|
 |
|
Case Report
| ||||||
| Jejunal angiodysplasia: A rare cause of obscure gastrointestinal bleeding | ||||||
| Gareth Zigui Lim1, Than Than Aye2, Thein Myint3 | ||||||
|
1MBBS, BSc, Medical Student, Gastroenterology Department, Yangon General Hospital, Yangon, Myanmar
2MBBS, MMEdSc (IntMed), MRCP (UK), Consultant, Department of Gastroenterology, Yangon General Hospital, University of Medicine 1, Yangon, Myanmar 3MBBS, MMEdSc (IntMed), MACTM (Aus), Dr.MedSc (Gastroenterology), MRCP (UK), FRCP (Edin), Professor/Head of Department, Department of Gastroenterology, Yangon General Hospital, University of Medicine 1, Yangon, Myanma | ||||||
| ||||||
|
[HTML Abstract]
[PDF Full Text]
[Print This Article] [Similar article in Pumed] [Similar article in Google Scholar] 
|
| How to cite this article |
| Lim GZ, Aye TT, Myint T. Jejunal angiodysplasia: A rare cause of obscure gastrointestinal bleeding. Int J Case Rep Images 2017;8(11):752–755. |
|
ABSTRACT
| ||||||
|
Introduction: Obscure gastrointestinal bleeding (OGIB) represents about 5% of all gastrointestinal bleeds. This can pose a huge diagnostic challenge for clinicians. Small bowel angiodysplasia is a rare but important cause of OGIB that is difficult to diagnose and treat. Keywords: Jejunal angiodysplasia, Obscure gastrointestinal bleeding | ||||||
|
INTRODUCTION
| ||||||
|
Angiodysplasia is a type of vascular malformation with fragile and leaky vessels that can affect anywhere along the gastrointestinal tract. It is responsible for about 6% of lower gastrointestinal bleeding and between 1.2–8% of upper gastrointestinal bleeding [1]. Obscure gastrointestinal bleeding (OGIB) represents about 5% of all gastrointestinal bleeds [2], with small bowel angiodysplasia estimated to account for around 30–40% of cases [3]. Thus, it is an important differential that must be considered. Clinically, its presentation can vary from being an incidental finding to OGIB or chronic anemia. These patients should be evaluated with oesophagogastroduodenoscopy (OGD), colonoscopy, video capsule endoscopy (VCE) and angiography. Additionally, a red blood cell scan can increase the sensitivity of diagnosis when used in combination with angiography [4][5]. In acute presentations, endoscopic therapy should be used to treat active bleeding from angiodysplasia. Options include argon plasma coagulation (APC), sclerosant injections and gel foam embolization. Double balloon enteroscopy (DBE) can be used for both diagnostic and therapeutic purposes. For long-term management, somatostatin analogues, hormonal therapy or anti-angiogenics can be used [6]. In refractory bleeding or if lesions are at inaccessible sites, surgical localization and resection of the diseased segment can be performed. | ||||||
|
CASE REPORT
| ||||||
|
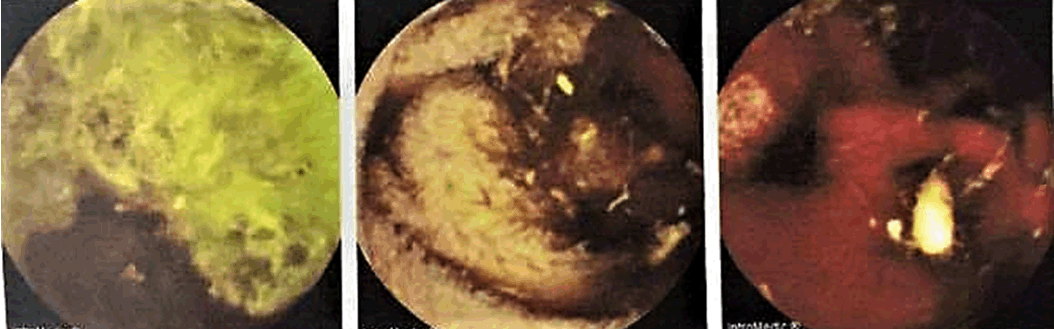
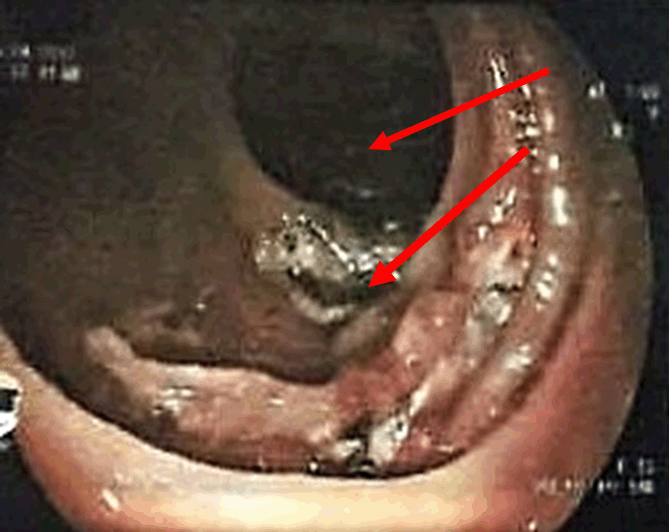
A 53-year-old female presented to Thingangyun Sanpya General Hospital, Yangon, Myanmar in February 2017 with a one-month history of increasing dyspnea, palpitations and pallor. She recalled a few episodes of melena. There were no other cardiac, respiratory or gastrointestinal symptoms. Apart from severe conjunctival pallor, physical examination and digital rectal examination were unremarkable. Blood tests revealed a hypochromic microcytic anemia (Hb 5.3, MCV 53.4) and she was found to have HbE trait on hemoglobin electrophoresis. She was transfused 5 units of blood. An OGD performed showed a duodenal ulcer and gastric vascular ectasia which was subsequently treated with argon plasma coagulation (APC). However, these findings could not explain her severe anemia and a colonoscopy was performed in March 2017. The colonoscopy revealed small polyps in the descending and sigmoid colon which were tubular adenomas on histology. These findings still could not explain her severe anemia. A month later, video capsule endoscopy was performed to locate potential sources of bleeding. This showed active small bowel bleeding in the last part of the duodenum and jejunum (Figure 1). An ultra-slim colonoscope was then used to better visualize the small bowel, showing multiple angiodysplastic spots with active bleeding in the proximal jejunum. Argon plasma coagulation was applied and a diagnosis of jejunal angiodysplasia was made (Figure 2). The patient presented again, this time to Yangon General Hospital, Yangon, Myanmar towards the end of April 2017 with similar worsening anemic symptoms (Hb 3.5). She was transfused 4 units of blood, stabilized and discharged. A computed tomography angiography (mesenteric angiogram) was performed in May 2017. The result showed contrast-enhancing wall thickening at the second part of the duodenum, but no serpiginous vascular channels or contrast extravasation was observed. Due to the equivocal results, a slim colonoscope was used to visualize the jejunum again, and this was normal up to the duodenal-jejunal junction. The patient was transfused 2 units of blood, discharged and followed-up in clinic, with a plan for a DBE if symptomatic anemia recurred. | ||||||
| ||||||
| ||||||
|
DISCUSSION
| ||||||
|
Small bowel angiodysplasia is a rare but important cause of OGIB or upper gastrointestinal bleeding. It should be considered in the differential list for gastrointestinal bleeding and chronic anemia, especially in patients with negative OGD and colonoscopies [3]. In this case, multiple gastrointestinal pathologies were initially discovered in this patient on OGD and colonoscopy. Sound clinical judgment was required to deduce that the findings could not explain the patient’s clinical presentation, hence further investigations were undertaken. In all, there was a four-month time period between symptom onset and final diagnosis. Small bowel angiodysplasia is a challenging condition to formally diagnose; video capsule endoscopy and computed tomography angiography play a key role, and these should be requested in patients with negative gastrointestinal scope procedures, or with results that do not correlate with clinical presentation. In this case, however, computed tomography angiography results were equivocal for angiodysplasia. This could be because the patient was not actively bleeding at the time of investigation. Additionally, radiologists recommended that the gastrointestinal hemorrhage computed tomography angiogram protocol should have been specifically requested according to local hospital guidelines. This should be stated on the request form to prompt radiologists to focus particularly on gastrointestinal mucosal vessels. A multidisciplinary team meeting was later conducted, with the team concluding that there was enough evidence for a formal diagnosis of jejunal angiodysplasia to be made despite the equivocal angiogram. This is a rare condition not commonly encountered by healthcare professionals, hence many were unfamiliar with diagnostic methods. A multidisciplinary team approach involving gastroenterologists, general surgeons and emergency physicians must be adopted early to ensure quick diagnosis and management of this potentially life-threatening condition. In terms of treatment, our patient was mainly managed supportively with blood transfusions when indicated. Endoscopic intervention via APC was only performed once. However, the patient’s symptoms recurred over four months. Long-term therapies such as octreotide could be considered in this case, and further surgical intervention should symptoms continue to persist. Many problems exist in the field of healthcare in Myanmar, including poor access to hospitals and a shortage of resources and health professionals [7]. There are a total of only five public endoscopy centers in the entire country and a shortage of gastroenterologists, which is insufficient for a population of over 51 million people. Private facilities are available, but many people live in poverty, and they are often unable to afford these services. In this case, the delay from presentation to diagnosis could be explained by the challenging nature of the illness, and also the difficulty in accessing relevant investigations more quickly. Doctors in resource-limited settings like these are forced to rely more on their clinical judgment in making diagnoses. They must also be more familiar with local hospital protocols and stay up to date with their knowledge given the lack of national guidelines and rare presentation of this case. | ||||||
|
CONCLUSION
| ||||||
|
In conclusion, small bowel angiodysplasia is a rare but important cause of obscure gastrointestinal bleeding (OGIB). It should be on the differential list for patients presenting with any gastrointestinal bleeding. There should be a higher suspicion for small bowel angiodysplasia if oesophagogastroduodenoscopy (OGD) and colonoscopy yield inconclusive results. Video capsle endoscopy and computed tomography angiography are useful investigations for its diagnosis. In the acute setting, management options include supportive blood transfusions and interventional endoscopy. Double balloon enteroscopy is a useful tool that can be considered for both diagnostic and therapeutic purposes. In resource-limited settings, it is important for doctors to be familiar with this condition and the diagnostic and management options available. | ||||||
|
REFERENCES
| ||||||
| ||||||
|
[HTML Abstract]
[PDF Full Text]
|
|
Author Contributions
Gareth Zigui Lim – Substantial contributions to conception and design, Acquisition of data, Analysis and interpretation of data, Drafting the article, Revising it critically for important intellectual content, Final approval of the version to be published Than Than Aye – Substantial contributions to conception and design, Acquisition of data, Analysis and interpretation of data, Revising it critically for important intellectual content, Final approval of the version to be published Thein Myint – Analysis and interpretation of data, Revising it critically for important intellectual content, Final approval of the version to be published |
|
Guarantor
The corresponding author is the guarantor of submission. |
|
Source of support
None |
|
Conflict of interest
Authors declare no conflict of interest. |
|
Copyright
© 2017 Gareth Zigui Lim et al. This article is distributed under the terms of Creative Commons Attribution License which permits unrestricted use, distribution and reproduction in any medium provided the original author(s) and original publisher are properly credited. Please see the copyright policy on the journal website for more information. |
|
|