|

|
 |
|
Letters to the Editor
| ||||||
| A large proximally pedicled random skin transposition flap for reconstruction of a critically compromised lower extremity | ||||||
| Ingo Schmidt | ||||||
|
SRH Poliklinik Gera GmbH, Straße des Friedens 122, 07548 Gera, Germany.
| ||||||
| ||||||
|
[HTML Abstract]
[PDF Full Text]
[Print This Article]
[Similar article in Pumed] [Similar article in Google Scholar] 
|
| How to cite this article |
| Schmidt I. A large proximally pedicled random skin transposition flap for reconstruction of a critically compromised lower extremity. Int J Case Rep Images 2016;7(10):685–686. |
|
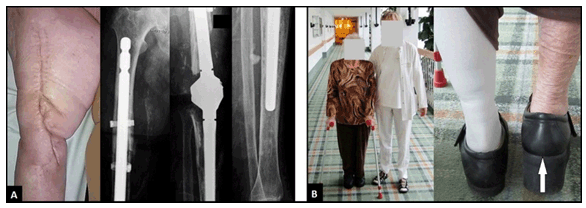
Postoperative soft tissue defect with exposure of relevant structures such as bone with or without hardware and tendon around the knee joint represents a challenging problem. A 77-year-old multimorbid female presented with a nail arthrodesis of the knee joint right that was performed five years ago. The nail and femoral bone were fractured proximally associated with a non-union distally, and additional a chronic fistula due to an infection was seen (Figure 1A). There was a history of three failed total knee arthroplasties (TKA). First, the arthrodesis nail was removed (Figure 1B), and the extremity was stabilized intramedullary with a provisional nail accompanied with incorporation of polymethyl methacrylate (PMMA) beads containing gentamycin (Figure 1C). After consolidation of infection, assessed by culture and histology, a new nail arthrodesis combined with two additional titanium cerclages was performed. A primary wound closure could not be achieved. Due to a considerable atrophy, the medial gastrocnemius muscle could not be used for coverage. For this condition, wound closure was possible using a proximally pedicled random skin transposition flap with a size of 13x6 cm from the medial aspect of knee joint (Figure 1D). The further course was uncomplicated (Figure 2A), and the patient could be mobilized with full weight-bearing on the affected lower extremity using a rise of her shoe rise of eight cm (Figure 2B). The use of local flaps for coverage of soft tissue defects around the knee joint is an option for treatment in patients who are not willing or healthy enough to undergo free microvascular tissue transplantation, and do not require microsurgical expertise. The medial gastrocnemius muscle flap has proven to be a suitable and reliable option for coverage of soft tissue defects after TKA or post-traumatic conditions [1] [2]. However, this was not possible in our case. Skin flaps are indicated when specialized tissue is needed for bulk tissue to fill contour defects. The advantage of skin transposition flap is that additional skin grafting is not almost required, and unlike with muscle flaps, no functional loss occurs. A skin flap consists of skin and subcutaneous tissue that survives on its own blood supply. Skin flaps are classified by the source and pattern of that blood supply, and the most basic of skin flaps are based on the non-specific or "random" blood supply of the subdermal plexus [3]. Random pattern skin transposition flaps can be used in a proximally or distally pedicled manner, the flap must be larger than the defect, and the length: width ratio should be 3:1 [4]. Recently, Haroon-Ur-Rashid et al. [5] published results of 21 patients treated with distally pedicled random skin flaps for coverage of the upper two- thirds of the lower leg, all flaps survived, mean flap length and width were 12 and 5.3 cm, and the maximum size was 15x7 cm. Keywords: Knee joint, Soft tissue defect, Random skin transposition flap |
|
|
|
|
|
|
|
References
|
|
|
[HTML Abstract]
[PDF Full Text]
|
|
Author Contributions:
Ingo Schmidt – Substantial contributions to conception and design, Acquisition of data, Analysis and interpretation of data, Drafting the article, Revising it critically for important intellectual content, Final approval of the version to be published |
|
Guarantor of submission
The corresponding author is the guarantor of submission. |
|
Source of support
None |
|
Conflict of interest
Authors declare no conflict of interest. |
|
Copyright
© 2016 Ingo Schmidt. This article is distributed under the terms of Creative Commons Attribution License which permits unrestricted use, distribution and reproduction in any medium provided the original author(s) and original publisher are properly credited. Please see the copyright policy on the journal website for more information. |
|
|