|

|
 |
|
Case Report
| ||||||
| Maxillomandibular rehabilitation using digital technology assisted with stereolithographic surgical guide and distraction osteogenesis: A case report | ||||||
| Pradeep Singh1, Deepal Haresh Ajmera2, Tao Wang3, Shui Sheng Xiao4 | ||||||
|
1(M.D.S), Department of Oral and Maxillofacial Surgery, The Affiliated Hospital of Stomatology, Chongqing Medical University, Chongqing Research Center for Oral Diseases and Biomedical Science, Chongqing City, People's Republic of China.
2(M.D.S), Department of Orthodontics and Dentofacial Orthopedics , The Affiliated Hospital of Stomatology, Chongqing Medical University, Chongqing Research Center for Oral Diseases and Biomedical Science, Chongqing City, People's Republic of China. 3(PhD), Department of Oral and Maxillofacial Surgery, The Affiliated Hospital of Stomatology, Chongqing Medical University, Chongqing Research Center for Oral Diseases and Biomedical Science, Chongqing City, People's Republic of China. 4(M.D.S), Department of Oral and Maxillofacial Surgery, The Affiliated Hospital of Stomatology, Chongqing Medical University, Chongqing Research Center for Oral Diseases and Biomedical Science, Chongqing City, People's Republic of China. | ||||||
| ||||||
|
[HTML Abstract]
[PDF Full Text]
[Print This Article]
[Similar article in Pumed] [Similar article in Google Scholar] 
|
| How to cite this article |
| Singh P, Ajmera DH, Wang T, Xiao SS. Maxillomandibular rehabilitation using digital technology assisted with stereolithographic surgical guide and distraction osteogenesis: A case report. Int J Case Rep Images 2016;7(6):402–407. |
|
Abstract
|
|
Introduction:
The aim of this paper is to describe a case of rehabilitation of trauma induced mandibular defect, reconstructed by distraction osteogenesis, and followed by the precise placement of implants aided with digital planning software.
Case Report: In the following case report, a 56-year-old male patient with mandibular segmental defect, was treated with distraction osteogenesis followed by the fabrication of stereolithographic surgical guide using integrated CBCT and SIMPLANT software for the precise placement of implants resulting in restoration of occlusal function. The treatment plan also included W-plasty to excise the facial scar resulting in better esthetics. Comprehensive treatment planning resulted into reconstruction of mandible, and restoration of occlusal function and facial appearance. Conclusion: Surgical planning based on stereolithographic technique is a safe procedure which can contribute in the preoperative treatment planning, assuring the quality and accuracy of surgery. | |
|
Keywords:
Digital technology, Distraction Osteogenesis, Maxillomandibular rehabilitation, Stereolithography
| |
|
Introduction
|
|
The treatment of complex anatomical deformities caused by trauma or congenital defects, have always been a challenging multidisciplinary task for clinicians. Although various treatment modalities have evolved, recent research emphasis is focused on computer-assisted surgical planning and augmentation systems [1]. In this regard, the use of cone beam computed tomography (CBCT) technology combined with 3D planning software by dental health professionals has emerged widely in recent years. The conventional workflow requires a complex logistic chain which is time-consuming and costly [2]. However, stereolithography is a contemporary technology for physical simulation of true maxilla-mandibular anatomic dimensions that uses a laser beam for selective solidification of ultraviolet-sensitive liquid resin. The surgical guides fabricated from these models, enables the placement of implants in vivo at the exact location and direction, as per planned computer simulation [3][4][5][6]. Following this approach implants are placed in the final position avoiding eventual anatomic structures [7]. The aim of this paper is to describe a case of rehabilitation of trauma induced mandibular defect, reconstructed by distraction osteogenesis, and followed by the precise placement of implants aided with digital planning software. |
|
Case Report
|
|
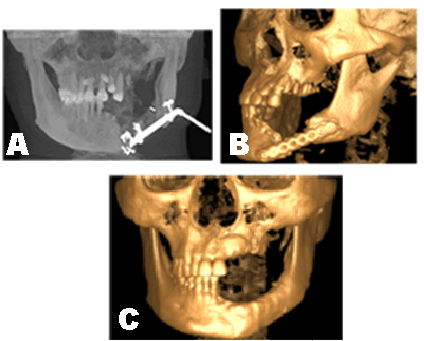
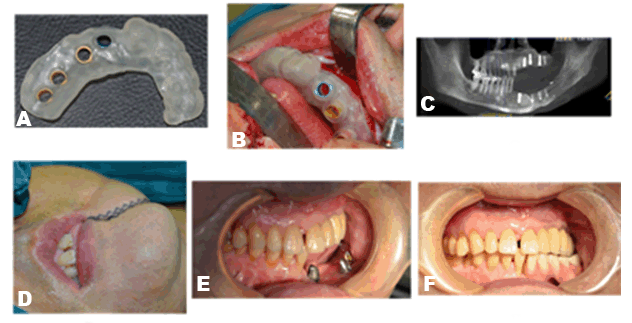
A 56-year-old male patient presented to the department of Oral and Maxillofacial Surgery, with the chief complaint of difficulty in mastication, caused by maxillofacial trauma 4 years back. High impact force in car accident resulted into left mandibular body fracture associated with soft tissue laceration, and right chest injuries. After the emergency treatment, patient was operated for open reduction and internal fixation of the mandibular fracture and right ribs at some other maxilofacial facility. A mandibular titanium reconstruction plate was used for open reduction and internal fixation (ORIF) of the fractured mandible. One year postoperatively patient suffered from facial wound infection and was reoperated for the removal of left mandibular titanium reconstruction plate. Meticulous history and clinical symptoms, were compatible with the diagnosis of Chronic Osteomyelitis. Postoperatively, occlusal derangement and significant dislocation of fracture site was apparent (Figure 1A-B). There was no previous history of any systemic pathology. Past medical, and family history were non-contributory and had no tissue abuse habits. Clinically left-right facial asymmetry was apparent, associated with deviated lower third facial midline, consistent with bilateral temporomandibular joint mobility, and two oblique scar lines at the left angle of mouth, limited mouth opening (about 2.0 cm) and no tenderness preauricularly. Intra-orally, there was obvious occlusal derangement, alveolar bone level on the left side was low, noticeable intraoral scar in left mandibular mucosa and gingiva, tooth number 22 to 27 and 33 to 37 (FDI system followed in the case report) were missing, Grade III mobile root stumps in 31 and 32 tooth region, bilateral submandibular and cervical lymph nodes were nonpalpable. Considering the subjective requirements of the patient and after obtaining full consent a three stage treatment plan was decided. In the first stage of the treatment, open reduction and internal fixation was performed under general anesthesia for old fractures of lower left mandibular region using titanium reconstruction plate in conjunction with left mandibular segmental resection (Figure 1C). Second stage of the treatment (nine months later) involved the removal of lower left mandibular reconstruction plate followed by left mandibular distraction osteogenesis (Figure 2A). A unidirectional distraction device was mounted parallel to the lower border of mandible with single external pin introduced into the distal segment. After a latency period of 6–7 days the distraction was started at the rate of 0.8 mm/day. Following a consolidation period of six months, distraction device was removed. However, the amount of bone regenerated at the distraction gap was not enough, hence a mandibular angle bone graft was harvested from the same side and implanted in the distraction gap. Besides, autogenous calvarial bone graft particles were placed along with mandibular angle graft to increase the amount of bone fill and to supplement and enhance the continuity of mandible. After six months of follow-up bone fill was good enough for further treatment (Figure 2B-C). According to the treatment plan, plastic surgery for the removal of scar and occlusal rehabilitation using implants was scheduled in the final stage of the treatment. Considering the surgical and prosthetic aspects of the treatment a 3D implant plan was designed. Preoperative anatomical information for the bone volume and quality, neighboring teeth, nerve, and sinuses was evaluated using CBCT scan, which revealed, fractured root with respect to 15, 31 and 32 root stumps, impacted teeth in maxillary anterior palatal region, bony defect with respect to 22, marked resorption in the left maxillary posterior region. Digital imaging and communications in medicine (DICOM) file generated through CBCT evaluation was opened with SimPlant (Materialize, Leuven, Belgium) to analyze the data in order to plan the surgery and for the construction of stereolithographic surgical guide. Custom-made bone supported stereolithographic surgical guide was used for the precise transfer of the digital plan to the surgery. After successful anesthesia intubation and following strict surgical protocol, surgery was performed. A full thickness incision of the left side of the lower lip up to the mandibular bone surface was placed with S.S scalpel. A full thickness mucoperiosteal flap was reflected, and root stumps with respect to 31, 32 were extracted. A 5.0 cm length curved incision, distal to 21 along the maxillary alveolar ridge was placed using S.S scalpel and after complete reflection of buccal and palatal soft tissues, bone tissue was exposed followed by the extraction of fractured 15. A direct maxillary sinus lift procedure was performed assisted with the placement of hydroxyapatite crystals (Bio-osteon, Beijing YHJ Science and Trade Co. Ltd, Beijing, China) for the resorbed left maxillary posterior region. After the extraction of compromised teeth, surgical guide was set directly on the residual alveolar bone. The position of the implants was decided according to predesigned stereolithographic surgical guide (Figure 3A-B). A total of eight implants were placed, four in maxilla and mandible each. According to predetermined implant dimensions, three implants of 3.7x12.0 mm (Dentis Co., Ltd., Daegu, South Korea) were placed in maxillary anterior, premolar and molar regions respectively, one implant of 3.5x11.5 mm (OSSTEM Implant Co. Ltd, Seol, Korea) was placed in maxillary molar region. Similarly, four implants of 4.0x10.0 mm (OSSTEM) were placed in mandibular anterior (one), premolar (one), and molar regions (two) (Figure 3C). A 4.0x3.0 cm partial thickness graft was obtained from the palatal mucosa after anesthetizing the area with 1% adrenalin. Palatal soft tissue graft was placed in the left mandibular region covering the implant area. Bony defect in 22 tooth region was curetted and hydroxyapatite crystals (bio-osteon, Beijing YHJ Science and Trade Co. Ltd, Beijing, China) were placed. The area was covered with 1.5x2.0 cm biomembrane (Haiao bio-membrane, Yantai Zhenghai Biotechnology Co. Ltd, Yantai, China)) for successful Guided Bone Regeneration (GBR). Follow-up period was four months. Finally, on the facial skin, incision line was marked with methylene blue along the jagged scar tissue at the left corner of mouth. A 'W Plasty' was performed for the excision of scar tissue (Figure 3D). Small interdigitating triangles were excised on either side of the scar line, resulting in better facial esthetics. Flaps approximated and two layered closure was done. After complete stabilization (after six months of follow up) of implants (Figure 3E) prosthesis was fabricated, thus completing the prosthetic phase of the treatment. Satisfactory occlusion was obtained after placement of the prosthesis (Figure 3F). |
|
|
|
|
|
|
|
Discussion
|
|
Prudent and analytical planning of implant placement not only facilitates minimal invasive treatment and reduced chair time but also enables the clinician to have clear communication with the patient and increases the patient's understanding and acceptance, thereby bringing surgery and restoration to a new level. Contemporary 3D imaging technologies provide clinician with an accurate overview of the availability of bone for the procedures like distraction osteogenesis and implant placement, together with the avoidance of critical anatomical structures. Besides, when CBCT examination is combined with a restorative driven implant plan in SimPlant, a custom-made stereolithographic drill guide can be fabricated accurately [8], the result is a well-planned surgical procedure that reflects the desired functional and esthetic outcome, making the treatment predictable for clinician and patient. Increasingly, studies confirm the high predictability of 3D planning software in regards to their ability to offer absolute precision between what is planned and what is accomplished surgically [7]. The use of computer guides allows implants to be inserted in a far more precise way [7] [8] [9] [10]. Currently, three types of surgical guides are available: tooth supported, bone supported, and mucosa supported. The accuracy of different surgical guides have been analyzed by various authors and all the surgical guides were found to be satisfactorily accurate [11] [12]. A study by Abboud (2012) compared the accuracy of two surgical guide systems, Nobel Guide (Nobel Biocare) and SimPlant (Materialize) for implant placement, and concluded that both types of surgical guide systems were sufficiently accurate [13]. Nokar et al. (2011) in their study compared the accuracy of surgical template based on Computer-Aided Design/Computer-Assisted Manufacture (CAD/CAM), with the conventional surgical template and concluded that accuracy of implant placement was improved using CAD/CAM surgical template [13] [14]. In the illustrated case, mandibular defect caused by segmental resection, affected the oral function and facial esthetics, thus the requirements for accuracy and high surgical quality became more stringent. Accordingly, the treatment plan was decided
The precise planning of osteotomies, bone manipulations, and distraction for such procedures remains a difficult challenge that requires the surgeon to balance the dual goals of functional rehabilitation and aesthetic outcome. Thus, the rationale behind the treatment plan was to relieve pain, mandibular reconstruction, refurbishment of occlusal function and restoration of facial esthetics. Besides, the use of distraction osteogenesis for the reconstruction after segmental resection of the mandible has been well established [15] [16][17]. Therefore, after evaluating the overall situation of the patient distraction osteogenesis was performed. To facilitate the primary stability of the maxillary implants, sinus elevation procedure, and GBR were also performed [18] [19] [20]. Contemporary technologies including, 3D CBCT images combined with Amira software package (Mercury Computer Systems, Berlin, Germany) are being used for visuohaptic simulation that allows the surgeon to rapidly experiment with various bone manipulations and plate/distractor configurations. This system provides the surgeon with a significant advantage in preparing for procedures that are both technically challenging and difficult to plan. Likewise, digital techniques including model reconstruction based on medical images, CAD, and additive manufacturing have been widely used in modern medicine to improve the accuracy and quality of diagnosis and surgery [21]. Moreover, in contemporary dentistry, the use of 3D imaging aided stereolithographic surgical guides has evolved from oral rehabilitation to the construction of definitive nasal prosthesis and handpiece guidance apparatus [22] [23] [24]. Furthermore, Implant installation based on stereolithographic surgical template can be performed using open flap implant surgery or flapless implant placement [25] with good accuracy. In the end, future of this combined technology (CBCT combined with 3D implant planning) will focus on the development of integrated software for distraction osteogenesis and computer assisted implant placement that can allow precise vector determination followed by rehabilitation with implants. |
|
Conclusion
|
|
Surgical planning based on stereolithographic technique is a safe procedure which can contribute in the preoperative treatment planning, assuring the quality and accuracy of surgery. Besides, precision of cone beam computed tomography (CBCT) scan combined with 3D dental implant planning software allows dentists not only to plan for ideal surgical placement but also offers precise translation of the treatment plan to the operating area. |
|
References
|
|
|
[HTML Abstract]
[PDF Full Text]
|
|
Author Contributions
Pradeep Singh – Substantial contributions to conception and design, Acquisition of data, Analysis and interpretation of data, Drafting the article, Revising it critically for important intellectual content, Final approval of the version to be published Deepal Haresh Ajmera – Analysis and interpretation of data, Revising it critically for important intellectual content, Final approval of the version to be published Tao Wang – Analysis and interpretation of data, Revising it critically for important intellectual content, Final approval of the version to be published Shui Sheng Xiao – Analysis and interpretation of data, Revising it critically for important intellectual content, Final approval of the version to be published |
|
Guarantor of submission
The corresponding author is the guarantor of submission. |
|
Source of support
None |
|
Conflict of interest
Authors declare no conflict of interest. |
|
Copyright
© 2016 Pradeep Singh et al. This article is distributed under the terms of Creative Commons Attribution License which permits unrestricted use, distribution and reproduction in any medium provided the original author(s) and original publisher are properly credited. Please see the copyright policy on the journal website for more information. |
|
|