|
 |
|
Case Series
| ||||||
| Richter’s hernia: Two observations in the Baka pygmies of Eastern Cameroon | ||||||
| Tsopmene Dongmo Marvin1, Nkeck Jan René2, Eloundou Ngah Joseph3 | ||||||
|
1Medical Doctor, General practitioner, Faculty of Medicine and Biomedical Sciences of the University of Yaoundé I; St. Mary of Salapoumbe’s Catholic Hospital
2Medical Doctor, Intern, Faculty of Medicine and Biomedical Sciences of the University of Yaoundé 3Professor of medicine, Neurosurgeon, Faculty of Medicine and Biomedical Sciences of the University of Yaoundé | ||||||
| ||||||
|
[HTML Abstract]
[PDF Full Text]
[Print This Article] [Similar article in Pumed] [Similar article in Google Scholar] 
|
| How to cite this article |
| Tsopmene MR, Nkeck JR, Eloundou NJ. Richter’s hernia: Two observations in the Baka pygmies of Eastern Cameroon. Int J Case Rep Images 2017;8(11):689–691. |
|
ABSTRACT
| ||||||
|
Introduction: Richter’s hernia has a misleading clinical presentation at the onset of the disease due to common lack of obstructive signs whereas there is visceral strangulation. The delay in diagnosis is therefore long leading to high morbidity and mortality in a rural context where access to essential surgical care is limited. Keywords: Cameroon, Diagnostic delay, Richter’s hernia, Strangulation | ||||||
|
INTRODUCTION
| ||||||
|
The first scientific description of the Richter’s hernia was made in 1778 by the German surgeon August Gottlob Richter. It accounts for about 5–15% of strangulated hernias, in which only part of the circumference of the antimesenteric border of the bowel wall is incarcerated within the hernia sac leading to strangulation [1]. The lack of bowel obstruction is the known cause of diagnosis and management delay. A delay in management is associated with a risk of bowel ischemia, gangrene and perforation, leading to high morbidity and mortality. | ||||||
|
CASE SERIES
| ||||||
|
Case 1 | ||||||
|
A 24-year-old female presented with a three-day history of a painful, non-reducible right inguinal swelling without any sign of bowel obstruction. The diagnosis of a right inguinal hernia was made. The surgical findings were those of a direct inguinal hernia with 5 cm of the antimesenteric side of the distal ileum incarcerated and gangrenous (Figure 1). A short sub-umbilical median laparotomy allowed mobilization of the incarcerated loop. Resection of the segment of ileum involved was done with ileoileal hand sewn anastomosis followed by a parietal repair. The total duration of hospitalization was 10 days and the postoperative outcome good with a four month follow-up. | ||||||
| Case 2 | ||||||
|
A 29-year-old male presented with a week history of a right inguinal pain. The patient was ill-looking with a body temperature 38.9°C, heart rate 102 bpm, and blood pressure 99/52 mmHg. In addition, he had an abdominal tenderness in the hypogastric and right iliac fossa regions with a non-reducible inflammatory groin mass. Surgery revealed a strangulated direct inguinal hernia with a gangrenous sac. Following a kelotomy, we performed a resection of the necrotic part of the ileum loop and performed an end-to-end anastomosis. The parietal cure was done according to Shouldice technique. The total duration of hospitalization was seven days and a good outcome following three months postoperative follow-up. | ||||||
| ||||||
|
DISCUSSION
| ||||||
|
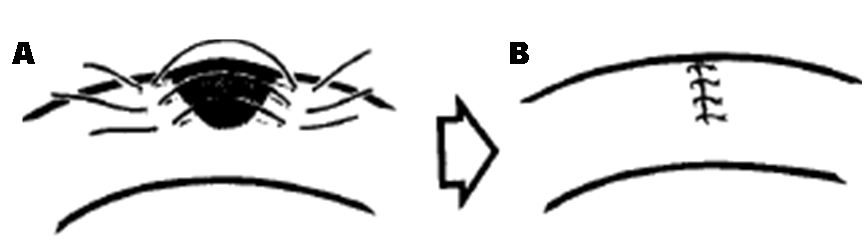
Richter’s hernia is the incarceration of part of the circumference of the wall of the antimesenteric side of the loop through a small hernia ring. It was named after its first scientific description by the German surgeon August Gottlieb Richter in 1778 [1]. In the Caucasian subjects, the most frequent localization is the femoral canal (36–88%) followed by the deep inguinal ring (12–36%) [2][3]. The two cases presented were direct inguinal hernias. This result is similar to that obtained by Wolfgang et al., and other authors who reported a clear predominance of direct inguinal hernias ranging from 78–94% [4][5][6]. The common use of laparoscopic surgery has led to increase abdominal wall incisional hernias [7]. Richter’s hernia represents in the general population 5–15% of the strangulated hernias [1]. This prevalence is higher in Africa where Hancock et al. reported in a study in Uganda a prevalence of 25% and Wolfgang et al. a prevalence of 81% in Sudan [1][4]. This discrepancy could be explained on one hand by anatomical particularities, namely the small hernia rings with firm margins and on the other hand the malnutrition responsible for the increased elasticity of the intestinal wall. Kadirov et al. reported a female predominance with 57% of women, while Tomaszewski et al. and Wolfgang et al. reported a female predominance with sex ratio 6.3 and 1.4 respectively [1][8][9]. The clinical diagnosis of partial enterocele is not easy, the clinical presentation being misleading at the beginning, marked by an irreducible painful inguinal swelling without bowel obstruction. This bowel strangulation without obstruction would be one of the causes of diagnostic delay hence, a high morbidity and mortality. Medical imaging has a prime role in the diagnosis of Richter’s hernias, particularly with ultrasonography and computed tomography. However, they are generally inconclusive at the onset of the disease [1][10][11]. Surgical treatment should be carried out as soon as possible, either by segmental resection with an end to end anastomosis or by extra-mucosal suture invaginating the gangrenous segment (Figure 2). This operative technique proposed by Horbach et al., which avoids bowel resection, is performed only under certain conditions; the gangrenous segment does not extend across more than half the circumference of the gut and its margins are clearly healthy [4]. | ||||||
| ||||||
|
CONCLUSION
| ||||||
|
The two cases presented illustrate the picture of the Richter’s hernia whose clinical signs are misleading. In presentation of any groin swelling, the need for an early and accurate diagnosis followed by prompt treatment cannot be overemphasized. The surgical treatment remains in relation with local and parietal conditions. | ||||||
|
REFERENCES
| ||||||
| ||||||
|
[HTML Abstract]
[PDF Full Text]
|
|
Acknowledgements
We would like to thank Nsalar Didier for patient management and for taking clinical photograph, and also thank to Ndoadoumgue Aude Laetitia for the translation of the manuscript. |
|
Author Contributions
Tsopmene Dongmo Marvin – Substantial contribution to conception and design, Acquisition of data, Drafting the article, Final approval of the version to be published Nkeck Jan René – Substantial contribution to conception and design, Revising the article critically for potential intellectual content, Final approval of the version to be published Eloundou Ngah Joseph – Substantial contribution to conception and design, Revising the article critically for potential intellectual content, Final approval for the version to be published |
|
Guarantor
The corresponding author is the guarantor of submission. |
|
Source of support
None |
|
Conflict of interest
Authors declare no conflict of interest. |
|
Copyright
© 2017 Tsopmene Dongmo Marvin et al. This article is distributed under the terms of Creative Commons Attribution License which permits unrestricted use, distribution and reproduction in any medium provided the original author(s) and original publisher are properly credited. Please see the copyright policy on the journal website for more information. |
|
|