|
Case Report
| ||||||
| Acute colonic pseudoobstruction (Ogilvie’s syndrome) as a postoperative complication: A case report and literature review | ||||||
| Alaa Sedik1, Mufid Maaly2, Salwa ElHoushy3 | ||||||
|
1,2King Khalid Hospital Hail, KSA, Department
of Surgery
3King Khalid Hospital Hail, KSA Department of Medicine | ||||||
| ||||||
|
[HTML Abstract]
[PDF Full Text]
[Print This Article] [Similar article in Pumed] [Similar article in Google Scholar] 
|
| How to cite this article |
| Sedik A, Maaly M, ElHoushy S. Acute colonic pseudoobstruction (Ogilvie’s syndrome) as a postoperative complication: A case report and literature review. Int J Case Rep Images 2017;8(6):394–396. |
|
ABSTRACT
| ||||||
|
Introduction:
Acute colonic pseudoobstruction, also known as Ogilvie’s syndrome, is an acute clinical condition with clinical and radiological features of an acute large bowel obstruction in the absence of any mechanical cause; yet a medical or surgical predisposing factors are present. Case Report: We describe a middle aged male victim of road traffic accident (RTA), who presented lately with acute colonic pseudoobstruction without any apparent cause following recent lumbar spine surgery for trauma. Conclusion: This case report highlights the rare, but potentially dangerous, diagnosis of Ogilvie’s syndrome after spinal fracture fixation. Rapid diagnosis is the key to avoid serious complications. Keywords: Ogilvie’ syndrome, Spine, Surgery | ||||||
|
INTRODUCTION
| ||||||
|
Acute colonic pseudoobstruction (Ogilvie’s syndrome) is characterized by abdominal distension and massive colonic dilatation without any mechanical cause of obstruction [1]. Ogilvie first described this syndrome in 1948 [2]. The pathogenesis remains unknown but likely involves imbalance between sympathetic and parasympathetic colon innervation [3]. Trauma, sepsis, and intrapelvic, neurosurgical or orthopedic surgery have been reported as etiological factors [4][5]. As regards surgical patients, some have been reported after cervical discectomy [1], after cesarean section [6], after spinal anesthesia, trauma or surgery [4] [5]. And after laparoscopic surgery [6]. We report a case of Ogilvie’s syndrome after lumbar vertebral surgery. The pathophysiology and treatment are discussed based on a review of literature. | ||||||
|
CASE REPORT
| ||||||
|
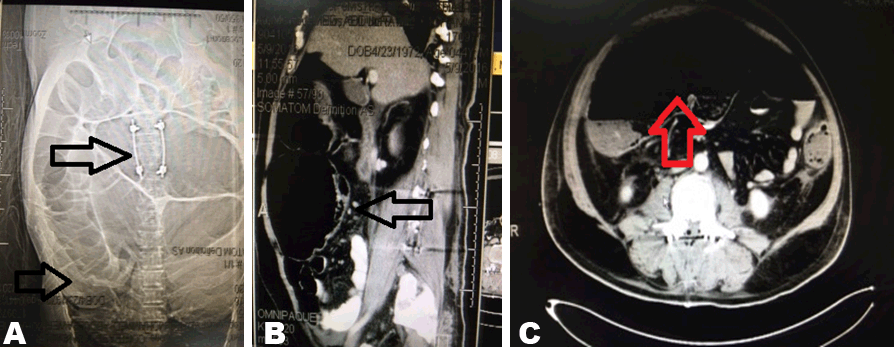
A 44-year-old Egyptian male; not known to have any medical problems before; was admitted as RTA victim. He had recently underwent operative fixation for unstable lumbar spinal fracture five days prior to surgery consultation. He had also a plaster cast applied to a fracture of left ankle. Patient had three-day history of progressive abdominal distension with diffuse pain, nausea and occasional nonbilious non bloody vomiting. Patient did not passed stools or flatus. On general examination, a bedridden obese male having stable vital signs and normal temperature. He was in pain, mildly dehydrated. Locally, the abdomen was diffusely distended with diffuse tenderness maximally over right lower quadrant with rigidity and positive rebound. A tympanic note was noted with sluggish bowel sounds. The rectum was empty. Labworks showed mild leukocytosis with elevated serum creatinine and urea. X-rays of the abdomen showed hugely distended colon. Volvulus then contrast enhanced abdominal and pelvic CT scan confirms the possibility of volvulus of cecum (Figure 1). Resuscitation was started to prepare for surgery and a nasogastric tube was inserted. The situation was fully discussed and informed consent obtained about the need for urgent laparotomy as its late to ask for colonoscopy. Patient was taken to the theatre and the abdomen explored through a long midline incision. Exploration showed intraperitoneal serosanguineous fluid and a hugely distended ischemic right colon up to the right half of the transverse colon with extensive serosal tears and edema of the wall. The cecal diameter exceeded 15 cm. The rest of the colon was distended down the rectum but looked viable. No masses or volvulus were found along the entire colon. The patient was offered right hemicolectomy with right quadrant stoma fashioned (ileostomy and mucus fistula) (Figure 2). The abdomen was closed over a pelvic drain. Postoperatively, he made uneventful recovery and tolerating gradually oral feeding with viable functioning stomas. He was discharged in good condition for possible outpatient department follow-up. | ||||||
| ||||||
|
| ||||||
|
DISCUSSION
| ||||||
|
Colon in the absence of an anatomic or mechanical lesion that obstructs the flow of intestinal contents. This form of adynamic ileus is also named Ogilvie’s syndrome. It carries the name of the British surgeon Sir William Heneage Ogilvie (1887–1971), who first reported it, in 1948 [2]. The most serious complication of Ogilvie’s syndrome is perforation of the cecum. Early recognition and treatment of pseudo-obstruction of the colon may prevent cecal perforation, which reportedly carries a mortality rate of 25–60% [4]. Signs and symptoms resemble those of paralytic ileus. It affects mainly elderly, bedridden patients. The pathogenesis remains unknown but likely involves imbalance between sympathetic and parasympathetic colon innervation [6]. The fact that Ogilvie’s syndrome may occur after manipulation of vertebral structures (spinal anesthesia, lumbar surgery) could support this hypothesis. It is known that the key is early recognition and rapid medical approach is the most appropriate treatment in patients presenting without complications. Medical treatment in the form of nasogastric suction, rectal tubes, keep Nulla per os, correction of fluid and electrolyte imbalance, and parasympathetic agent neostigmine administration if the diagnosis is made early and abdominal radiograph shows a diameter of the distended cecum less than 9 cm [8] [9]. If cecum overdistention occurs, then colonoscopic decompression can be proposed with possible passing a rectal tube [10]. Surgical management is indicated if cecal diameter is greater than 9 cm or conservative treatment is ineffective after or there is evidence of cecal perforation. In absence of perforation or bowel ischemia, cecostomy is the procedure of choice but in cases of bowel ischemia and perforation resection with or without primary anastomosis should be performed [7][11]. The complications of Ogilvie syndrome include perforation, peritonitis and shock. The mortality rates in cases of colonic perforation are 43–50%.In our case, no medical treatment or endoscopic decompression was attempted because the clinical and radiological evidences warranted urgent surgery. | ||||||
|
CONCLUSION
| ||||||
|
Ogilvie’s syndrome is a rare condition and should be differentiated from toxic megacolon where urgent surgery is recommended. Vertebral surgery or trauma probably acts as predisposing factor. Complications following pseudo-obstruction may be avoided if pseudo-obstruction is recognized early and treated with optimal conservative treatment including para-sympathetic drugs. In case of failure of medical treatment or complications, surgery remains the treatment of choice. | ||||||
|
REFERENCES
| ||||||
| ||||||
|
[HTML Abstract]
[PDF Full Text]
|
|
Author Contributions
Alaa Sedik – Substantial contributions to conception and design, Acquisition of data, Analysis and interpretation of data, Drafting the article, Revising it critically for important intellectual content, Final approval of the version to be published Mufid Maaly – Analysis and interpretation of data, Revising it critically for important intellectual content, Final approval of the version to be published Salwa ElHoushy – Analysis and interpretation of data, Revising it critically for important intellectual content, Final approval of the version to be published |
|
Guarantor
The corresponding author is the guarantor of submission. |
|
Source of support
None |
|
Conflict of interest
Authors declare no conflict of interest. |
|
Copyright
© 2017 Alaa Sedik et al. This article is distributed under the terms of Creative Commons Attribution License which permits unrestricted use, distribution and reproduction in any medium provided the original author(s) and original publisher are properly credited. Please see the copyright policy on the journal website for more information. |
|
|