|

|
 |
|
Case Report
| ||||||
| Port site hydatid cyst in operated case of laparoscopic cystostomy for liver hydatid cyst: A rare complication of laparoscopic hydatid cystostomy | ||||||
| Chirag K. Patel1, Samir M. Shah2, Smit M. Mehta3, Vikram B. Gohil4 | ||||||
|
1Resident doctor, Dept. of General Surgery, Govt. Medical College, Bhavnagar, P.G. Hostel 2, room no 702, Sir T. Hospital campus, Bhavnagar.
2Professor & Head, Department of General Surgery, Govt. Medical College, Bhavnagar. 3Resident doctor, Dept. of General Surgery, Govt. Medical College, Bhavnagar. 4Associate professor, Department of General Surgery, Govt. Medical College, Bhavnagar. | ||||||
| ||||||
|
[HTML Abstract]
[PDF Full Text]
[Print This Article]
[Similar article in Pumed] [Similar article in Google Scholar] 
|
| How to cite this article |
| Patel CK, Shah SM, Mehta SM, Gohil VB. Port site hydatid cyst in operated case of laparoscopic cystostomy for liver hydatid cyst: A rare complication of laparoscopic hydatid cystostomy. Int J Case Rep Images 2016;7(9):603–605. |
|
Abstract
|
|
Introduction:
Hydatid disease in human is mainly caused by infection with the larval stage of the dog tapeworm Echinococcus granulosus. It is an important pathogenic, zoonotic and parasitic infection (acquired from animals) of humans, following ingestion of tapeworm eggs excreted in the feces of infected dogs. Location at unusual sites in the body had a great diagnostic challenge. The modern treatment of hydatid cyst of the liver varies from surgical intervention to percutaneous drainage or medical therapy. Surgery is still the treatment of choice for liver hydatid cyst and operation can be performed by the conventional or laparoscopic approach.
Case Report: We are reporting a case of occurrence of hydatid disease at port sites of abdominal wall in 42-year-old female patient operated previously for laparoscopic live hydatid cystostomy. Conclusion: Occurrence of port site hydatid cyst is rare complication after laparoscopic hydatid cystostomy, but can occur due to lodgment of scolices at port site during laparoscopy. | |
|
Keywords:
Laparoscopic hydatid cystostomy, Liver hydatid cyst, Port site hydatid cyst
| |
|
Introduction
| ||||||
|
Hydatid disease in human is mostly caused by infection with the larval stage of the dog tapeworm Echinococcus granulosus. It is an important pathogenic, zoonotic and parasitic infection of humans, following ingestion of tapeworm eggs excreted in the feces of infected dogs. Cystic hydatid disease usually affects the liver (50–70%) and less frequently the lung, the spleen, the kidney, the bones, and the brain [1]. Treatment of hydatid liver cyst has to be considered in symptomatic cysts and recommended in viable cysts because of the risk of severe complications [1]. The modern treatment of hydatid cyst of the liver varies from surgical intervention to percutaneous drainage. Surgery is still the treatment of choice and can be performed by the conventional or laparoscopic approach. | ||||||
|
Case Report
| ||||||
|
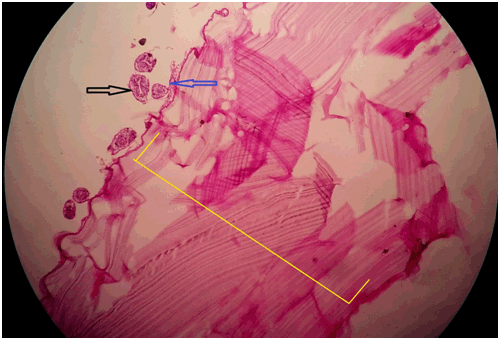
A case of 45-year-old female which was operated for laparoscopic cystostomy for single liver hydatid cyst (6×5 cm in right anterior lobe of liver, diagnosed by CECT abdomen). After four months of laparoscopic cystostomy, she was admitted in our hospital with complain of swelling and pain at the abdomen over previous laparoscopic port site scar. On per abdominal examination, there was a single 5×5 cm sized tender swelling at right hypochondrial port site scar with inflamed and reddish overlying skin. Ultrasonography (USG) scan of abdomen suggestive of 5×4×4 cm sized hypo echoic lesion with internal septation at the anterior abdominal wall at port site with extension to right sub diaphragmatic space with normal liver. Rest of biochemical and hematological investigation were normal. Initially, we suspected an abscess at port site, so we had planned for incision and drainage of material. But during operation, we came to know that the material resemble the endocyst and brood capsule of hydatid cyst. So we had removed all material and site washed with 0.5% cetrimide solution and flower tip malecot catheter inserted under USG guidance into the sub diaphragmatic extension. There was approximately 30 cc output from the malecot catheter for two days, and it was removed on fourth postoperative day. Wound at port site healed secondarily within two weeks. We had sent material for histopathological examination which was reveled hydatid cyst material (Figure 2). | ||||||
| ||||||
| ||||||
|
Discussion
| ||||||
|
Diagnosis of hydatid disease of liver can be made easily but hydatid cyst at unusual sites needs clinical correlation, serological tests, and imaging study (USG, CT scan, and MRI scan) before any intervention is planned. The diagnosis is often difficult when hydatid cyst occurs at unusual locations. As USG provide information that resembles the abscess, we recommend further imaging with MRI scan to delineate the lesion and adequate planning of management. Serologic tests usually allow hydatid cysts to be distinguished from nonparasitic cysts and abscesses [2]. Surgery remains the gold standard treatment for hydatid liver disease and can be performed by the conventional or laparoscopic approach. The aim of surgical intervention is to inactivate the parasite, to evacuate the cyst along with resection of the germinal layer, to prevent peritoneal spillage of scolices and to obliterate the residual cavity. However, surgery may be impractical in patients with multiple cysts localized in several organs and if surgical facilities are inadequate. The introduction of chemotherapy and of the PAIR hydatid cysts of the liver (puncture - aspiration-injection-respiration) offers an alternative treatment, especially in inoperable patients and for cases with a high surgical risk. Cysts with homogeneously calcified cyst walls need, probably, no surgery but only a 'wait and observe' approach. Laparoscopic liver hydatid cystostomy is now considered as minimal invasive surgery without mach complication but following the laparoscopic liver cystostomy recurrence is the major problem [3]. Here we reported a case operated for liver hydatid cyst, which was later on presented as a port site hydatid cyst as clinically (clinical feature) resembling the abscess. There was no study reporting the port site occurrence of hydatid cyst. As we hypothesized, the occurrence of port site hydatid cyst most probably due to contamination of ports with hydatid material and lodgment of scolices at port site during laparoscopy. On reporting this case we also recommend that the wash of port site with scolicidal agent after laparoscopic cystostomy can helpful to prevent port site recurrence, but further research work were needed. | ||||||
|
Conclusion
| ||||||
|
Occurrence of port site hydatid cyst is rare complication after laparoscopic hydatid cystostomy, but can occur due to lodgment of scolices at port site of laparoscopy. | ||||||
|
References
| ||||||
| ||||||
|
[HTML Abstract]
[PDF Full Text]
|
|
Author Contributions
Chirag K. Patel – Substantial contributions to conception and design, Acquisition of data, Analysis and interpretation of data, Drafting the article, Revising it critically for important intellectual content, Final approval of the version to be published Samir M. Shah – Analysis and interpretation of data, Revising it critically for important intellectual content, Final approval of the version to be published Smit M. Mehta – Analysis and interpretation of data, Revising it critically for important intellectual content, Final approval of the version to be published Vikram B. Gohil – Analysis and interpretation of data, Revising it critically for important intellectual content, Final approval of the version to be published |
|
Guarantor of submission
The corresponding author is the guarantor of submission. |
|
Source of support
None |
|
Conflict of interest
Authors declare no conflict of interest. |
|
Copyright
© 2016 Chirag K. Patel et al. This article is distributed under the terms of Creative Commons Attribution License which permits unrestricted use, distribution and reproduction in any medium provided the original author(s) and original publisher are properly credited. Please see the copyright policy on the journal website for more information. |
|
|