|

|
 |
|
Case Report
| ||||||
| Metastasis in neck of clear cell renal carcinoma: A case report | ||||||
| Andrés C. Limardo1, Emilio Soza1, Adrían Ortega1, Rubén Padín1,2 | ||||||
|
1Surgeon of Head and Neck of the Prof. A. Posadas Hospital (El Palomar, Buenos Aires, Argentina).
2Chief of Head and Neck Surgery Section of the Prof. A. Posadas Hospital (El Palomar, Buenos Aires, Argentina). | ||||||
| ||||||
|
[HTML Abstract]
[PDF Full Text]
[Print This Article]
[Similar article in Pumed] [Similar article in Google Scholar] 
|
| How to cite this article |
| Limardo AC, Soza E, Ortega A, Padín R. Metastasis in neck of clear cell renal carcinoma: A case report. Int J Case Rep Images 2016;7(12):844–847. |
|
Abstract
|
|
Introduction:
Clear cell renal carcinoma (ccRc) accounts for 3% of all neoplasms of the adults. It is the third most frequent cause of tumors that metastasize to head and neck, after primary carcinoma of the lung and breast. The most frequent areas of metastasis are the lung and bone. In patients with clear cell renal carcinoma, head and neck lesions should make us suspicious of metastatic processes.
Case Report: A 50-year-old male presented with a right supraclavicular swelling. Computed tomography (CT) scan revealed left renal primary typical tumor. There was a secondary lesion in the right supraclavicular hollow. Fine needle aspiration (FNA) of right supraclavicular tumor showed metastasis of well differentiated adenocarcinoma. After evaluation by urology and oncology, it was decided to give radiotherapy and subsequent treatment with immunotherapy. Resection of cervical tumor of level V and right cervical lymphadenectomy of level II, III, IV, V was done on third day of hospitalization. Microscopic study revealed clear cell renal carcinoma. Conclusion: The patients with clear cell renal carcinoma, and head and neck tumors, should make us suspicious of metastatic processes. | |
|
Keywords:
Clear cell renal carcinoma, Supraclavicular neoplasia, Metastases of clear cell renal carcinoma
| |
|
Introduction
| ||||||
|
Clear cell renal carcinoma (ccRc) accounts for 3% of all neoplasms of the adult. The most frequent place of metastases is lung and bone [1]. The natural history of renal cell carcinoma is highly variable. Metastasis may present decades after removal of the primary disease. However, only 1% patients with renal cell carcinoma have metastasis confined only to the head and neck. Solitary cervical metastatic mass is rare. Currently, there is no explanation for its routes of progression. It even seems to be non-existent based on the rare tumor implant sites [2]. We describe the resolution of a case of solitary mass in the supraclavicular hollow in a patient with ccRc. | ||||||
|
Case Report
| ||||||
|
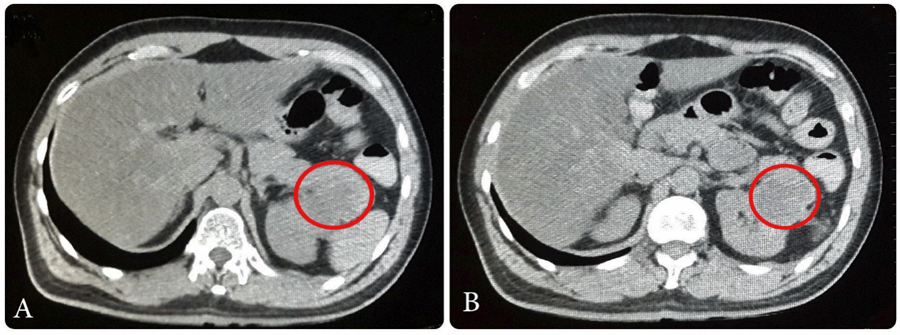
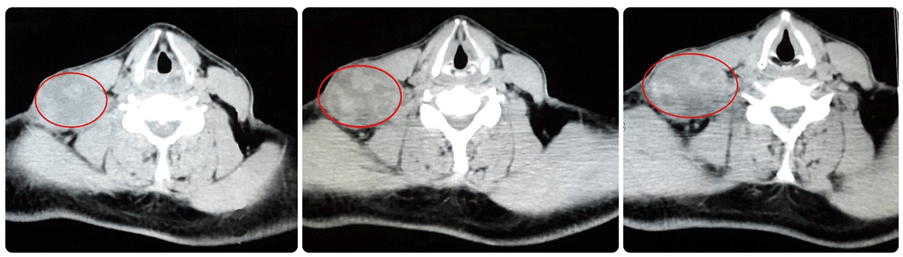
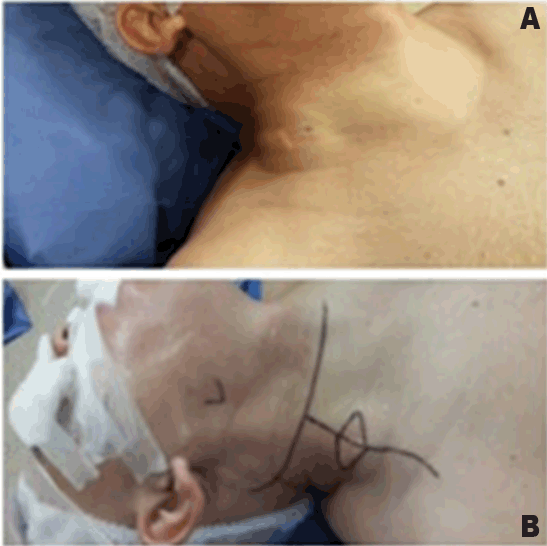
A 50-year-old male presented with history of hypertension and hemorrhagic stroke in 2012 with sequel of right hemiparesis. The patient presented with a right supraclavicular firm, incompressible and immobile swelling of 55 mm. Body computed tomography (CT) with contrast was done. It showed left renal mass in lower pole measuring 65x38 mm as a focal bulging of the renal contour, mainly isodense to the renal parenchyma. The corticomedullary phase clearly showed renal malignancy which was moderately and heterogeneously enhancing (Figure 1). Heterogeneous contrast enhancement on imaging should always suggest renal malignancy preoperatively. There was a secondary heterogeneous lesion in the right supraclavicular hollow measuring 56x42 mm with central necrosis (Figure 2). Fine needle aspiration (FNA) of right supraclavicular tumor showed metastasis of well differentiated adenocarcinoma. His biopsy was unsatisfactory. He was evaluated by urology and oncology services so it was decided to like radiotherapy for local control and subsequen treatment with interferon α 5 million IU/week and sunitinib 50 mg/day for one year for down staging (six weeks cycles). Treatment was started with pazopanib 800 mg/day. The lesion increased in size for six months. He had poor clinical response. He was evaluated by head and neck surgeons and surgery was done: resection of cervical tumor of level V and right cervical lymphadenectomy of levels II, III, IV, V (Figure 3). The surgery was done on third day of hospitalization. Ambulatory monitoring was done by head and neck and oncology services. Microscopic study of respected lymph nodes revealed clear cell renal carcinoma (ccRc). After 45 days, laparoscopic nephrectomy was performed. The immunohistochemical profile was the same for both the neck and renal tumor. No recurrences occurred after two years of follow-up. | ||||||
|
| ||||||
| ||||||
| ||||||
|
Discussion
| ||||||
|
The clear cell renal carcinoma (ccRc) is very often diagnosed in advanced stages. It is associated with high mortality. This tumor is usually resistant to chemotherapy and radiotherapy. Treatment with immunotherapy is the best option. An increase of incidence has been observed from 1975, perhaps as a result of the availability of computed tomography that has allowed identifying incidental small masses. Tumors presents resistance to chemotherapy. The reason for this is not known. The treatments is effective in less than 6% patients [2]. This may be due to expression of resistant proteins to drugs [3] . The tumor is also observed to be resistant to radiotherapy. Tumor requires extremely high doses of radiation that are not tolerated due to their indirect effect, reserving its use only for palliative care. This resistance is explained due to presence of a pseudocapsule and a high degree of vascularization (only surpassed by glioblastoma multiform), that confers the tumor tolerance to hypoxia. Other alternatives a treatment is immunotherapy [4]. The participation of the immune system in the ccRC has been demonstrated. Based on the cases of spontaneous remission of metastasis, the presence of infiltrates of lymphocytes within the tumor, the increase of dendritic cells presenters of antigens in the tumor and the treatment of advantaged stages with experimental vaccine [5]. The immunotherapy with IL-2, GM-CSF and interferon is shown to be effective in 24% of cases. Unfortunately, in the ccRc we do not know a predictable pattern of dissemination to other organs, like in the rest of the urological tumors. It prevents establishing the stage and a plan of follow-up, as well as the treatment of the systemic disease. Also, this makes suspect that a pattern of dissemination by hematopoetic route predominates, although many times it does not have an anatomical correlation. It is postulated that when the tumor invades very vascularized neighboring structures the metastasis to other organs. For example, the direct invasion to adjacent structures irrigated by mesentery or the presence of arterial venous short circuits, allows the tumor cells the access to gastrointestinal tract. Through paravertebral plexus, it could accede to the axial skeleton and regions such as head and neck. The formation of collateral circulation can facilitate the extension to thyroid and neck, explaining these cases of metastasis [6]. With regard to the metastases in the genitals, it would be possible to explaining by retrograde growth of the tumor at level of the ovarian or spermatic vein. To be able to metastasize to the skin and extremities, it would be possible to be acceded through caval venous system without settling down in lung. The most frequent areas of metastasis are the lung and bone, however, it can be migrated to any part of the body [7]. This tumor is characterized by many clinical symptoms. It has been associated with other tumors, greater histologic degree and worse prognosis [8]. Natural history is very variable [9]. The metastasis can be present at the moment of diagnosis, although these can appear decades after the first tumor. The presence of delayed metastasis (>10 years) happens in 4.7% and 11% of the cases. The cases with solitary metastasis are only diagnosed in 1.6–3.6% cases. In these cases due to chemotherapy and radiotherapy resistance, the surgery is the best option if the tumor can be resected. It leaves minimal functional sequels. For cases of atypical metastasis, the sober-life after surgery is similar to tumors with metastasis in frequent sites [10]. The patients with clear cell renal carcinoma and head and neck tumors, should make us suspicious of metastatic processes. | ||||||
|
Conclusion
| ||||||
|
Clear cell renal carcinoma (ccRc) accounts for 3% of all neoplasms of the adults. The most frequent place of metastases is lung and bone. Metastases in head and neck regions are rare. The ccRc is diagnosed very often in advanced stages. It is associated with high mortality. Unfortunately, in the ccRc, we do not know a predictable pattern of dissemination to other organs, like in the rest of the urological tumors. The patients with clear cell renal carcinoma, and head and neck tumors, should make us suspicious of metastatic processes. | ||||||
|
References
| ||||||
| ||||||
|
[HTML Abstract]
[PDF Full Text]
|
|
Author Contributions
Andrés C. Limardo – Substantial contributions to conception and design, Acquisition of data, Analysis and interpretation of data, Drafting the article, Revising it critically for important intellectual content, Final approval of the version to be published Emilio Soza – Substantial contributions to conception and design, Acquisition of data, Analysis and interpretation of data, Drafting the article, Revising it critically for important intellectual content, Final approval of the version to be published Adrían Ortega – Substantial contributions to conception and design, Acquisition of data, Analysis and interpretation of data, Drafting the article, Revising it critically for important intellectual content, Final approval of the version to be published Rubén Padín – Substantial contributions to conception and design, Acquisition of data, Analysis and interpretation of data, Drafting the article, Revising it critically for important intellectual content, Final approval of the version to be published |
|
Guarantor of submission
The corresponding author is the guarantor of submission. |
|
Source of support
None |
|
Conflict of interest
Authors declare no conflict of interest. |
|
Copyright
© 2016 Andrés C. Limardo et al. This article is distributed under the terms of Creative Commons Attribution License which permits unrestricted use, distribution and reproduction in any medium provided the original author(s) and original publisher are properly credited. Please see the copyright policy on the journal website for more information. |
|
|
|
About The Authors
| |||
| |||
| |||
| |||
| |||