|

|
 |
|
Case Report
| ||||||
| Adenoid cystic carcinoma of trachea: A rare tumor managed by diode laser and tracheal resection | ||||||
| Navin Bhambhani1, Jayesh Gori2, Vishwanath Masurkar3, Sonal Thombre4 | ||||||
|
1MS, Consultant Surgical Oncologist, Jupiter Hospital, Thane (w), Maharashtra, India.
2MS, (General Surgeon) Registrar, Department of Surgical Oncology, Inlaks and Budhrani Hospital, Pune, Maharashtra, India. 3DNB, (General Surgeon) Assistant Surgeon, Jupiter Hospital, Thane (w), Maharashtra, India. 4BAMS, (Physician Assistant) Physician Assistant, Jupiter Hospital, Thane (w), Maharashtra, India. | ||||||
| ||||||
|
[HTML Abstract]
[PDF Full Text]
[Print This Article]
[Similar article in Pumed] [Similar article in Google Scholar] 
|
| How to cite this article |
| Bhambhani N, Gori J, Masurkar V, Thombre S. Adenoid cystic carcinoma of trachea: A rare tumor managed by diode laser and tracheal resection. Int J Case Rep Images 2014;5(10):680–684. |
|
Abstract
|
|
Introduction:
Adenoid cystic carcinoma (ACC) is a rare type of cancer, which mostly occurs in the salivary glands of the head and neck, and has also been reported in other parts including trachea as case reports or small case series. The patient may present as asthma or acute tracheobronchial obstruction and may require urgent management to relive obstruction. It has a propensity to spread along both submucosal and perineural planes which are responsible for late local recurrence even after complete resection. The best results can be obtained by resection with or without adjuvant radiotherapy.
Case Report: We report a rare case of endoluminal adenoid cystic carcinoma of the distal trachea presenting with acute tracheal obstruction managed bronchoscopically with high power diode laser followed by segmental resection of trachea and radiotherapy with 18 months of follow-up with no evidence of recurrence. Conclusion: There are only very few reports available for the use of diode laser with flexible bronchoscope in tracheobronchial adenoid cystic carcinoma. However, rarity of such tumors makes it impossible to obtain such data. This technique, in such rare tumors, is safe with almost no or limited morbidity from our experience and available data. | |
|
Keywords:
Adenoid cystic carcinoma, Diode laser, Tracheal resection, Bronchoscopy
| |
|
Introduction
| ||||||
|
Adenoid cystic carcinoma (ACC) is a rare type of cancer which mostly occurs in the salivary glands of the head and neck, and has also been reported in the breast, lacrimal gland of the eye, lung, brain, Bartholin's gland, trachea, and the paranasal sinuses as case report or small case series [1]. Adenoid cystic carcinoma of the upper airway is a rare tumor. It is most common in the fifth and sixth decades of life but it can appear at any age [2]. Patients with ACC are usually misdiagnosed and treated as asthma as it has a similar presentation with symptoms of coughing, wheezing and dyspnea [3]. It has a propensity to spread along both submucosal and perineural planes which are responsible for late local recurrence (reported up to 29 years) even after complete resection. The best results can be obtained by resection and adjuvant radiotherapy (assumed to favorably influence survival) [1]. Herein, we report case of ACC initially treated with diode laser fulguration for acute airway obstruction and then completion segmental resection of trachea. | ||||||
|
Case Report
| ||||||
|
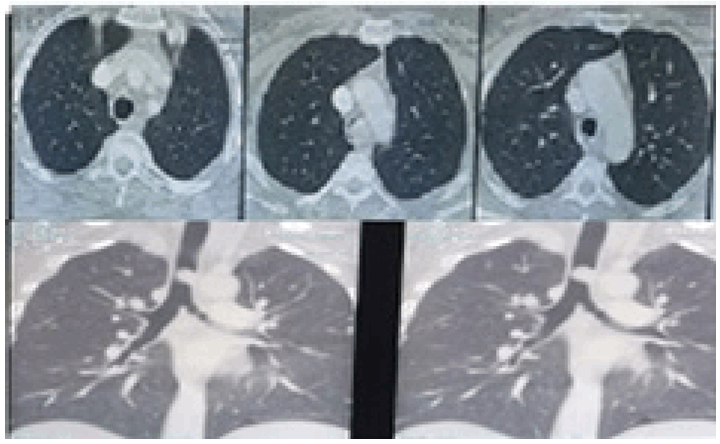
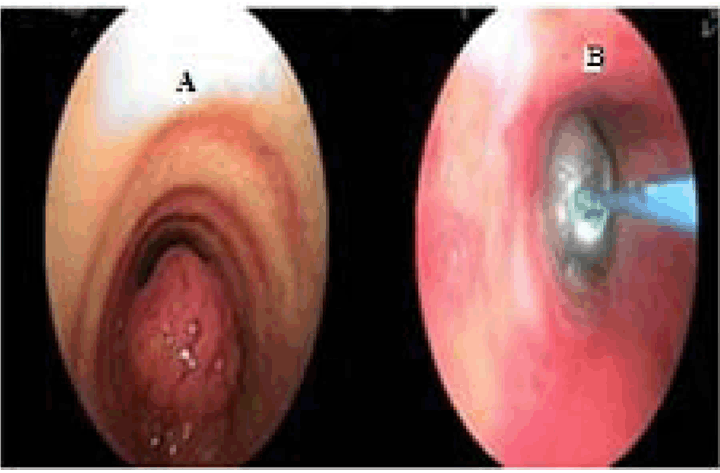
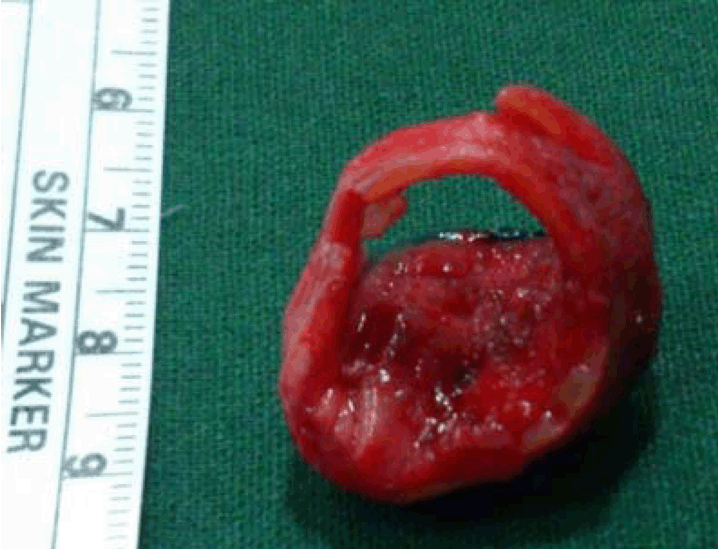
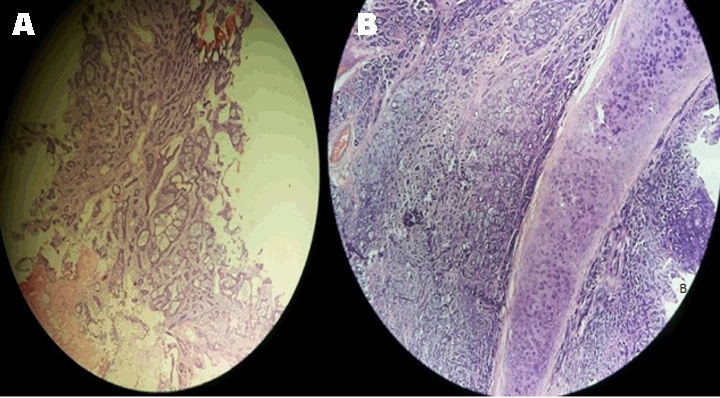
A 45-year-old female, nonsmoker, presented to casualty with tachypnea and tachycardia. She was admitted to the intensive care unit with respiratory acidosis. There was a history of irritant cough with expectoration and breathlessness since 20–25 days. A past history of hyperthyroidism was noted, for which she was on treatment since last six months. After admission, she was diagnosed with diabetes mellitus incidentally. Chest X-ray showed mediastinal widening. Computed tomography (CT) scan suggestive of 2x1.8 cm sized enhancing polypoid lesion arising from the lateral wall of the distal trachea, just proximal to carina, protruding into the lumen, almost obliterating the entire tracheal lumen (Figure 1). Flexible bronchoscopy confirmed the CT findings (Figure 2A). However, the lesion was just negotiable enough to permit visualization of the distal carina, and a preliminary toilet of all accumulated secretions from both left and right endobronchial trees was done. Under conscious sedation, almost near complete fulguration of the tumor was done with using diode laser (GaAIA) after collecting adequate specimen for histopathology (Figure 2B). The luminal obstruction was relieved totally with careful fulguration of the pedicle to avoid intrabronchial hemorrhage. Histopathology reported adenoid cystic carcinoma. Repeat CT virtual bronchoscopy showed residual asymmetric 8 mm thickening and irregularity along the left lateral wall of the trachea, extending over 1.7 cm, approximately 2.1 cm proximal to the carina. A week after optimization, she was taken up for segmental resection of the distal trachea. The approach used was transmediastinal through a median sternotomy. Intraoperative first bronchoscopy was performed to confirm the exact position of residual lesion and length of segment to be resected. Median sternotomy with a collar incision was taken (T-shaped). Trachea was dissected along its entire length anteriorly and posteriorly preserving lateral segmental blood supply, inferiorly up to carina to mobilize the distal trachea to achieve length and tension free resection-anastomosis. Under intraoperative bronchoscopic guidance anterior wall of trachea divided just proximal and distal to lesion (just above carina) and patient ventilated through distal tracheal intubation with a flexometallic endotracheal tube placed through the surgical field. Posterior membranous trachea was divided taking care of esophagus and specimen delivered (Figure 3). After confirming free margins on frozen section, end to end tracheal anastomosis performed using 4.0 PDS, where posterior wall sutures taken continuous; then, from lateral to anterior wall interrupted sutures taken with knots placed outside the tracheal lumen. During this period, oroendotracheal tube is placed distal to anastomosis. No peritracheal leak seen on leak test. Postoperative check bronchoscopy confirmed patency and completeness of suture line. Patient tolerated procedure well, extubated on table and shifted to intensive case unit (ICU) for monitoring. On postoperative day (POD) 1 the patient developed respiratory distress with air bubbling in the mediastinal drain. Check bronchoscopy showed a gape in suture line in posterior wall of trachea along the left lateral aspect over a region of 1–2 stitches. After a multidisciplinary meeting (MDM), it was decided to reintubate the patient to reduce airway pressures and the patient was kept on a T-piece with spontaneous breathing. The bubbling in the drain stopped post-intubation. On POD 3 after a repeat MDM patient extubated. On POD 5 the patient shifted out of ICU with full Ryle's Tube feeds. On POD 7 check bronchoscopy done suggestive of granulation tissue noted over the gaped area. Rest of the suture line was normal. With symptomatic improvement and serial chest X-rays suggestive of reduction in mediastinal widening patient discharged on POD 14. Final histopathology report confirmed adenoid cystic carcinoma of the trachea with negative margins with no lymphovascular emboli or perineural invasion and negative lymph node (Figure 4A-B). Postoperative adjuvant radiotherapy of 56 Gy in 28 fractions for 46 days given to the tumor bed with three-dimensional conformal radiation therapy. She is on six monthly follow-ups with check bronchoscopy and annual CT scan. The patient remains asymptomatic with normal check bronchoscopy (Figure 5) and CT scan at 18th month post-procedure. | ||||||
| ||||||
|
| ||||||
| ||||||
|
| ||||||
| ||||||
|
Discussion
| ||||||
|
Adenoid cystic carcinoma of the trachea is a rare occurrence. Tracheal tumors as a whole account for 0.2% of all respiratory malignancies and only 10% of these cases are adenoid cystic carcinoma [4]. It often shows indolent behavior with a prolonged slow and insidious progression, often over several years, despite propensity of local recurrence and distant metastasis [5]. Treatment options include surgery alone, radiation therapy alone, or a combination. The surgical operations are primary tracheal resection and reconstruction, primary tumor resection, and endoscopic resection, either by coring or using a laser. Only complete surgical resection provides the best chance of prolonged survival or even complete remission. Adjuvant radiotherapy may have some effect on local control but did not affect survival rate [6]. Inoue et al. reported only tracheal resection in nine patients, resection of the trachea plus carina in four patients, tracheal incision and tumor enucleation in one patient of ACC and 11 of 13 patients with adenoid cystic carcinoma were alive without recurrence at last follow-up, and this ranged from 2–9 years [7]. A less extensive surgical resection may also be possible after preoperative bronchoscopic treatment [8]. Laser photocoagulation [Nd:YAG] offered effective treatment in the majority of patients with obstructing tracheobronchial tumors, with acceptable morbidity even for unresectable or unfit patient [9]. Zdenko Tudjman and Vedran Ostojic study of 1244 patients of which 971 were malignant cases of which 53% resected completely and 40% patients resected incompletely with 6% patients were inoperable and remaining benign lesions. They were managed with Nd:YAG and diode laser, and results confirm that laser therapy is highly effective and safe therapeutic method in carefully selected patients, if performed by well-equipped and skilled team of experts. It has been suggested that the Nd:YAG laser is more effective in cases of larger tumor masses and diode laser is more precise with less risk of hemorrhage, perforation and other complications [10]. In our case with use of diode laser, we were able to relieve the acute tracheal obstruction with no complications in conscious sedation and were able to do tracheal resection electively after optimizing the patient with minimal morbidity. | ||||||
|
Conclusion
| ||||||
|
There are only very few reports available for the use of diode laser with flexible bronchoscope in tracheobronchial adenoid cystic carcinoma. However, rarity of such tumors makes it impossible to obtain such data. This technique in such rare tumors is safe with almost no or limited morbidity from our experience and available data. | ||||||
|
References
| ||||||
| ||||||
|
[HTML Abstract]
[PDF Full Text]
|
|
Author Contributions
Navin Bhambhani – Conception and design, Acquisition of data, Analysis and interpretation of data, Critical revision of the article, Final approval of the version to be published Jayesh Gori – Conception and design, Acquisition of data, Analysis and interpretation of data, Drafting the article, Critical revision of the article, Final approval of the version to be published Vishwanath Masurkar – Acquisition of data, Analysis and interpretation of data, Critical revision of the article, Final approval of the version to be published Sonal Thombre – Acquisition of data, Analysis and interpretation of data, Drafting the article, Critical revision of the article, Final approval of the version to be published |
|
Guarantor of submission
The corresponding author is the guarantor of submission. |
|
Source of support
None |
|
Conflict of interest
Authors declare no conflict of interest. |
|
Copyright
© 2014 Navin Bhambhani et al. This article is distributed under the terms of Creative Commons Attribution License which permits unrestricted use, distribution and reproduction in any medium provided the original author(s) and original publisher are properly credited. Please see the copyright policy on the journal website for more information. |
|
|
|
About The Authors
| |||
| |||
| |||
| |||
| |||