|

|
 |
|
Case Report
| ||||||
| Metastatic transitional cell carcinoma to the inguinal lymph nodes from an unknown primary: A case report | ||||||
| Ghassan Almaimani | ||||||
|
MBBS, Resident, Department of Surgery, Main-Kinzig-Clinics, Gelnhausen, Germany
| ||||||
| ||||||
|
[HTML Abstract]
[PDF Full Text]
[Print This Article]
[Similar article in Pumed] [Similar article in Google Scholar] 
|
| How to cite this article |
| Almaimani G. Metastatic transitional cell carcinoma to the inguinal lymph nodes from an unknown primary: A case report. Int J Case Rep Images 2017;8(4):275–278. |
|
Abstract
| ||||||
|
Introduction: The carcinoma of unknown primary (CUP) is uncommon in the inguinal region, accounting for 1–3% of all CUPs. The diagnostic workup for CUP includes histopathological examination, imaging and, more recently, molecular testing. Nevertheless, the primary site frequently remains unknown. Keywords: Carcinoma of unknown primary, Inguinal lymph node, Transitional cell carcinoma | ||||||
|
Introduction
| ||||||
|
The carcinoma of unknown primary (CUP) is an uncommon diagnosis that is offered when diagnostic evaluation fails to identify the primary tumor site. 0.5–4% of all diagnosed cancers are CUPs [1][2]. The CUPs vary in both presentation and histological type, but the most frequent presentation is as metastatic disease. The CUPs rapidly progress in most cases and often show atypical metastatic patterns for the presumed primary origin. The CUP is more common in the head and neck and axillary regions, with inguinal involvement accounting for only 1–3% of cases [3][4]. Extensive workup with comprehensive histopathological evaluation (microscopy, immunohistochemistry, electron microscopy, and molecular testing where appropriate) and modern imaging (computed tomography (CT) scan, mammography, positron-emission tomography (PET)) has improved the diagnosis and identification of the primary site [5], which nevertheless remains elusive in most patients even at autopsy. Thus, the diagnosis and treatment of CUPs still challenge the multidisciplinary cancer team (surgeons, pathologists, and oncologists). | ||||||
|
Case Report
| ||||||
|
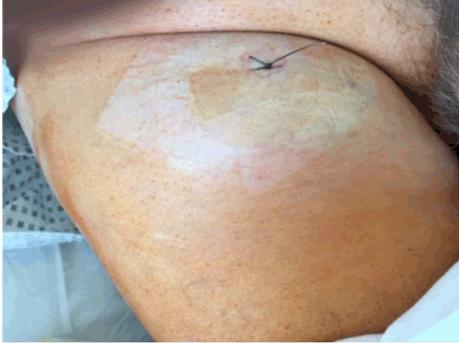
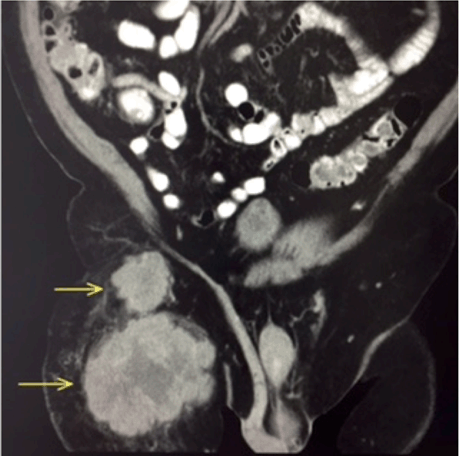
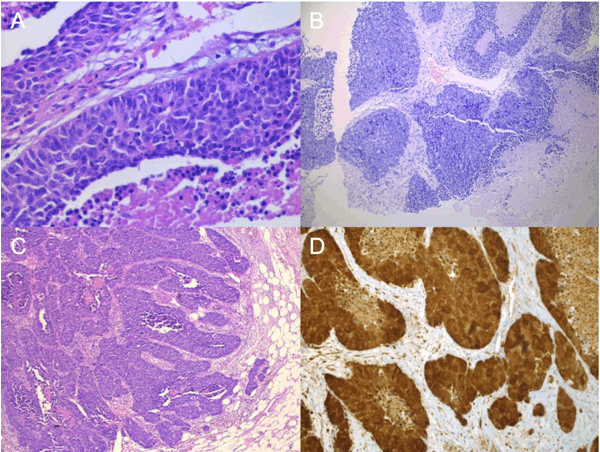
A 78-year-old male was referred for evaluation of a growing painless swelling in the right inguinal region that he had noticed eight weeks previously (Figure 1). He had a past medical history of left ventricular hypertrophy and hypertension. He reported no weight loss or gastrointestinal symptoms. There was no history of tobacco smoking, chemical exposure, or family history of cancer. Physical examination revealed a 10x10 cm painless mass in the right inguinal region but was otherwise normal. All routine hematological and biochemical parameters were normal. Serologic tumor markers (CEA, lactate dehydrogenase, alpha-fetoprotein, prostate-specific antigen, human chorionic gonadotropin, CA125, and CA19-9) were within normal limits. An abdominal CT scan with contrast revealed two inhomogeneous masses anterior to the right rectus femoris (proximal 3.4x4.8 and 6.3x10.7; (Figure 2)) suggestive of enlarged lymph nodes. Chest CT and colonoscopy were normal. The patient underwent punch biopsy of the inguinal mass, which was suggestive of poorly differentiated transitional cell carcinoma (TCC) (Figure 3A). The decision was made to perform tumor extirpation with right ilioinguinal lymph node dissection. Final histopathological examination confirmed TCC (Figure 3B-C), with immunoreactivity for CK7, CK20, and p16 but not thyroid transcriptase factor-1 (TTF-1), synaptophysin, and CK5/6 (Figure 3D). A diagnosis of metastatic TCC in the right inguinal lymph node was made on clinical, histological, and immunohistochemical grounds. However, the primary site remained unknown even after a search for a primary tumor using pelvic magnetic resonance imaging (MRI), anorectal examination, and meticulous urological examination including cystoscopy. His inpatient stay was uncomplicated and he was discharged from hospital on the fifth postoperative day. He subsequently underwent adjuvant radiotherapy and received regular follow-up. At the most recent follow-up at 24 months there was no recurrence. | ||||||
| ||||||
| ||||||
|
| ||||||
|
Discussion
| ||||||
|
The carcinomas of unknown primary are defined as patients who present with histologically confirmed metastatic cancer for which no site of origin can be detected even after comprehensive investigations [1][2]. Although the exact etiology of CUP is poorly understood, CUP is thought to either represent: (i) a concurrent but undetected primary cancer, or (ii) a spontaneously regressed primary cancer that was either misdiagnosed, ignored, or went unnoticed. The incidence of CUP has declined, mainly due to the evolution of new detection methods and diagnostic modalities to identify the primary site [5][6] . Histologically, CUPs are categorized into four major subtypes by routine light microscopy:
Over 50% of CUP patients present with multiple sites of involvement, with a single site affecting the remainder, most commonly the liver, lymph nodes, peritoneum, lung, bone, and brain [1][2]. The inguinal area is a relatively uncommon metastatic site for CUP [7] [8]. The inguinal nodes are affected by a wide variety of metastases, mainly from the pelvis, genitalia, or lower limb but also more distant sites such as the nasopharynx, breast, tracheobronchial tree, salivary glands, and orbit [2][7][8]. The diagnostic evaluation of patients with CUP should be directed by the histopathological findings and be multi-modal. Recently, PET scans have proven to be a very useful imaging modality to detect the primary site, but cases in which the origin cannot be found are abundant [5]. In our case, contrast-enhanced CT scan of the abdomen and thorax were performed as PET-CT was not available. Molecular tumor profiling (MTP) is a powerful diagnostic tool for identifying the primary site. However, validation of the accuracy and clinical value of MTP has been difficult because the anatomic primary site in most patients is never identified [9]. Zaren et al. examined over 2000 patients with metastases in the inguinal lymph nodes and reported that the primary site could not be identified in 22 (1%), whereas Guarischi et al. examined 56 similar patients in whom the primary site could not be identified at all [4][8]. In our case, even after extensive attempts to find the primary site, the site of the primary tumor could not be determined. The management of CUP needs to be individualized according to the clinical features. Surgery with adjuvant radiotherapy has been reported as the preferred treatment for inguinal metastasis from a CUP [10]. To our knowledge, this is the first report of pure metastatic TCC in the inguinal lymph nodes from an unknown primary site, although there is one report of mixed transitional and squamous cell carcinoma [7]. | ||||||
|
Conclusion
| ||||||
|
Carcinoma of unknown primary remains clinically challenging. In spite of new diagnostic tests, the optimal diagnostic algorithm for metastatic tumors with unknown primary has yet to be established. Carcinomas of unknown primary are an important group of tumors to be aware of because their progression differs from other malignant tumors and is difficult to predict. Since the benefits of current therapies are either limited or of uncertain benefit in many patients, the evaluation of novel treatments is essential. | ||||||
|
Acknowledgements
| ||||||
|
We would like to thank Dr. Sebastian Blasius and Dr. Amal Hassan for preparing the histology illustrations. | ||||||
|
References
| ||||||
| ||||||
|
[HTML Abstract]
[PDF Full Text]
|
|
Author Contributions
Ghassan Almaimani – Substantial contributions to conception and design, Acquisition of data, Analysis and interpretation of data, Drafting the article, Revising it critically for important intellectual content, Final approval of the version to be published |
|
Guarantor
The corresponding author is the guarantor of submission. |
|
Source of support
None |
|
Conflict of interest
Authors declare no conflict of interest. |
|
Copyright
© 2017 Ghassan Almaimani et al. This article is distributed under the terms of Creative Commons Attribution License which permits unrestricted use, distribution and reproduction in any medium provided the original author(s) and original publisher are properly credited. Please see the copyright policy on the journal website for more information. |
|
|