|

|
 |
|
Letters to the Editor
| ||||||
| Schwannoma of the median nerve | ||||||
| Ingo Schmidt | ||||||
|
SRH Poliklinik Gera GmbH, Straße des Friedens 122, 07548 Gera (Germany)
| ||||||
| ||||||
|
[HTML Abstract]
[PDF Full Text]
[Print This Article]
[Similar article in Pumed] [Similar article in Google Scholar] 
|
| How to cite this article |
| Schmidt I. Schwannoma of the median nerve. Int J Case Rep Images 2017;8(4):290–292. |
| To the Editors, |
|
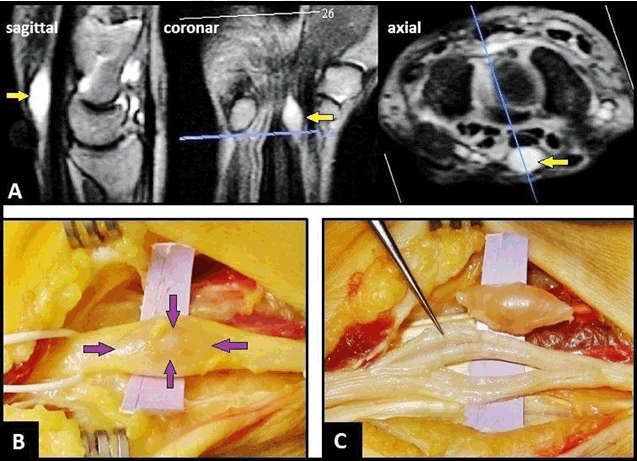
A 57-year-old female presented with a two-year history of increasing painful swelling on the flexor surface in the left distal forearm that was associated with progredient paraesthesias in the peripheral area of the median nerve since six months. On physical examination, a non-tender mass was palpable shortly before entry into carpal tunnel, and the Tinel's sign along the distribution of median nerve upon percussion of the tumor was positive. Magnetic resonance imaging (MRI) scan revealed an oval and strictly demarcated tumor within the median nerve with a hyperintense signal relative to skeletal muscle (Figure 1A). The surgical procedure was done through a palmar incision over the carpal tunnel and extending up to the distal forearm with the use of a tourniquet. After that, the carpal tunnel was released. Intraoperatively, a strictly encapsulated tumor within the median nerve was seen (Figure 1B). The tumor was carefully dissected under microscope, followed by an extracapsular excision of the entire tumor with size of 1.5x0.5 cm. After that, excision-related fascicle lesions were not present (Figure 1C). Histological examination revealed a benign Schwannoma. Six months after surgery, the patient remained neurologically intact. Schwannomas, also known as neurilemmomas, are benign nerve tumors that originate from the cells of the Schwann sheath, and constitute 5% of all benign soft tissue tumors. They are most commonly occur in the head and neck involving the brachial plexus and spinal nerves whereas the upper and lower limbs being affected less often. Schwannomas are the most common benign nerve tumors occurring in the upper extremity, the incidence for appearance in the median nerve is reported to be 14% [1]. They are usually found on the flexor surface of the forearm and hand, and multiple occurrences involving the median and ulnar nerve was observed [2]. Schwannomas of the upper extremity usually occur in patients aged 30–60 years, have no race or sex predilection, usually grow slowly for several years before being diagnosed; and they are sometimes misdiagnosed as lipoma, neurofibroma that grow usually intraneurally with infiltration of the nerve, ganglion or xanthoma [3]. Simple removal of the tumor after careful dissection is recommended if pure sensory deficit is present, because recurrence and/or malignant transformation rate is low [3] [4]. In literature, there is no strict consensus about whether the tumor should become extracapsular excised or intracapsular enucleated to avoid fascicle lesions intraoperatively [5] [6]. Even though there are some radiological features that point to the diagnosis of Schwannoma, ultrasonography and MRI scan cannot predict whether the tumor can be completely enucleated when a portion has fascicular involvement leading to residual neurological deficit after excision [4]. If there is a mixed and/or pure motor nerve involvement preoperatively that was found in 62.5% of patients, a sural nerve graft is recommended in younger patients; whereas it is not recommended since the level of neurological deficit is likely insignificant for the decreased level of activities of daily living in the elderly [4]. Recurrence has been seen in different areas of the nerves, but not in operated sites. |
|
|
|
Keywords: Median nerve, Neurilemmomas, Schwannoma |
|
References
|
|
|
[HTML Abstract]
[PDF Full Text]
|
|
Author Contributions
Ingo Schmidt – Substantial contributions to conception and design, Acquisition of data, Analysis and interpretation of data, Drafting the article, Revising it critically for important intellectual content, Final approval of the version to be published |
|
Guarantor of submission
The corresponding author is the guarantor of submission. |
|
Source of support
None |
|
Conflict of interest
Authors declare no conflict of interest. |
|
Copyright
© 2017 Ingo Schmidt. This article is distributed under the terms of Creative Commons Attribution License which permits unrestricted use, distribution and reproduction in any medium provided the original author(s) and original publisher are properly credited. Please see the copyright policy on the journal website for more information. |
|
|
|
About the Author
| |||
| |||
|
|