|

|
 |
|
Clinical Image
| ||||||
| Severe proptosis due to infection | ||||||
| Saifuldeen Al-Qaisi1, Ahmed Abdulameer2 | ||||||
|
1Chief resident and junior faculty member, Internal medicine department, St. Joseph's Hospital and Medical Center, Phoenix, Arizona, USA.
2Research volunteer, Internal medicine department, St. Joseph's Hospital and Medical Center, Phoenix, Arizona, USA. | ||||||
| ||||||
|
[HTML Abstract]
[PDF Full Text]
[Print This Article]
[Similar article in Pumed] [Similar article in Google Scholar] 
|
| How to cite this article |
| Al-Qaisi S, Abdulameer A. Severe proptosis due to infection. Int J Case Rep Images 2016;7(10):671–673. |
|
Case Report
|
|
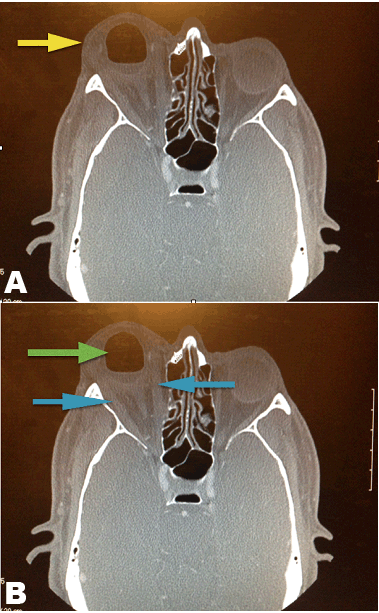
A 48-year-old male with history of type 2 diabetes and intravenous illicit drugs use, presented to the emergency department complaining of severe pain, decreased vision, swelling of the eyelids, and proptosis all in the right eye that has progressed over the previous three days. His symptoms started two days following vitrectomy for tractional retinal detachment and proliferative diabetic retinopathy with intraoperative injection of intravitreal ranibizumab in the same eye. On examination, his visual acuity was 20/30 in left eye and hand motion perception in right eye. His right eye also showed marked proptosis (new onset) with limitation of extraocular movements, lid edema, conjunctival injection and a hazy cornea. Contrast computed tomography (CT) scan of the head showed severe proptosis of right eye ( Figure 1A, yellow arrow) with swelling of extraocular muscles ( Figure 1B, blue arrows), stretching of the optic nerve, and a gas bubble in the right vitreous ( Figure 1B, green arrow) consistent with injection of intraocular gas tamponade during vitrectomy. His findings were consistent with a diagnosis of acute postoperative proptosis, orbital cellulitis, and endophthalmitis. Ophthalmology consult was requested and cultures were sent. Intravenous and intravitreal antibiotic therapy were started and the patient condition significantly improved prior to discharge. |
|
|
|
Discussion
|
|
Orbital cellulitis is an infection involving the contents of the orbit (fat and ocular muscles). It must be distinguished from preseptal cellulitis (sometimes called periorbital cellulitis), which is an infection of the anterior portion of the eyelid. Neither infection involves the globe itself. Although preseptal and orbital cellulitis may be confused with one another because both can cause ocular pain and eyelid swelling and erythema, they have very different clinical implications. Preseptal cellulitis is generally a mild condition that rarely leads to serious complications, whereas orbital cellulitis may cause loss of vision and even loss of life. Orbital cellulitis can usually be distinguished from preseptal cellulitis by its clinical features (ophthalmoplegia, pain with eye movements, and proptosis) and by imaging studies [1]. In cases in which the distinction is not clear, clinicians should treat patients as though they have orbital cellulitis. Both conditions are more common in children than in adults, and preseptal cellulitis is much more common than orbital cellulitis [1]. Proptosis (also called exophthalmos), which is one of the complications that can happen with orbital cellulitis, is the external bulging of the eyeball anteriorly and out of the orbit. It can be unilateral on one side as in this reported case image due to infection, or bilateral due to Graves' disease. It can also happen due to a neoplasm or trauma. Proptosis can be diagnosed clinically and also by imaging like CT scan and magnetic resonance imaging (MRI) scan. Measurement of the degree of exophthalmos is performed using an exophthalmometer. Most sources define exophthalmos/proptosis as a protrusion of the globe greater than 18 mm [2]. The Treatment of proptosis should be targeted mainly towards reversing the primary cause, which may be evident from the clinical presentation or guided by history. |
|
Conclusion
|
|
This is a case of a significant unilateral proptosis that was diagnosed based on the clinical findings and computed tomography scan. It is important to recognize this diagnosis early on as it may be the initial presentation of an underlying orbital infection or neoplasm, for which early management could be vision and life-saving. Keywords: Endophthalmitis, Orbital cellulitis, Proptosis |
|
References
|
|
[HTML Abstract]
[PDF Full Text]
|
|
Author Contributions
Saifuldeen Al-Qaisi – Substantial contributions to conception and design, Acquisition of data, Analysis and interpretation of data, Drafting the article, Revising it critically for important intellectual content, Final approval of the version to be published Ahmed Abdulameer – Analysis and interpretation of data, Revising it critically for important intellectual content, Final approval of the version to be published |
|
Guarantor of submission
The corresponding author is the guarantor of submission. |
|
Source of support
None |
|
Conflict of interest
Authors declare no conflict of interest. |
|
Copyright
© 2016 Saifuldeen Al-Qaisi et al. This article is distributed under the terms of Creative Commons Attribution License which permits unrestricted use, distribution and reproduction in any medium provided the original author(s) and original publisher are properly credited. Please see the copyright policy on the journal website for more information. |
|
|