|

|
 |
|
Case Report
| ||||||
| Selective arterial embolization in hepatic trauma | ||||||
| Fred John1, Mary Rithu Varkey2 | ||||||
|
1MBBS, R.M.O, Department of Internal Medicine, J.M.M.C & RI, India.
2MBBS, R.M.O, Department of Internal Medicine, S.R.M Hospital, India. | ||||||
| ||||||
|
[HTML Abstract]
[PDF Full Text]
[Print This Article]
[Similar article in Pumed] [Similar article in Google Scholar] 
|
| How to cite this article |
| John F, Varkey MR. Selective arterial embolization in hepatic trauma. Int J Case Rep Images 2014;5(10):712–716. |
|
Abstract
|
|
Introduction:
Blunt abdominal trauma accounts for about (80%) of abdominal injuries seen in the emergency department. The spleen and liver are the most commonly injured solid organs in a blunt abdominal trauma. There has been a change in the trend towards the conservative management of liver injuries with improvement of the imaging techniques. Nowadays non-operative management has been preferred as the treatment of choice in hemodynamically stable cases of liver injuries. Transarterial embolization has been introduced as an effective tool for the management of hemodynamically stable patients with blunt hepatic trauma. This case illustrates the potential benefits of using hepatic artery embolization technique as a treatment modality in patients in whom active surgical intervention was not successful.
Case Report: A 21-year-old male presented to the emergency department with alleged history of fall from a building. On examination the patient was conscious and oriented, hypotensive, tachycardia and generalized abdominal tenderness. Focused assessment with sonography for trauma (FAST) was positive. So an emergency ultrasonography and contrast-enhanced computed tomography (CECT) scan of the abdomen were done which revealed gross hemoperitoneum with liver lacerations. Patient underwent an exploratory laparotomy, the surgeon was not able control the bleeding. So the patient was shifted to cath lab for an emergency hepatic artery embolization with gel foam. Bleeding was controlled with the procedure and he was discharged after two weeks. Conclusion: The non-operative management of blunt hepatic trauma is considered to be the gold standard care for hemodynamically stable patients. Since angiography can offer both diagnostic and therapeutic benefits, angiography should be considered in localizing the site of hemorrhage and in providing an opportunity for the interventional radiologist to proceed to transcatheter embolization of bleeding sites. | |
|
Keywords:
Embolization, Hepatic trauma, Abdominal trauma, Liver
| |
|
Introduction
| ||||||
|
Blunt abdominal trauma accounts for about (80%) of abdominal injuries seen in the emergency department [1]. The spleen and liver are the most commonly injured solid organs in a blunt abdominal trauma [2] [3] [4]. Motor vehicle collision is one of the most common mechanism of injury in an abdominal trauma [5]. The large size of the liver, its position and the friable parenchyma, makes it prone to blunt injury. Right lobe is more often involved in trauma. The management of blunt hepatic trauma remains a topic of debate. The management of blunt abdominal injuries has changed dramatically over the last 25 years [6]. In the past decade, surgical interventions such as arterial ligation, omental packing, liver resection, Pringle manoeuvre, etc. were done in cases of liver injuries, and the mortality was high. Recently, there has been a change in the trend towards conservative management of liver injuries with the advanced imaging techniques. Nowadays non-operative management has been preferred as the treatment of choice in cases of hemodynamically stable patients with blunt hepatic injury. Transarterial embolization has been introduced as an effective tool for the management in hemodynamically stable patients with higher grade injuries or evidence of contrast blush [7]. This case report illustrates a severe blunt hepatic injury successfully managed non-operatively using transarterial embolization. | ||||||
|
Case Report
| ||||||
|
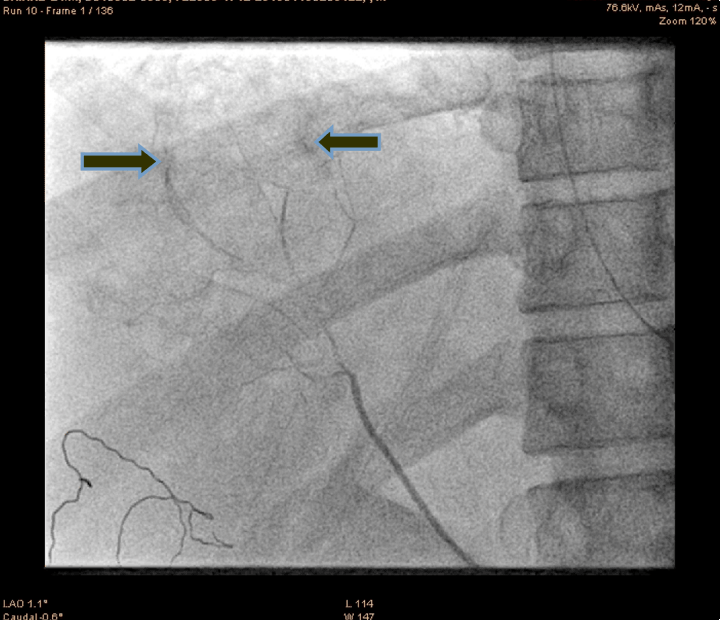
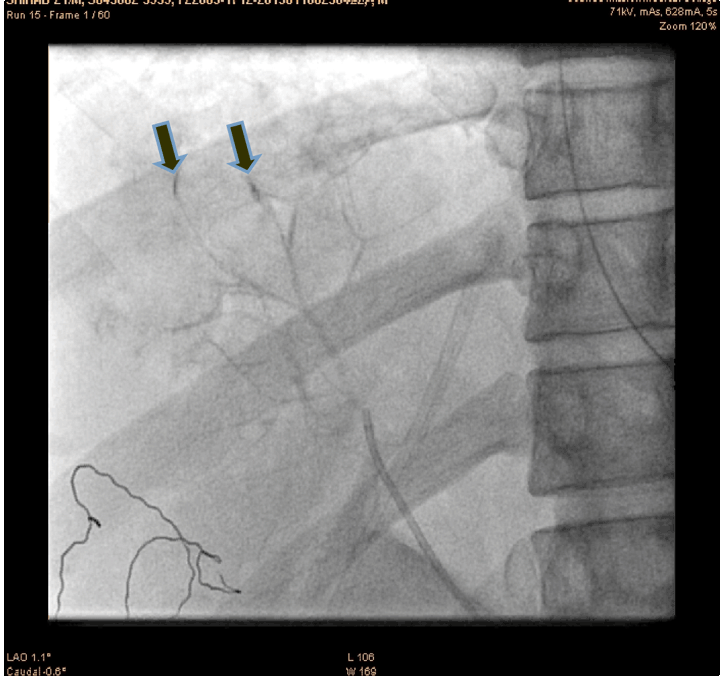
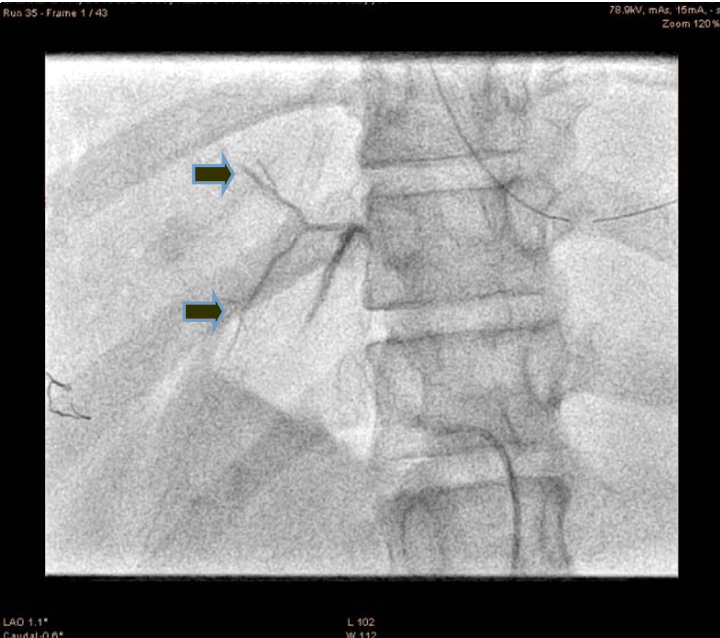
A 21-year-old male presented to the emergency department with alleged history of fall from height of about 10 feet three hours back. The patient was fully conscious and oriented with patent airway and normal breathing and ventilation. On examination, hypotensive (blood pressure 70/50 mmHg), tachycardia (110 bpm) and generalized abdominal tenderness were found. Focused assessment with sonography for trauma (FAST) was positive. So an emergency ultrasonography and contrast-enhanced computed tomography (CECT) scan of the abdomen were done which confirmed significant hemorrhage consistent with a grade III injury by the American Association for the Surgery of Trauma Organ Injury Scale. The patient was resuscitated and shifted to the operation theatre for an exploratory laparotomy, laceration of 4x2 cm with active hemorrhage were noted, the surgeon was not able control the hemorrhage successfully. So the patient was shifted to cath lab. An angiogram of superior mesenteric artery (SMA) showed bleeding from accessory hepatic artery (Figure 1). The diagnostic catheterization of accessory hepatic artery, followed by gel foam infusion to the accessory hepatic artery (Figure 2) and (Figure 3). Figure 4 shows the distal part of accessory hepatic artery occluded. Figure 5 shows occluded right artery following embolization. Repeat arteriography confirmed the occlusion of the vessel. The patient was then transferred to the ICU and transfused one unit of whole blood. He remained hemodynamically stable thereafter, without significant decrease in hematocrit. The patient gradually improved over the next several days and was discharged after two weeks. Follow-up CT scan one month after discharge showed a mild hematoma with no evidence of any infection or complication of the embolization procedure. | ||||||
| ||||||
| ||||||
| ||||||
| ||||||
| ||||||
|
Discussion
| ||||||
|
The most common cause of liver injury is following a blunt abdominal trauma. Over the past few decades most of these cases were treated surgically. Studies have shown that as many as 80% of liver injuries have stopped bleeding by the time surgical exploration is performed [8]. With advanced imaging techniques such as CT scan, have made a great impact on the treatment and marked reduction in the number of patients requiring surgery. Computed tomography scan helps to localize the site and extent of injury. Hepatic artery angiography should be used when CT scan suggests an intrahepatic arterial bleed or high-grade injury in the management of hepatic injuries [9]. Selective arterial embolization of blunt hepatic trauma is considered to be the gold standard care for hemodynamically stable patients with higher grade injuries or the evidence of contrast blush visible in CT scan [10] [11] . It is considered as a conservative management as well as adjunct to surgery in cases of severe injury [12]. A history of blunt trauma of abdomen should always rise a suspicion of liver injury. Most common presentation would be a right upper quadrant tenderness, guarding and rebound abdominal tenderness. Even though there are no specific laboratory tests for hepatic injury. Some studies have been reported that patients with ALT and AST greater than two times normal should be assumed to possess major hepatic trauma [13]. The degree of anemia is based on the volume of blood lost. Earlier diagnostic peritoneal lavage (DPL) were done. Diagnostic peritoneal lavage is non-specific and invasive, time consuming, and oversensitive to presence of blood resulted in higher rate of non-therapeutic laparotomies. The DPL has been replaced by ultrasonography. The focused assessment sonography in trauma (FAST) is non-invasive which can be performed easily. An emergent operative intervention is required in cases of hemodynamically unstable patients and severe grades of injury [14] [15]. Damage control surgery is done for the treatment of major liver injuries with significant survival advantages compared to traditional prolonged surgical techniques. Here perihepatic packing and closure of the abdominal incision is done either using a Bogota bag or partial closure of proximal abdominal incision. Kreig et al. recommend six folded laparotomy pads to be placed between the liver and the abdominal wall to provide a tamponade [16]. The patient is then resuscitated and stabilized and later under goes re-exploration surgery once all metabolic parameters are corrected. The timing of re-exploration depends upon the correction of acidosis, coagulopathy. Usually, 24 hours period for re-exploration surgery. Hepatic embolization appears to be most successful when in hemodynamically stable patients who demonstrate extravasation of contrast on the initial abdominal CT scan. In this procedure, a catheter is introduced into the hepatic artery and a dye is injected which helps to locate the site of hemorrhage and then embolic particles are injected to plug the bleeding vessel. Depending upon the nature of the injury and technical factors Stent graft, embolization coils, microspheres, absorbable gelatin sponge, used to control the hemorrhage. Stent graft can be used only in arteries with a straight course which limits its use in tortous or bifurcating arteries. Embolization can also be done with coils, gel foam, etc. coil embolic works by inducing thrombosis in proximal part of vessels, the disadvantage is that repeat intervention is not possible, once blocked the portion distal to the block cannot be accessed. Gel form is a temporary embolic agent to seal active bleeding quickly and it gets absorbed by body and therefore the vessel recanalize in three weeks. Pitfalls may arise, anatomical variation may occur in visceral vasculature. So one should anticipate aberrant arteries during the procedure. An initial angiogram would help to rule out any anomalies. In some patients, while on embolization may have a temporary vasospasm of the bleeding vessels ceasing the hemorrhage for a while which can misinterpreted by the surgeon and may lead to delayed hemorrhage. Many complications have been reported following non-operative transarterial embolization for liver injuries with bleeding. Fever is commonly seen in about 69% of patients who undergo embolization procedure [17]. Many patients experience a post-embolization syndrome which includes abdominal pain, fever, and ileus. Some cases of cholecystitis, and pancreatitis have also been reported in the embolization of the cystic or gastroduodenal arteries. Others include liver abscess, inadvertent embolization of other organs, contrast nephropathy and allergic reaction to contrast dye. The most dangerous complications of embolization are liver abscess and major hepatic necrosis [18]. Major hepatic necrosis can be managed with a series of operative debridements or with hepatic lobectomy, However, hepatic lobectomy was found to associate with a lower complication rate [19]. | ||||||
|
Conclusion
| ||||||
|
Selective arterial embolization has reduced mortality in cases of hepatic trauma. The non-operative management of blunt hepatic trauma is considered to be the gold standard care for hemodynamically stable patients. Angiography can offer both diagnostic and therapeutic benefits. It should be considered in localizing the site of hemorrhage and in providing an opportunity for the interventional radiologist to proceed to transcatheter embolization of bleeding sites. An emergent operative intervention must be considered in cases of hemodynamically unstable patients and severe grades of hepatic injury. | ||||||
|
References
| ||||||
| ||||||
|
[HTML Abstract]
[PDF Full Text]
|
|
Author Contributions
Fred John – Substantial contributions to conception and design, Acquisition of data, Analysis and interpretation of data, Drafting the article, Revising it critically for important intellectual content, Final approval of the version to be published Mary Rithu Varkey – Acquisition of data, Drafting the article, Revising it critically for important intellectual content, Final approval of the version to be published |
|
Guarantor of submission
The corresponding author is the guarantor of submission. |
|
Source of support
None |
|
Conflict of interest
Authors declare no conflict of interest. |
|
Copyright
© 2014 Fred John et al. This article is distributed under the terms of Creative Commons Attribution License which permits unrestricted use, distribution and reproduction in any medium provided the original author(s) and original publisher are properly credited. Please see the copyright policy on the journal website for more information. |
|
|
|
About The Authors
| |||
| |||
| |||