|

|
 |
|
Clinical Image
| ||||||
| Clavicle chronic recurrent multifocal osteomyelitis: Surgical excision and neo-clavicle | ||||||
| Jorge H. Costa1, Tiago P. Marques2, Miguel Pádua3 | ||||||
|
1MD, Orthopedics and Traumatology Resident at Hospital Curry Cabral,Lisboa, Portugal.
2MD,Orthopedics and Traumatology Resident at Hospital Santarém,Santarém, Portugal. 3MD, Orthopedics and Traumatology Resident at Hospital Fernando da Fonseca, Amadora, Portugal. | ||||||
| ||||||
|
[HTML Abstract]
[PDF Full Text]
[Print This Article]
[Similar article in Pumed] [Similar article in Google Scholar] 
|
| How to cite this article |
| Costa JH, Marques TP, Pádua M. Clavicle chronic recurrent multifocal osteomyelitis - Surgical excision and neo-clavicle.. Int J Case Rep Images 2015;6(4):251–254. |
|
Case Report
| ||||||
|
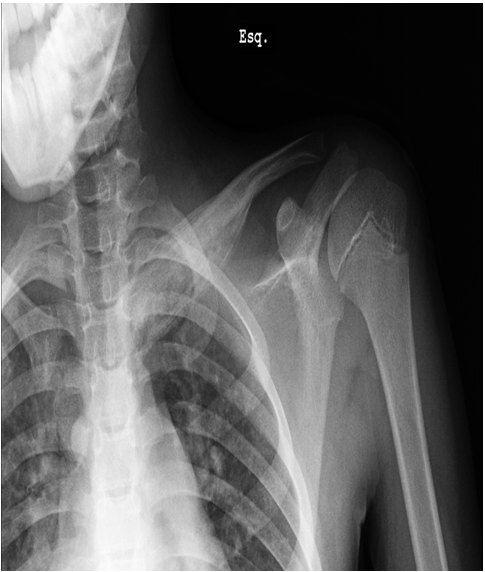
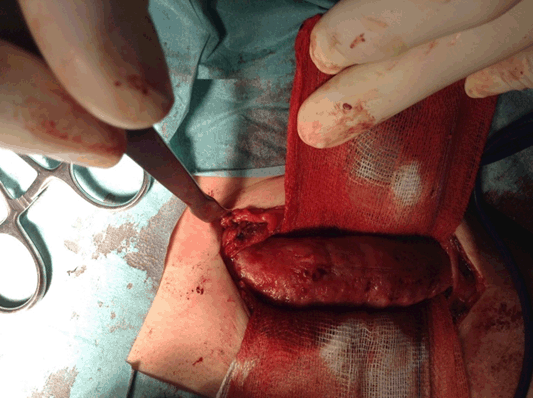
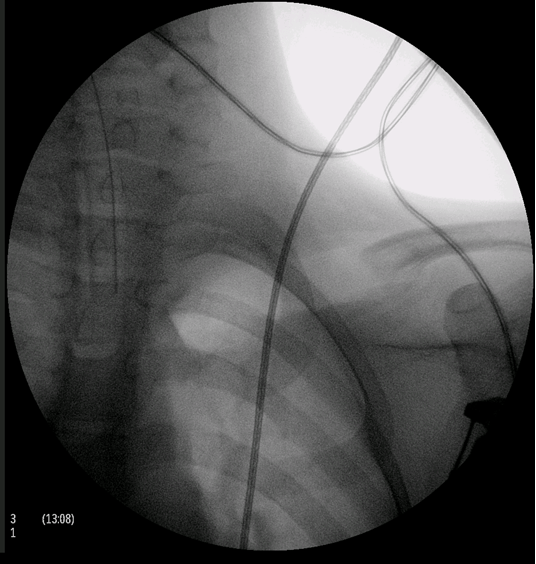
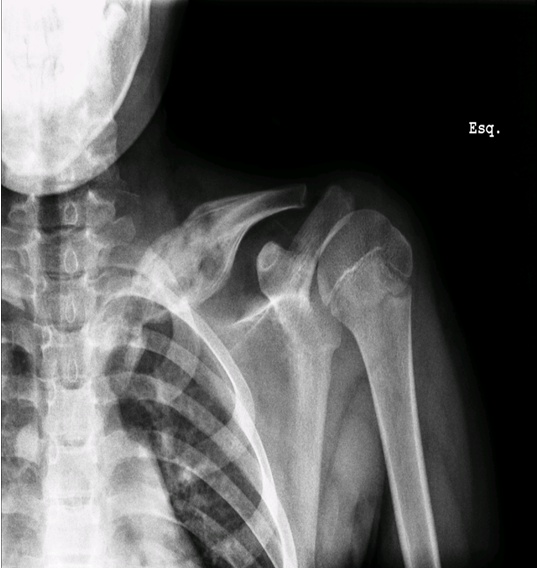
This is a case of an 11-year-old boy with left clavicle pain with two months of evolution presented to emergency department. No history of trauma, fever or systemic signs, recent illness and no relevant personal or familiar medical history. No neurological or vascular abnormalities were found in the upper arms. Left shoulder X-ray revealed a hyperdense lesion and increased thickness of left clavicle (Figure 1). In this context a computed tomography (CT) scan and after a magnetic resonance imaging (MRI) scan were ordered. Both scans demonstrated morphological changes of the median half of the clavicle, cortical destruction and periosteal reaction. Also changes in the surrounding soft and muscular tissue and bulky and numerous locoregional ganglion formations (Figure 2) and (Figure 3). Blood analysis, blood cultures and bone biopsy were negative for infection and neoplastic disorder. In this context, by exclusion, and in the presence of two Jansson major diagnostic criteria (radiologically proven osteolytic/osteosclerotic bone lesions and sterile bone biopsy with signs of inflammation) [1], we reached the diagnosis of chronic recurrent multifocal osteomyelitis (CMRO) (Table 1). Patient was treated with NSAIDs for six months and a short course of corticoids without any response. By keeping complaints of marked and recalcitrant pain in clavicle region, we opted for the surgical treatment: resection of the lesion en bloc, about 7 cm of clavicle (Figure 4), maintaining the integrity of periosteum to allow neo-osteogenesis of the clavicle. No bone grafting or another material was interposed in the dead space left by the resection of the clavicle. Post operatory X-ray, showing a radiopaque area corresponding to the excision of the medial portion of the clavicle (Figure 5). At third month after surgery, there is an image compatible with a neo-clavicle and patient is asymptomatic (Figure 6). | ||||||
| ||||||
| ||||||
|
| ||||||
| ||||||
| ||||||
| ||||||
|
| ||||||
| ||||||
|
Discussion
| ||||||
|
Chronic recurrent multifocal osteomyelitis is a non-bacterial bone inflammation (osteitis), that has symptoms similar to the conventional osteomyelitis, but without infection. It is characterized by multifocal bone lesions with pain and swelling recurring over months to years, accounting of 2 to 5% of all cases of osteomyelitis [2] [3] mostly children and adolescents. The differential diagnosis includes bacterial osteomyelitis, Ewing sarcoma, leukemia, lymphoma, rhabdomyosarcoma, neuroblastoma metastasis, eosinophilic granuloma or Langerhans cell histiocytosis. The tubular long bones, pelvis, hip, sternum and mandible are the most affected bones [4] [5]. The CRMO, in pediatric patients , may be associated with various skin disorders: Pustulosis palmoplantar is syndrome [6] [7] [8], diffuse pustulosis, psoriasis vulgaris, acne [9] [10] [11], Sweet's syndrome and pyoderma gangrenosum [9]. Multiple sites of apparent osteomyelitis with negative pathology and cultures and no response to antibiotherapy characterize it [12]. NSAIDs as naproxen, indomethacin or aspirin are the initial therapy. A short course of corticosteroids can be used in refractory cases. Other treatments such as sulfasalazine or methotrexate [6], bisphosphonates [13] and hyperbaric chamber [14] are also indicated in refractory cases. Antibiotics do not seem to be helpful. Although surgical treatment has been used, its role is not yet clearly defined. We opted for a surgical excision of the clavicle, because of the constant and intense pain with no response to six months of conservative treatment. We think that the good response to surgery makes this case exceptionally unusual. The prognosis for these patients is however good. In one study, 17 of 23 patients had complete resolution of the clinical findings, at an average of 5.6 years after diagnosis. Six patients continue to have active disease, and the other six had intermittent relapses or chronic pain. 78% had no physical impairment [2], but further prospective studies are needed to determine the optimum outcome measures and treatment strategy [15], | ||||||
|
Conclusion
| ||||||
|
The absence of positive microbiologic results, the clinical course and the presence of reactivating and remitting lesions over time suggest the diagnosis of chronic recurrent multifocal osteomyelitis. As the disease is self-limiting, knowledge of its characteristics appearance can lead to the most appropriated treatment, and can prevent overly aggressive medical and surgical evaluation and treatment. | ||||||
|
References
| ||||||
| ||||||
|
[HTML Abstract]
[PDF Full Text]
|
|
Author Contributions
Jorge H. Costa – Substantial contributions to conception and design, Acquisition of data, Analysis and interpretation of data, Drafting the article, Revising it critically for important intellectual content, Final approval of the version to be published Tiago P. Marques – Analysis and interpretation of data, Revising it critically for important intellectual content, Final approval of the version to be published Miguel Pádua – Analysis and interpretation of data, Revising it critically for important intellectual content, Final approval of the version to be published |
|
Guarantor of submission
The corresponding author is the guarantor of submission. |
|
Source of support
None |
|
Conflict of interest
Authors declare no conflict of interest. |
|
Copyright
© 2015 Jorge H. Costa et al. This article is distributed under the terms of Creative Commons Attribution License which permits unrestricted use, distribution and reproduction in any medium provided the original author(s) and original publisher are properly credited. Please see the copyright policy on the journal website for more information. |
|
|