|

|
 |
|
Case Report
| ||||||
| Cardiac rehabilitation for cardiac syndrome X and microvascular angina: A case report | ||||||
| Wipawee Laksanakorn1, Tanaporn Laprattanagul1, Janet Wei2, Chrisandra Shufelt3, Margo Minissian4, Puja K Mehta5, C. Noel Bairey Merz6 | ||||||
|
1MD, Rehabilitation Department, Golden Jubilee Medical Center, NakhonPathom, Thailand.
2MD, FACC, Barbra Streisand Women's Heart Center, Cedars-Sinai Heart Institute, Cedars-Sinai Medical Center, Los Angeles, CA, United States. 3MD, MS, FACP, Associate Director, Barbra Streisand Women's Heart Center, Cedars-Sinai Heart Institute, Cedars-Sinai Medical Center, Los Angeles, CA, United States. 4Ph.Dc, ACNP, FACC, Cardiology Nurse Practitioner, Barbra Streisand Women's Heart Center, Cedars-Sinai Heart Institute, Cedars-Sinai Medical Center, Los Angeles, CA, United States. 5MD, FACC, Director, Non-Invasive Vascular Function Research Lab, Barbra Streisand Women's Heart Center, Cedars-Sinai Heart Institute, Cedars-Sinai Medical Center, Los Angeles, CA, United States. 6MD, FACC, FAHA, Director, Barbra Streisand Women's Heart Center, Cedars-Sinai Heart Institute, Cedars-Sinai Medical Center, Los Angeles, CA, United States. | ||||||
| ||||||
|
[HTML Abstract]
[PDF Full Text]
[Print This Article]
[Similar article in Pumed] [Similar article in Google Scholar] 
|
| How to cite this article |
| Laksanakorn W, Laprattanagul T, Wei J, Shufelt C, Minissian M, Mehta PK, Merz CNB. Cardiac rehabilitation for cardiac syndrome X and microvascular angina: A case report. Int J Case Rep Images 2015;6(4):239–244. |
|
Abstract
|
|
Introduction:
Therapeutic strategies for cardiac syndrome X, characterized by the three features of angina, evidence of myocardial ischemia and no obstructive coronary artery disease, are not well known. Recent data indicate that angina secondary to microvascular coronary dysfunction is a common pathogenesis of cardiac syndrome X. While cardiac rehabilitation is well-known to be effective for angina due to obstructive coronary artery disease, less is known in cardiac syndrome X and microvascular angina patients.
Case Report: A 34-year-old female with history of pre-eclampsia during three pregnancies, recurrent non-ST-segment-elevation myocardial infarctions, no obstructive coronary artery disease, microvascular coronary dysfunction documented by coronary reactivity testing, ischemic cardiomyopathy, overweight, factor V Leiden mutation, and persistent microvascular angina was referred to cardiac rehabilitation five weeks after a non-ST-segment-elevation myocardial infarction. The patient was taking a beta blocker, ACE, statin and low dose aspirin. She underwent four sessions of supervised cardiac rehabilitation program which progressed to a duration of 45 minutes at a level of 3.3 metabolic equivalents of aerobic exercise. A normal cardiovascular response without arrhythmias was observed. A home program was suggested with moderate intensity of aerobic exercise, 30–45 minutes per day, most days of the week. She experienced decreased angina, improved quality of life and increased functional capacity at the fourth-year of follow-up. Conclusion: Cardiac rehabilitation was beneficial in the patient angina due to microvascular coronary dysfunction. Increased exercise intensity and duration, increased functional capacity, decreased anginal symptoms and improved quality of life were found. | |
|
Keywords:
Cardiac rehabilitation, Cardiac syndrome X, Exercise training, Microvascular angina, Microvascular coronary dysfunction
| |
|
Introduction
| ||||||
|
Therapeutic strategies for cardiac syndrome X (CSX), characterized by three features, including angina, evidence of myocardial ischemia on stress testing, and no obstructive coronary artery disease (CAD) are not well known. Data from the National Heart, Lung and Blood Institute-sponsored Women's Ischemia Syndrome Evaluation (NHLBI-WISE) study demonstrates that microvascular coronary dysfunction (MCD) is present in approximately half of women with CSX [1]. In addition, prognosis for patients with CSX may not be as benign as previously thought especially in patients with evidence of microvascular coronary dysfunction. The NHLBI-WISE study demonstrated a five-year cardiovascular event rate of 16% for women with non-obstructive CAD and 7.9% for women with normal coronary arteries, compared to 2.4% for asymptomatic women with no history of heart disease [2]. Nevertheless the contributing pathogenesis of angina in CSX remains controversial. Possible mechanisms for the angina have been reported, including myocardial ischemia due to microvascular and endothelial coronary dysfunction, and abnormal cardiac pain perception [3]. While there is wide acceptance of the benefits of cardiac rehabilitation (CR) for patients with obstructive CAD [4], CR is underutilized with the approximate mean referral rate of 34%. Among CAD patients eligible for CR, participation rates for women are lower than men in most studies [5] . Furthermore, there are few studies evaluating impact of CR on CSX patients and microvascular angina patients. In this report, the case of woman with microvascular angina is examined to highlight the potential benefit of CR in this group of patients. | ||||||
|
Case Report
| ||||||
|
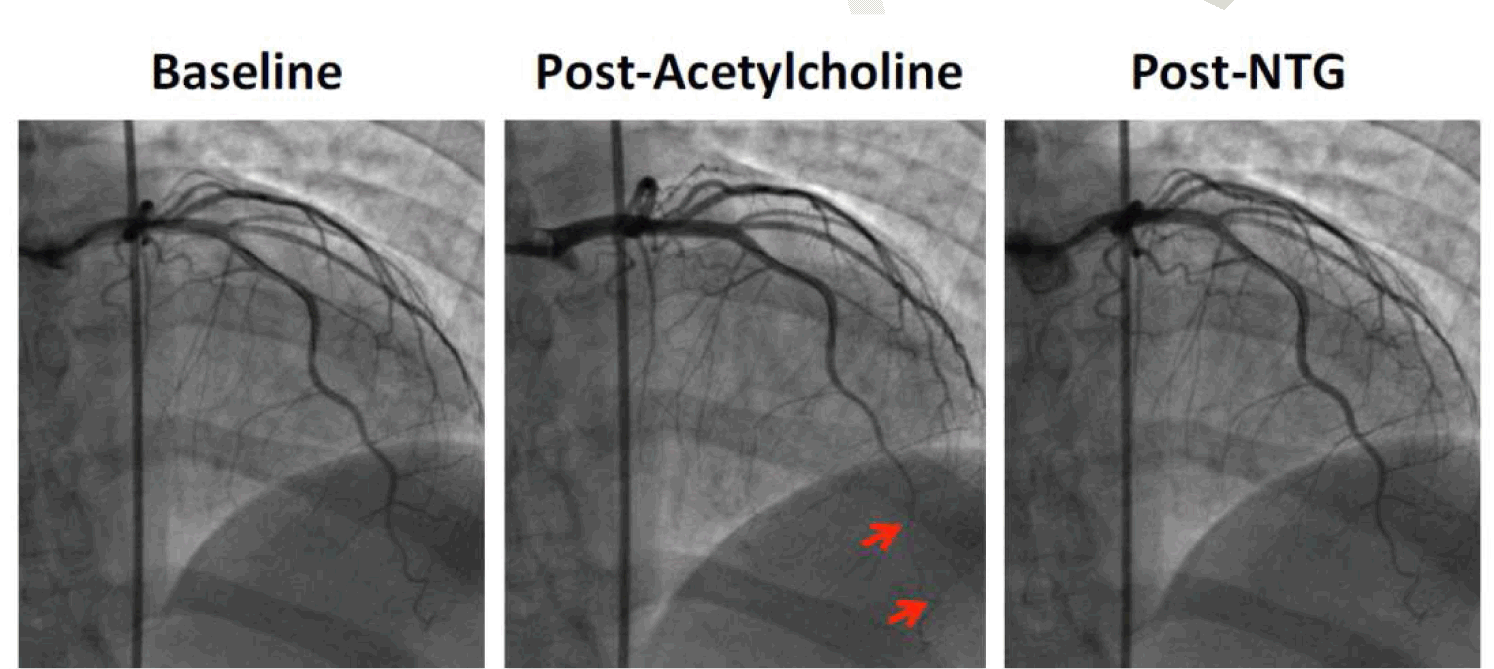
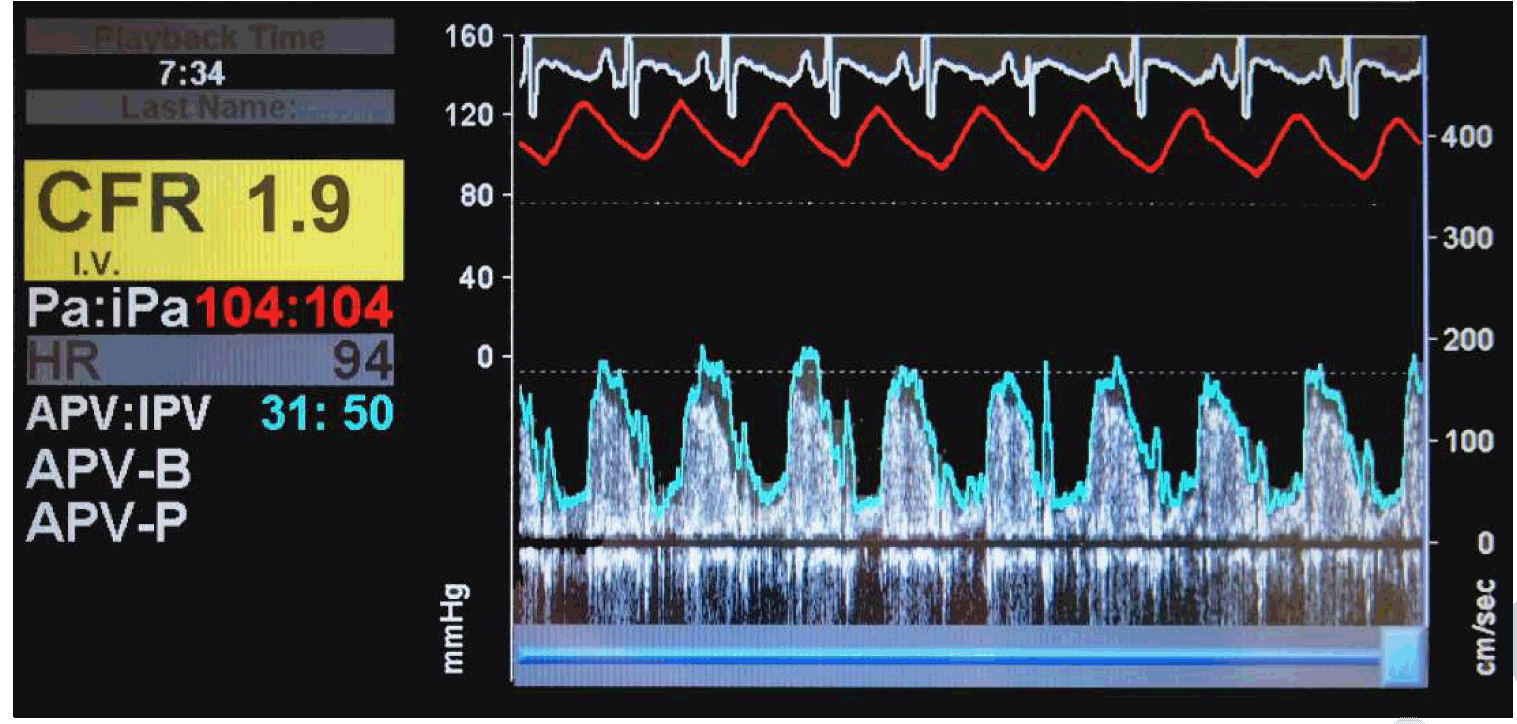
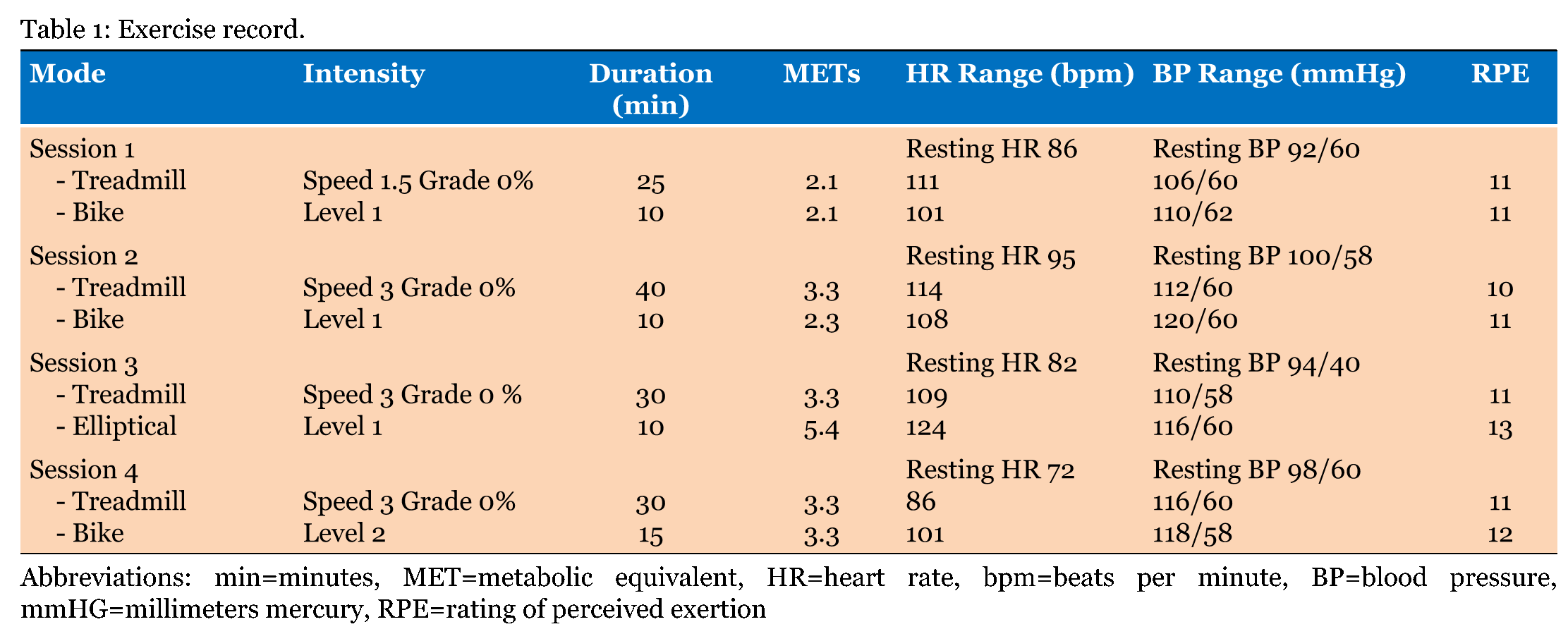
A 34-year-old female was referred to cardiac rehabilitation five weeks after a non-ST-segment-elevation myocardial infarction (NSTEMI) in 2008. She had a prior history of pre-eclampsia with three pregnancies and was heterozygous for factor V Leiden mutation. She had a history of NSTEMI with no obstructive CAD in 2005 and had persistent exertional and non-exertional episodes of angina. She had multiple emergency department visits for angina. She was diagnosed with MCD by invasive coronary reactivity testing using intra-coronary adenosine and acetylcholine [6] in 2007. MCD was diagnosed by invasive coronary reactivity testing as previously published (Figure 1) [6]. She had normal coronary arteriography without luminal irregularity and left ventricular end-diastolic filling pressure was elevated at 17 mmHg. Coronary flow reserve (CFR) in response to adenosine (Figure 2) was abnormal at 1.9 (normal >2.5), coronary blood flow response to acetylcholine was mildly abnormal at 48% increase (normal is =50% increase), coronary artery diameter dilation response to acetylcholine was markedly abnormal at 22% constriction (normal is dilation >0%), and nitroglycerin response was normal at 46% dilation (normal >20%) as depicted in Figure 1 and Figure 2. Resting echocardiogram in 2005 demonstrated a left ventricular ejection fraction (LVEF) of 55% with basal to mid-septal hypokinesis. From 2005–2010, she had a total of 11 NSTEMI admissions with elevated cardiac troponin I ranging between 0.1 ng/ml in 2008 and 33 ng/ml in 2009. Resting echocardiogram in 2007 demonstrated basal to mid-inferior wall akinesis with hypokinesis of inferolateral wall and interventricular septum with an LVEF of 35–45%. Myocardial biopsy revealed focal fibrosis without vasculitis or inflammation. During the NSTEMI admission prior to CR referral, she had substernal and left sided chest pain which woke her up from sleep. Normal sinus rhythm with inferolateral T wave inversions was shown on ECG, accompanied by an elevated troponin I to 1.72 ng/ml. A diagnosis of ischemic cardiomyopathy and microvascular angina secondary to coronary microvascular dysfunction was made. At the time of cardiac rehabilitation referral in 2008, cardiovascular risk factor profile revealed a body mass index of 26.3 (overweight), no diabetes, no dyslipidemia, no history of smoking and no family history of premature CAD. She experienced fatigue during ordinary daily activity and shortness of breath during moderate to strenuous physical activity. She did not exercise regularly and had exertional and stress-related angina. No symptoms and signs of heart failure were found. Previously, she was a school teacher and practiced figure skating a few times per week. She was unemployed at the time of CR referral. A Duke Activity Status Index (DASI) questionnaire score was 15.2 corresponding to 4.3 metabolic equivalents (METs) [7]. A general quality of life (QOL) rating was 3 in answer to the question "Overall, how would the patient rate her QOL?" The possible responses fall along an interval scale from 0 (worst) to 10 (best). During CR, the patient initially had resting blood pressure (BP) of 92/60 mmHg and heart rate (HR) of 86 beats per minute (bpm). Her physical examination was unremarkable. Her CR plan included reconditioning exercises three times a week for 12 weeks, including aerobic and strengthening exercises, as well as nutritional counseling and stress management. She exercised to 2.1 METs for 35 minutes using treadmill and stationary cycling in the first session. Peak HR rose to 111 bpm, BP was 110/62 mmHg and the rating of perceived exertion (RPE) was 11. No arrhythmia on ECG telemetry was noted and no abnormal symptoms were reported. Due to conflicts with childcare, she only attended four CR sessions (Table 1). She increased her exercise tolerance to 45 minutes of treadmill and cycling with the intensity of 3.3 METs. A home CR program with moderate intensity of aerobic exercise such as brisk walk, 30–45 minutes per day for most days of the week was advised because she could not return to a supervised program. The patient was treated medically with aspirin, dabigatran, metoprolol, ramipril, atorvastatin, nitroglycerin transdermal patch and acetaminophen-codeine as needed for pain. In 2012, she underwent implantable cardioverter-defibrillator placement due to a declined LVEF to 30%. Subsequently, her symptoms were improved, and she continued walking exercise at home. At four-year follow-up, she reported decreased anginal symptoms, improved overall health status, improved functional capacity demonstrated by a DASI questionnaire score of 26.95 (7.7 METs) and a general QOL rating of 5/10. | ||||||
|
| ||||||
|
| ||||||
| ||||||
|
Discussion
| ||||||
|
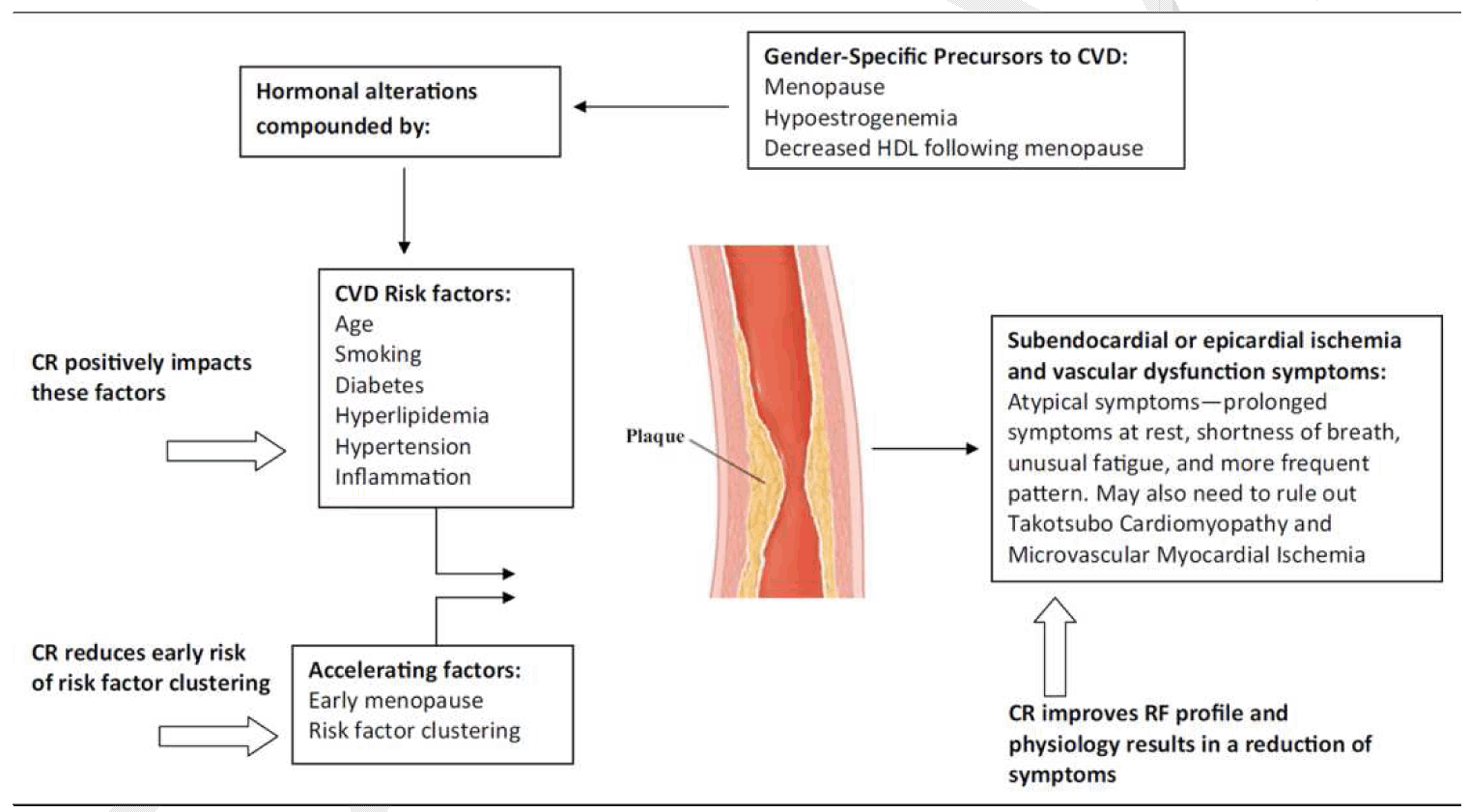
The patient had the general characteristic features of CSX, including angina, evidence of myocardial ischemia and no obstructive CAD by coronary angiography. These findings along with further evaluation and abnormal coronary reactivity testing indicated the specific diagnosis of ischemic cardiomyopathy with microvascular angina secondary to CMD. She was able to increase exercise intensity from 2.1 to 3.3 METs after four sessions of CR program without abnormal chest pain and arrhythmia. While the exercise duration was optimal at 45–50 minutes, low exercise intensity and poor functional capacity were observed. Ideally, a supervised CR program should have been continued but she could not complete a full program of 36 sessions. Home CR program played a key role in this patient, including aerobic exercise, strengthening exercise, stress management technique and healthy heart diet intake. As a multifaceted structured program that encourages exercise, education, nutrition counseling and psychosocial intervention, CR provides a therapeutic opportunity in CSX and microvascular angina patients (Figure 3) [8]. Eriksson et al revealed that there was improvement in exercise capacity by 34%, delayed onset of chest pain during exercise by 100% and tendency to increased endothelium-dependent blood flow in CSX after eight weeks of aerobic exercise [9]. Moreover, the eight-week CR program was shown to modify cardiovascular risk factors, including lower resting diastolic blood pressure and body mass index, improved physical fitness from Shuttle Walk Test performance, reduced symptom severity and improved QOL in CSX patients [10]. In microvascular angina patients, Carvalho et al. reported a case with improved endothelium-dependent vasodilator response of brachial artery, reversal of the ischemic myocardial perfusion defect from single-photon emission computed tomography, improved angina symptoms and QOL after the four-month aerobic training [11]. Our report showed the benefits of CR, including increased exercise intensity, exercise duration, improved functional capacity and decreased anginal symptoms in this patient with proven microvascular angina. Women with CSX often have impaired functional capacity and/or are deconditioned. The DASI is a 12-item self-reported questionnaire that captures functional capacity. The DASI score is validated to estimate maximal oxygen consumption from exercise stress test. By dividing the DASI score by 3.5, METs are derived. The application of DASI might be used instead of exercise stress test to identify at-risk symptomatic women, predict prognosis and target risk management. Among symptomatic women with suspected myocardial ischemia from the NHLBI-WISE study, functional impairment measured by the exercise stress test and DASI-estimated METs =4.7 correlated with an adverse prognosis, including higher death and nonfatal myocardial infarction rates [7]. Notably, even small increases in functional capacity after CR participation could reduce cardiovascular mortality and morbidity. In a retrospective review in women referred for stress testing, for every MET increase in exercise capacity, there was a 25% reduction in the rate of all-cause death [12]. Our patient also reported functional capacity improvement, demonstrated by 3.4 METs increase of DASI score at the fourth-year of follow-up, which suggests better prognosis. In terms of QOL, the eight-week CR program improved QOL scales in women with CSX based on a SF-36 questionnaire [10] [13]. Similarly, a slight increase of a general QOL rating scale and improved overall health status was reported in our patient at the four-year follow-up. Although CR is recommended for all patients with CAD and chronic angina, participation rate is low especially in women [14]. Women are faced with several barriers to CR attendance, including caregiving responsibilities observed in our patient. Referral of women to CR should be strongly considered by physicians, as it positively affects physical and psychological outcomes in patients with CSX, MCD and microvascular angina. | ||||||
| ||||||
|
| ||||||
|
Conclusion
| ||||||
|
This report suggests that cardiac rehabilitation was beneficial in a patient with cardiac syndrome X, cardiac syndrome X, diagnosed with ischemic cardiomyopathy and microvascular angina secondary to microvascular coronary dysfunction. Even though the patient did not complete the cardiac rehabilitation (CR) session plan, CR increased her exercise intensity and duration, improved functional capacity, decreased anginal symptoms and improved quality of life. | ||||||
|
Suggested Reading
| ||||||
| ||||||
|
References
| ||||||
| ||||||
|
[HTML Abstract]
[PDF Full Text]
|
|
Author Contributions
Wipawee Laksanakorn – Substantial contributions to conception and design, Acquisition of data, Analysis and interpretation of data, Drafting the article, Revising it critically for important intellectual content, Final approval of the version to be published Tanaporn Laprattanagul – Substantial contributions to conception and design, Acquisition of data, Analysis and interpretation of data, Drafting the article, Revising it critically for important intellectual content, Final approval of the version to be published Janet Wei – Analysis and interpretation of data, Revising it critically for important intellectual content, Final approval of the version to be published Chrisandra Shufelt – Analysis and interpretation of data, Drafting the article, Revising it critically for important intellectual content, Final approval of the version to be published Margo Minissian – Acquisition of data, Analysis and interpretation of data, Revising it critically for important intellectual content, Final approval of the version to be published Puja K. Mehta – Analysis and interpretation of data, Revising it critically for important intellectual content, Final approval of the version to be published C. Noel Bairey Merz – Substantial contributions to conception and design, Analysis and interpretation of data, Revising it critically for important intellectual content, Final approval of the version to be published |
|
Guarantor of submission
The corresponding author is the guarantor of submission. |
|
Source of support
None |
|
Conflict of interest
Authors declare no conflict of interest. |
|
Copyright
© 2015 Wipawee Laksanakorn et al. This article is distributed under the terms of Creative Commons Attribution License which permits unrestricted use, distribution and reproduction in any medium provided the original author(s) and original publisher are properly credited. Please see the copyright policy on the journal website for more information. |
|
|