|
 |
|
Case Report
| ||||||
| Paraplegia as initial presentation of acute myeloid leukemia: A case report | ||||||
| Adama Isah Ladu1, Aisha Abba Mohammed2, Halima Talba3, Yakaru Kundili4, Yakura Abba Kawu3, Ridhwan Aliyu Tukur3 | ||||||
|
1MBBS, MSc, FMC Path: Lecturer 1/ Consultant Haematologist
2MBBS, FMC Path: Lecturer 1/ Consultant Haematologist 3MBBS, Registrar 4MBBS, Senior Registrar | ||||||
| ||||||
|
[HTML Abstract]
[PDF Full Text]
[Print This Article] [Similar article in Pumed] [Similar article in Google Scholar] 
|
| How to cite this article |
| Ladu AI, Abba AM, Talba H, Kundili Y, Abba Kawu Y, Tukur RA. Paraplegia as initial presentation of acute myeloid leukemia: A case report. Int J Case Rep Images 2017;8():703–706. |
|
ABSTRACT
| ||||||
|
Introduction: Acute myeloid leukemia (AML) represents a state of dysregulated clonal expansion of immature myeloid progenitor cells with arrest of differentiation at a particular stage. Involvement of the central nervous system (CNS) may result acutely from the disease at the initial diagnosis, and the symptoms range from muscle weakness, paresthesias, and hypoesthesia to fecal and urinary incontinence. Paraplegia is an extremely rare initial presentation of undiagnosed leukemia. Keywords: Acute myeloid leukemia, Central nervous system, Paraplegia | ||||||
|
INTRODUCTION
| ||||||
|
Acute myeloid leukemia (AML) represents a state of dysregulated clonal expansion of immature myeloid progenitor cells with arrest of differentiation at a particular stage, it accounts for 15–30% of all cases of newly diagnosed cases of leukemia [1]. The condition is more frequently encountered in infants and adolescents. Clinical features include pallor, easy fatigability, lethargy, bleeding and fever. Organ infiltration is less frequent compared to acute lymphoblastic leukemia (ALL). However, AML is more likely to produce aggregates of leukemic cells known as chloroma; these are frequently encountered in the head and neck region, the central nervous system (CNS), where they may produce neurological symptoms [2]. Symptoms range from muscle weakness, paresthesias, hypoesthesia to fecal and urinary incontinence. Paraplegia due to epidural mass is an extremely rare presentation of undiagnosed leukemia [3]. The thoracic region is the most frequently involved region, followed by the lumbar region. The sacral cord is the rarest region implicated [4][5]. Here, we present a case of AML presenting with paraplegia at the initial diagnosis. | ||||||
|
CASE REPORT
| ||||||
|
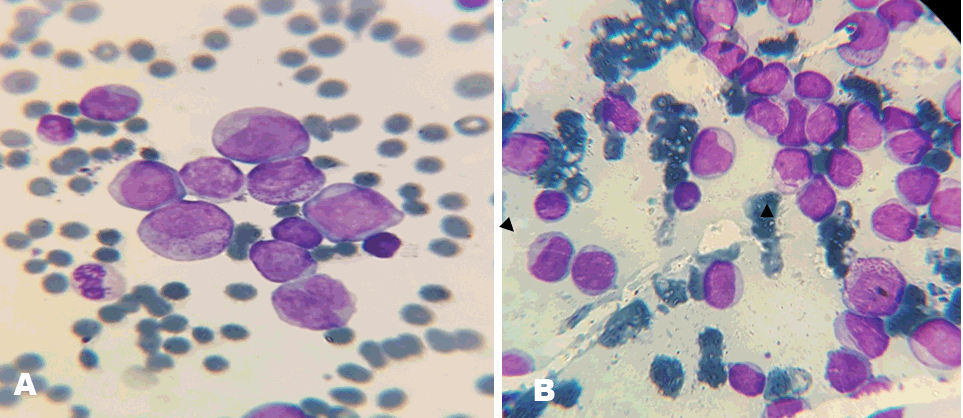
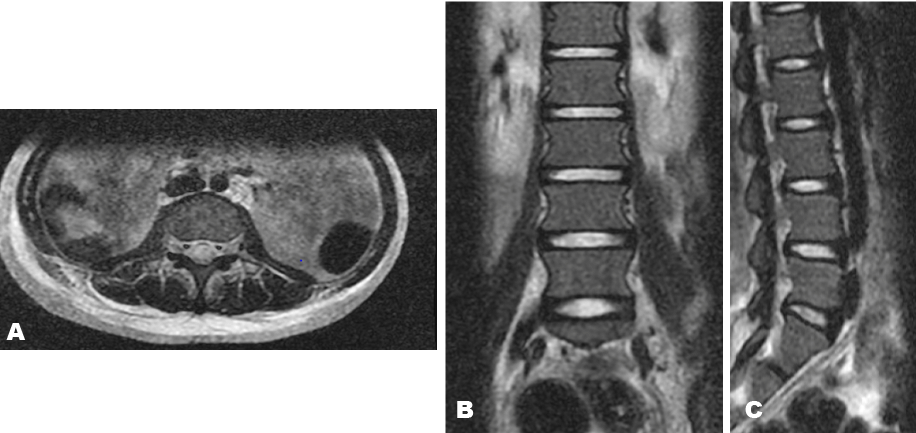
A 15-year-old girl was seen by the medical team with history of fever, malaise and lower back pain, she had two units of blood transfused along with antibiotics and antimalarials for severe malaria and presumed septicemia, however, two weeks later, she developed acute urinary and fecal incontinence, and a day later developed inability to move both lower limbs. There was no preceding history of trauma; no associated history of paresthesias, numbness, visual blurring. On physical examination, she was febrile at 38.2°C, pale, anicteric. No lymphadenopathy was noted. Her chest was clear to auscultation. Cardiovascular and abdominal examinations were unremarkable. There was vertebral tenderness involving the lower lumber to sacral region. The examination of both lower limbs revealed decreased tone and reflexes with bilateral extensor reflexes and power of 0/5. There was loss of sensation around the perianal region with absent anal tone. Cranial nerve and sensory examination were normal. Complete blood count revealed hematocrit of 21%, total white cell count of 29.3x109/L (myeloblast 47%, neutrophil 29%, eosinophil 1%, lymphocyte 20%, monocyte 3%) and platelet 90x109/L. Peripheral blood film (PBF) showed leukocytosis with variable number of myeloblast (Figure 1A). Bone marrow aspiration (BMA) cytology showed a hypercellular marrow with maturation arrest along the myeloid cell line. The myelogram showed a myeloblast count of >20% with maturation arrest at the myelocytic stage, some of the blast cells contained Auer rods (Figure 1B), megakaryocytes were reduced. Both PBF and BMA were consistent with acute myeloid leukemia (AML) FAB M-4 subtype. Cerebrospinal fluid analysis (CSF) analysis was negative for malignant cells. A lumbosacral X-ray was normal. Magnetic resonance imaging of the lumbosacral region was obtained in the axial, sagittal and coronal view. Both T1- and T2-weighted sequences showed no signal intensity in the spinal cord, theca and cauda, with normal signal intensity involving the intervertebral disc (Figure 2). An assessment of cauda equina syndrome secondary to leukemic infiltration was made. The patient was commenced on supportive therapy and induction chemotherapy using daunorubicin 45 mg/m2 days 1–3 and cytosine arabinoside 200 mg daily days 1–7. However, patient succumbed to her disease and passed away 10 days into treatment as a result of respiratory complication. | ||||||
| ||||||
| ||||||
|
DISCUSSION
| ||||||
|
The exact incidence of central nervous system (CNS) involvement in patients with AML is unknown, but is lower compared with the incidence in children and adults with ALL; for that reason routine CSF examination is not performed as part of the diagnostic workup in asymptomatic patients [6][7]. Involvement of the CNS may result acutely from the disease at the diagnosis, as in the index case; from relapse of the disease or from complications of agents used in treatment. It may be classified into three as CNS 1 (when there is no blast in the CSF), CNS 2 (< 5 WBC/ml of CSF with blast cells) and CNS 3 (>5 WBC/ml of CSF with blast cells or signs of cranial nerve palsy, meningeal involvement) [8]. The presence of certain factors has been associated with increased risk of neurological complication. These include hyperleukocytosis, high level of lactate dehydrogenase and high expression of CD56 [7]. In a single institution study of 290 pediatric patients with AML, the authors found significant relation between CNS involvement in patients with AML having the cytogenetic abnormality Inv 16, t [9], or AML M4 and M5 subtype. The authors concluded that CNS involvement is common in those with favorable cytogenetics [8]. As mentioned above, the PBF and BMA cytology of the index patient was in keeping with AML M4 subtype, and therefore belonged to a high risk group for CNS involvement. Several mechanism have been put forward to explain the pathogenesis of CNS involvement in leukemia, this include contamination of the CSF through the choroid plexus or infiltration of the cerebral parenchyma through brain capillaries; direct extension of aggregates of leukemic cells called chloroma, from the bone marrow through the cortical bones into the spinal cord, may cause symptoms as a result of mass effect on neural tissue [9]. Hyperleukocytosis with thrombosis may result in leukostasis and consequently poor CNS perfusion. Intracranial hemorrhage with focal neurological deficit may also arise. Hemorrhage into the spinal canal can occur following diagnostic procedures in cases presenting with thrombocytopenia [9]. In the index case, the CSF was negative for malignant cells and the MRI scan showed no obvious pathology. The presence of urinary and fecal incontinence indicates pathology involving the sacral canal. Relatively small tumor in this region may manifest with profound symptoms, unfortunately such tumors can be particularly difficult to image [9]. Consequently, the absence of findings on MRI scan does not completely exclude cord compression as seen in the index case report. The involvement of CNS may be without symptoms. In symptomatic patients, the clinical picture will depend on which part of the CNS is involved. Features of advanced disease include irritability, headaches, seizures symptoms of raised intracranial pressure and cord compression [7][9]. Amongst the leukemia, AML is the most common leukemia to produce cord compression; however, it is a rare initial presentation of AML [4]. The patient may presents with pain in the back, abdomen, lower limbs and perianal region. Muscle weakness to paraplegia may also be present. Fecal and urinary incontinence often represents dangerous signs as in all cases of cord compression [10]. Therefore, the acute physician needs to have a high index of suspicion of AML in young patients presenting with neurological symptoms, and make every effort to diagnose it. Early identification and prompt intervention can prevent the development of irreparable neurological complications. This is reflected in this case report, where the patient had developed irreversible neurological deficit prior to referral to the hematology team. Therefore, the presence of laboratory evidence of AML can be used to commence active treatment and prevent further delay. | ||||||
|
CONCLUSION
| ||||||
|
In conclusion, central nervous system involvement is a rare initial presentation of acute myeloid leukemia. Several pathogenic mechanisms have been implicated including direct extension of leukemic aggregate resulting in compressive effect on the neural tissue. The absence of abnormality on magnetic resonance imaging (scan) does not rule out spinal cord involvement. Consequently, late recognition may delay treatment and lead to irreversible neurological complication. | ||||||
|
REFERENCES
| ||||||
| ||||||
|
[HTML Abstract]
[PDF Full Text]
|
|
Author Contributions
Adama Isah Ladu – Substantial contributions to conception and design, Revising it critically for important intellectual content, Final approval of the version to be published Aisha Abba Mohammed – Substantial contributions to conception and design, Revising it critically for important intellectual content, Final approval of the version to be published Halima Talba – Acquisition of data, Drafting the article, Final approval of the version to be published Yakaru Kundili – Acquisition of data, Drafting the article, Final approval of the version to be published Yakura Abba Kawu – Acquisition of data, Drafting the article, Final approval of the version to be published Ridhwan Aliyu Tukur – Acquisition of data, Drafting the article, Final approval of the version to be published |
|
Guarantor
The corresponding author is the guarantor of submission. |
|
Source of support
None |
|
Conflict of interest
Authors declare no conflict of interest. |
|
Copyright
© 2017 Adama Isah Ladu et al. This article is distributed under the terms of Creative Commons Attribution License which permits unrestricted use, distribution and reproduction in any medium provided the original author(s) and original publisher are properly credited. Please see the copyright policy on the journal website for more information. |
|
|