|

|
 |
|
Case Series
| ||||||
| Knotty problems: Two cases of challenging JJ stent removal | ||||||
| K. Bonev1, I. Donkov1, A. Simpson1 | ||||||
|
1Department of Urology, Lincoln County Hospital, United Lincolnshire Hospitals NHS Trust, Lincoln, United Kingdom.
| ||||||
| ||||||
|
[HTML Abstract]
[PDF Full Text]
[Print This Article]
[Similar article in Pumed] [Similar article in Google Scholar] 
|
| How to cite this article |
| Bonev K, Donkov I, Simpson A. Knotty problems: Two cases of challenging JJ stent removal. Int J Case Rep Images 2015;6(8):462–464. |
|
Abstract
|
|
Introduction:
The JJ stent insertion and removal is quite common urological procedure, which could be challenging sometimes as per knot formed on proximal stent end. By using rigid 8cH ureteroscope the authors provide recommendations for difficult stent removal.
Case Series: Two cases of difficult JJ stent removal on two patients who had previously renal colic. The stents were 6cH/26cm; most common used ones. JJ stents looked unremarkably on the fluoroscopy before their retrieval. On the extraction their proximal ends formed knots, which were bigger than the diameter of the ureter. By use of short 8cH rigid ureteroscope positioned distally adjacent to the stent, sufficient dilatation of the ureter was gained. Conclusion: The JJ stent removal is a delicate procedure, which nevertheless its technical simplicity could bring up unexpected complication to raise urologist's awareness. | |
|
Keywords:
Complication, Fluoroscopy, JJ stent, Knotty problems, Ureteroscopy
| |
|
Introduction
| ||||||
|
Renal colic presents one the most common urological emergencies. Decompression of an acute renal obstruction due to a ureteric calculus can be achieved by insertion of a JJ stent. Usually, the procedure of JJ stent insertion is safe and routine, but sometimes the procedure of removal of the same JJ stent could be challenging. | ||||||
|
Case Series
| ||||||
|
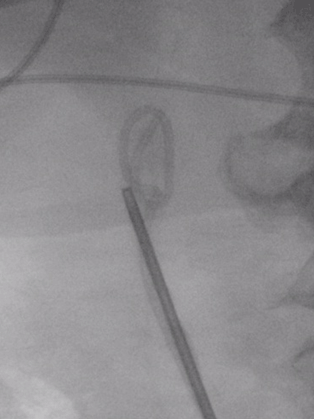
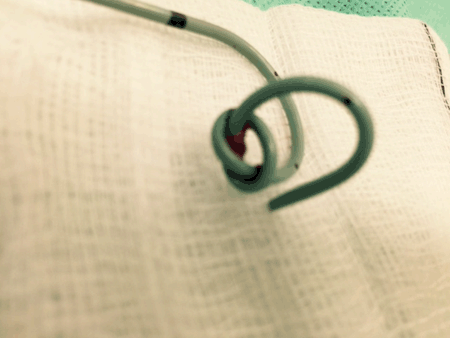
Case 1: A 44-year-old male was presented with two days history of sudden onset of right loin to groin pain, colicky in nature, nausea, vomiting, temperature 36.8°C, blood pressure 120/75 mmHg, urine dipstick: 4(+)Blood, Leu1(+). Diagnosis: Right renal colic with 6.5 mm calculus in the proximal ureter confirmed by computed tomography scan. Case 2 : A 53-year-old male was presented with 12 h history of sudden onset of right loin pain, colicky in nature, irradiating to the right inguinal area, nausea, temperature 37°C, blood pressure 118/82 mmHg, Urine dipstick:3(+)Blood. Diagnosis: Right renal colic with 7 mm calculus in the middle ureter confirmed by computed tomography scan. In these two cases, male patients of 44 and 53 years presented with renal colic. A 6Ch/26 cm JJ stent [1] was inserted cystoscopically under general anesthesia to relieve obstruction due to ureteric stones measuring 6–7 mm in diameter located respectively in middle and the distal ureteric segments. The procedures were performed using 22Ch cystoscope and standard PTFE (polytetrafluoroethylene) guide wire under fluoroscopic control. JJ stents looked unremarkably on the fluoroscopy following their insertion. After 2–3 weeks JJ stent removal and stone retrieval were attempted in each case. Moderate traction on the distal end of JJ stent positioned in the bladder was performed under direct vision. After resistance was felt, a fluoroscopy was performed. Knot-like formation greater that the PUJ (pelvi-ureteric junction) diameter was seen on the proximal end of the JJ stent. Insertion of the flexible guide wire through the JJ stent was attempted in an attempt to straighten the stent was unsuccessful. Rigid ureteroscopy using 6–7.5 Ch ureteroscope confirmed (Figure 1) the knot formed on the part of the JJ stent, located in the renal pelvis. Gentle traction was performed under endoscopic control, but this was also unsuccessful. Ultimately, rigid ureteroscopy with a 8Ch ureteroscope, positioned adjacent to the knot on JJ stent under direct vision allowed sufficient dilation of the ureter to enable successful removal of the complicated stent, with knot still in place, in each case (Figure 2) and (Figure 3). Following second ureteroscopy were found fragmented stone fragments which were successfully retrieved using a Zero Tip 1, 9" stone basket. | ||||||
| ||||||
| ||||||
|
| ||||||
| ||||||
|
Discussion
| ||||||
|
Knotting of proximal end of the JJ stent and its removal is a rare complication with less than 20 cases reported in literature [2] [3]. Failure to recognise a knotted stent can have serious consequences, including ureteric injury, stent fracture and stent retention. Various techniques have been described to achieve stent removal, including simple traction [2], ureteroscopy, ureterotomy, percutaneous removal and Holmium laser incision of the knot [3]. We have shown in two cases that ureteroscopic dilation followed by gentle traction under direct vision with the 8Ch ureteroscope provides a safe and effective technique for dealing with this complication. | ||||||
|
Conclusion
| ||||||
|
Removing JJ stent in ambulatory setting is a common procedure. In most cases this is undertaken without easy access to fluoroscopy or ureteroscopy. Complications such as stent knotting can occur even after a short dwell time operators should be aware of this possibility if resistance is felt. Appropriate management with a combination of fluoroscopy and direct vision ureteroscopy is described. | ||||||
|
References
| ||||||
| ||||||
|
[HTML Abstract]
[PDF Full Text]
|
|
Author Contributions:
K. Bonev – Substantial contributions to conception and design, Acquisition of data, Analysis and interpretation of data, Drafting the article, Revising it critically for important intellectual content, Final approval of the version to be published I. Donkov – Analysis and interpretation of data, Revising it critically for important intellectual content, Final approval of the version to be published A. Simpson – Analysis and interpretation of data, Revising it critically for important intellectual content, Final approval of the version to be published |
|
Guarantor of submission
The corresponding author is the guarantor of submission. |
|
Source of support
None |
|
Conflict of interest
Authors declare no conflict of interest. |
|
Copyright
© 2015 K. Bonev et al. This article is distributed under the terms of Creative Commons Attribution License which permits unrestricted use, distribution and reproduction in any medium provided the original author(s) and original publisher are properly credited. Please see the copyright policy on the journal website for more information. |
|
|