|

|
 |
|
Case Report
| ||||||
| Local invasion of jaw osteosarcomass | ||||||
| Roberto Fiori1, Dominique De Vivo1, Angela Lia Scarano1, Silvia D'Onofrio1, Eros Calabria1, Simonetti Giovanni2 | ||||||
|
1MD, Department of Diagnostic and Molecular Imaging, Interventional Radiology and Radiation Therapy, Fondazione Policlinico "Tor Vergata", Viale Oxford 81, Rome, Italy.
2MD, PhD, Prof, Department of Diagnostic and Molecular Imaging, Interventional Radiology and Radiation Therapy, Fondazione Policlinico "Tor Vergata", Viale Oxford 81, Rome, Italy. | ||||||
| ||||||
|
[HTML Abstract]
[PDF Full Text]
[Print This Article]
[Similar article in Pumed] [Similar article in Google Scholar] 
|
| How to cite this article |
| Fiori R, De Vivo D, Scarano AL, D'nofrio S, Calabria E, Giovanni S. Local invasion of jaw osteosarcoma. Int J Case Rep Images 2015;6(4):224–227. |
|
Abstract
|
|
Introduction:
One of the most common primary malignant bone tumor is osteosarcoma that counts high percentages in the level of incidence the 5% of all tumor in children, and the 9% of all sarcomas. Osteosarcoma are malignant bone tumors developing from mesenchymal tumor cells that growth as disorganized immature bone or osteoid tissue. Patients affected by osteosarcoma show a peak incidence related to puberty (for young female 12±2 years and for young male 16±1.8 years). Regardless of the favorable biological behaviour, the patients of jaw osteosarcoma usually exhibit advanced tumor as it often goes unnoticed by the dental professional thus stressing on the need for early diagnosis of the lesion.
Case Report: We report an unusual case history of a 34-year-old male with swelling and blood loss in anterior gingival of maxilla with loss of teeth. Conclusion: There are three main methods to diagnose the tumor based on clinical and radiographic characteristics before confirmation by histology and to bring attention to dental professional to approach cases diagnosing them at an early stage leading to better prognosis. | |
|
Keywords:
Bone tumor, Jaw, Maxillofacial neoplasms, Mesenchymal neoplasia, Osteosarcoma
| |
|
Introduction
| ||||||
|
One of the most common primary malignant bone tumor is osteosarcoma that counts high percentages in the level of incidence the 5% of all tumor in children, and the 9% of all sarcomas. Osteosarcoma are malignant bone tumors developing from mesenchymal tumor cells that growth as disorganized immature bone or osteoid tissue [1] [2]. Patients affected by osteosarcoma show a peak incidence related to puberty (for young female 12±2 years and for young male 16±1.8 years) [1]. Osteosarcoma is an osteoid-producing malignant mesenchymal tumor and accounts for 15–35% of all primary bone tumors although only 6–10% of osteosarcomas occur in the craniofacial region [3]. The international ranks consider the mandible as the common site of involvement, immediately followed by maxilla and skull [4] [5]. The gold standard is an early diagnosis in order to prevent its continuous infiltrative growth [6]. Osteosarcoma usually metastasizes through the blood such as mesenchymal malignancy. The aim of this case report is to highlight how malignant neoplasm with continuous autonomous growth, and to make a comparison between osteosarcoma in general and osteosarcoma of the jaw that is known to have a relatively low incidence of metastasis and a better prognosis [7]. | ||||||
|
Case Report
| ||||||
|
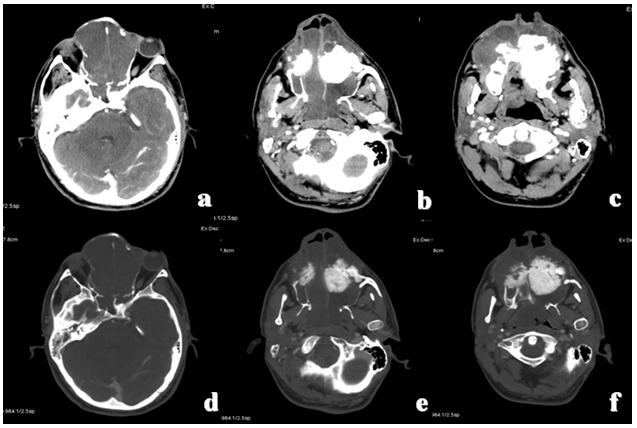
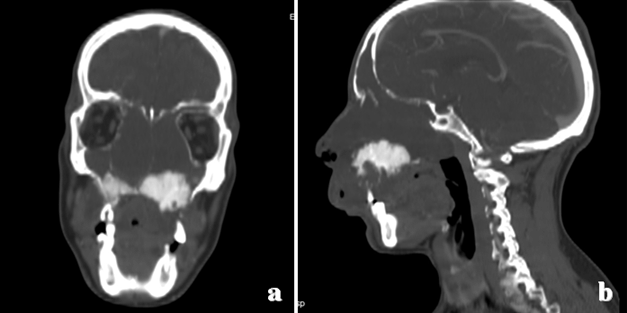
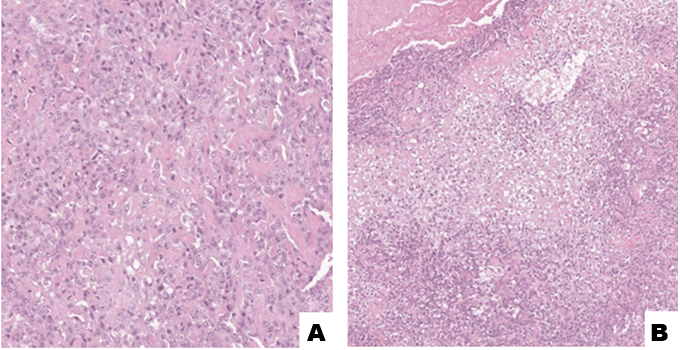
A 34-year-old male was admitted to our emergency department with the complaint of a painless swelling of the cheek gradually enlarging for over nine months and difficulty in swallowing solids and liquids and progressive loss of teeth in the upper maxilla. On physical examination, the patient presented mild displacement of the eye, difficulty in opening the mouth, gingival swelling, tears from eyes and loss of teeth on the upper maxilla. He showed pain on palpation, the swelling was firm, hard and immovable and was fixed to the underlying bone. At intraoral examination, the patient had a great mass extending intraoral into the hard palate as an ulcerated, painful mass invading the nasal cavity. Blood pressure, pulse and respiratory rate and temperature were normal. After admitting to emergency department the patient underwent contrast-enhanced computed tomography (CT) scan which revealed tumor with a major component like soft tissue, central calcification/ossification, originating in the left upper quadrant of the maxilla and invading the nasal cavity, the ethmoid cells, the sphenoidal and frontal sinuses, the right upper quadrant of the maxilla, the left alveolar process, the hard palate and the base of the orbit without involvement of the orbital adipose tissue. Computed tomography scan examination before and after injection of contrast medium also showed the involvement of the tumor mass to the parotid gland, the masseteric fossa and the infra-temporal fossa bilaterally with multiple increased lymph nodes on mandibular angle and in lateral cervical region the invasion (Figure 1) and (Figure 2). We elaborated three-dimensional images to better define the extension of the lesion (Figure 3). In the suspicion of distal localization the patient underwent CT whole body which was negative. A biopsy under local anesthesia proved coexistence of osteoblastic and chondroblastic osteosarcoma (Figure 4). So-called osteoblastic osteosarcoma is dominated by the production of extracellular bone matrix. This picture demonstrates immature bone deposition into which tumor cells are incorporated. So-called chondroblastic osteosarcoma. This picture is dominated by cellular hyaline cartilage with wisps of osteoid formation. The patient was admitted to oncological center for further evaluation and treatment. Chemotherapy was performed and nowadays the patient is in a periodical follow-up. Osteosarcoma is the second primary malignant tumor of the bone after multiple myeloma although its localization in the orofacial region is rare [8]. Among the possible symptoms that patients usually present there are pain, paresthesia and swelling of the area similar to osteomyelitis, ossifying fibroma, periostitis, osteoblastoma, suppurative osteomyelitis, and even fibrous dysplasia [7] [9]. | ||||||
|
| ||||||
|
| ||||||
| ||||||
|
| ||||||
|
Discussion
| ||||||
|
Osteosarcoma is a frequent primary malignant bone tumor and it rarely appears in the orofacial anatomical region. The patients usually refer pain, swelling and sometimes bleeding from the interested area. In a relatively short time the affected patients present paresthesias, initial mobility and then loss of the tooth. These clinical non-specific symptoms are similar to some benign tumors, malign tumors and infective disease (osteoblastoma, ossifying fibroma, fibrous dysplasia and infective pathologies like osteomyelitis with proliferative periostitis, suppurative osteomyelitis)[1] [2] [3] [4] [5] [6] [7]. For these reasons radiologic and histopathologic characterization in association with clinical examination are necessary in detecting the kind of disease in order to plan a correct management of the case. On a radiographic examination osteosarcoma can present as radiopacity, radiolucency or a mixed aspect [4]. In some cases, there should be widening of the periodontal ligament space also known as Garrington sign [10]. A plain radiograph usually demonstrates a destructive mass associated to irregular, spiculated periosteal reaction [11]. An integrative CT scan confirms irregular mass with periosteal and endosteal reaction even if osteosarcoma and fibrous dysplasia have a similar presentation even if as "sunray spiculations" in soft tissue could indicate osteosarcoma. For these reason the gold standard is a histologic evaluation through a biopsy. The histological appearance of osteosarcoma is highly variable, in the jaw the most frequent variant is the chondroblastic pattern. Deep biopsy should be recommended to avoid the histological characterization of the periosteal reaction (Table 1). In osteosarcoma, there is a direct formation of osteoid from a sarcomatous tissue variable from a sclerotic osseous tumor to diffuse osteoid aspect. The stromal cells may be osteoblastic, chondroblastic, and/or fibroblastic. The most common form is osteoblastic growth but in the jaws localization the most common aspect is chondroblastic pattern. In case of osteosarcoma, a not rare event is the recurrence or metastases appearances. The most frequent target organ is the lung, for this reason a chest X-ray or a chest CT scan is mandatory for surgical and or oncological planning. In our case, the patient was in an advanced stage of the disease and there was a high probability of metastatic lesions. The patient underwent cycles of chemotherapy and surgical intervention in another hospital and he is actually undergoing trimestral clinical and radiological follow-up. A late diagnosis do not allow good life expectancy and the prognosis is very poor. | ||||||
| ||||||
|
| ||||||
|
Conclusion
| ||||||
|
In conclusion, osteosarcoma of the jaw is an aggressive bone tumor that should be treated at referral centres, by a multidisciplinary team (radiologist, oncologists, maxillofacial, and head and neck surgeons, radiotherapist, maxillofacial prosthodontist including plastic surgeons) with a experience managing these lesions because an early diagnosis could allow a better prognosis for the patient consisting in a complete tumor resection and planning maxillofacial reconstruction. | ||||||
|
References
| ||||||
| ||||||
|
[HTML Abstract]
[PDF Full Text]
|
|
Author Contributions
Roberto Fiori – Substantial contributions to conception and design, Acquisition of data, Analysis and interpretation of data, Drafting the article, Revising it critically for important intellectual content, Final approval of the version to be published Dominique De Vivo – Analysis and interpretation of data, Drafting the article, Revising it critically for important intellectual content, Final approval of the version to be published Angela Lia Scarano – Analysis and interpretation of data, Drafting the article, Revising it critically for important intellectual content, Final approval of the version to be published Silvia D'Onofrio – Analysis and interpretation of data, Drafting the article, Revising it critically for important intellectual content, Final approval of the version to be published Eros Calabria – Analysis and interpretation of data, Drafting the article, Revising it critically for important intellectual content, Final approval of the version to be published Simonetti Giovanni – Analysis and interpretation of data, Drafting the article, Revising it critically for important intellectual content, Final approval of the version to be published |
|
Guarantor of submission
The corresponding author is the guarantor of submission. |
|
Source of support
None |
|
Conflict of interest
Authors declare no conflict of interest. |
|
Copyright
© 2015 Roberto Fiori et al. This article is distributed under the terms of Creative Commons Attribution License which permits unrestricted use, distribution and reproduction in any medium provided the original author(s) and original publisher are properly credited. Please see the copyright policy on the journal website for more information. |
|
|