|
Case Report
| ||||||
| A misdiagnosis of benign abdominal mass as a non-Hodgkin lymphoma | ||||||
| Luma Haj Kassem1, Ahmad Ghazal2, Khawla Mayoh1, Najat Mehio Sailam1 | ||||||
|
1MD, University of Aleppo Faculty of Medicine, Aleppo, Syria
2MD, PhD, Gs, Surgery Department, Aleppo University Hospital, Aleppo, Syria | ||||||
| ||||||
|
[HTML Abstract]
[PDF Full Text]
[Print This Article] [Similar article in Pumed] [Similar article in Google Scholar] 
|
| How to cite this article |
| Kassem LH, Ghazal A, Mayoh K, Sailam NM. A misdiagnosis of benign abdominal mass as a non-Hodgkin lymphoma. Int J Case Rep Images 2017;8(6):397–401. |
|
ABSTRACT
| ||||||
|
Introduction:
Vascular transformation of sinuses (VTS) is a rare reactive process. The lymph node sinuses got converted into a complex anastomosing network of vascular channels. Keywords: Lymph node, Lymphoma, Misdiagnosis, Vascular transformation | ||||||
|
INTRODUCTION
| ||||||
|
Vascular transformation of sinuses (VTS) is a rare condition in which the lymph node sinuses are characterized by vascular proliferations. In this condition, capsule, parenchyma and perinodal fibroadipose tissues are not involved [1][2]. It is often found incidentally in surgical specimens of lymph nodes, but it can also be present as lymphadenopathy [3]. Vascular transformation of sinuses (VTS) has variant histological features such as vasodilation with minimal changes and vascular proliferations, which resemble Kaposi’s sarcoma [4][5]. These histological features, result of the duration of regional lymphatic and/or venous obstruction [3][5][6]. We report a unique case of VTS in a healthy young female, who complained only of abdominal pain. She was misdiagnosed as a non-Hodgkin lymphoma and administered with chemotherapy before performing an excisional biopsy. To our knowledge, the case described here may be the first case to be reported about VTS in a child in literature. | ||||||
|
CASE REPORT
| ||||||
|
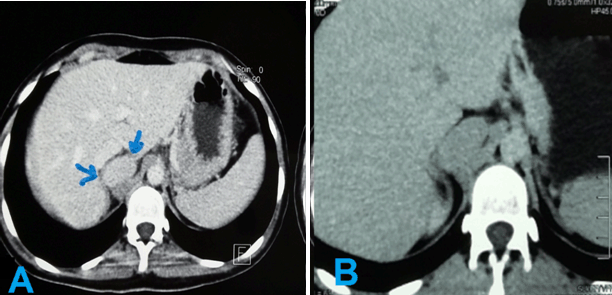
A 13-year-old female presented to the hospital complaining of intermittent, moderate and vague abdominal pain for several months. The pain has a sudden onset, without any radiation or relieving /exacerbating factors. She denied any fever, vomiting, nausea or weight loss. Her medical and family history was unremarkable. Her vital signs were completely normal. On physical examination, there were not any visceral enlargements or masses, any axillary or inguinal lymph nodes could be palpated; there were not any positive findings. All laboratory tests were almost normal except of erythrocyte sedimentation rate (ESR) which was raised 1st hour 25 mm. An abdominal ultrasound was performed and showed a 4.5x3 cm mass (Figure 1), which was confirmed on abdominal computed tomography (CT) scan. Abdominal pelvic multi slice CT scan before and after contrast in sagittal and coronal sections demonstrated that the mass was retro caval adjacent to the right adrenal gland (Figure 2) (Figure 3) (Figure 4). The mass was oval, well defined, homogeneous without fatty components and no calcification or necrosis. The mass was high density (35 HU) before contrast and clearly homogeneously enhancing mass in arterial time. Fine needle aspiration (FNA) was performed and the specimen revealed proliferation of lymphoid cells, part of them were small and had indistinct cytoplasm, round and inconspicuous nuclei. The FNA was followed by immune chemical stains, which revealed positivity for CD3; as a result, it was diagnosed as T cell lymphoma. Unfortunately, the FNA slides are not available. Our patient underwent a chemical course with (CHOP) for five months; her pain improved. On follow-up, ultrasound and CT demonstrated no change of the mass. Unfortunately, after a year, our patient reported that her pain had recurred; the clinician decided that it is a recurrence of lymphoma, so another course of chemotherapy was determined. Nevertheless, the patient and her parents refused it because she was unable to tolerate the side effects of chemotherapy and they requested a consultation of another clinician, who reviewed the whole case and suspected the diagnosis. Therefore, the decision was taken to perform an excisional biopsy of the mass. The pathology revealed vascular transformation of the lymph node with no malignancy (Figure 5). The patient tolerated the procedure well and had uneventful course. At the time of writing, our patient is 22-year-old. She has been completely healthy. | ||||||
| ||||||
| ||||||
|
| ||||||
|
| ||||||
|
| ||||||
|
DISCUSSION
| ||||||
|
Vascular transformation of sinuses (VTS) is a reactive process. The sinuses of lymph node were converted into a complex anastomosing network of vascular channels, which vary from capillaries to cavernous spaces [1][3][5][6] [7] . Haferkamp et al. used the term vascular transformation of sinuses (VTS) in 1971 for the first time. He described the sinuses of lymph node, which resembled blood capillaries [1][2][5][7] . Most of the VTS cases were diagnosed incidentally in excised lymph nodes during a variety of surgical procedures mostly for neoplastic lesions [1][3] [4] . VTS can occur in any age group regardless of sex and in lymph nodes of any location [8]. The frequency of VTS may be dependent upon the anatomic location of lymph nodes and determined in part by the mode of nodal blood supply [6]. Intra-abdominal lymph nodes are the most common to be affected by VTS, cervical being relatively rare [1] [2][8].Vascular thrombosis, severe congestive heart failure, constrictive pericarditis and previous operation or radiotherapy may also contribute to the pathogenesis of this condition[8]. The unique aspects of our case are: First, on review of literature, most of case reports have described VTS in adult patients, whereas we report a unique case of VTS in a child. Secondly, it is known that the majority of VTS cases, which were reported, associated with neoplasia, in contrast to our patient who had VTS without any apparent cause or cancer. Treatment is not indicated, but when vascular transformation is found, a search for occult cancer causing lymph node obstruction is warranted [2][3][5]. In 1995, Cook et al. reported 18 cases of VTS. In 15 of these cases, the lesion was identified in retroperitoneal lymph nodes which were removed as part of radical nephrectomies for renal cell carcinoma, all of the tumors were high histologic grade, and one case was exhibiting sarcomatoid features. In these cases, there seems to be a pathogenetic relationship between the two entities, the changes in the lymph nodes probably are representing a reaction to the renal carcinoma. Renal cell carcinomas are known for their rich vasculature. It is thought that it is due to the production of angiogenic factors by the tumor cells. Theoretically, these angiogenic factors could drain into the regional lymph nodes and elicit the changes of VTS [9]. Thirdly, of rather interest of this case is the misdiagnosing followed by mismanagement. When we seriously doubt of non-Hodgkin lymphoma, there are many topics which must be considered before making decision of chemotherapy. These topics include the best type of biopsy for diagnosis, genetic testing, the role of fluorodeoxyglucose (FDG) positron emission tomography (PET) computed tomography (CT) scan in staging, patient information needs and survivorship but biopsy is an essential one. According to NICE guideline (National Institute for health and Care Excellence), it is considered that an excision biopsy as the first diagnostic procedure for people with suspected non-Hodgkin lymphoma at first presentation [10]. By contrast, our patient was diagnosed as lymphoma by performing an FNA not by an excisional biopsy; furthermore, she was administered with course of chemotherapy. The reason for not performing an excisional biopsy was the high risk of a surgical procedure which outweighs the potential benefits of an excision biopsy. The retrocaval lymph node and its adjustment to the right adrenal gland need special instruments and experts for excisional biopsy; unfortunately, these instruments were not available in our country at that time. Kaposi’s sarcoma and all vasoproliferative lesions of lymph node can be included in the differential diagnosis of VTS. Reactive vascular proliferations which include proliferation of high endothelial venules such as peripheral T cell lymphoma, Hodgkin’s disease and reactive paracortical hyperplasia are also included [1][2][3] [4][5][7] [8][9]. From histological point of view, the spindle cells of VTS lack well-formed fascicles and are always accompanied by an appreciable number of irregular narrow vascular channels, the cellular areas of VTS display maturation into well-formed vascular channels toward the capsular aspect [1][9]. Important limitations in understanding the misdiagnosis of VTS are the significant time lapse from the diagnosis to reporting of this case and unavailability of the FNA slides. We can interpret the misdiagnosis of this rare condition because VTS is a structural change of lymph node sinuses, which needs a histological assessment to recognize. An FNA procedure provides cytological samples and no microarchitecture of lymph node is visualized. In our case, the FNA cytology sample which was followed by immune chemical stains revealed positivity for CD3 which is restricted to the T cell lineage and occurs virtually throughout T cell differentiation. CD3 is the most sensitive and specific marker of T cell lineage available for the immunophenotyping of lymph proliferative disorders. Consequently, the pathologist considered T cell lymphoma as the main diagnosis [11]. Actually, this is an important aspect of our case; in spite of rarity of VTS, which could be unthinkable; the misunderstanding of lymphoma approach leads to mismanagement of this case; hence, the whole path of this case was changed, which was ended by in giving chemotherapy to a healthy young girl, who suffered all its adverse effects. | ||||||
|
CONCLUSION
| ||||||
|
Nevertheless, vascular transformation of sinuses (VTS) is incidentally found in surgical specimens and often associated with malignancy; doctors should consider VTS in the differential diagnosis especially when the clinical picture of malignancy is incomplete. Misdiagnosis of other conditions could occur when fine needle aspiration is performed instead of excisional biopsy to diagnosis non-Hodgkin lymphoma. | ||||||
|
REFERENCES
| ||||||
| ||||||
|
[HTML Abstract]
[PDF Full Text]
|
|
Acknowledgements
We are thankful to Dr. Mohamed Imad Eddin Mouhandes (MD), Consulting Pathologist, Dr. Rama Faour (MD), University of Aleppo faculty of Medicine, Ms. Manal Mehio Sailam and Ms. Nour Ajam, University of Aleppo, faculty of Arts and Humanities, Aleppo, Syria, for their contribution. |
|
Author Contributions
Luma Haj Kassem – Substantial contributions to conception and design, Acquisition of data, Analysis and interpretation of data, Drafting the article, Revising it critically for important intellectual content, Final approval of the version to be published Ahmad Ghazal – Analysis and interpretation of data, Revising it critically for important intellectual content, Final approval of the version to be published Khawla Mayoh – Substantial contributions to conception and design, Acquisition of data, Analysis and interpretation of data, Drafting the article, Revising it critically for important intellectual content, Final approval of the version to be published Najat Mehio Sailam – Substantial contributions to conception and design, Acquisition of data, Analysis and interpretation of data, Drafting the article, Revising it critically for important intellectual content, Final approval of the version to be published |
|
Guarantor
The corresponding author is the guarantor of submission. |
|
Source of support
None |
|
Conflict of interest
Authors declare no conflict of interest. |
|
Copyright
© 2017 Luma Haj Kassem et al. This article is distributed under the terms of Creative Commons Attribution License which permits unrestricted use, distribution and reproduction in any medium provided the original author(s) and original publisher are properly credited. Please see the copyright policy on the journal website for more information. |
|
|