|

|
 |
|
Case Report
| ||||||
| Classic case of cleidocranial dysplasia with an infected mandibular cyst | ||||||
| Madhu P. Sivan1, Jayakumar K.2, Jayalakshmi P. S.3, N. Sruthi4 | ||||||
|
1MDS, Provisional Lecturer, Department of Oral and Maxillofacial Surgery, Government Medical College, Thrissur, Kerala State, India 2MDS, Associate Professor and Head, Department of Oral and Maxillofacial Surgery, Government Medical College, Thrissur, Kerala State, India 3MDS, Assistant Professor, Department of Oral and Maxillofacial Surgery, Government Medical College, Thrissur, Kerala State, India 4BDS, Provisional Lecturer, Department of Oral and Maxillofacial Surgery, Government Medical College, Thrissur, Kerala State, India | ||||||
| ||||||
|
[HTML Abstract]
[PDF Full Text]
[Print This Article]
[Similar article in Pumed] [Similar article in Google Scholar] 
|
| How to cite this article |
| Sivan MP, Jayakumar K, Jayalakshmi PS, Sruthi N. Classic case of cleidocranial dysplasia with an infected mandibular cyst. Int J Case Rep Images 2017;8(4):242–247. |
|
Abstract
| ||||||
|
Patients with cleidocranial dysplasia commonly present with significant dental problems, such as retention of multiple deciduous teeth, impaction or delayed eruption of teeth and the presence of multiple supernumerary teeth. In fact, the presence of multiple supernumerary teeth is one among the pathognomonic triad for this condition; the other two being partial or complete absence of clavicles, and open sagittal sutures and fontanelles. This case report describes a patient having typical features of cleidocranial dysplasia who had to undergo surgical enucleation and debridement for an infected mandibular cyst. Factors dictating the treatment plan and the current trends in rehabilitation for such a patient have been discussed from a dental surgeon’s perspective acknowledging the shift in management paradigm for this condition over the years. Keywords: Cleidocranial dysplasia, Delayed eruption, Enucleation, Infected mandibular cyst, Supernumerary teeth | ||||||
|
Introduction
| ||||||
|
Cleidocranial dysplasia, is a congenital disorder of bone formation with prominent manifestations being clavicular hypoplasia/agenesis with a narrow thorax, delayed ossification of skull bones, excessively large fontanelles and delayed closing of sutures [1]. One of the earliest description of this condition was given by Martin in 1765[2]. Marie and Sainton in 1897 used the term cleidocranial dysostosis [3] . It has since been known as cleidocranial dysplasia in recognition of its underlying pathology being more of a generalized skeletal dysplastic condition. One in a million people and both genders are rather equally affected [1]. Genetic mutation as an etiologic factor for this condition was proposed by Kalliala et al. with 20–40% caused by spontaneous gene mutation [4]. Cleidocranial dysplasia follows autosomal dominant pattern of inheritance with high penetrance and variable degree of expression. The locus of the gene is either the long or short arm of chromosome 6p21 [5]. Zheng et al. reported that humans with cleidocranial dysplasia have altered endochondral ossification due to perturbed RUNX2 regulation of hypertrophic chondrocytes. This gene is essential for osteoblast and dental cell differentiation, and thus for normal bone and tooth formation [6] . Recent studies have indicated that RUNX2 serves as a master gene regulating osteoblast-specific gene expression. The gene is expressed in the cells of osteoblast lineage only, and its expression is regulated by calciotropic agents. In odontogenesis, RUNX2 regulates key epithelial mesenchymal interactions that control the progress of morphogenesis and histodifferentiation of the epithelial enamel organ [7]. Still more recently, CCAAT/enhancer-binding protein beta (Cebpb) which is a key factor of Runx2 expression has been proposed as an additional aetiological factor for cleidocranial dysplasia [8]. Herein, we present a case report of a patient with classical features of cleidocranial dysplasia with symptomatic infected mandibular cyst probably secondary to multiple impacted teeth and its management with surgical enucleation and debridement. | ||||||
|
Case Report
| ||||||
|
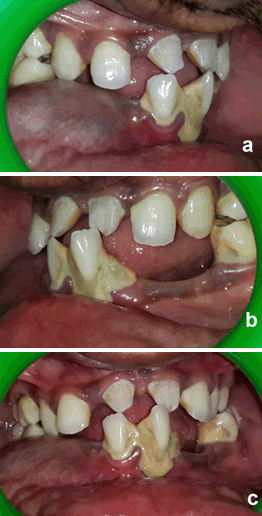
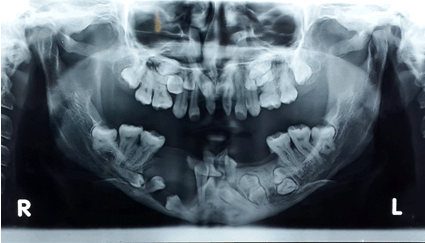
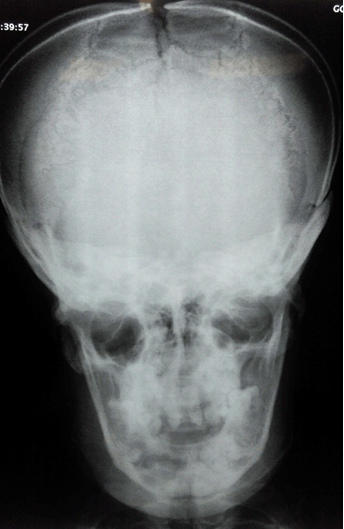
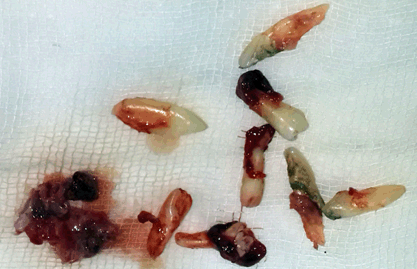
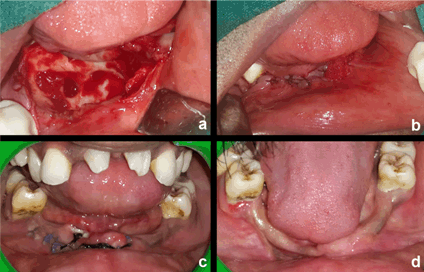
A 26-year-old male presented with chief complaint of tender swelling gradually increasing in size in lower right jaw region of 4–6 months duration. Intraoral examination showed a fluctuant swelling approximately 3x2 cm in size in mandibular right canine-premolar region tender to palpation (Figure 1). An active site of pus discharge along the crevices of adjacent molar teeth was seen. Multiple teeth were missing and generalized periodontitis owing to heavy calculus build-up was observed around the few teeth present in the oral cavity. Maxillary incisors were malformed. A total of 16 teeth were present in the oral cavity. A deep and high arched palate was noted. General physical examination demonstrated a thin build, short stature, slurred speech, narrow thorax and shrugged shoulders which were easily apposable. Prominent forehead with hypertelorism, a depressed nasal bridge, and mid-facial hypoplasia with relative mandibular prognathism were noted. Frontal, parietal and occipital bossing was present, giving the skull a large globular and brachycephalic shape (Figure 2). The panoramic radiograph on examination revealed a diffuse radiolucency in the area of interest suggestive of excessive bone loss due to the cystic lesion along with multiple impacted teeth (around 24 in number) and non-prominent gonial angle bilaterally (Figure 3). Posteroanterior cephalogram suggested non-ossified cranial sutures (Figure 4). Additionally, his elder brother, showed similar external facial and general appearance (Figure 5). Subsequently, a surgical treatment plan involving surgical enucleation and debridement of affected tissue and disimpaction of multiple involved impacted teeth in the area of concern under general anesthesia with supportive systemic antibiotics and analgesics was planned and executed. A difficult airway was anticipated during general anesthesia. Following enucleation, a total of nine teeth in and around the area of interest were disimpacted, tissue debrided and primary closure was achieved. Post-surgical healing was uneventful and satisfactory (Figure 6). Histopathological examination was confirmatory for dentigerous cyst. The patient is under regular follow-up and Prosthodontic rehabilitation is planned in the coming months once the presence of adequate bone support is confirmed clinically and radiographically (Figure 7). | ||||||
| ||||||
| ||||||
| ||||||
| ||||||
| ||||||
| ||||||
| ||||||
|
Discussion
| ||||||
|
Cleidocranial dysplasia shows a wide degree of varying manifestations clinically which may or may not affect the quality of life of the patient. They typically have a shorter stature, brachycephaly with frontal, parietal and occipital bossing, and increased intraorbital distance, wide and flat bridge of the nose, underdeveloped maxilla and relative mandibular prognathism. Hypoplasia of masseter muscle due to discontinuity of zygomatic arches may result in compensatory hyperfunctioning of temporalis muscles. Consequently, anterior border of the mandibular ramus is usually parallel to the posterior border, and the coronoid process is directed upwards and backwards. There is typical delayed closure of the fontanel. Clavicular hypoplasia/agenesis and unusually formed/placed muscles attachments to the clavicles may be seen. Further, unusual positioning of hip joint, abnormalities of the bones of the spine, fingers and hands have been reported. Occasional abnormalities associated with this condition includes scoliosis, extra ribs, small pelvis, cleft palate, recurrent ear infections(otitis media) related to abnormal formation of palate and/or Eustachian tube dysfunction and respiratory problems. These individuals typically have normal ability to learn [9][10]. The pathognomonic triad for cleidocranial dysplasia were present in this patient. He reported for treatment only when he started experiencing significant discomfort which is often the case elsewhere. It may be assumed that the slow growing cystic lesion associated with the multiple impacted teeth may have been secondarily infected after substantial erosion of the associated bony structure of the mandible. Since the expression of the disorder shows significant variation and is rarely expressed to a degree causing significant discomfort or disfigurement to the patient, the condition is often diagnosed incidentally or at a much later age when there is an associated secondary pathology. The timing of diagnosis is important in choosing an appropriate treatment plan and in attaining a successful result. With significant advances in medicine and dentistry clubbed with increase in awareness, accessibility and affordability to rehabilitation procedures for the patient, there has been a significant shift in management protocol for this condition. Many years ago, minimal intervention to address any symptomatic pathology or no intervention was recommended. Over the next few years, rehabilitation procedures to improve the overall quality of life became more prevalent. In early 20th century, orthodontic- surgical intervention for forced eruption, use of partial dentures etc. gained popularity. Still more recently, dental implants and implant supported dentures have been used for oral rehabilitation. Orthognathic surgeries for correction of facial aesthetics have also gained acceptance. From a dental practitioner’s perspective, elimination of clinical pathology followed by achieving a functional dentition and an overall aesthetically satisfying facial appearance should be the ultimate treatment objectives. Psychological support to the patient and parent is often necessary. Multidisciplinary approach is of prime importance. Affected infants should receive their first dental evaluation by one year of age. Extraction of primary teeth does not hasten the eruption of permanent teeth here. Jensen and Kreiborg have suggested that supernumerary teeth form as a result of activation of remnants of dental lamina left unresorbed during odontogenesis. The contributory role of supernumerary teeth to the arrested eruption of permanent teeth is believed to be secondary to that of diminished bone resorption [9][10]. In late mixed dentition period and permanent dentition period, combination of orthodontic and maxillofacial surgical approaches are recommended. Following the orthodontic phase, skeletal discrepancies (usually a Class III skeletal malocclusion) are corrected with orthognathic surgeries after completion of growth. Prosthodontic rehabilitation with/without the use of dental implants are carried out further to establish a functional dentition and to fulfil aesthetic requirements. The cystic lesion here was a dentigerous cyst which was enucleated and confirmed histopathologically. Since the bone loss was significant and extended very close to the lower border of the mandible, we handled the soft tissue and hard tissue with care. However, no graft was required. Instructions were given to the patient for adequate care during postoperative period. We have also delayed the prosthodontic rehabilitation until clinical and radiographic evidence for adequate bone presence is established. The first case of cystic involvement in cleidocranial dysplasia was reported by Oatis et al. in 1975 [11]. Since then very few cases such cases have been documented. This is an interesting aspect when we take into perspective the number and frequency of multiple dental impactions seen in cleidocranial dysplasia patients. | ||||||
|
Conclusion
| ||||||
|
Planning treatment for a patient with cleidocranial dysplasia is complicated by a host of factors and is often complicated further due to non-coincident dental and chronological age. The patient’s perception of the need for treatment may deviate from that of the treating practitioner. It may be difficult to obtain consent to a treatment involving multiple surgical exposures and forced eruption of teeth. The treatment plan thus requires to be tailored to address the individual’s chief complaint taking into consideration the extent of motivation of the patient and a host of other clinical factors as discussed above. With proper anticipatory guidance, people with cleidocranial dysplasia usually lead healthy and productive lives. | ||||||
|
References
| ||||||
| ||||||
|
Suggested Reading
| ||||||
|
| ||||||
|
[HTML Abstract]
[PDF Full Text]
|
|
Author Contributions
Madhu P. Sivan – Substantial contributions to conception and design, Acquisition of data, Analysis and interpretation of data, Drafting the article, Revising it critically for important intellectual content, Final approval of the version to be published Jayakumar K. – Substantial contributions to conception and design, Acquisition of data, Analysis and interpretation of data, Revising it critically for important intellectual content, Final approval of the version to be published Jayalakshmi P. S. – Substantial contributions to conception and design, Acquisition of data, Analysis and interpretation of data, Revising it critically for important intellectual content, Final approval of the version to be published Sruthi N. – Substantial contributions to conception and design, Acquisition of data, Analysis and interpretation of data, Revising it critically for important intellectual content, Final approval of the version to be published |
|
Guarantor
The corresponding author is the guarantor of submission. |
|
Source of support
None |
|
Conflict of interest
Authors declare no conflict of interest. |
|
Copyright
© 2017 Madhu P. Sivan et al. This article is distributed under the terms of Creative Commons Attribution License which permits unrestricted use, distribution and reproduction in any medium provided the original author(s) and original publisher are properly credited. Please see the copyright policy on the journal website for more information. |
|
|