|

|
 |
|
Case Report
| ||||||
| Iatrogenic saline toxicity complicated by malnutrition | ||||||
| Muhammad Uneib1, Parin Rimtepathip2, Harold P. Katner3 | ||||||
|
1MS III, Ross University School of Medicine.
2MS III, Mercer University School of Medicine. 3MD, Department of Infectious Disease, MUSM. | ||||||
| ||||||
|
[HTML Abstract]
[PDF Full Text]
[Print This Article]
[Similar article in Pumed] [Similar article in Google Scholar] 
|
| How to cite this article |
| Uneib M, Rimtepathip P, Katner HP. Iatrogenic saline toxicity complicated by malnutrition. Int J Case Rep Images 2015;6(4):216–219. |
|
Abstract
|
|
Introduction:
Hypotension is a common presenting symptom in elderly patients with malnutrition and dehydration, often being treated with a continuous volume of 0.9% normal saline. Since normal saline is slightly hypertonic, prolong continuous treatment with normal saline can result in hyperchloremic non-anion gap metabolic acidosis. Patients with a low albumin state are also at risk for third spacing that can lead to generalized edema.
Case Report: We present a 63-year-old Caucasian female with history of schizophrenia, traumatic brain encephalopathy, and chronic kidney disease stage III who presented to the emergency room from a nursing home due to altered mental status and low blood pressure. The patient received continuous infusion of normal saline despite failure of improvement in blood pressures due to the wrong diagnosis of the cause of hypotension. The patient ended up with iatrogenic normal saline toxicity. Conclusion: It is important for healthcare professionals to recognize signs and symptoms of normal saline toxicities especially in elderly patients with many chronic illnesses. Hypotension treated with continuous normal saline will eventually led to hyperchloremic metabolic acidosis with edema from third spacing in patients with low albumin secondary to malnutrition. | |
|
Keywords:
Hyperchloremic metabolic acidosis, Malnutrition, Normal saline, Toxicity
| |
|
Introduction
| ||||||
|
Infusing large volumes of 0.9% sodium chloride (saline) to patients can cause toxicities of both hyperchloremic metabolic acidosis and edema of the surrounding tissues [1]. The most commonly used resuscitation fluid in the United States especially for patients presenting with signs and symptoms of dehydration is 0.9% normal saline. Malnutrition and dehydration present very similar among the elderly patients, especially those with altered mental status and underlying causes such as psychiatric disturbances, stroke, or chronically ill. Both the chronic hypoalbuminemia that accompanies critical illness and the acute dilutional hypoalbuminemia that accompanies rapid crystalloid infusion effectively reduce the upper limit of the normal range of the anion gap because approximately 75% of the normal anion gap is composed of the negatively charged albumin molecule [2]. Malnutrition patients who are often misdiagnosed as dehydration often get treated for dehydration with large volumes of 0.9% saline but with lack of clinical improvement. Health care professionals need to properly screen and assess for malnutrition especially in vulnerable population. Without the right treatment for the cause, high volume of normal saline can be hazardous to those patients because it can cause metabolic derangement. We describe a case of 63 years old Caucasian female with a history of schizophrenia, traumatic brain encephalopathy, and chronic kidney disease stage III, who presented to the emergency department from a nursing home due to altered mental status with hypotension. | ||||||
|
Case Report
| ||||||
|
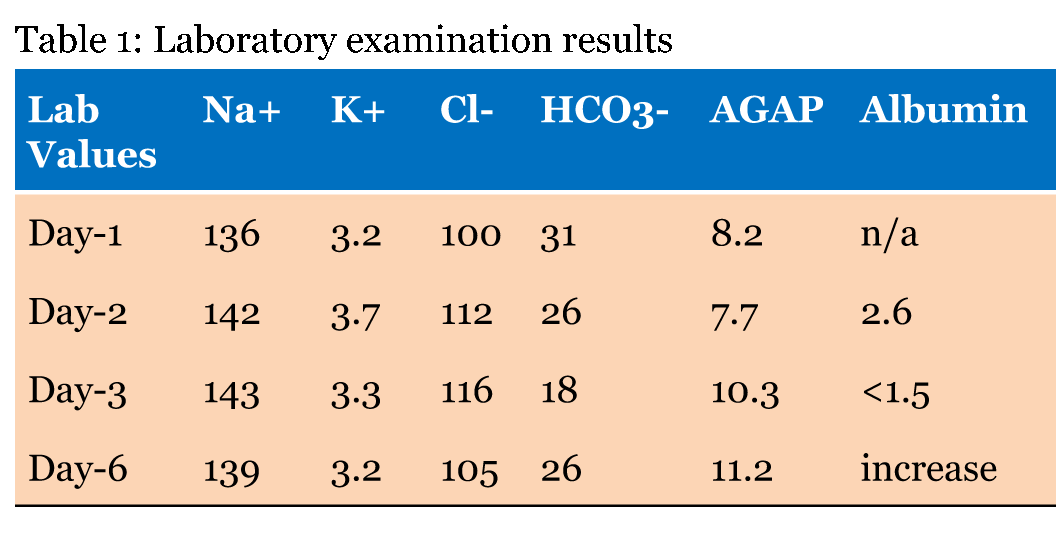
A 63-year-old Caucasian female with history of schizophrenia, traumatic brain encephalopathy, and chronic kidney disease stage III, presented to the emergency department due to altered mental status and a decline in blood pressures. Upon admission, the blood pressure was initially 107/56 mmHg but dropped to 73/56 mmHg, her heart rate was 75 bpm, respiratory rate 16 bpm, and temperature 36.9 °C. The patient was given norepinephrine 8µg/min IV infusion and IV fluids in the emergency department for stabilization. Her laboratory values were obtained which showed sodium 136, potassium 3.2, chloride 100, and bicarbonate 31. coagulations, liver enzymes, urinalysis, and chest X-ray were within normal limits. On day-2 of admission, the patient continuously received 0.9% saline IV fluids for hypotension with the blood pressure of 84/45, heart rate of 76, respiratory rate of 13, and oxygen saturation of 100 on nasal canula. Laboratory examination on day-2 showed Na+ 142, K+ 3.7, Cl- 112, HCO3- 26, and albumin 2.6. Blood cultures were positive for Staphylococcus capitis in one of the four cultures. The patient was treated with oxacillin. On day-3 of admission, despite the continuous 0.9% saline IV and treatment of bacteremia, patient was still hypotensive with blood pressure of 85/43. Serum chemistries on day-3 showed Na+ 135, K+ 3.7, Cl- 116, HCO3- 18, and albumin of <1.5. Physical examination showed new findings of pitting edema on her extremities. Computed tomography scan of the abdomen and pelvis was obtained due to possible internal bleed as the cause of hypotension. The patient was scanned through the abdomen pelvis with no intravenous of oral contrast. The study did not reveal any retroperitoneal or intraperitoneal hemorrhage. However, there were small bilateral pleural effusions, small ascites, and small free fluid in the pelvis. There was mild diffuse mesenteric edema, mild edema at the pelvic floor and in the perirectal soft tissues. On day-4, infection disease department was consulted due to failure of improvement of the blood pressure despite antibiotic treatment with additional onset of pitting edema and new findings on the CT scan. Per consultation; Staphylococcus capitis bacteremia was not the cause of hypotension due to only one out of the four cultures was positive with normal white blood cell count and lactic acid level. Laboratory values also showed normal anion gap with increased in chloride level (Table 1). Staphylococcus capitis was probably positive on blood culture due to contaminant. The consultation described the low albumin level as possible malnutrition due to normal liver enzyme with no protein in the urine as patient was not swallowing her food per discussion with the nurses plus the history of being an elderly with AMS and schizophrenia. The patient was then replaced with 25 g albumin infusion (25% solution) with monitored blood pressure. On day-6 of admission, the hypotension resolved with albumin with blood pressure of 116/75 mmHg. Patient was considered for peg tube placement for malnutrition with stoppage of the 0.9% normal saline due to normal saline toxicity. | ||||||
| ||||||
|
Discussion
| ||||||
|
Malnutrition is defined as imbalance of nutrients mainly due to poor oral intake often seen in the elderly patients, especially those with underlying causes such as psychiatric disturbances, stroke, and chronically ill. Physical factors that affect malnutrition include oral health (i.e., decrease oral intake), physical impairment, early satiety, and taste and smell changes [3]. As the research statistics indicate, not only is malnutrition prevalent in the elderly, but also frequently misdiagnosed or unrecognized. Many health care professionals are not properly screening or assessing malnutrition in the elderly [4]. This case described an elderly patient with history of schizophrenia, although initial presentation was consistent with dehydration from abnormal laboratory values, the lack of improvement after normal saline infusion for a prolonged time course, suggested needs for additional diagnosis. After the exclusion of bacteremia as the cause of hypotension, abnormally low albumin level should have been considered as the culprit for hypotension, especially with no proteinuria and normal liver enzymes. Correct treatment is absolutely dependent on differentiation of hyperchloremic (non-anion gap) acidosis from lactic acidosis [5]. Aggressive attempts to improve organ perfusion, based on misdiagnosis of lactic acidosis, could prove harmful just like our patient with normal lactic acidosis and non-anion gap metabolic acidosis. Normal saline is considered as hypertonic solution because it has an osmolality of 308 mOsm/L, with electrolyte composition consisting of 154 mmol/L of Na+ and 154 mmol/L of Cl- [6]. While normal saline is slightly hypertonic and does not create a huge imbalance in body fluids or electrolytes, there are few major precautions. Two major complications of normal saline toxicities are hyperchloremic non-anion gap metabolic acidosis and the edematous state from third spacing especially in patients with low albumin level. The index patient showed signs of normal saline toxicity with both two major complications proven with CT scan of abdomen pelvis and abnormal laboratory values. It is important to point out that aggressive fluid therapy should be carefully monitored as our patients were almost "flood" with excessive fluid. Prolonged course of uncorrected hypotension with normal saline solutions accompanied by laboratory values of hyperchloremia, non-anion gap metabolic acidosis, no proteinuria, normal liver function, and low albumin should prompt a differential diagnosis of malnutrition. Albumin played an important role by maintaining intravascular oncotic pressure and homeostasis. Decrease in albumin level will eventually led to decrease in oncotic pressure with increased in capillary pressure. A prolonged decreased in oncotic pressure and increased in capillary pressure will eventually resulted in dehydration due to the escape of fluid from intravascular to interstitial space. These patients need to be taken off the fluid immediately with prompt administration of albumin as a correct treatment for their dehydration. | ||||||
|
Conclusion
| ||||||
|
In conclusion, elderly patients are at the pinnacle upon risk for malnutrition. Malnutrition is often unrecognized and under-treated by healthcare professionals. When these patients presented with clinical symptoms of severe dehydration with no improvement upon normal saline infusion, electrolytes, anion gap, and albumin level should be acquired. These laboratory values especially the anion gap and chloride level should be taken advantaged of due to their availability to assist in diagnosing underlying reasons for hypotension in malnutrition versus bacteremia in elderly patients especially those with history of physiological and mental incapability. | ||||||
|
References
| ||||||
| ||||||
|
[HTML Abstract]
[PDF Full Text]
|
|
Author Contributions
Muhammad Uneib – Substantial contributions to conception and design, Drafting the article, Revising it critically for important intellectual content, Final approval of the version to be published Parin Rimtepathip – Substantial contributions to conception and design, Drafting the article, Revising it critically for important intellectual content, Final approval of the version to be published Harold P. Katner – Substantial contributions to conception and design, Drafting the article, Revising it critically for important intellectual content, Final approval of the version to be published |
|
Guarantor of submission
The corresponding author is the guarantor of submission. |
|
Source of support
None |
|
Conflict of interest
Authors declare no conflict of interest. |
|
Copyright
© 2015 Muhammad Uneib et al. This article is distributed under the terms of Creative Commons Attribution License which permits unrestricted use, distribution and reproduction in any medium provided the original author(s) and original publisher are properly credited. Please see the copyright policy on the journal website for more information. |
|
|