|

|
 |
|
Case Report
| ||||||
| Vulvar bilharzia on nine-year old girl: A case report | ||||||
| Pauline Dioussé1, Haby Dione1, Mariama Bammo1, Chérif Dial2, Mariétou Thiam3, Aissatou Amy Diamé4, Bernard Marcel Diop3, Mamadou Mourtalla Ka3 | ||||||
|
1MD, Department of Dermatology-Venereology, Faculty of Health Sciences, Thies University, Thies, Senegal.
2MD, Department of pathology, University Cheikh Anta Diop, Dakar, Senegal. 3MD, Department of Health Sciences, Thies University, Senegal. 4MD, Department of Urology, Regional Hospital, Thies, Senegal. | ||||||
| ||||||
|
[HTML Abstract]
[PDF Full Text]
[Print This Article]
[Similar article in Pumed] [Similar article in Google Scholar] 
|
| How to cite this article |
| Dioussé P, Dione H, Bammo M, Dial C, Thiam M, Diamé AA, Diop BM, Ka MM. Vulvar bilharzia on nine-year old girl: A case report. Int J Case Rep Images 2016;7(11):724–728. |
|
Abstract
|
|
Introduction:
In Senegal, West Africa, the overall prevalence of schistosomiasis varies from 0.3 to 1%. A major focus of schistosomiasis urogenital is known around the banks of the Senegal River where the average infestation rate reached 71.8%. Vulvar location is rare, the case of uro-digestive is even more so.
Case Report: It was a girl aged 9, from a village situated on the banks of the Senegal River, received for swollen labia lasting for three years. There was a notion of contact with the river water. At dermatological examination, she had an itchy swelling of the large labia, small labia, clitoris, the groin with a palpation papulonodular, fibrous. There was hyper eosinophilia. Dermal histology showed under an acanthotic epidermis, a granulomatous inflammatory reaction around the dermis of an infestation of viable eggs of Schistosoma species terminal spur characteristic of Schistosoma haematobium. The abdominal-pelvic ultrasound revealed bilateral ureteral hydronephrosis The computed tomography urography without product injection noted an irregular parietal calcification of the bladder, ureters under pyelics, urethra, rectum, sigmoid, and the left colon with segmental dilatation of the ureters. She was put under praziquantel (40 mg/kg in two spaced taken 15 days). The outcome was favorable with a clear regression of swelling after one month. Resection of residual disease was made. Conclusion: We reported a vulvar bilharzia, remarkable by a clinical presentation, an urogenital tract case and the multidisciplinary management. | |
|
Keywords:
Children, Schistosoma haematobium, Vulvar
| |
|
Introduction
| ||||||
|
Schistosomiasis or bilharzia is the second global parasitic disease after malaria, it affects 239 million people in 2009 and 80–90% of them live in Africa [1]. In Senegal, the overall prevalence of schistosomiasis varies from 0.3–1%. A major focus is known around the banks of the Senegal River where the average infestation rate reached 71.8% [2] [3]. Vulvar location is rare, few case series have been described in literature [4][5][6][7][8]. It results in papules and nodular lesions. Treatment is primarily medical and for large lesions, it must always be followed by surgical resection of residual lesions. | ||||||
|
Case Report
| ||||||
|
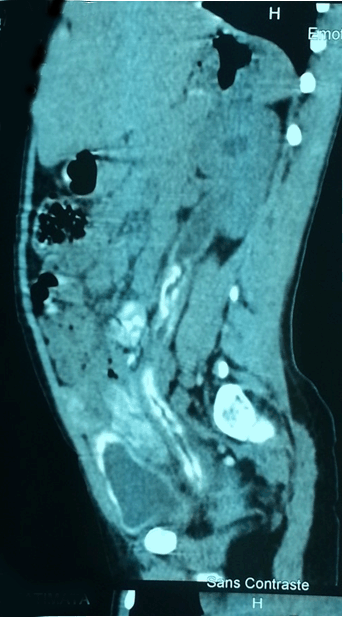
A nine-year-old girl from a village situated on the banks of the Senegal River received in dermatological consultation for swollen labia evolving for three years. She would get an urinary schistosomiasis four years ago. It was found in her personal history, frequent bathing in the river water. She was treated by unspecified drugs according to her parents. She had a good condition with a weight of 22 kg for a height of 1,26 cm with a BMI 13.90 kg/m2, corresponding to normal but close to the area of underweight build. At dermatological examination, the patient had an itchy swelling of the big labia, small labia, clitoris, and groin folds of the aspect of papulo-fibrous and nodular on palpation (Figure 1). No abnormalities found in the gastrointestinal examination. The rest of the examination was unremarkable. Diagnostic hypotheses were discussed: cutaneous calcinosis, vulvar tuberculosis, cutaneous sarcoidosis and cutaneous schistosomiasis. The blood count showed anemia (hemoglobin 8 g/dl), normocytic (MCV 80.9 fl), normocytic (MCHC 33.2 g/dl) and hypereosinophilia 21.1%. The erythrocyte sedimentation rate was accelerated, CRP was positive. The parasitological examination of urine was normal. The skin histology showing under acanthotic epidermis, inflammatory granulomatous reaction around bilharzia viable eggs of Schistosoma haematobium, grouped into small clusters of a few elements surrounded by lymphocytes plasma cells, eosinophil's polynuclear, histiocytes, épithélo?des and multi-nucleated. Images of microabscesses were visible around Schistosoma eggs in entering the squamous epithelium to the keratin layer (Figure 2) and (Figure 3). The diagnosis of vulvar skin bilharzia was set. The abdominal pelvic ultra sound showed a bilateral ureteral hydronephrosis, uroscanner without product injection noted an irregular parietal calcification of the bladder, ureters under pyelic, urethra, rectum, sigmoid colon and left with segmental dilatation of the ureters and expansions moderate bilateral pelvicalyceal (Figure 4). The remaining tests were normal: IDR tuberculin, fasting glucose, HBsAg, TPHA/ VDRL, transaminases, creatinine, the KAOP stools, chest X-ray. Praziquantel (40 mg/kg in two spaced taken 15 days) was prescribed. The outcome was favorable with a clear regression of the swelling after a month. Resection of residual lesions was performed by urologists from the hospital. The outcome was favorable with skin scarring of recurrence-free lesions with six months of decline. | ||||||
| ||||||
| ||||||
| ||||||
|
| ||||||
|
Discussion
| ||||||
|
Vulvar localization of S. haematobium is rare. Some case series have described six cases in Burkina [6] and 8 in Mali [4]. In the Malian series, the mean age was 11 years but cases have been reported in adults [9] [10]. The consultation period ranged from 7 to 13 months in the Malian study while it was a year in one of Diallo and colleagues [5] and 3 years in our case, in line with late cutaneous schistosomiasis. The pathophysiologic mechanism is not completely clarified. The symptoms of urinary S. haematobium is related to injuries caused by migration or embolization of eggs and granuloma formation indicating a defensive response of the host [11] [12][13]. The diagnosis of the cutaneous form is provided by the histology of the granuloma, consisting of three concentric areas with the center of ovular debris then a crown of macrophages, eosinophils and giant cells and finally an outer zone fibrosis [11] [12][13]. Urogenital symptoms are usual manifestations of S. haematobium. The digestive signs are characterized by a rectal involvement, often asymptomatic, with granulomas found in the endoscopic examination. Those granulomas are numerous whitish granules on a hyperemic mucosa, there are confluent giving an aspect of pellets or candle stains. Inflammatory adenomatous pseudopolyps, sessile or stalked can sometimes been observed. These polyps can be responsible of occlusive syndrome [14]. Cutaneous schistosomiasis may be associated with obstructive consequences of urogenital apparatus which result in a ureteral hydronephrosis in some cases, hence the importance of abdominal ultrasound. These complications were described by Garba in Niger and N'guessan in Ivory Coast (West Africa) [15] [16]. They found about 329 students, 2.74% of cases of dilatation urinary tract and bladder lesions of 40.43%; among bladder lesions, the wall thickening was noted in 14.89%. Computed tomography (CT) scan without injection is the preferred exam to confirm the calcification of the bladder, ureter and urinary tract [17]. Due to its cost in our context of limited resources, the application is not systematic. In our case, it helped to highlight the digestive and urinary calcifications. S. haematobium is more found in black Africa: Madagascar (west), the Nile Valley (Egypt), Middle East (Saudi Arabia, Yemen). This parasitic disease directly related to agricultural development and increased irrigation (water), raging in homes on an endemic epidemic way [18]. In Senegal (West Africa), due development works in Senegal River by the construction of two dams (Diama Manantali), we are seeing an emergence of waterborne diseases in a Sahelian environment [19] [20]. Chemotherapy with praziquantel prescribed orally at a dose of 40 mg/kg causes a sterilization visceral foci [21] [22]. The treatment of nodular lesions requires a large surgical excision of residual disease [23]. Clinical tests in phase III vaccine against schistosomiasis or Bilhvax® (composed of a glutathione S-transferase 28 000 Daltons) in infected children, vaccine developed by the Pasteur Institute of Lille promoted with the french National Institute of health and medical research (Inserm) would hope in combating this public health disease [24]. | ||||||
|
Conclusion
| ||||||
|
We reported vulvar bilharzia, remarkable for its clinical presentation, concomitant urinary and gastrointestinal involvement and multidisciplinary management. | ||||||
|
References
| ||||||
| ||||||
|
[HTML Abstract]
[PDF Full Text]
|
|
Author Contributions
Pauline Dioussé – Substantial contributions to conception and design, Acquisition of data, Analysis and interpretation of data, Drafting the article, Revising it critically for important intellectual content, Final approval of the version to be published Haby Dione – Substantial contributions to conception and design, Acquisition of data, Analysis and interpretation of data, Drafting the article, Final approval of the version to be published Mariama Bammo – Analysis and interpretation of data, Revising it critically for important intellectual content, Final approval of the version to be published Chérif Dial – Analysis and interpretation of data, Revising it critically for important intellectual content, Final approval of the version to be published Mariétou Thiam – Analysis and interpretation of data, Revising it critically for important intellectual content, Final approval of the version to be published Aissatou Amy Diamé – Analysis and interpretation of data, Revising it critically for important intellectual content, Final approval of the version to be published Bernard Marcel Diop – Analysis and interpretation of data, Revising it critically for important intellectual content, Final approval of the version to be published Mamadou Mourtalla Ka – Analysis and interpretation of data, Revising it critically for important intellectual content, Final approval of the version to be published |
|
Guarantor of submission
The corresponding author is the guarantor of submission. |
|
Source of support
None |
|
Conflict of interest
Authors declare no conflict of interest. |
|
Copyright
© 2016 Pauline Dioussé et al. This article is distributed under the terms of Creative Commons Attribution License which permits unrestricted use, distribution and reproduction in any medium provided the original author(s) and original publisher are properly credited. Please see the copyright policy on the journal website for more information. |
|
|