Article] [Similar article in Pumed] [Similar article in Google Scholar] 
|
| How to cite this article |
| Boskani SW, Ali SM, Amin NA, Neamat AH, Kh. Mahmud P. Condylar osteoma unusual cause of facial asymmetry: A short surgical practice. Int J Case Rep Images 2017;8(7):433–438. |
|
ABSTRACT
| ||||||
|
Introduction:
Osteoma is a benign neoplasm resulting from the continuous formation of cortical or cancellous bone. Osteomas of the maxillofacial region mostly occur in the mandible. However, rarely osteomas seen in the mandibular condyle. Keywords: Facial asymmetry, Malocclusion, Mandibular condyle, Osteoma | ||||||
|
INTRODUCTION
| ||||||
|
Osteoma is benign osteogenic lesion composed of both cortical and cancellous bone that increases in size by continuous formation of bone [1]. The pathogenesis of osteoma is unknown. Some authors consider it a hamartoma, while others consider it a true neoplasm [2]. The first reported case of osteoma of condyle was described by Ivy in 1927 [3]. The reactional mechanism, trauma or infection is also suggested as possible causes [4]. Usually, osteoma located in muscle insertions, suggesting that the muscle pulls acts on the development of the lesion. It is possible that minor traumas, which are not even remembered by the patients, may have caused a sub-periosteal hematoma which, associated with the muscle pull, starts the lesion [4]. Really, it is slow growing, asymptomatic, usually solitary lesion, however, osteomas involving the mandibular condyle may result in morphologic and functional disturbances. There are two types of osteomas:
Histologically, osteomas have two distinct variants. One is made up of relatively dense compact bone with scarce medullary tissue, while the other has lamellar or cancellous bone trabeculae with abundant medullary spaces of fibrous-adipose tissue. Osteoblastic activity is usually prominent [6]. The traditional radiographic image is usually enough to diagnose an osteoma. It is presented as a radiopaque mass with a density similar to that of a normal bone. The panoramic X-ray, Waters view or CT scan usually shows the location and the benign nature of the lesion [7]. Osteoma treatment is based on complete surgical removal, on the base, where the bone cortical is located. There are no reports of osteoma malignant transformation [8]. Osteomas recurrence is rare also it believed to be relatively uncommon [2]. | ||||||
|
CASE REPORT
| ||||||
|
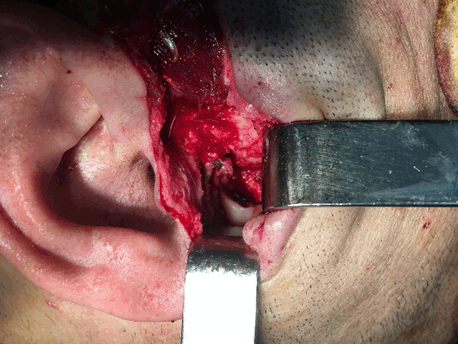
A 33-year-old male patient arrived at the oral and maxillofacial surgery department, with the main complaints of malocclusion and facial asymmetry, he had noted a gradual change in the deviation of the jaw and inability to chew for two years duration. The patient was unable to occlude teeth with painless non-tender swelling on right preauricular region. He had a history of trauma (fall from the bike) during childhood. At the initial examination, extra-orally, asymmetrical facial morphology, the mandible was noted to be deviated to the left, and the median plane of the face was distinctly shifted to the left. On palpation, there was no pain on a temporomandibular joint region and movements of the joint were normal. Intra-oral examination revealed the mandibular central incisors deviated 7–9 mm to the left with respect to the maxillary central incisors (midline was shifted) (Figure 1) but there was no pain associated with mouth opening, and the mandible deviated to the right during the wide opening, the interincisal mouth opening was 35 mm. Based on clinical examination provisional diagnosis given as condylar hyperplasia. Radiographic investigations included OPG, computed tomography 3D and axial view showed a radiopaque osseous mass around the head of the condyle, well-defined pedunculated bony growth was seen on anteromedial aspect of the right condyle. Superiorly extending into left temporomandibular joint space and abutting articular tubercle, which causes dislocation of the condylar head to anterolateral (Figure 2). Tomography Clinical and radiological findings were suggestive of benign tumor of the condyle: osteochondroma, condylar osteoma, chondroblastoma and osteoid osteoma considered for differential diagnosis. While the patient under general anesthesia, the tumor was excised. The upper and lower compartments of the temporomandibular joint were accessed by standard preauricular approach with tragal modification for aesthetic purpose, skin prepared and infiltrated with local anesthesia to make bloodless field, high condylar incision done with preservation of meniscus (Figure 3), after wide opening of the mouth space created to approach the mass which was anteromedial to the condylar head, also mass was dissected and separation from the surrounding tissue mass extracted with a small piece of condylar head (Figure 4) and the specimen obtained was sent for histopathological examination. Based on the histopathological examination, diagnosis as osteoma. Postoperative follow-up the patient occlusion and deviation of jaw return normally with good ability to chewing no any facial palsy (Figure 5). | ||||||
| ||||||
| ||||||
| ||||||
| ||||||
| ||||||
|
DISCUSSION
| ||||||
|
Osteoma of the condyle may cause a slow, progressive shift in the patient’s occlusion with a deviation of the midline of the chin towards the unaffected side. This results in facial asymmetry and temporomandibular joint dysfunction. The most common clinical manifestations involving the condyle are malocclusion and facial asymmetry [9]. The mandible is the common area for osteoma in the maxillofacial region. There are no sex predilection differences in the incidence of occurrence. Osteomas of the condyle are uncommon. Osteoma was first described by Monsarrat in 1913. The first reported case was described by Ivy in 1927 about condylar osteoma [3] . The etiology of osteomas is unclear. It may be developmental, neoplastic or, most likely, reactive in nature [6]. A combination of trauma and muscle traction, which may initiate an osteogenic reaction, has been suggested as the underlying pathogenesis of osteoma [6]. However, may be the possible precipitating cause in this case. Radiographic images show osteomas as circumscribed masses similar in density to normal bone. They are a smooth surface with a thin sclerotic rim at the centers, these masses may exhibit a mixed radiolucent-radiopaque appearance depending on the amount of marrow tissues present. Osteomas can be confused with complex odontomas. Smaller endosteal osteomas are difficult to differentiate from foci of condensing osteitis or focal chronic sclerosing osteomyelitis or idiopathic osteosclerosis [10]. According to the pattern of proliferation, condylar process osteomas can be classified into two types:
In the current case, the osteoma is presented a bilobed structure, one lobe presenting as a pedunculated mass and the other lobe is seen as a replacement of the condyle. Histologically, an osteoma consists of either normal appearing dense mass of lamellar bone with minimal marrow tissue (compact osteoma), or of trabeculae of mature lamellar bone with intervening fatty or fibrous marrow (cancellous osteoma) [11]. A large osteoma resulting in pain, facial asymmetry and malocclusion may require surgical excision (condylectomy) as in the present case, whereas for small, asymptomatic lesions periodic observation is necessary. Recurrence after excision is extremely rare [6]. Up to date, there is only one reported case of recurrence of a periosteal osteoma of the mandible following excision [12]. Furthermore, there are no reports of malignant transformation of osteomas [12]. | ||||||
|
CONCLUSION
| ||||||
|
Osteoma of the mandibular condyle is a benign, rare, bony growth that may cause a painless interference in mouth opening and facial asymmetry. Osteoma should be considered as one of the possible etiologies in a patient with facial asymmetry, malocclusion, deviation of jaw & difficulty in chewing, especially in a patient with the previous history of trauma. Surgery with complete lesion removal is an adequate treatment, with low recurrence rates. | ||||||
|
REFERENCES
| ||||||
| ||||||
|
[HTML Abstract]
[PDF Full Text]
|
|
Acknowledgements
We would like to thank ministry of health Kurdistan regional government and sulaimany teaching hospital for made facility to this operation. |
|
Author Contributions
Saman W. Boskani – Substantial contributions to conception and design, Analysis and interpretation of data, Final approval of the version to be published Shakhawan M. Ali – Substantial contributions to conception and design, Acquisition of data, Analysis and interpretation of data, Drafting the article, Revising it critically for important intellectual content, Final approval of the version to be published Nazar A. Amin – Analysis and interpretation of data, Revising it critically for important intellectual content, Final approval of the version to be published Ali H. Neamat – Analysis and interpretation of data, Revising it critically for important intellectual content, Final approval of the version to be published Payman Kh. Mahmud – Analysis and interpretation of data, Revising it critically for important intellectual content, Final approval of the version to be published |
|
Guarantor
The corresponding author is the guarantor of submission. |
|
Source of support
None |
|
Conflict of interest
Authors declare no conflict of interest. |
|
Copyright
© 2017 Saman W. Boskani et al. This article is distributed under the terms of Creative Commons Attribution License which permits unrestricted use, distribution and reproduction in any medium provided the original author(s) and original publisher are properly credited. Please see the copyright policy on the journal website for more information. |
|
ABOUT THE AUTHORS
| |||||||||||||||
| |||||||||||||||
|
|