|
Editorial
| ||||||
| Alloimmunization against Rh and Kell blood groups antigens is the main obstacle for blood transfusion in transfusion dependent thalassemia patients in Iran | ||||||
| Akbar Dorgalaleh1, Mohammad Saeed Gholami1, Mohammad Shokuhiyan1, Mohsen Valikhani1, Esmaei Saneei Moghaddam2, Majid Naderi3 | ||||||
|
1Department of Hematology and Blood Transfusion, School of Allied Medical Sciences, Iran University of Medical Sciences, Tehran, Iran 2Genetic Research Center in Non-Communicable Disease, Zahedan University of Medical sciences, Zahedan, Iran 3Iranian Blood Transfusion Organization Research Center, Zahedan, Iran | ||||||
| ||||||
|
[HTML Abstract]
[PDF Full Text]
[Print This Article] [Similar article in Pumed] [Similar article in Google Scholar] 
|
| How to cite this article |
| Dorgalaleh A, Gholami MS, Shokuhiyan M, Valikhani M, Moghaddam ES, Naderi M. Alloimmunization against Rh and Kell blood groups antigens is the main obstacle for blood transfusion in transfusion dependent thalassemia patients in Iran. Int J Case Rep Images 2017;8(6):358–363. |
| ALLOIMMUNIZATION IN THALASSEMIA MAJOR | ||||||
|
Thalassemia is the most common inherited single-gene disorder, causes by decrease or absence of a-globin or ß-globin chain production. The disorder commonly inherited in autosomal recessive manner and is more common in areas with high rate of consanguinity [1][2][3]. Thalassemia belt is an extensive area which extend from Mediterranean east through Middle-East and India to Southeast Asia and south through Africa. Estimated incidence of thalassemia in this area is varies from 1–20% depend on area. Iran as a Middle-East country with high rate of consanguineous marriage has a considerable number of patients with ß-thalassemia major [4][5][6]. The precise incidence of disorder is not clear in Iran but it was estimated that there are between two and three million beta thalassemia carriers and about 20,000 patients with beta thalassemia major. The main therapeutic choice in these patients is packed red blood cell (pRBC) transfusion. Continuous blood transfusion imposed a number of transfusion related complications, most importantly iron overload and related complications as well as alloimmunization against transfused red blood cell antigens [6] [7] [8][9][10]. The reported rate of alloimmunization among transfused dependent patients with thalassemia varies between 4–50% and has a lower incidence in homologues populations. Some of these alloantibodies are important and even cause severe life-threatening transfusion related hemolytic reactions while others are clinically insignificant. Both of alloantibodies and autoantibodies may decrease survival of transfused pRBC and increase transfusion rate. Such patients may require immunosuppressive drugs, splenectomy as well as other alternative treatments. Therefore, alloimmunization and autoimmunization can significantly affect patients’ quality of life and overall survival [11][12][13]. | ||||||
| ALLOIMMUNIZATION IN THALASSEMIA MAJOR IN IRAN | ||||||
|
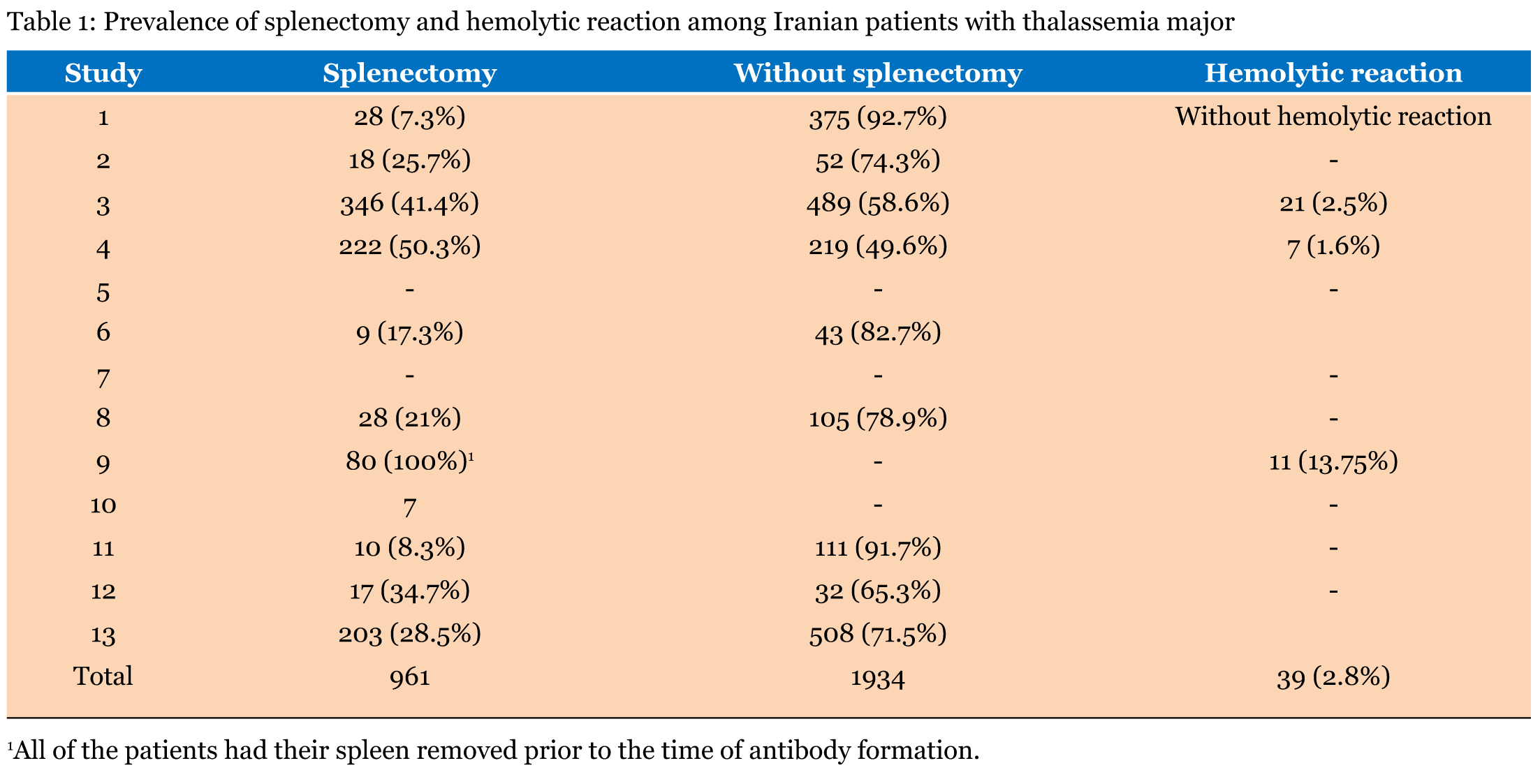
A considerable number of studies were performed in patients with ß-thalassemia major in different areas of Iran. The most common used method for detection of alloimmunization, was conventional tube technique (~80%), while gel method was used in minority (~20%) [5][6][7][8]. In the majority of studies, in addition to alloantibodies, autoantibody (8 out of 13 studies) (61.5%) also were detected [1][3][4][12]. Among these studies, the rate of autoimmunization ranges from 1–~19% [4][9]. The rate of alloimmunization varied between ~3–76%. The lower incidence of alloimmunization was reported in Tehran province, while the highest incidence was observed in Isfahan province [6] [9]. Among alloantibodies the majorities are against Rh and Kell blood group systems. The prevalence of alloantibody against, Rh system ranged from 7.5–100% and this prevalence for Kell system varied from 14–60% [3] . Among these studies on Iranian patients, the rate of splenectomy was reported from ~8–100%. The rate of alloimmunization against these totally splenectomies patients was ~4% (Table 1). In Rh blood group system, most of antibodies directed against, E, C and c antigens respectively, while in Kell blood group system the majority were directed against K antigen (Table 2). | ||||||
| COMPARISON BETWEEN ALLOIMMUNIZATION IN IRAN WITH OTHER COUNTRIES | ||||||
|
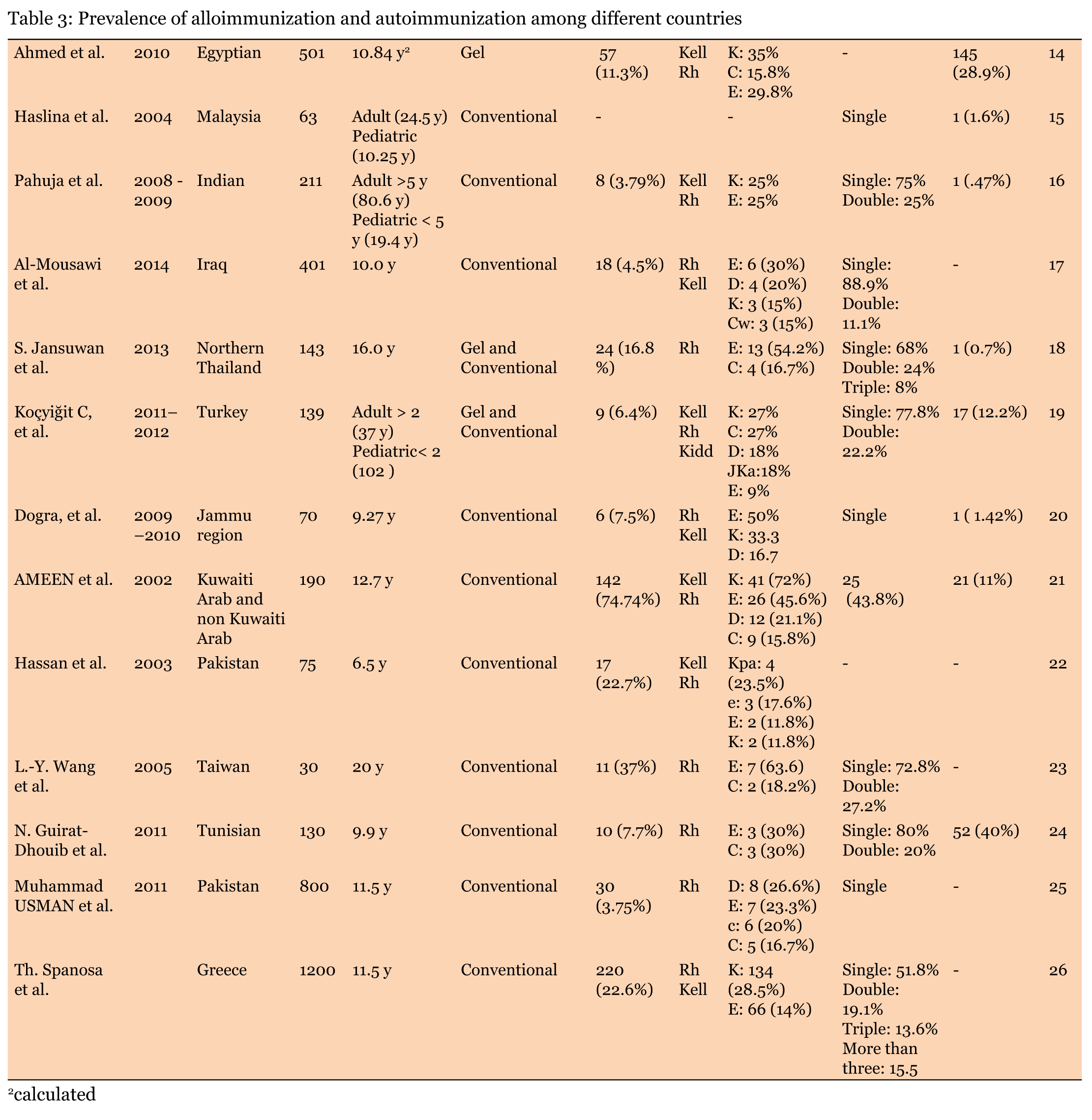
Similar to Iran the most common antibodies against transfused red blood cells were anti-Rh and anti-Kell antibodies in other countries [14] [15][16][17][18][19][20][21][22]. The rate of alloimmunization varies between these countries from ~4% in India and Pakistan to ~75% in Kuwait [16][21][22]. Similar to Iran, conventional tube method is the most commonly used method for antibody detection and identification in other countries [23] [24][25] [26]. Although as low as 0.7% of autoantibody was reported in other countries, most studies reported a significantly higher incidence of autoimmunization in other countries [18][22][23][23][24][25]. In Kell blood group system, the most commonly alloantibodies directed against K antigen [14][18][19][20]. In Rh blood group system, majority of antibody directed against D, E and C antigens (Table 3). With regards to these studies it seems that alloimmunization and even autoimmunization are a major concern in transfusion dependent thalassemia patients [5][7][22]. In Iranian patients with ß-thalassemia major, transfusion related reaction was reported with a prevalence of about 15% in some studies [15][20]. Sometime, in patients with alloimmunization is significant and can have life-threatening consequences. In emergency situations, appropriate blood selection is really difficult and required sophisticated laboratory investigations that only can be performed in specialized laboratories. In addition to this condition, clinically significant alloantibodies and autoantibodies can affect quality of life of these patients and affect overall survival of patients with ß-thalassemia major. To prevent such conditions, its appropriate to use more suitable preventable strategies such as phenotyping of patients prior to beginning blood transfusion and used of relatively complete matched pRBC. Another way to prevent, is application of direct donation instead of random pRBC transfusion that increase the rate of alloimmunization and related consequences. Keywords:Alloimmunization, Blood transfusion, Kell, Rh, ß-thalassemia major | ||||||
| ||||||
| ||||||
| ||||||
|
REFERENCES
| ||||||
| ||||||
|
[HTML Abstract]
[PDF Full Text]
|
|
Acknowledgements
We appreciate all patients with thalassemia that taking part in our researches and improved our knowledge about different aspects of thalassemia. |
|
Author Contributions
Akbar Dorgalaleh – Substantial contributions to conception and design, Acquisition of data, Analysis and interpretation of data, Drafting the article, Revising it critically for important intellectual content, Final approval of the version to be published Mohammad Saeed Gholami – Analysis and interpretation of data, Revising it critically for important intellectual content, Final approval of the version to be published Mohammad Shokuhiyan – Analysis and interpretation of data, Revising it critically for important intellectual content, Final approval of the version to be published Mohsen Valikhani – Analysis and interpretation of data, Revising it critically for important intellectual content, Final approval of the version to be published Esmaei Saneei Moghaddam – Analysis and interpretation of data, Revising it critically for important intellectual content, Final approval of the version to be published Majid Naderi – Analysis and interpretation of data, Revising it critically for important intellectual content, Final approval of the version to be published |
|
Guarantor
The corresponding author is the guarantor of submission. |
|
Source of support
None |
|
Conflict of interest
Authors declare no conflict of interest. |
|
Copyright
© 2017 Akbar Dorgalaleh et al. This article is distributed under the terms of Creative Commons Attribution License which permits unrestricted use, distribution and reproduction in any medium provided the original author(s) and original publisher are properly credited. Please see the copyright policy on the journal website for more information. |
|
|