|
 |
|
Clinical Image
| ||||||
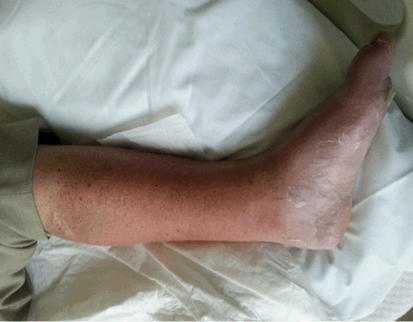
| Lower limb cellulitis associated with ski boot compression trauma | ||||||
| Claire Marie Murphy1, Mark Conal Murphy2 | ||||||
|
1MB, BS, M.R.C.P.(UK), MRCPI., Senior House Officer, General Internal Medicine, St. Vincent’s University Hospital, Elm Park, Elm Park, Merrion Rd, Dublin, D04 T6F4, Ireland 2MB, B.Ch., B.A.O., M.R.C.S.I., Senior House Officer, General surgery, St. Vincent’s University Hospital, Elm Park, Merrion Rd, Dublin, D04 T6F4, Ireland | ||||||
| ||||||
|
[HTML Abstract]
[PDF Full Text]
[Print This Article]
[Similar article in Pumed] [Similar article in Google Scholar] 
|
| How to cite this article |
| Murphy CM, Murphy MC. Lower limb cellulitis associated with ski boot compression trauma. Int J Case Rep Images 2017;8(7):484–486. |
|
CASE REPORT
| ||||||
|
A 77-year-old male was admitted from the emergency department with left lower leg cellulitis failing to respond to oral penicillin V and flucloxacillin. There was no history of previous cellulitis, diabetes, venous disease or surgery to the leg. On physical examination the legs were red, warm to touch, edematous and the skin was intact and very dry. Likely sources of entry were either the dry flaking skin or a small ooze from a problematic in-growing toenail but which on routine culture was negative for pathogens. The C-reactive protein was raised at 165 mg/L as was his white blood cell count 11.7x109/L, (72% neutrophils) but he had no fever. There was no observable lymphadenopathy or tracking lymphangitis. The C-reactive protein settled to 39 mg/L with four days of intravenous flucloxacillin and benzyl penicillin and he was discharged home on oral flucloxacillin after five days. The patient required readmission within 48 hours for worsening symptoms of cellulitis although the C-reactive protein was 29 mg/L, (Figure 1) and (Figure 2). Doppler ultrasound showed no venous thrombosis. Venous duplex scan showed incompetence at the saphenofemoral junction and the great saphenous vein bilaterally and at the saphenopopliteal junction and the small saphenous vein on the right with normal arterial flow and patent deep veins. Antibiotics were changed to clindamycin and vancomycin but clinical improvement was very slow (Figure 3), and although a carrier site screen was negative for methicillin resistant Staphylococcus aureus the antibiotics were escalated to linezolid. He was not known to have diabetes but he had a body mass index of 40 kg/m2, weighed 111 kg and had a high fasting sugar of 8–9 mmol/L with a HbA1c of 46 mmol/mol in keeping with a pre-diabetic state. Magnetic resonance imaging scan revealed edema over the lateral lower leg but no drainable collection. He was discharged 23 days after the initial admission with a C-reactive protein of 17 mg/L and WBC of 8.5x103/L. At follow-up one year later his legs appeared normal on inspection, were not inflamed but on palpation there was a marked temperature difference in a lateral and distal 7x5 cm approximate area just above the ankle joint which was markedly cooler that the rest of the lower legs. Also present was definite edema demonstrated by finger pressure but also restricted to the same cooler lateral area of the calf without any more general or foot edema. Maximum calf diameter was 17 cm. Unusual in the history was a prolonged compression injury to his calves from over tightened ski boots. He said he felt his lower legs were never normal since an event 20 years previously when he had skied all day in pain, without a break, from boots overtightened by an external screw control mechanism. The boot design was contemporary to 20 years ago and semi rear entry with wiring which could be tightened by an external screw control mechanism. The patient described deliberately overtightening the boots in the hope of achieving better ski control and he had persisted skiing despite considerable pain throughout the day. | ||||||
| ||||||
| ||||||
| ||||||
|
DISCUSSION
| ||||||
|
As there was no clinical lymphoedema evident on presentation, other than a general lower leg swelling, lymphoscintigraphy was not performed although it has been shown that lymphatic abnormalities are commonly present in lower leg cellulitis without clinical signs of edema [1]. Conditions that reduce the circulation of blood in the veins or that reduce circulation of the lymphatic fluid (such as venous insufficiency, obesity, pregnancy, or surgeries) may also increase the risk of developing cellulitis, although different studies have given conflicting risk factors [2][3]. Possible risk factors in this patient were obesity, pre-diabetes, superficial venous insufficiency, dry skin, and a slight ooze from an ingrowing toenail. Halpern et al. in a single centre case control study of 150 cases identified local risk factors to be of prime importance rather than systemic risk factors and also identified blunt injury as a significant risk factor. This patient reported a specific and very clearly remembered painful history of compression trauma with consequent residual abnormal signs in this lateral aspect of his lower leg which have never been described. Most ski boots are designed to fit a 13–14 inch calf and this patient had a 17 inch calf which may have predisposed him to tight fitting boots [4]. The importance of good fitting ski boots is better recognized today and the skier with wider calves can now be accommodated with boots with lower cuffs and insoles with a heel lift. Also custom liners can be professionally made for a more personal fit and boots can have upper cuff adjustments to fit a wide calf. Boot top fractures have also been recognized as a risk from overtightened boots and safety release designs but are less common today due to upward as well as rotational binding release design [5] [6]. It is likely this sustained compression trauma permanently damaged the superficial venous/lymphatic system leading to the tendency towards recurrent cellulitis. This presentation may have been more serious on this occasion by a pre-diabetic state which may have further compromised recovery. | ||||||
|
CONCLUSION
| ||||||
|
We believe this case of lower leg cellulitis is the first described to identify a new risk factor for cellulitis with a chronic persistent abnormality attributable to ski boot sustained compression trauma 20 years previously. Keywords: Cellulitis, Lower limb, Ski boot compression trauma, Tight fitting boots | ||||||
|
REFERENCES
| ||||||
| ||||||
|
[HTML Abstract]
[PDF Full Text]
|
|
Author Contributions
Claire Marie Murphy – Acquisition of data, Analysis and interpretation of data, Drafting the article, Revising it critically for important intellectual content, Final approval of the version to be published Mark Conal Murphy – Acquisition of data, Analysis and interpretation of data, Drafting the article, Revising it critically for important intellectual content, Final approval of the version to be published |
|
Guarantor
The corresponding author is the guarantor of submission. |
|
Source of support
None |
|
Conflict of interest
Authors declare no conflict of interest. |
|
Copyright
© 2017 Claire Marie Murphy et al. This article is distributed under the terms of Creative Commons Attribution License which permits unrestricted use, distribution and reproduction in any medium provided the original author(s) and original publisher are properly credited. Please see the copyright policy on the journal website for more information. |
|
|