|

|
 |
|
Case Report
| ||||||
| Recurrent osteosarcoma of maxilla presenting as fungating mass: A case report | ||||||
| T. T. Sivakumar1, Pratheep Jeevadhas2, Varun B. Raghavanpillai3, Subramonian Sivaraj2, Anna P. Joseph1, Saira E. Denny4 | ||||||
|
1Professor, Department of Oral Pathology and Microbiology, PMS College of Dental Science and Research, Thiruvananthapuram, Kerala, India.
2Reader, Department of Oral and Maxillofacial Surgery, Rajas Dental College and Hospital, Tamil Nadu, India. 3Reader, Department of Oral Pathology and Microbiology, PMS College of Dental Science and Research, Thiruvananthapuram, Kerala, India. 4Post Graduate, Department of Oral pathology and Microbiology, PMS College of Dental Science and Research, Thiruvananthapuram, Kerala, India. | ||||||
| ||||||
|
[HTML Abstract]
[PDF Full Text]
[Print This Article]
[Similar article in Pumed] [Similar article in Google Scholar] 
|
| How to cite this article |
| Sivakumar TT, Jeevadhas P, Raghavanpillai VB, Sivaraj S, Joseph AP, Denny SE. Recurrent osteosarcoma of maxilla presenting as fungating mass: A case report. Int J Case Rep Images 2016;7(3):149–153. |
|
Abstract
|
|
Introduction:
Osteosarcoma is the most common primary malignant bone tumor excluding hematopoietic neoplasms. It is thought to arise from a primitive mesenchymal bone-forming cell and is characterized by production of osteoid. Despite osteosarcomas of the jaws being less aggressive than those occurring in the long bones, local recurrence after surgical therapy is a major complication.
Case Report: We report a case of recurrent osteosarcoma of maxilla, within three years after surgical resection presenting as a rapidly growing fungating mass in a 24-year-old female. Conclusion: Osteosarcoma affecting the maxilla is a relatively rare condition when compared to the long bones. Early diagnosis and treatment can improve the survival rate. Management of super added fungal infections associated with chemoradiotherapy can prevent further complications and improve the general health of the patient in recurrent lesions. | |
|
Keywords:
Local recurrence, Osteosarcoma of maxilla, Secondary fungal infection
| |
|
Introduction
| ||||||
|
Osteosarcomas of the jaws are uncommon and represent 6–8% of all osteosarcomas [1]. It occurs most often in the third and fourth decades of life, with the mean age being 33 years. As in the long bones a slight male predominance is noted in gnathic osteosarcomas. The maxilla and mandible are involved with about equal frequency. Maxillary lesions are seen commonly involving the inferior portion (alveolar ridge, sinus floor, palate) than the superior aspects (zygoma, orbit) [2]. Although it is generally believed that osteosarcoma of the jaws is less aggressive than those of the long bones, current clinicopathological studies suggest that osteosarcomas of the jaws are aggressive neoplasms. The ability to achieve initial complete removal of the lesion with clear surgical margins of greater than 5 mm is said to demonstrate a better survival, fewer local recurrences, and less metastasis [3]. Osteosarcomas arising from the maxilla are often more difficult to resect completely than mandibular lesions reflecting in a relatively high recurrence rate [4][5]. Here we present a diagnostically challenging case of osteosarcoma with a unique clinical presentation. | ||||||
|
Case Report
| ||||||
|
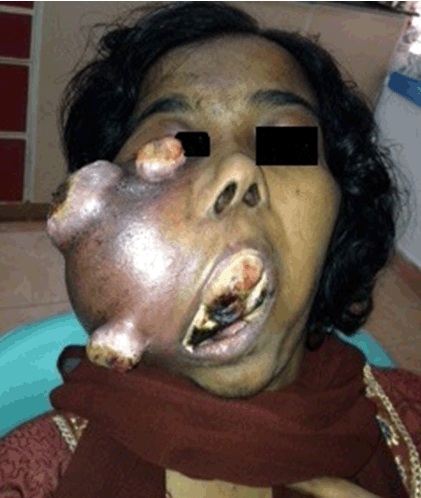
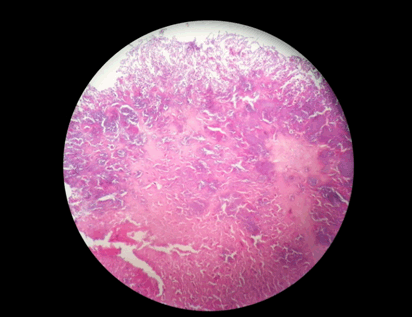
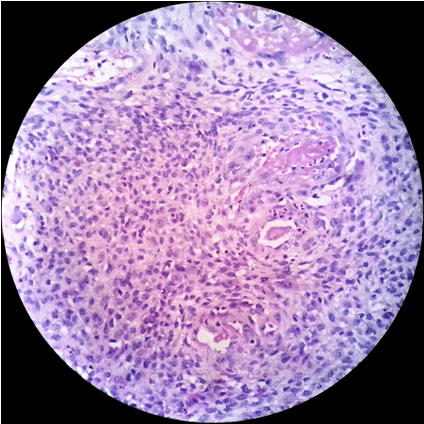
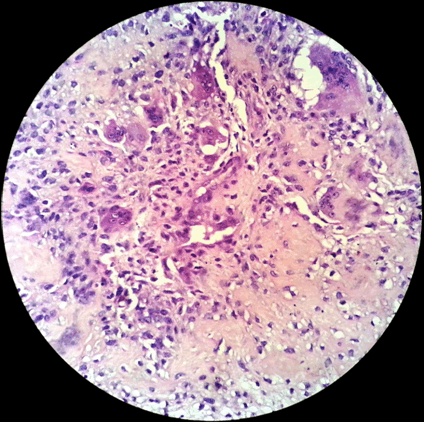
A 24-year-old female reported to the clinic with the chief complaint of a large swelling on the right side of face. She also complained of foul smell, inability to open mouth and multiple ulcers over the swelling. History revealed that the patient developed a right maxillary swelling two years back for which an intra-oral incisional biopsy was performed. The lesion was then given a diagnosis of osteosarcoma. The patient was treated with hemimaxillectomy and chemotherapy with adriamycin 90 mg and ifosfamide 3000 mg, with addition of cisplatin 60 mg to the regimen on the second cycle. She received postoperative adjuvant radiotherapy of 60 Gy/30# by IMRT using 6 MV over a span of one month and nine days. Presently, the patient reported to the clinic with a swelling in the same region which rapidly increased in size. On examination, a large extra oral swelling involving the entire right side of face with multiple superficial polypoid masses was seen. The overlying skin appeared dark and erythematous, with polypoid masses exhibiting superficial ulcerations. Intraoral examination revealed huge mass involving the entire oral cavity with necrotic areas causing dysphonia and dysphagia (Figure 1). Radiographically, anterioposterior view showed right hemimaxillectomy and a mixed radiolucent-radiopaque lesion with ill-defined borders (Figure 2). Computed tomography scan revealed large infiltrating heterogeneous isodense mass with areas of cystic density and hemorrhagic foci. The lesion was causing erosion of the right side of the facial structures involving lateral wall of orbit, zygomatic arch, ethmoid sinus, hard palate. The lesion was extending to the right aspect of nose displacing nasal septum to left and was protruding into oral cavity. Right submental enlarged lymph node of size 1x10.9 cm was observed. Tc99m-MDP bone scan revealed an abnormal increased radiotracer uptake in the right maxillary bone and rest of the skeletal system appeared normal. An incisional biopsy was performed from the intraoral lesion and was sent for histopathological examination. Microscopic examination revealed numerous fungal hyphae and spores along with large areas of necrotic debri (Figure 3). A repeat biopsy after antifungal therapy was performed. The histopathology revealed numerous ovoid to polygonal neoplastic cells showing nuclear pleomorphism with increased mitosis. Osteoid formation (Figure 4) and with associated tumor giant cells were noticed within the stroma and the lesion was diagnosed as high grade recurrent osteosarcoma (Figure 5). The patient was put on chemotherapy with doxyrubicin (60 mg), ifosfamide (3000 mg), methotrexate (12 mg) and cisplatin (60 mg). The patient expired during course of the treatment. | ||||||
| ||||||
| ||||||
| ||||||
| ||||||
| ||||||
|
Discussion
| ||||||
|
Osteosarcomas are malignant connective tissue tumors originating from undifferentiated mesenchymal cells that are able to form bone or osteoid tissue. It can occur in any bone, the most common site being the long bones of the extremities near metaphyseal growth plate. Osteosarcomas of the craniofacial region are relatively rare. Although mandible is reported as the most common site of involvement in the craniofacial region, equal frequencies of maxillary osteosarcomas have also been reported [6]. Mean age of onset of osteosarcomas of craniofacial region is in the third to fourth decade of life. There is usually a predilection for occurrence in males. However, some author report it to be more frequent in females or with an equal gender predilection [6]. Although it is generally believed that osteosarcoma of the jaws is less aggressive than those of the long bones, current clinicopathological studies suggest that osteosarcomas of the jaws are aggressive neoplasms. Our case is an example of such an aggressive neoplasm in the maxilla. The multiple large polypoid masses seen on the surface of the lesion were unique to our case. These superficial masses were due to the secondary infection by opportunistic fungi. The patient's compromised immune status due to the previous chemotherapy and radiotherapy could have contributed to the fungal infection, which in turn can cause serious morbidity and mortality. The radiographic appearance of osteosarcoma is variable ranging from osteolytic to mixed osteolytic-osteoblastic to predominantly osteoblastic lesions [7]. It depends on the amount of tumor bone synthesized by the malignant osteoblasts. Our case showed mixed radiolucent -radiopacity with ill-defined borders. The common histological types of osteosarcomas are chondroblastic, osteoblastic and fibroblastic. The typical histological criteria for the diagnosis of a high grade osteosarcoma include bizarrely arranged tumor cells, immature bone formation (osteoid), atypical fibroblasts and infiltration of adjacent soft tissues. In our case the histopathological examination revealed a high grade osteoblastic type of osteosarcoma. Clear surgical margins play a role in the eradication of the disease and limitation of intramedullary extension. However, due to the complexity of the anatomical location and proximity to vital structures, osteosarcomas arising from the maxilla are often more difficult to resect with a sufficiently safe margin. This is reflected by a relatively high local recurrence rate which is a major complication after surgical therapy, as presented in this case. Study by Delgado et al. suggested that when surgical margins are not free of disease, the use of radiation does not improve the outcome [8]. The recurrence in our case was noted within three years. In the study by Tabone et al., the median interval between the diagnosis of the primary osteosarcoma and the first recurrence was found to be 21 months. They concluded that the most important prognostic indicator at first recurrence seems to be the possible complete resection of disease. Patients not amenable to surgery and patients with a second or a third recurrence have a poor prognosis [9]. If surgical resection is not attempted or cannot be performed, progression of the disease can be fatal [10]. The overall a 5-year survival rate of osteosarcoma patients is found to be 62%. The ability to achieve initial complete removal of the lesion with clear surgical margins of greater than 5 mm is said to demonstrate a better survival, decreased recurrences and less metastasis than those with margins less than 5 mm [3]. | ||||||
|
Conclusion
| ||||||
|
Osteosarcoma affecting the maxilla is relatively rare condition when compared to those in the long bones. Anatomic limitations in the orofacial region cause difficulties in achieving uninvolved margins and for this reason local recurrence of the lesion is high. Superficial fungal infections can cause alterations in both clinical and histopathological presentation. A regular follow-up of the patients after maxillary osteosarcoma resection is advised to rule out further recurrence. | ||||||
|
Acknowledgements
| ||||||
|
We would like to thank Dr. P. S. Thaha, Chairman, PMS College of Dental Science and Research, for providing the facilities and infra-structure; and Dr. Bindu J. Nair, Professor, Department of Oral Pathology and Microbiology, PMS College of Dental Science and Research, for the support and motivation. | ||||||
|
References
| ||||||
| ||||||
|
[HTML Abstract]
[PDF Full Text]
|
|
Author Contributions
T. T. Sivakumar – Substantial contributions to conception and design, Acquisition of data, Analysis and interpretation of data, Drafting the article, Revising it critically for important intellectual content, Final approval of the version to be published Pratheep Jeevadhas – Analysis and interpretation of data, Revising it critically for important intellectual content, Final approval of the version to be published Varun B. Raghavanpillai – Analysis and interpretation of data, Revising it critically for important intellectual content, Final approval of the version to be published Ubramonian Sivaraj – Analysis and interpretation of data, Revising it critically for important intellectual content, Final approval of the version to be published Anna P. Joseph – Analysis and interpretation of data, Revising it critically for important intellectual content, Final approval of the version to be published Saira E. Denny – Analysis and interpretation of data, Revising it critically for important intellectual content, Final approval of the version to be published |
|
Guarantor of submission
The corresponding author is the guarantor of submission. |
|
Source of support
None |
|
Conflict of interest
Authors declare no conflict of interest. |
|
Copyright
© 2016 T. T. Sivakumar et al. This article is distributed under the terms of Creative Commons Attribution License which permits unrestricted use, distribution and reproduction in any medium provided the original author(s) and original publisher are properly credited. Please see the copyright policy on the journal website for more information. |
|
|