|

|
 |
|
Case Report
| ||||||
| Unusual presentation of adenoid cystic carcinoma: A case report | ||||||
| Bhargavi Dasari1, Ravi Kiran A.2, Kartheeki B.3, Shaik Izaz3, Sudheer Koutha4, Shilpa Guntaka5 | ||||||
|
1Senior Lecturer, KIMS Dental College, Amalapuram, A.P, India, Preceptor, Oral and Maxillofacial Radiology, Rutgers School of Dental Medicine, Newark, New Jersey 2Professor and Head of the Department, Department of Oral Medicine and Radiology, Sibar Institute of Dental Sciences, Thakkellapadu, A.P., India 3M.D.S, Sibar Institute of Dental Sciences, Thakkellapadu, A.P., India 4MPH in Epidemiology and Biostatistics, University of Southern Missisippi, Hattiesburg 5Resident in Oral and Maxillofacial Radiology, Rutgers School of Dental Medicine, Newark, New Jersy | ||||||
| ||||||
|
[HTML Abstract]
[PDF Full Text]
[Print This Article]
[Similar article in Pumed] [Similar article in Google Scholar] 
|
| How to cite this article |
| Dasari B, Kiran RA, Kartheeki B, Izaz S, Koutha S, Guntaka S. Unusual presentation of adenoid cystic carcinoma: A case report. Int J Case Rep Images 2017;8(5):309–312. |
|
ABSTRACT
|
|
Adenoid cystic carcinoma is a slow growing, aggressive malignant tumor. It is an uncommon tumor seen in the palate. This case report presents a patient with adenoid cystic carcinoma in the hard palate with a very unique presentation of the neoplasm. Keywords: Adenoid cystic carcinoma, Hard palate |
|
INTRODUCTION
|
|
Adenoid cystic carcinoma is a rare malignant tumor that accounts only 10% of the salivary gland tumors [1]. In addition to the salivary glands, it affects the lacrimal glands, ceruminous glands and occasionally the excretory glands of the female genital tract. It is known for its long clinical course and plodding growth. It is unique for its local recurrence, late distant metastasis encouraging longer survival rate and spread through perineural lymphatics [2]. This is a case report of a 32-year-old male who presented with a seven-months-old swelling in the palate. |
|
CASE REPORT
|
|
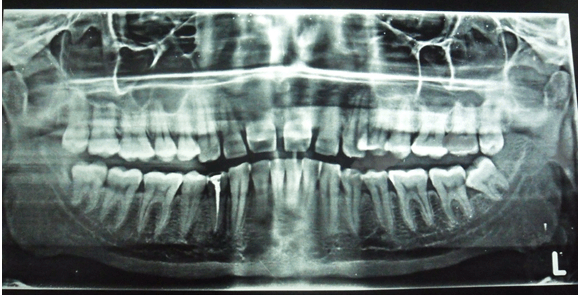
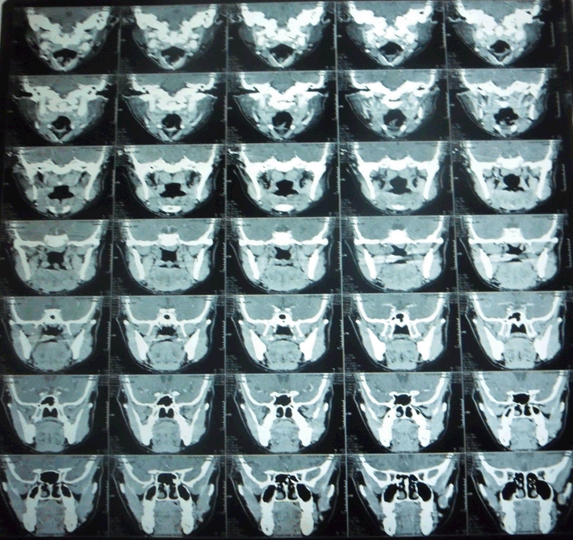
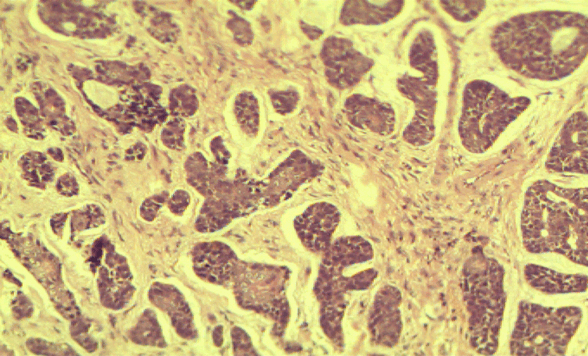
A 32-year-old male came to the emergency department with chief complaint of a growth in the left side of the palate region since seven months. It was initially smaller, gradually increasing in size and attained present size. Patient gave history of pain initially when it was started. Pain was sudden in onset, moderate, dull aching type, intermittent. No specific aggravating and relieving factors. On extraoral examination, solitary submandibular lymph nodes palpable bilaterally of size 0.5x1 cm on right side and 1x1 cm on left side. They were of oval shaped, firm in consistency, freely movable and non-tender. On intra oral hard tissue examination, 44 were restored. On inspection, an ulceroproliferative growth was seen on the left side of the hard palate. It was of oval shaped. It was of size 2x3 cm extending medially from mid-palatal region, laterally up to marginal gingiva, and anteriorly from the rugae region to the junction of hard palate and soft palate posteriorly. Color was whitish at the centre and erythematous at the periphery. On palpation it was tender, rough surfaced. Margins were everted and rolled out. Base was indurated (Figure 1). Based on the history and clinical examination, a provisional diagnosis was given as mucoepidermoid carcinoma. Differential diagnosis was given as adenoid cystic carcinoma, carcinoma involving hard palate and carcinoma involving maxillary sinus. Blood investigations were done in which there was no abnormality except the raise in erythrocyte sedimentation rate. Panoramic radiograph was not suggestive of any pathology near hard palate (Figure 2). Hence, advanced imaging computed tomography scan was advised which revealed area of altered attenuation showing heterogeneous enhancement on contrast. It also revealed soft tissue attenuation of left maxillary sinus (Figure 3). Based on these findings, the radiographic differential diagnosis was as carcinoma involving the hard palate. A soft tissue specimen of size 1.5x1 cm was taken and subjected to histology. 4x view revealed parakeratinized stratified squamous surface epithelium with tumor cells in the fibrocellular connective tissue stroma. 20x view showed aggregates of hyperchromatic tumor cells having scanty cytoplasm with central cystic spaces in the fibrocellular connective tissue stroma (Figure 4). Thus histopathological diagnosis confirmed it as adenoid cystic carcinoma. |
| ||||||
| ||||||
| ||||||
| ||||||
|
DISCUSSION
| ||||||
|
Billroth in 1859 was the first person to describe this infrequent malignant salivary gland tumor adenoid cystic carcinoma (ADCC) under the name cylindroma attributing to its cribriform appearance formed by the tumor cells with cylindrical pseudo spaces. The term ‘adenoid cystic carcinoma’ was instigated by Ewing (Foote and Frazell) in 1954. Adenoid cystic carcinoma (ACC) is an aggressive neoplasm with a phenomenal capacity for recurrence. The most common site for adenoid cystic carcinoma was palate as reported in the present case. It affects both genders equally and is mostly encountered in fourth and fifth decades of life which is not a correlating factor in the present case. Usually, the clinical presentation is asymptomatic growth with a co-presentation of pain and paresthesia at times. It is also described as an aggressive tumor because of the neural and lymphatic spread in other ways. Adenoid cystic carcinoma has a relatively indolent course and rare lymph node metastases but is familiar for its tendency for neurotropic spread and late local recurrences [3] [4]. In a study of 160 patients of adenoid cystic carcinoma by Fordice et al., disease-specific survival was 89% at five years but only 40% at 15 years. Distant metastasis was the most common type of treatment failure (in 22% patients), lungs being the most common site followed by liver [5]. Treatment of adenoid cystic carcinoma includes a complete excision of the local disease followed by post-operative radiotherapy. Radiation therapy used alone has a high rate of local recurrence but may provide useful palliation in inoperable/disseminated disease [5] [6] . | ||||||
|
CONCLUSION
| ||||||
|
As adenoid cystic carcinoma is a slow growing rare malignant tumor, its early detection by the dental specialist aids in favorable prognosis in almost all cases. The role of various diagnostic modalities like biopsy and advanced diagnostic imaging techniques like computed tomography scan has been mentioned in the present case. The therapy involving combination of surgery and radiotherapy remains the modality of choice in most cases. | ||||||
|
REFERENCES
| ||||||
| ||||||
|
[HTML Abstract]
[PDF Full Text]
|
|
Author Contributions
Bhargavi Dasari – Substantial contributions to conception and design, Acquisition of data, Analysis and interpretation of data, Drafting the article, Revising it critically for important intellectual content, Final approval of the version to be published Ravi Kiran A. – Analysis and interpretation of data, Revising it critically for important intellectual content, Final approval of the version to be published Kartheeki B. – Analysis and interpretation of data, Revising it critically for important intellectual content, Final approval of the version to be published Shaik Izaz – Analysis and interpretation of data, Revising it critically for important intellectual content, Final approval of the version to be published Sudheer Koutha – Analysis and interpretation of data, Revising it critically for important intellectual content, Final approval of the version to be published Shilpa Guntaka – Analysis and interpretation of data, Revising it critically for important intellectual content, Final approval of the version to be published |
|
Guarantor
The corresponding author is the guarantor of submission. |
|
Source of support
None |
|
Conflict of interest
Authors declare no conflict of interest. |
|
Copyright
© 2017 Chiranjeev Kumar Gathwal et al. This article is distributed under the terms of Creative Commons Attribution License which permits unrestricted use, distribution and reproduction in any medium provided the original author(s) and original publisher are properly credited. Please see the copyright policy on the journal website for more information. |
|
|
|
About the Author
| |||||||||||||||
| |||||||||||||||
|
|