|
 |
|
Case Report
| ||||||
| A rare case of a plastic foreign body (suction tip) within the soft tissues in the lingual aspect of the mandible | ||||||
| Eirini Boutiou1, Ioannis A. Ziogas2, Georgios Koloutsos3, Margarita Vafiadou4, Konstantinos Antoniades5 | ||||||
|
1Dental Student, School of Dentistry, Aristotle University of Thessaloniki, Thessaloniki, Greece
2Medical Student, School of Medicine, Aristotle University of Thessaloniki, Thessaloniki, Greece 3MD, DDS, MSc, PhD, Department of Oral and Maxillofacial Surgery, School of Dentistry, Aristotle University of Thessaloniki, Thessaloniki, Greece 4MD, DDS, Department of Oral and Maxillofacial Surgery, School of Dentistry, Aristotle University of Thessaloniki, Thessaloniki, Greece 5MD, DDS, PhD, Department of Oral and Maxillofacial Surgery, School of Dentistry, Aristotle University of Thessaloniki, Thessaloniki, Greece | ||||||
| ||||||
|
[HTML Abstract]
[PDF Full Text]
[Print This Article] [Similar article in Pumed] [Similar article in Google Scholar] 
|
| How to cite this article |
| Boutiou E, Ziogas IA, Koloutsos G, Vafiadou M, Antoniades K. A rare case of a plastic foreign body (suction tip) within the soft tissues in the lingual aspect of the mandible. Int J Case Rep Images 2017;8(11):735–738. |
|
ABSTRACT
| ||||||
|
Introduction: A rare occasion for the oral and maxillofacial surgeon as well as the dentist is to find a foreign object in a patient’s oral cavity. The underlying etiology may be a trauma, therapeutic interventions (dentoalveolar or implant surgery), or even a tooth dislocation. It may cause symptoms and thus be a reason for the patient to visit the dentist or the oral and maxillofacial surgeon or it can be an incidental finding on radiographic evaluation. Keywords: Adverse event, Foreign bodies, Maxillofacial surgery | ||||||
|
INTRODUCTION
| ||||||
|
Coming across a foreign body in the oral cavity is an uncommon event. Foreign bodies can be ingested, aspirated, inserted by certain patient’s habits or even accidentally placed by traumatic or iatrogenic injury. They can be fractured burr tips, dislocated teeth, dental implants or restorative material. Most of the times, the foreign bodies are made of plastic, metal, glass and they can be identified on X-ray, computed-tomography (CT) scan and magnetic resonance imaging (MRI) scan [1]. When it comes to the occurrence of an adverse event in relation with dental practice, oral surgery comes third [2]. At the same time cases with residual foreign bodies related to oral and maxillofacial surgery are extremely rare [3]. The majority of them can induce tissue reactions, such an abscess formation, or even a septicemic or a hemorrhagic event. They may also cause pain, discomfort, functional disorders and infection, but they do not usually threat patient’s life [1][4]. Retrieval of foreign objects can be a challenging and difficult aspect of the therapeutic approach, mostly due to the restricted access of the oral cavity and the close anatomic relations of the foreign body with vital structures, while normal anatomy may also come up with variations [1][5]. The aim of this case report is to present a case of a patient with an uncommon foreign object in the oral cavity that was identified during surgery. | ||||||
|
CASE REPORT
| ||||||
|
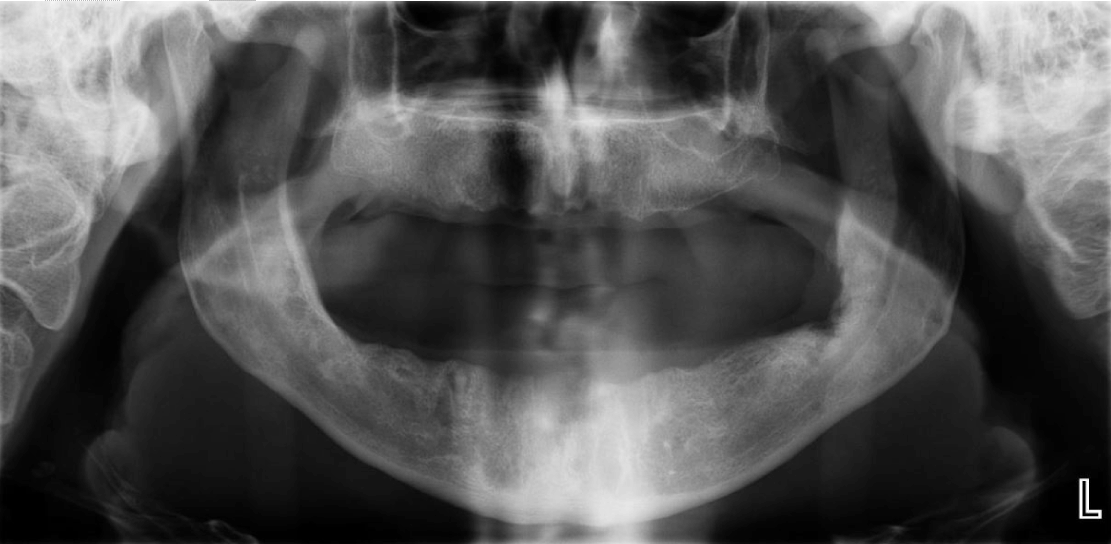
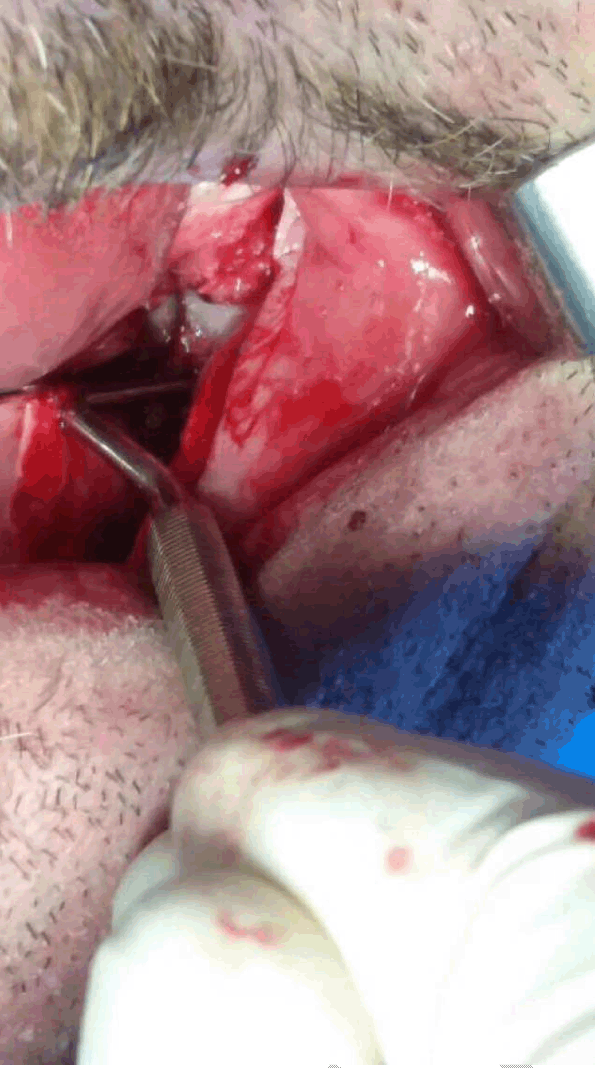
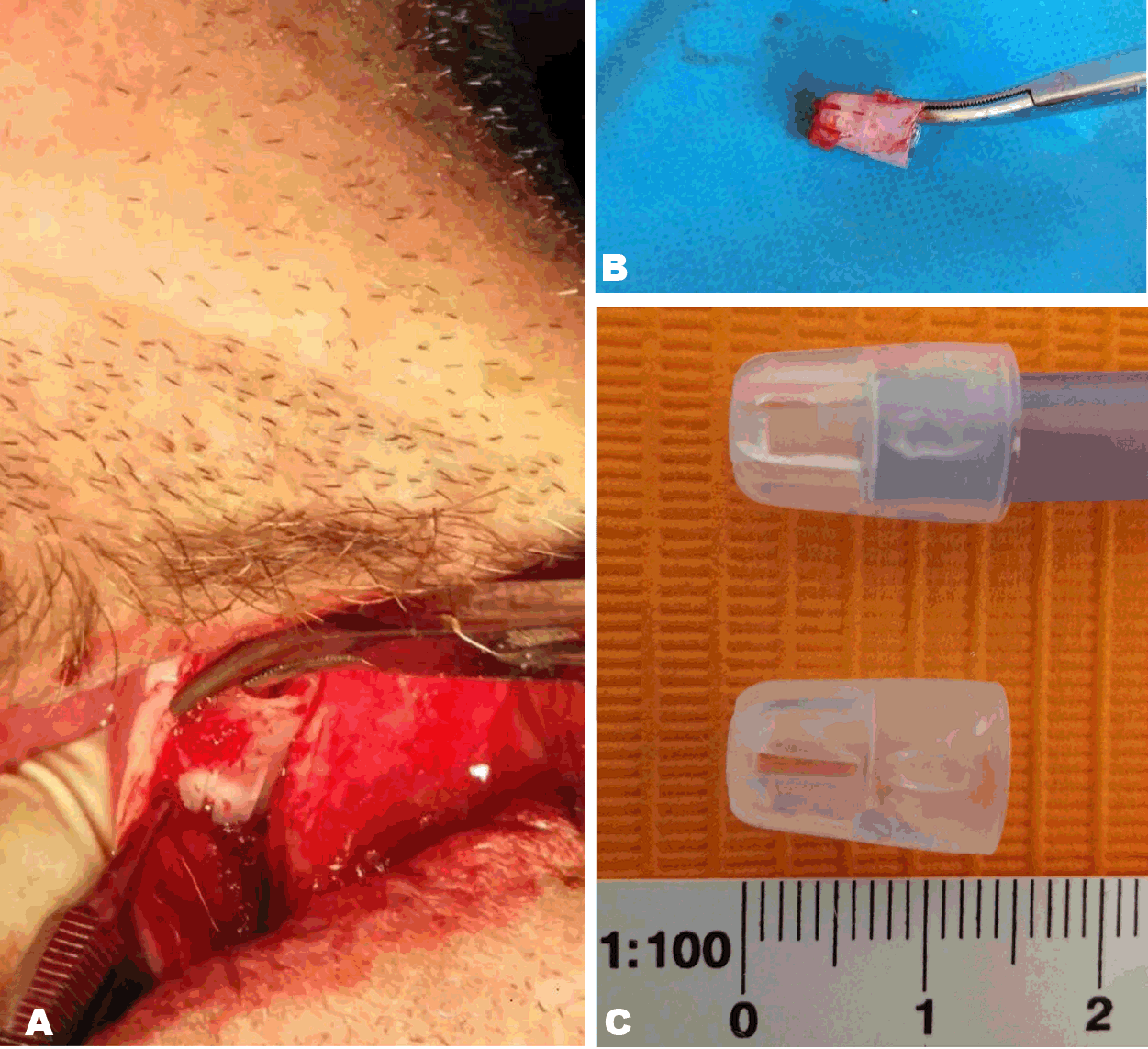
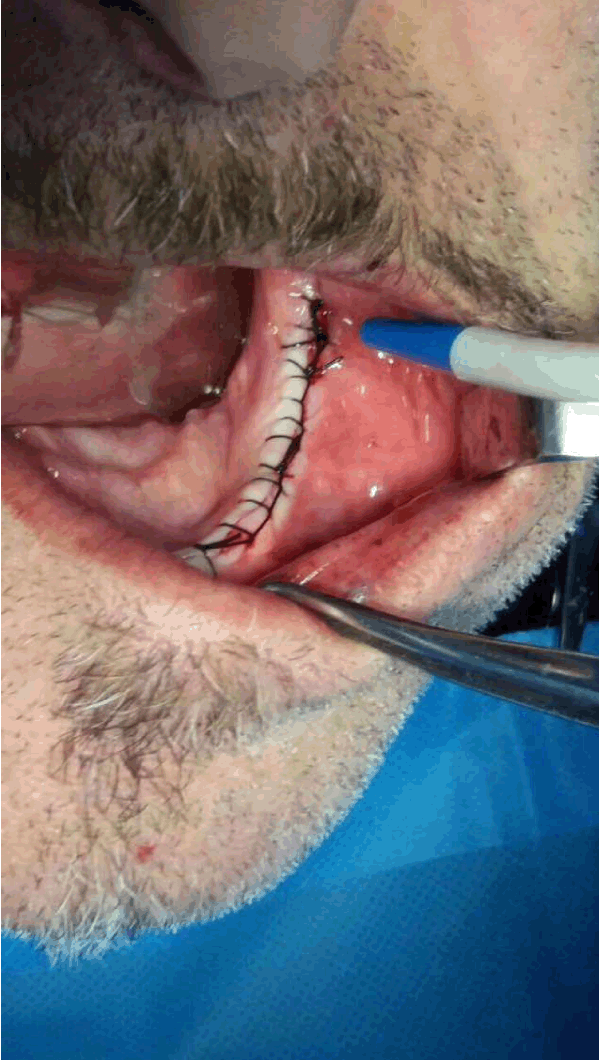
A 54-year-old edentulous man was referred to our outpatient department, complaining of a pain in the deep lingual aspect of the mandible on his left side, when he was wearing his lower denture. His past medical history was free and his surgical history only comprised of an appendicectomy. A bulge that was thought to be arising lingually of the left inferior 3rd molar post-extraction socket, right under the internal oblique line, was palpated upon clinical examination and the patient was scheduled for surgical removal of the diagnosed exostosis in order to relieve his relentless pain. Before proceeding in the operation, the patient was radiographically assessed, but nothing unusual was noticed (Figure 1). In the operating room, we performed left inferior alveolar nerve block along with several lingual and parietal local infusions. Then we went on with a longitudinal incision on the edentulous alveolar ridge of the left mandible and we raised the mucoalveolar flap. This revealed an absolutely normal bone surface and at the same time an abnormal mass within the corresponding soft tissues. Initially, it was thought to be a residual root of the 3rd molar (Figure 2), which was extracted several years before. This was a two step procedure for an initial unsuccessful attempt from a dentist was followed by an oral surgeon’s intervention. Then as we tried to pull out the foreign object, we surprisingly discovered that it was a suction tip (Figure 3). After removing it, the wound was closed with continuous locked suture (Figure 4). The patient was prescribed antibiotics and analgesics and was discharged. | ||||||
| ||||||
| ||||||
| ||||||
| ||||||
|
DISCUSSION
| ||||||
|
In this case, an adverse event occurred by the previous two step dentist and oral surgeon’s intervention, during the extraction of the lower 3rd molar. Unfortunately, we cannot be aware of what exactly happened during this procedure. Thus, a meticulous history of the patient, which can provide more accurate information about the etiology, as well as radiographs are the cornerstone of delivering high quality medical therapy. Radiographs, in particular, can be found very useful, especially in case of a radiopaque foreign body [5]. Regarding radiolucent objects, such as those made of plastic or wood, CT scan may be the most reliable method. CT scan can also provide information about their relationship with the surrounding anatomical structures [6]. We suggest taking CT preoperatively in case we are aware of a foreign body existence. The fact is that the patient was totally unaware of this and the panoramic X-ray was not indicative of such a case. He was referred to us in order to remove surgically a lingual exostosis. So, no CT scan was prescribed. Clinical presentation can also vary according to the type of the foreign object; steel and glass may not cause severe inflammation, but organic materials can lead to secondary infection with formation of an abscess, or a fistula [3][7]. Gui et al. [4] reported an increase in the incidence of identifying foreign bodies in the deep maxillofacial area during the last years. Also, it is suggested that all foreign bodies presenting with clinical manifestations or found near vital structures should be removed in order to prevent further complications. A problem that an oral and maxillofacial surgeon may face during the removal procedure is the tendency of the foreign objects to move within the soft tissues, thus implying difficulties due to its mobility. Sometimes fibrous connective tissue can develop around them, just as in this case, which may prevent further movements, hence providing an obvious advantage to the surgeon. As far as removal of the foreign bodies is concerned, a computer-based image guided navigation system can be beneficial for the surgeon. After acquiring intraoperative three dimensional imaging data of the anatomy, injury to anatomical areas can be prevented and preoperative planning can be improved. Additionally, operating time may be decreased with the simultaneous precision and accuracy of a minimally invasive procedure. However, its implementation depends on the location of the foreign object and as such it cannot be universal [1]. Generally, in order to achieve high-level patient safety, the dentist should be careful enough to prevent adverse events from happening. | ||||||
|
CONCLUSION
| ||||||
|
The dentists and the surgeons in general should be very careful, when treating their patients, so as not to leave a foreign object in the oral cavity. However, if an adverse event occurs, the patient should be informed accordingly. | ||||||
|
REFERENCES
| ||||||
| ||||||
|
[HTML Abstract]
[PDF Full Text]
|
|
Author Contributions
Eirini Boutiou – Substantial contributions to conception and design, Acquisition of data, Acquisition of data, Analysis and interpretation of data, Drafting the article, Revising it critically for important intellectual content, Final approval of the version to be published Ioannis A. Ziogas – Acquisition of data, Analysis and interpretation of data, Drafting the article, Revising it critically for important intellectual content, Final approval of the version to be published Georgios Koloutsos – Substantial contributions to conception and design, Acquisition of data, Acquisition of data, Drafting the article, Revising it critically for important intellectual content, Final approval of the version to be published Margarita Vafiadou – Substantial contributions to conception and design, Acquisition of data, Acquisition of data, Revising it critically for important intellectual content, Final approval of the version to be published Konstantinos Antoniades – Substantial contributions to conception and design, Acquisition of data, Drafting the article, Revising it critically for important intellectual content, Final approval of the version to be published |
|
Guarantor
The corresponding author is the guarantor of submission. |
|
Source of support
None |
|
Conflict of interest
Authors declare no conflict of interest. |
|
Copyright
© 2017 Eirini Boutiou et al. This article is distributed under the terms of Creative Commons Attribution License which permits unrestricted use, distribution and reproduction in any medium provided the original author(s) and original publisher are properly credited. Please see the copyright policy on the journal website for more information. |
|
|