|

|
 |
|
Case Report
| ||||||
| Chlamydophila psittaci infection complicated by emboli in a healthy patient | ||||||
| S. S. Guillen1, J. H. Elderman1, A. M. E. van Well2, M. van Rijn3, A. Dees4 | ||||||
|
1Resident, Department of Internal Medicine, Ikazia Hospital, Rotterdam, The Netherlands.
2Vascular Surgeon, Department of Surgery, Ikazia Hospital, Rotterdam, The Netherlands. 3Microbiologist, Department of Microbiology, Ikazia Hospital, Rotterdam, The Netherlands. 4Internist, Department of Internal Medicine, Ikazia Hospital, Rotterdam, The Netherlands. | ||||||
| ||||||
|
[HTML Abstract]
[PDF Full Text]
[Print This Article]
[Similar article in Pumed] [Similar article in Google Scholar] 
|
| How to cite this article |
| Guillen SS, Flderman JH, van Well AME, van Rijn M, Dees A. Chlamydophila psittaci infection complicated by emboli in a healthy patient. Int J Case Rep Images 2015;6(8):507–510. |
|
Abstract
|
|
Introduction:
Chlamydophilae are obligate intracellular bacteria which cause a wide variety of infectious diseases in humans and animals. The species of Chlamydophila psittaci is associated with severe complications.
Case Report: A 51-year-old healthy female presented with a lobar pneumonia due to Chlamydophila psittaci infection. The clinical course was complicated by peripheral arterial emboli, necessitating partial amputation of the right foot. Conclusion: In patients with Chlamydophila psittaci pneumonia severe complications may develop which require multidisciplinary treatment. | |
|
Keywords:
Arterial emboli, Complications, Chlamydophila psittaci, Pneumonia
| |
|
Introduction
| ||||||
|
Psittacosis is a rare 'atypical pneumonia' that is caused by Chlamydophila psittaci; an intracellular gram-negative bacteria. Birds and other avian species are the natural reservoirs. They are frequently involved in the transmission of Chlamydophila psittaci to humans. The illness is a multisystem disease that can either go unnoticed or may vary from mild to severe pneumonia [1]. A known complication of the illness is cardiovascular involvement, and few cases of peripheral arterial emboli have been reported [2]. In this report, we describe a case of psittacosis in an otherwise healthy patient that led to severe arterial emboli and partial amputation of her foot. | ||||||
|
Case Report
| ||||||
|
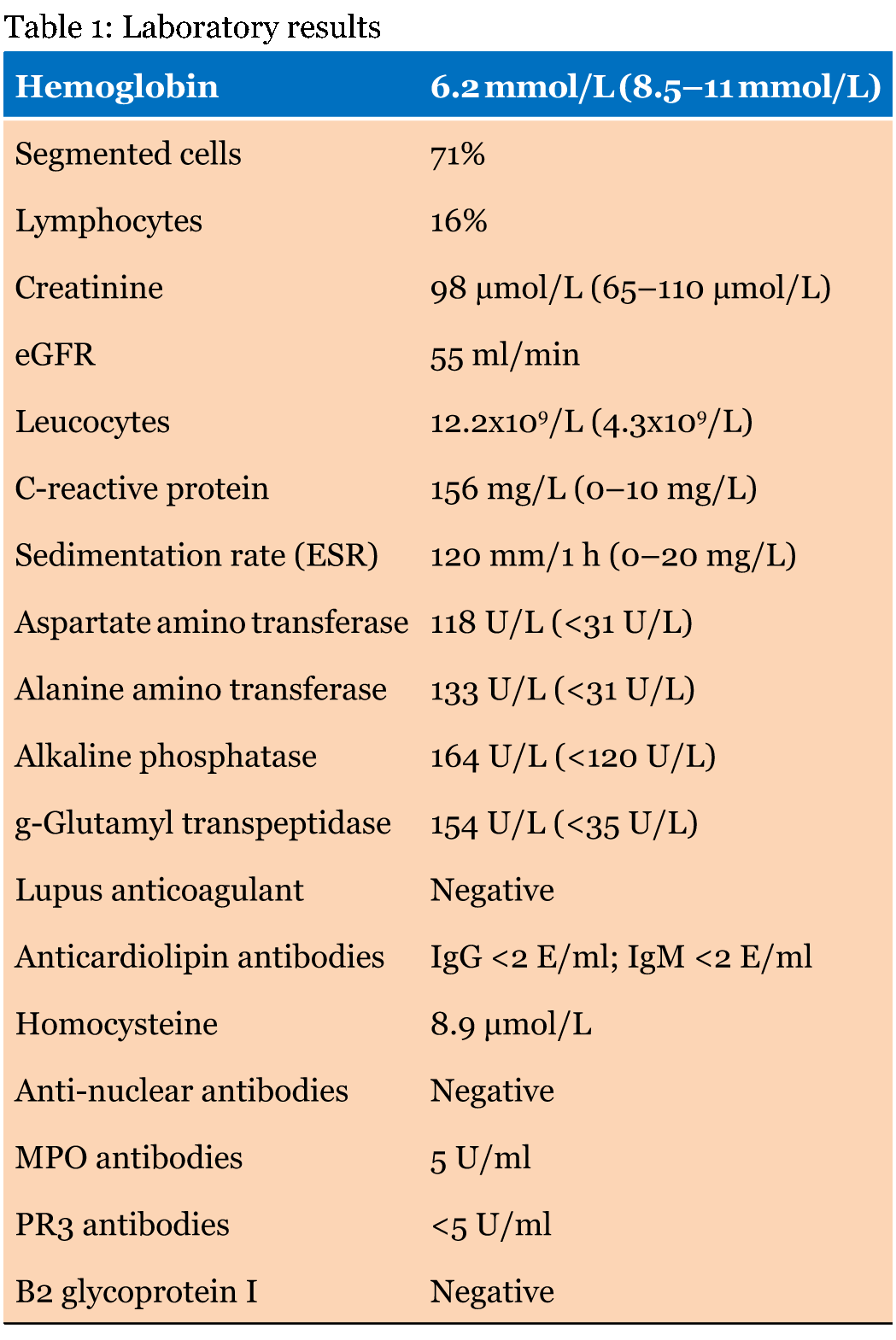
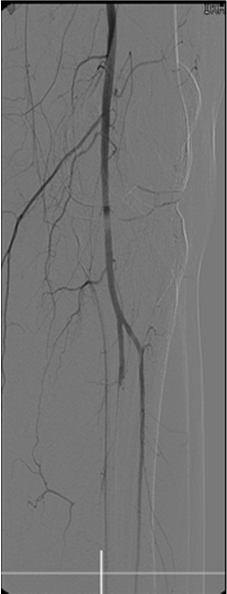
A 51-year-old Caucasian female was admitted to the hospital with complaints of fever, headache and confusion. She had no complaints during the five days prior to admission. Her medical history included knee surgery and hyper menorrhea. Her family history included a brother who experienced sudden cardiac death. She did not use any medication and was a heavy smoker. In her free time, she worked in a centre for diseased, wild, non-domestic birds. Her physical examination revealed a blood pressure of 150/80 mmHg, a regular pulse rate of 110 per minute, a body temperature of 39.6°C, and normal heart sounds. Crackles and amphoric breathing were heard over her right lung. However, a further physical examination showed no abnormalities. Laboratory examination of the patient showed signs of infection as well as elevated liver enzymes (Table 1). A chest X-ray revealed lower right lobe pneumonia (Figure 1). Tetracycline treatment was started (doxycycline); ELISA serology testing indicated positive IgG antibody titres for Chlamydophila psittaci that became significantly elevated after several weeks (Table 2). The patient recovered quickly and was discharged five days after the admission. Unfortunately, one day after her discharge, the patient was admitted to the emergency department with progressive pain in both of her feet and the loss of color and sensation in her toes. A physical examination revealed that her feet were cyanotic, and no arterial pulsations were found over the posterior tibial and dorsalis pedis arteries on either side. The clinical presentation suggested acute arterial obstruction. In the differential diagnosis we considered advanced atherosclerotic disease, atrial fibrillation, endocarditis with cardiac emboli, and complicated autoimmune disease, such as giant cell-arteritis. An immediate angiography showed bilateral occlusions of the peroneal artery and the distal posterior tibial artery (Figure 2). Additionally, a thrombus was observed in the right side of the anterior tibial artery. Local treatment with urokinases and systemic treatment with heparin were started. The latter treatment had to be withdrawn because of thrombocytopenia: the patient had a count of 62x109/L (274x109/L before treatment). Following the withdrawal of the urokinase and heparin treatments, the thrombocyte count eventually rose to 268x109/L (the HIT-test that was performed later was negative). After the urokinase treatment, the patient's circulation completely recovered on the left side. To enable recovery on the right side of the arcade, the patient underwent surgical embolectomy, which initially restored the circulation. Unfortunately, on the following day, the arterial arcade was again occluded and necessitated a partial amputation of the right foot. Further investigations, such as extensive clotting tests, an autoimmune blood panel (Table 1), repeated transthoracic echocardiography, a transesophageal echocardiography, and angiographic visualization of the abdominal arteries did not reveal any cardiovascular abnormalities. Her recovery was successful following the amputation, and she was started on oral anticoagulants. During a follow-up period of three years, the patient had no further complaints. | ||||||
| ||||||
| ||||||
| ||||||
| ||||||
|
Discussion
| ||||||
|
In this report, we described a patient diagnosed with psittacosis who was treated with the correct antibiotics and experienced good clinical recovery. Unfortunately, shortly thereafter she was re-admitted with arterial emboli in both legs, with no evidence of cardiac involvement. Psittacosis is a rare infection caused by the gram-negative Chlamydophila psittaci bacterium. The primary reservoirs of Chlamydophila psittaci are exotic and domestic birds; however, transmission from other animals has also been reported. Most patients with psittacosis have a history of close contact with birds, as was the case here. Our patient spent much of her free time as a volunteer in a centre for diseased non-domestic birds, Infection occurs following inhalation of the bacteria, which is spread through the excreta and dust from the feathers of affected, typically parrot-like birds. The clinical course varies from an asymptomatic or light flu-like illness to severe illness. There have been rare reports of complications such as myocarditis, endocarditis, encephalitis, jaundice and multi-organ disease [1] [3]. Previous reports in the literature have also indicated that Chlamydophila psittaci is pathogenic to the vascular system and may cause vascular obstruction [2]. The association between psittacosis and peripheral arterial obstructive disease (PAOD) has been described in a number of cases [4]. Chlamydophila pneumoniae, a closely related species, is one of the most actively studied organisms in this field. In a meta-analysis by Gutierrez, it was stated that immunohistochemical and polymerase chain reactions (PCR) studies of arterial biopsies have become the techniques of choice to demonstrate bacterial involvement [5]. The billion dollar question here remains whether Chlamydophila psittaci infection in our patient did provoke the severe complications. Since repeated echocardiographic investigations did not reveal a cardiac emboli origin and clotting tests were normal, along with the serological results, we assumed so in this particular case. Although the precise molecular mechanisms are not completely understood, recent research has shed some light on the pathophysiology. There is evidence that C. pneumonia infection stimulates growth of vascular cells and plays a role in the pathogenesis of atherothrombosis. Previous studies have also provided evidence that C. pneumoniae infection can induce the expression of procoagulant proteins and proinflammatory cytokines in human atherosclerotic lesions [6]. Dechend et al. found that C. pneumoniae infection of human endothelial cells (ECs) and vascular smooth muscle cells (VSMCs) resulted in the overexpression of tissue factor (TF), plasminogen activator inhibitor (PAI-I), and interleukin-6 (IL-6), as well as NF-kB activation. These mechanisms might explain how a stable plaque is transformed into an unstable one, thereby increasing the thrombogenicity of infected plaques [7]. | ||||||
|
Conclusion
| ||||||
|
In the patient presented here, we suggest that psittacosis has been involved in the development of severe arterial emboli. Clinicians should be aware of the potential dangers associated with C. psittaci infections. | ||||||
|
References
| ||||||
| ||||||
|
[HTML Abstract]
[PDF Full Text]
|
|
Author Contributions
S.S. Guillen – Substantial contributions to conception and design, Acquisition of data, Analysis and interpretation of data, Drafting the article, Critical revision of the article, Final approval of the version to be published J.H. Elderman – Substantial contributions to conception and design, Acquisition of data, Analysis and interpretation of data, Drafting the article, Critical revision of the article, Final approval of the version to be published A.M.E. van Well – Substantial contributions to conception and design, Acquisition of data, Analysis and interpretation of data, Drafting the article, Critical revision of the article, Final approval of the version to be published M. van Rijn – Substantial contributions to conception and design, Acquisition of data, Analysis and interpretation of data, Drafting the article, Critical revision of the article, Final approval of the version to be published A. Dees – Substantial contributions to conception and design, Acquisition of data, Analysis and interpretation of data, Drafting the article, Critical revision of the article, Final approval of the version to be published |
|
Guarantor of submission
The corresponding author is the guarantor of submission. |
|
Source of support
None |
|
Conflict of interest
Authors declare no conflict of interest. |
|
Copyright
© 2015 S.S. Guillen et al. This article is distributed under the terms of Creative Commons Attribution License which permits unrestricted use, distribution and reproduction in any medium provided the original author(s) and original publisher are properly credited. Please see the copyright policy on the journal website for more information. |
|
|