|
 |
|
Case Report
| ||||||
| Cerebral hemorrhagic infarction as the initial manifestation of deep venous thrombosis in a child with patent foramen ovale: A case report | ||||||
| Dimitrios Panagopoulos1, Sofia Loukopoulou2, Georgios Markogiannakis1, Nikos Eleftherakis3 | ||||||
|
1Consultant Neurosurgeon, Neurosurgical Department, Pediatric Hospital, Aglaia Kyriakou, Athens, Greece
2Consultant cardiologist, Cardiology Department, Pediatric Hospital, Agia Sophia, Athens, Greece 3Consultant Cardiologist, Director of the Hemodynamic Cardiology Department, Pediatric Hospital, Agia Sophia, Athens, Greece | ||||||
| ||||||
|
[HTML Abstract]
[PDF Full Text]
[Print This Article] [Similar article in Pumed] [Similar article in Google Scholar] 
|
| How to cite this article |
| Panagopoulos D, Loukopoulou S, Markogiannakis G, Eleftherakis N. Cerebral hemorrhagic infarction as the initial manifestation of deep venous thrombosis in a child with patent foramen ovale: A case report. Int J Case Rep Images 2017;8(11):739–745. |
|
ABSTRACT
| ||||||
|
Introduction: Arterial ischemic stroke (AIS), with an estimated incidence of 1.1–4.3 per 100,000, is an important cause of morbidity and mortality in children and the recurrence risk is high. Keywords: Cryptogenic stroke, Foramen ovale | ||||||
|
INTRODUCTION
| ||||||
|
Ischemic stroke in children is a relatively rare entity relative to the adult population. The definition includes ischemic and hemorrhagic infarction· in children, 55% are believed to be ischemic, and the remainder hemorrhagic. The wide range of pathophysiological processes associated with pediatric strokes mandates a careful diagnostic evaluation to maximize the chances for optimal patient outcome. Pediatric arterial ischemic stroke (AIS) is an important cause of neurologic morbidity in children. Consequences can include sensorimotor deficits, language impairment, and intellectual disability, behavioral problems, and epilepsy [1]. Unfortunately, the diagnosis of stroke in children is often delayed [2][3]. Children with cardiac disease represent one of the most significant subsets of pediatric AIS patients. Across most series, cardiac risk factors are present in 2–31% of children with AIS [4] [5][6] [7] [8][9]. A point of uncertainty persists regarding the role of an isolated patent foramen ovale (PFO), in part because there is significant variability in how this has been considered across studies, with some lumping it in with other structural heart diseases while others have separated it as a distinct diagnosis. While there is some evidence suggesting an important role of right-to-left shunting across an atrial defect, particularly among patients with prothrombotic conditions or cryptogenic stroke [10], the role of device closure remains undefined due to lack of sufficient evidence [11]. We present a rare clinical case of a young girl harboring a latent deep venous thrombosis (DVT), a thrombus in the right atrium with subsequent arterial ischemic stroke (AIS) of the brain, possibly due to a patent foramen ovale (PFO)· This was the first clinical manifestation of an otherwise unrecognized clinical condition. | ||||||
|
CASE REPORT
| ||||||
|
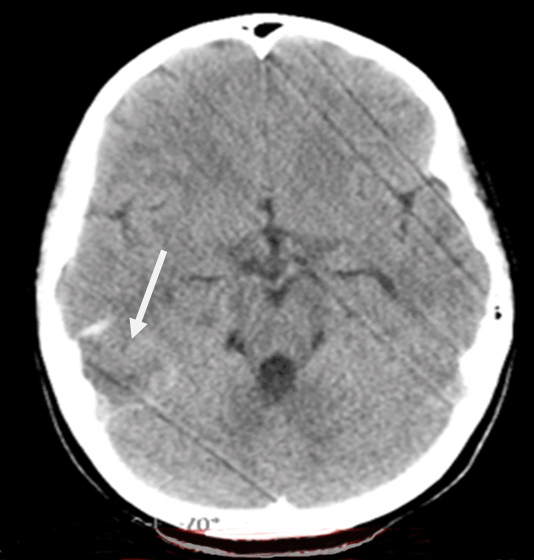
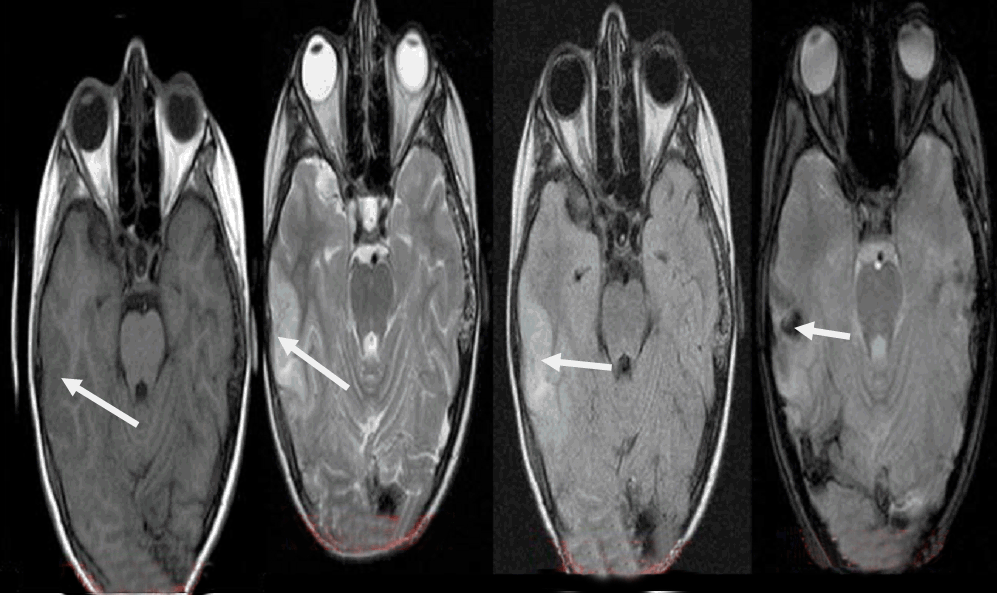
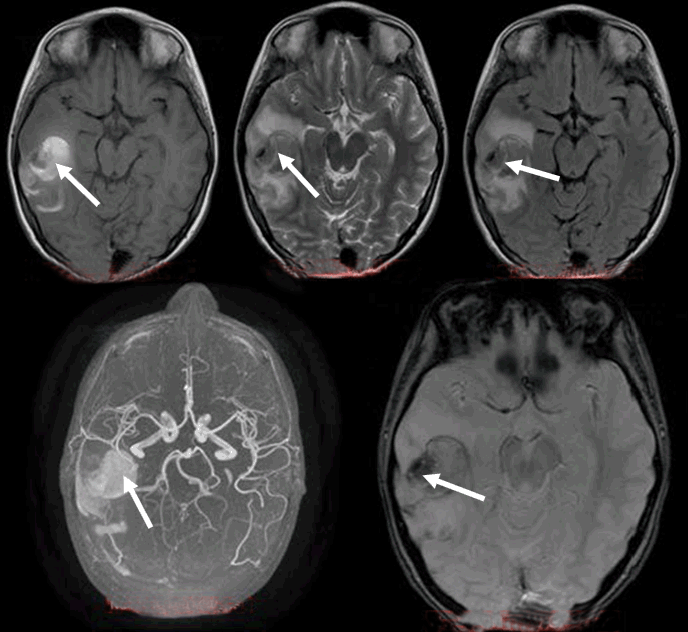
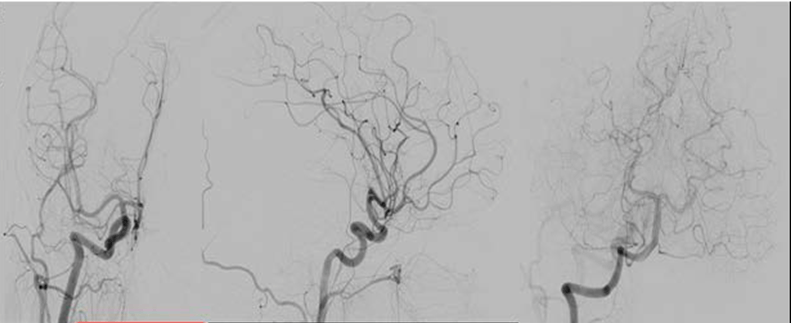
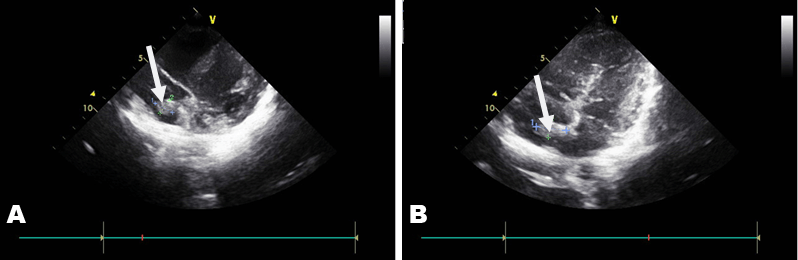
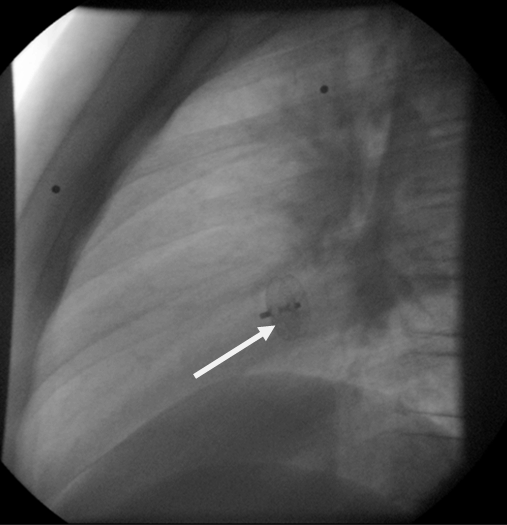
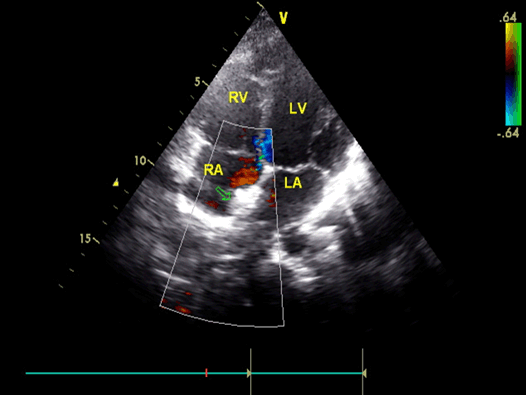
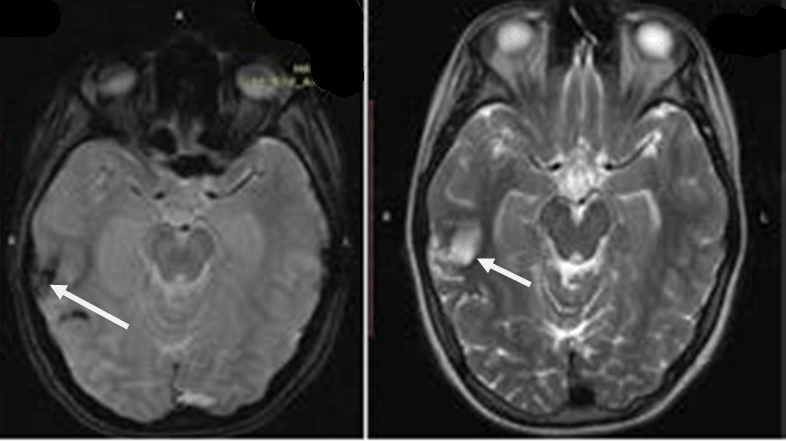
An 11-year-old girl presented with headache, vomiting, dizziness, dysphasia and gaze dedication for a few seconds. The initial computed tomography (CT) scan revealed intracerebral hematoma (ICH) in the right parieto-occipital region with perilesional edema (Figure 1). Patient was admitted in the neurosurgical clinic and was initiated on anticonvulsant medication. Neurological and ophthalmological examination did not reveal any focal deficits. Magnetic resonance imaging performed the same day revealed edematous configuration of the nearby gyri with concurrent presentation of hemorrhagic elements (Figure 2). An electroencephalography (EEG) study detected focal cerebral disturbances. A repeat MRI scan (with contrast) and magnetic resonance angiography (MRA), indicated a hemorrhagic infarct in the territory in a subacute phase with related edema (hemorrhagic stroke). Magnetic resonance angiography further recognized stenosis of the right middle cerebral artery (MCA) with obstruction of the posterior peripheral branches (Figure 3). Consequently, a digital subtraction angiography (DSA) from the femoral artery was performed which did not reveal underlying vascular abnormalities (Figure 4). A thorough investigation for hypercoagulable states (deficiencies of protein C and anti III, protein S, antithrombin and plasminogen, molecular studies for factor V Leiden, prothrombin 20210A, homocysteine, MTHFR gene mutations), and immunological – rheumatological conditions (HLA-51, c-ANCA, p-ANCA, anti – GBM, LA1 and LA2, Iß-2GPI, ACA IgM and IgG antibodies) did not reveal any abnormalities. An ultrasound study of the vessels of the lower extremities revealed an intraluminal thrombus of the left superficial femoral and popliteal vein. A thoroughly detailed investigation of patient’s history revealed a minor sports related blunt injury of the left lower extremity a day before the initial symptoms, which was associated with lower extremities ultrasound findings. Additionally, an echocardiogram visualized a thrombus (2x1.5 cm) attached to the right atrium in conjunction with patent foramen ovale (Figure 5). Due to the relative contraindication for thrombolysis, patient was initiated immediately on anticoagulation therapy with low molecular weight heparin and warfarin. Two days later, she developed acute symptoms of dyspnea and chest pain and a subsequent spiral thorax CT scan revealed pulmonary emboli at the left pulmonary artery, as long as the persistence of the atrial thrombus. Anticoagulation therapy was continued and a foramen ovale umbrella placement was later performed (Figure 6). Patient remained symptom free in the follow-up period and serial cardiac ultrasound examinations revealed gradual resolution of the right atrial thrombus (Figure 7). A few months later, a repeat MRI scan was performed, while the patient being neurologically normal. The examination verified the known lesion at the right temporal-occipital lobe region, which revealed characteristics, compatible with a chronic lesion. More specifically, the imaging of the lesion identified a territory with intermediate to hypo-intensity signal at FLAIR sequences and hemosiderin ring at T2-GRE sequences (Figure 8). | ||||||
| ||||||
|
| ||||||
|
| ||||||
| ||||||
| ||||||
| ||||||
| ||||||
| ||||||
|
DISCUSSION
| ||||||
|
Epidemiology: Definition of cryptogenic stroke | ||||||
|
Arterial ischemic stroke (AIS), with an estimated incidence of 1.1–4.3 per 100,000, is an important cause of morbidity and mortality in children and the recurrence risk is high [12].
It is defined as an acute clinical syndrome with a neurological deficit referable to a cerebral arterial territory and a brain MRI scan showing a corresponding area of acute infarct. A stroke is termed cryptogenic when its etiology cannot be attributed to any specific cause after an extensive search for the most common causes, such as atherosclerosis of the intracranial vessels, lacunar damage from hypertension, or embolus derived from a thrombus located in the left atrium, the left ventricular apex, or at the level of an ulcerated plaque of the aortic arch. | ||||||
| Etiology | ||||||
|
The etiology of AIS remains undetermined in a high proportion of children. Predisposing conditions for ischemic cerebrovascular accidents in children include congenital heart malformations (congenital cyanotic complex heart malformations or acquired heart disease), sickle cell disease, infections, and collagen tissue abnormalities [13], but around half occur in children who were previously well (cryptogenic stroke) [14]. It is well known from literature, that one of the most common conditions associated with AIS is congenital heart malformations (like patent foramen ovale) [15][16][17][18][19][20][21][22][23][24][25]. | ||||||
| Paradoxic embolism and stroke | ||||||
|
Recently, paradoxical embolism across the PFO was suggested as a possible etiology in some of these children [26]. Patent foramen ovale is reported, as an autopsy finding, to remain patent in about 25% of adults, thus presenting a potential passageway for paradoxical embolization. On some particular circumstances such as during Valsalva maneuver, which is reproduced by the act of defecating or coughing, the reversal of the physiologic inter-atrial pressure gradient results in right-to-left shunting across the PFO and contributes to the passage of embolic material. The prevalence of PFO was significantly higher in patients with cryptogenic stroke versus those with known causes of stroke (42% vs 7%), indicating that PFO is associated with cryptogenic stroke [27][28]. The association is documented in case reports [13][14][29][30][31][32][33]. However, the direct role of a PFO in stroke remains unclear [34]. In our case, the dual (and simultaneous) detection of thrombi in the deep venous system and the right atrium along with the rapid sequence of embolic events in the absence of other underlying pathological conditions, point out the paradoxical embolism through a patent PFO as the most plausible scenario for the ischemic stroke. | ||||||
| Prothrombotic disorders | ||||||
|
Prothrombotic disorders are frequently identified in pediatric patients with stroke [18] and case control studies demonstrate an association of arterial ischemic stroke in children with hereditary prothrombotic risk factors [15]. Another study reports prothrombotic abnormalities present in 20–50 % of children with arterial ischemic stroke [22][35]. Reasoning the coexistence of deep venous thrombosis and right atrial cavity thrombus in our patient with the absence of positive laboratory results for hypercoagulable disorders, we speculate either a transient hypercoagulable state, possibly associated with patient’s minor sport related injury or an unidentified mechanism by our thrombophilia screening. | ||||||
| Deep venous thrombosis and cryptogenic stroke | ||||||
|
Young adults with cryptogenic ischemic stroke are more likely to have both patent foramen ovale and pelvic deep vein thrombosis (DVT) than young adults with ischemic stroke of known cause. Young patients with cryptogenic transient ischemic attack (TIA) or stroke and patent foramen ovale (PFO) should be evaluated for lower-extremity or pelvic venous thrombosis, which would be an indication for anticoagulation. In this case, screening for underlying causes of cryptogenic stroke with ultrasound of the lower extremities revealed venous thrombosis The most probable releasing factor (and causative) of this event was a few days previously reported, sport’s related, minor lower extremity injury, a relationship supported by literature. | ||||||
| Right atrial thrombus and stroke | ||||||
| ||||||
| Treatment guidelines | ||||||
|
Young patients with cryptogenic TIA or stroke and PFO should be evaluated for lower-extremity or pelvic venous thrombosis, which would be an indication for anticoagulation. In the setting of a large acute stroke, however, full-dose anticoagulation is not recommended, and an inferior vena cava filter may be the safest alternative. In patients with cryptogenic TIA or stroke, a PFO, and DVT, guidelines from the ACCP currently recommend VKA therapy for three months and consideration of PFO closure rather than no VKA therapy or aspirin therapy. For patients with an ischemic stroke or TIA and both a PFO and a venous source of embolism, anticoagulation is indicated, depending on stroke characteristics (Class I; Level of Evidence A). When anticoagulation is contraindicated, an inferior vena cava filter is reasonable (Class IIa; Level of Evidence C). (New recommendation). In cases of concomitant venous and arterial embolism that paradoxical embolism is strongly considered, chronic anticoagulant therapy and an inferior vena cava filter can be justified to prevent further recurrences of both pulmonary and paradoxical embolism [37]. In the incident of right atrial thrombus, different treatment modalities are reported such as surgical thrombectomy, thrombolysis, anticoagulation therapy or observation only, the choice of which depended mainly on underlying etiology [36]. In this case, because of the hemorrhagic transformation of the cerebral stroke was an absolute contraindication for the initiation of fibrinolytic therapy, anticoagulation with subcutaneous low molecular weight warfarin along with foramen ovale umbrella placement constituted the selected treatment strategy. This strategy proved to be efficacious during the follow-up period. | ||||||
| Prognosis | ||||||
|
Regarding outcome data, it is referred that permanent moderate-to-severe motor or cognitive disabilities occur in 75–87% of children with stroke, and death occurs in 5–28% [25]. In this case, patient presented with indirect symptoms, such as headache and epileptic fit, these symptoms appearing late from stroke ictus, as seen from the initial MRI presentation of the stroke which was in the hemorrhagic transformation phase and the patient was not on anticoagulation therapy for any reason or did not report aspirin uptake. Furthermore, she did not suffer any major clinical and neurologic sequelae from the event. These findings, possibly due to the clinically silent anatomical area of the stroke, are contrary to the majority of the cases described in literature that have unfavorable neurological prognosis. | ||||||
|
CONCLUSION
| ||||||
|
Cryptogenic arterial ischemic stroke is a diagnosis of exclusion. The emergence of cases reporting patients with cryptogenic AIS harboring a patent foramen ovale, tends to reveal the presence of an associated causative factor. For all the aforementioned reasons, and because many of the aspects of the issue of AIS remain unresolved, we consider that it would be meaningful to present a case that mismatches a lot of aspects of the reported clinical cases and promotes a non-well elucidated pathophysiologic mechanism, supported widely by a lot of clinical and laboratory data. | ||||||
|
REFERENCES
| ||||||
| ||||||
|
[HTML Abstract]
[PDF Full Text]
|
|
Author Contributions
Dimitrios Panagopoulos – Substantial contributions to conception and design, Acquisition of data, Analysis and interpretation of data, Drafting the article, Revising it critically for important intellectual content, Final approval of the version to be published Sofia Loukopoulou – Substantial contributions to conception and design, Analysis and interpretation of data, Revising it critically for important intellectual content, Final approval of the version to be published Georgios Markogiannakis – Acquisition of data, Analysis and interpretation of data, Drafting the article, Final approval of the version to be published Nikos Eleftherakis – Substantial contributions to conception and design, Analysis and interpretation of data, Revising it critically for important intellectual content, Final approval of the version to be published |
|
Guarantor
The corresponding author is the guarantor of submission. |
|
Source of support
None |
|
Conflict of interest
Authors declare no conflict of interest. |
|
Copyright
© 2017 Dimitrios Panagopoulos et al. This article is distributed under the terms of Creative Commons Attribution License which permits unrestricted use, distribution and reproduction in any medium provided the original author(s) and original publisher are properly credited. Please see the copyright policy on the journal website for more information. |
|
|