|
 |
|
Case Report
| ||||||
| Radiographic changes of the mandible after proton beam radiotherapy for oral cancer: A case report | ||||||
| Masaru Konishi1, Yoshikazu Suei2, Minoru Fujita3, Keiji Tanimoto4 | ||||||
|
1D.D.S., PhD, Assistant Professor, Department of Oral and Maxillofacial Radiology, Hiroshima University Hospital, Hiroshima, Japan
2D.D.S., PhD, Lecturer, Department of Oral and Maxillofacial Radiology, Hiroshima University Hospital, Hiroshima, Japan 3D.D.S., PhD, Associate Professor, Department of Oral and Maxillofacial Radiology, Institute of Biomedical and Sciences, Hiroshima University, Hiroshima, Japan 4D.D.S., PhD, Professor, Department of Oral and Maxillofacial Radiology, Institute of Biomedical and Sciences, Hiroshima University, Hiroshima, Japan | ||||||
| ||||||
|
[HTML Abstract]
[PDF Full Text]
[Print This Article] [Similar article in Pumed] [Similar article in Google Scholar] 
|
| How to cite this article |
| Konishi M, Suei Y, Fujita M, Tanimoto K. Radiographic changes of the mandible after proton beam radiotherapy for oral cancer: A case report. Int J Case Rep Images 2017;8():787–791. |
|
ABSTRACT
| ||||||
|
Introduction: Radiation-induced osteomyelitis or osteoradionecrosis of the jaw bone is one of the most severe adverse effects of radiotherapy sometimes experienced by head and neck cancer patients. We report on the observed radiographic changes after proton radiotherapy for a patient with squamous cell carcinoma in the mandibular bone. Keywords: Bone regeneration, Osteoradionecrosis, Proton beam radiotherapy, Radiation-induced osteomyelitis | ||||||
|
INTRODUCTION
| ||||||
|
One of the adverse effects of radiotherapy for head and neck cancer is radiation-induced osteomyelitis or osteoradionecrosis (ORN) of the jaw bone. A lot of clinical and physical factors have been reported to be associated with the risk of ORN. They include patient-, tumor-, and treatment-related variables [1][2]. Tolerance dose of the mandibular bone was reported from 60–72 Gy [3]. Fujita et al. reported that a total dose of 90 Gy or more and a dose rate of 0.55 Gy/h or higher were associated with a significant increase in the incidence of ORN at the brachytherapy for oral tongue cancer [4]. Oral health status is a risk factor for ORN, and oral health care is an important element in the prevention of ORN. Good oral conditions before and after radiotherapy for all irradiated head and neck cancer patients are very important to prevent ORN [2][5]. The multidisciplinary team communications like the consultation of dentists or dental hygienists before the radiotherapy are commonly recommended. The managements of ORN are reported such as a conservative management, ultrasound therapy, hyperbaric oxygen [6][7]. In any case, once ORN occurred, it often can persist for a long time and be hard to manage. Owing to the physical characteristics depositing the bulk of the radiation dose in a highly confined area of the proton beam, some lesions became treatable with the proton beam radiotherapy even if it was the treatment-resistant tumors in sensitive location [8]. Numerous studies have reported on ORN resulting from radiotherapy with X-rays. However, few reports exist on ORN resulting from proton beam radiotherapy. We report on the observed radiographic changes after proton radiotherapy for a patient with squamous cell carcinoma in the mandibular bone. | ||||||
|
CASE REPORT
| ||||||
|
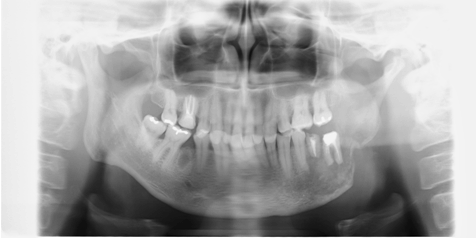
A 60-year-old male was referred to the department of oral and maxillofacial surgery with a history of persistent swelling on the left side of his face. He has been presenting with soft swelling of the left cheek and sub-mandibular region for two weeks. He was also experiencing paresthesia of the third division of the trigeminal nerve, and had limited range of motion of the jaw. The lower left second molar had been extracted and the socket was covered with soft granulation tissue. Histopathological diagnosis was based on a biopsy of the gingiva confirmed squamous cell carcinoma. Panoramic radiography at the initial visit showed a moss-eaten appearance of the left mandible (Figure 1). Computed tomography (CT) scan revealed a well-enhanced mass and bone destruction of the left mandible (Figure 2). Initially, a surgical approach for treatment was considered. However, after 18F-fluorodeoxyglucose positron emission tomography of the region, the case was deemed inoperable as tumor invasion into the cranial fossa and was suspected along the trigeminal nerve. The patient was thus treated with chemotherapy (cisplatin and 5-fluorouracil) and proton beam therapy to 70 Gy in 35 fractions. A panoramic image one month after proton beam therapy is shown in (Figure 3). At that time, there was obvious resorption and deformity in the left mandible. The images of cone-beam computed tomography (CBCT) one month after proton radiotherapy (Figure 4) showed a possible trabecular bony formation at the location of the primary lesion. The cortical bone once adjacent to the lesion was nearly destroyed. A panoramic image at 10th month post-proton beam therapy (Figure 5) showed a defect where the left mandible (and tumor) had originally existed and the first molar presented as a floating tooth. Computed tomography scan images at 10th month after proton beam therapy (Figure 6) showed continued new bone formation and regeneration of the cortical bone of the mandible. The patient experienced extreme occlusal dysfunction as a result of the bone resorption, which was exacerbated at meal times. The patient had a local recurrence one year after proton beam therapy and perished about 19 months after proton beam therapy and 26 months after the first visit. | ||||||
| ||||||
|
| ||||||
| ||||||
| ||||||
| ||||||
|
| ||||||
|
DISCUSSION
| ||||||
|
Proton beam therapy is one of the most technologically advanced forms of radiotherapy. Protons differ from traditional megavoltage X-ray radiotherapy owing to the characteristic Bragg peak of a proton beam. The Bragg peak can be described as the deposition of energy at a specific depth in the body as the protons decelerate. The Bragg peak can be placed at any depth in the body (corresponding to a tumor location), depending on the energy of the beam selected. Conventional radiation therapy faces challenges from side effects because of a relatively high entrance dose as well as a non-zero exit dose. By contrast, proton therapy has a substantially lower entrance dose and no exit dose that reduces damage to healthy tissue surrounding a tumor [9]. In addition to differences in dose deposition; protons have different radiobiological properties compared with photons. Specifically, the relative biological effectiveness (RBE) of protons beam is considered to be 1.1, compared with 1.0 for photons. The head and neck squamous cell carcinoma observed in this case was well suited for proton therapy owing to the improved dose deposition and RBE. The radiographic features of ORN have many similarities to those of chronic osteomyelitis [10]. An early characteristic change due to therapeutic doses of radiation is a well-defined area of bone resorption within the outer cortical plate of the mandible. Late changes are quite variable and may be predominantly osteolytic or osteosclerotic, or a mixture. Typically, the periphery of a lesion is ill-defined, and the cortical bone of the jaws shows irregular resorption. New periosteal bone formation is uncommon. For comparison, the radiographic findings of the present case and relevant published data resulting from X-ray radiotherapy are given in Table 1 [11]. Published data from patients treated with X-ray radiotherapy showed sequestrum formation, and the present case also demonstrated an unclear trabecular bone sequestrum formation in the mandible. However, the presentation of this formation in this case was different than what is typically observed with osteoradionecrosis resulting from X-ray radiotherapy. Sequestral formations typically occur in the normal bone areas of the jaw as a result of X-ray radiotherapy. In the present case, the new bone formation started in the mandible where bone resorption had occurred because of the lesion. The amount of new bone formation was very small in the present case and showed a sequestrum formation without bone trabeculae upon CT imaging. With time, it may have been possible to more clearly observe the cancellous and cortical bone on CT images and the trabecular pattern might have been observable with long-term follow-up. However, as the patient passed away 19 months after proton beam therapy, we were not able to observe such radiographic changes. For this reason, we were unable to identify whether the new bone formation observed was a sequestrum. In the present case, the mandible was almost destroyed by the cancerous invasion, but any surviving osteoblasts would have proliferated and led to the bone formation after the proton beam therapy had eliminated the cancer cells. We compared the radiographic findings of ORN resulting from X-ray radiotherapy with those of ORN from proton beam radiotherapy. One of the main factors in choosing a form of radiotherapy (X-rays or protons) is the physiological state of the disease. Conventional radiotherapy was not indicated for the present case because the lesion had infiltrated deep into the mandibular bone. Osteoradionecrosis resulting from X-ray radiotherapy typically occurs secondary to the treatment of the primary lesion. In the present case, as the primary lesion had extensively infiltrated the mandibular bone, it was assumed that the mandibular bone was concurrently absorbed with the reduction of the lesion resulting from proton beam radiotherapy. Future investigations should consider the radiation-induced changes to bone separately whether or not the primary lesion exists in the bone. | ||||||
|
||||||
|
CONCLUSION
| ||||||
|
Most lesions in the bone do not qualify for curative radiotherapy with X-rays. Typically, radiotherapy is used as a palliative treatment for pain relief or reduction of paralysis risk in patients with bone metastasis. Therefore, it is difficult to predict if the bone absorbed because of the presence of a cancerous lesion will or will not experience new bone formation in the area of the destructed lesion. With the advent of proton beam radiotherapy, the number of diseases which can be curatively treated has increased. As more patients with cancers in the jaw bone are treated with protons, careful observation of any radiation-induced effects such as osteoradionecrosis need to be monitored, classified, and disseminated appropriately. | ||||||
|
REFERENCES
| ||||||
| ||||||
|
[HTML Abstract]
[PDF Full Text]
|
|
Author Contributions
Masaru Konishi – Substantial contributions to conception and design, Acquisition of data, Analysis and interpretation of data, Drafting the article, Revising it critically for important intellectual content, Final approval of the version to be published Yoshikazu Suei – Acquisition of data, Drafting the article, Final approval of the version to be published Minoru Fujita – Analysis and interpretation of data, Drafting the article, Final approval of the version to be published Keiji Tanimoto – Analysis and interpretation of data, Drafting the article, Final approval of the version to be published |
|
Guarantor of Submission
The corresponding author is the guarantor of submission. |
|
Source of Support
None |
|
Conflict of Interest
Authors declare no conflict of interest. |
|
Copyright
© 2017 Masaru Konishi et al. This article is distributed under the terms of Creative Commons Attribution License which permits unrestricted use, distribution and reproduction in any medium provided the original author(s) and original publisher are properly credited. Please see the copyright policy on the journal website for more information. |
|
|