|

|
 |
|
Case Report
| ||||||
| Primary intratesticular leiomyosarcoma in a 78-year-old male | ||||||
| Wissem Hmida1, Faouzi Mallat1, Mouna Ben Othmen1, Khaled Ben Ahmed1, Sidiyaould Chavey2, Sarra Mestiri3, Amel Ben Abdallah2, Faouzi Mosbah4 | ||||||
|
1MD, Department of Urology, Sahloul Hospital, Sousse, Tunisia.
2MD, Department of Radiology, Sahloul Hospital, Sousse, Tunisia. 3MD, Department of Pathology, Farhat Hached Hospital, Sousse, Tunisia. 4Professor, Department of Urology, Sahloul Hospital, Sousse, Tunisia. | ||||||
| ||||||
|
[HTML Abstract]
[PDF Full Text]
[Print This Article]
[Similar article in Pumed] [Similar article in Google Scholar] 
|
| How to cite this article |
| Hmida W, Mallat F, Othmen MB, Ben Ahmed K, Chavey S, Mestiri S, Abdallah AB, Mosbah F. Primary intratesticular leiomyosarcoma in a 78-year-old male. Int J Case Rep Images 2014;5(10):717–722. |
|
Abstract
|
|
Introduction:
Primary leiomyosarcoma of the testis is a rare entity with only less than 20 cases were reported. The standard therapy is difficult to recommend because of the rarity of this tumor.
Case Report: We reported a case of primary intratesticular leiomyosarcoma in a 78-year-old male with unremarkable past medical history. The patient was presented within isolated testicular enlargement. Ultrasound revealed a large solid, homogenous and hyper echoic mass of the right testicle. Lactate dehydrogenase (LDH) was elevated, however, serum alpha-fetoprotein (AFP) and beta-human chorionic gonadotropin (β-hCG) were within normal limits. A right radical orchidectomy was performed. The diagnosis of primary leiomyosarcoma of testis was confirmed by histopathology. Conclusion: The primary leiomyosarcoma of testis is a rare diagnosis which should be one of the differential diagnoses of testicular mass with normal tumor markers. | |
|
Keywords:
Testis, Intratesticular tumor, Leiomyosarcoma, Radical orchiectomy
| |
|
Introduction
| ||||||
|
Leiomyosarcomas are malignant soft-tissue tumors arising from any tissues containing smooth muscles. However, intratesticular leiomyosarcoma are extremely rare compared with the paratesticular leiomyosarcoma [1]. We report a case of intratesticular leiomyosarcoma in a 78-year-old male who underwent right radical orchiectomy. | ||||||
|
Case Report
| ||||||
|
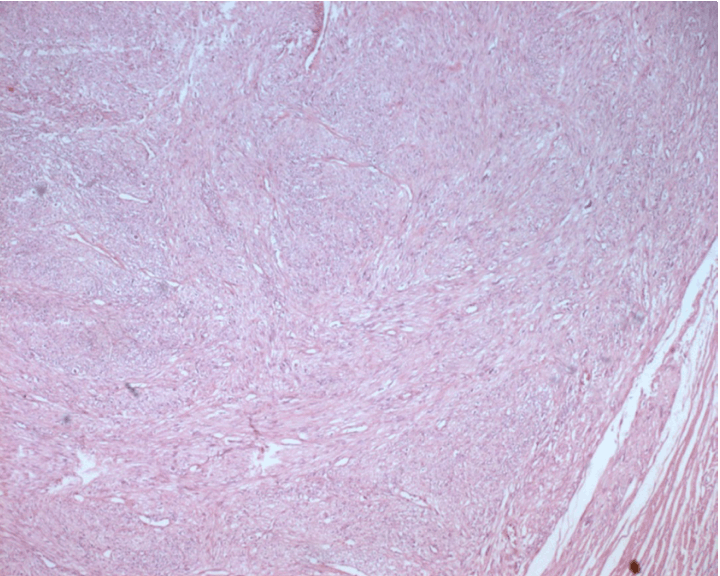
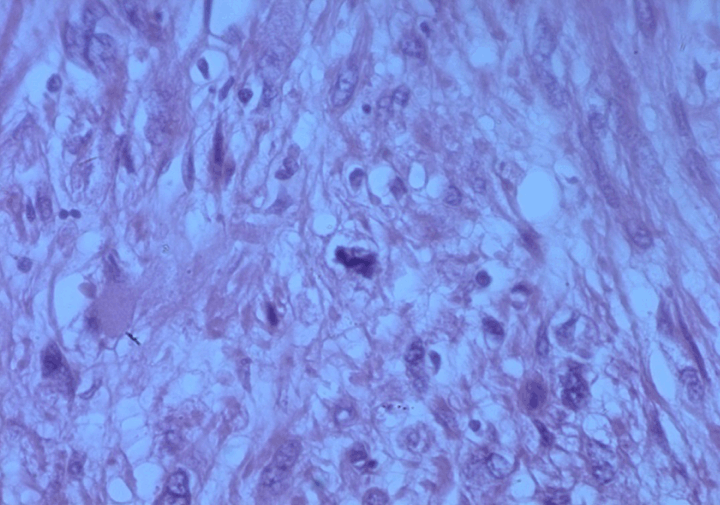
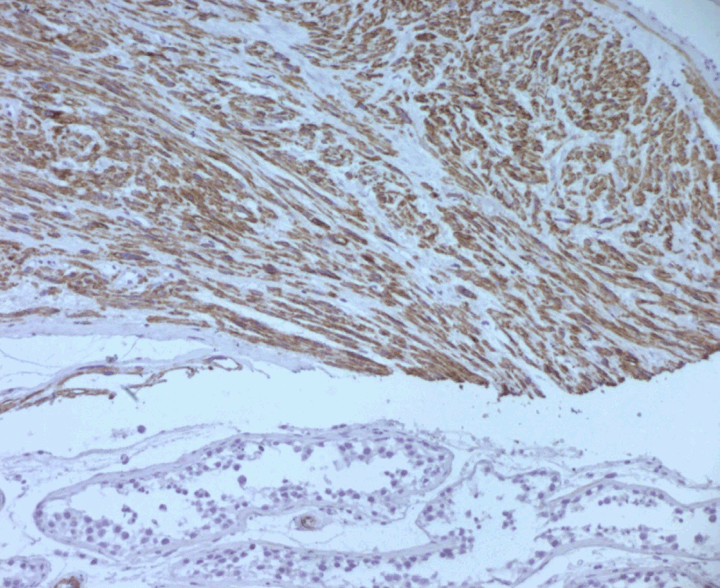
A 78-year-old male patient was presented with a two-year history of right scrotal mass. He had no significant past medical history. He did not receive any radiation therapy or anabolic corticosteroids in the past. No urologic or constitutional symptoms such as voiding complaints, weight loss, fatigue or fever were present.Physical examination revealed a hard, non-tender, right scrotal mass measuring 10x8x8 cm and did not reveal any superficial lymph node swelling. No ulceration of the overlying skin was evident. The digital rectal examination revealed a benign enlarged prostate. Scrotal ultrasonographic examination revealed a solid homogenous hyperechoic mass of the right testicle measuring 9x8x8 cm. The left testicle and both epididymides were unremarkable and there was no evidence of hydrocele or paratesticular pathology.Computed tomography (CT) scan of the chest, abdomen and pelvis revealed no evidence of metastatic disease or lymphadenopathy. Tumor markers serum beta-human chorionic gonadotropin (β-hCG) and alpha-fetoprotein (AFP) were within normal ranges. Serum lactate dehydrogenase (LDH) was raised (880 U/L, normal limit 100–190 U/L). The patient underwent a high ligation of the cord with right radical orchiectomy. Macroscopically, the tumor was a well-encapsulated grey white solid mass with hemorrhage and necrosis. There was no invasion to the spermatic cord or tunica vaginalis. The weight of the tumor was 450 grams and the size was approximately 11×10×9 cm. Microscopic examination showed a high degree of cellular proliferation composed of spindle cells with round or oval-shaped nuclei implicating a storiform growth pattern (Figure 1). Necrosis was evident. Immunohistochemical examination revealed that the tumor cells were strongly positive for calponin, epithelial membrane antigen (EMA) smooth muscle actin and vimentin (Figure 2) and (Figure 3) but negative for S-100 and myogenic regulatory protein (MyoD1) proteins. The combined histologic and immunohistochemical findings were diagnostic of primary high-grade intratesticular leiomyosarcoma. With 24 months of follow-up, which included computed tomography scan of the abdomen, pelvis, bone, and chest, the patient remained free of disease. | ||||||
| ||||||
| ||||||
| ||||||
|
Discussion
| ||||||
|
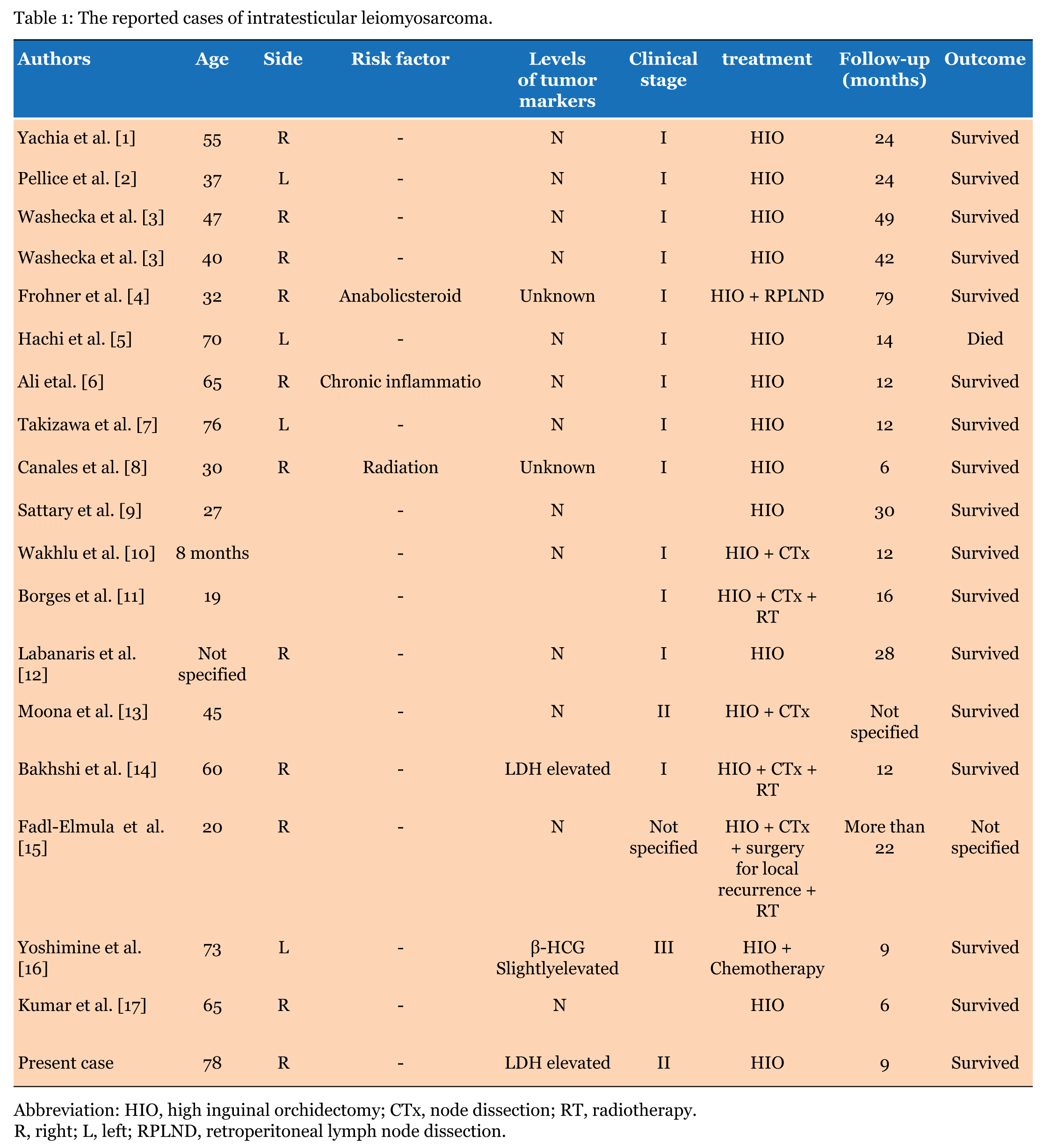
Primary leiomyosarcoma of the testis is an extremely rare tumor. To our knowledge, only less than 20 cases have been reported (Table 1). Smooth muscle elements of the testicular parenchyma, especially blood vessels and the contractile cells of seminiferous tubules, appear to be the origin of intratesticular leiomyosarcoma [1] [18]. The real etiology of testicular leiomyosarcoma is already unknown, but hormonal stimulation has been suggested to have a role in the carcinogenesis of leiomyosarcoma [4]. In fact, it mostly occurs in young men in whom there is an associated history of high doses of anabolic steroids [4] or chronic inflammation [6]. Our patient does not have any risk factor. The clinical presentation and radiological finding of this tumor are non-specific. It seems to be not different from other malignant testicular tumors. Tumor markers (AFP, β-hCG and LDH) used in the previously reported cases were almost within the normal range, except two cases: one case with an elevated LDH [14] and the second with elevated β-hCG [16]. This case had an elevated LDH. Diagnosis is based only on histologic and immunohistochemical findings. Histologically, the nuclei of malignant smooth muscle cells are typically and selectively stain with antibodies against smooth muscle actin and desmin vimentin, but negative for S-100, CD-34, CD-68 and HMB-45. The high mitotic activity is considered an important criterion for malignancy [9]. These tumors might spread via three routes: local invasion, lymphatic dissemination and hematogenous metastasis [8]. Metastasis was extremely rare, only one case developed pulmonary metastasis 14 months after surgery [5]. The treatment of leiomyosarcoma is not codified, it is difficult to recommend due to the few reported cases, and multi-therapy approach may be needed. High inguinal orchiectomy (HIO) appears to be the treatment of choice in cases at low stage [18] [19]. Although, adjuvant treatment chemotherapy and radiotherapy may be used for intratesticular leiomyosarcoma with high stage [14]. This case was treated with HIO without any adjuvant treatment and after 24 months of follow-up the patient was free of disease. | ||||||
| ||||||
|
| ||||||
|
Conclusion
| ||||||
|
Testicular leiomyosarcoma is a rare disease. Based on a review of literature, high radical orchidectomy and strict surveillance is the treatment of choice of intratesticular leiomyosarcoma at stage I. However, standard management of stage II or stage III disease is difficult to recommend. | ||||||
|
References
| ||||||
| ||||||
|
[HTML Abstract]
[PDF Full Text]
|
|
Author Contributions
Wissem Hmida – Substantial contributions to conception and design, Acquisition of data, Drafting the article, Revising it critically for important intellectual content, Final approval of the version to be published Faouzi Mallat – Substantial contributions to conception and design, Acquisition of data, Drafting the article, Final approval of the version to be published Mouna Ben Othmen – Substantial contributions to conception and design, Acquisition of data, Drafting the article, Final approval of the version to be published Khaled Ben Ahmed – Substantial contributions to conception and design, Acquisition of data, Drafting the article, Final approval of the version to be published Sidiya Ould Chavey – Substantial contributions to conception and design, Acquisition of data, Drafting the article, Revising it critically for important intellectual content, Final approval of the version to be published Sarra Mestiri – Substantial contributions to conception and design, Acquisition of data, Drafting the article, Final approval of the version to be published Amel Ben Abdallah – Substantial contributions to conception and design, Acquisition of data, Drafting the article, Final approval of the version to be published Faouzi Mosbah – Substantial contributions to conception and design, Acquisition of data, Drafting the article, revising it critically for important intellrctual content, Final approval of the version to be published |
|
Guarantor of submission
The corresponding author is the guarantor of submission. |
|
Source of support
None |
|
Conflict of interest
Authors declare no conflict of interest. |
|
Copyright
© 2014 Wissem Hmida et al. This article is distributed under the terms of Creative Commons Attribution License which permits unrestricted use, distribution and reproduction in any medium provided the original author(s) and original publisher are properly credited. Please see the copyright policy on the journal website for more information. |
|
|
|
About The Authors
| |||
| |||
| |||
| |||
| |||
| |||
| |||
| |||
| |||