|

|
 |
|
Case Report
| ||||||
| Low grade malignant schwannoma of tibial nerve | ||||||
| Horia Orban1, Gabriel Stan2, Boris Feghiu3, Mihaela Dragusanu3, George Simion4 | ||||||
|
1Head of Department, Orthopaedics and Traumatology, Elias Universitary Hospital, Bucharest, Romania.
2Specialist, Surgeon, Orthopaedics and Traumatology, Elias Universitary Hospital, Bucharest, Romania. 3Surgeon, Orthopaedics and Traumatology, Elias Universitary Hospital, Bucharest, Romania. 4Anatomo-pathologist, Emergency Universitary Hospital, Bucharest, Romania. | ||||||
| ||||||
|
[HTML Abstract]
[PDF Full Text]
[Print This Article]
[Similar article in Pumed] [Similar article in Google Scholar] 
|
| How to cite this article |
| Orban H, Stan G, Feghiu B, Dragusanu M, Simion G. Low grade malignant schwannoma of tibial nerve. Int J Case Rep Images 2014;5(10):671–674. |
|
Abstract
|
|
Introduction:
The aim of this paper is to report a rare case of a sizeable low grade malignant schwannoma of the posterior tibial nerve and to underline the method of treatement.
Case Report: A 37-year-old white male presented himself with a slowly growing mass in his left calf. According to the slower rate of growing and to the mobility of the tumor diagnosis was oriented to a benign lesion of posterior calf muscles. The decision was to perform a excisional biopsy of the tumor. The examined tumor was classified as low-grade malignant peripheral nerve sheath tumor. We did not have a suspicion of malignancy in our case due to the slowly growing rate. The treatment performed was surgical excision of the tumor with adequate exposure of normal nerve proximally and distally. Conclusion: Clinical and radiological findings of this case suggested a benign tumor. According to this, the decision was to perform a excisional biopsy of the tumoral mass and not only a biopsy first. | |
|
Keywords:
Malignant schwannoma, Marginal excision, Survival rate, Neurofibromatosis, Tibial nerve
| |
|
Introduction
| ||||||
|
The most common forms of schwannomas are benign. They originate from the sheath of Schwann surrounding peripheral nerve fibers and malignant transformation is uncommon. The patients may have a history of neurofibromatosis type I (NF-1) or tumors may arise spontaneously [1]. Benign peripheral nerve sheath tumor appears as an asymptomatic, slowly growing lesion, while malign lesion is aggressive. Literature studies showed that malignant peripheral nerve sheath tumors are aggressive, presenting as a rapidly growing and painful lump. These tumors are associated with poor prognosis unless wide excision of the tumor is undertaken before local invasion or distant metastasis can occur [2]. Some authors advocated that the operation undertaken, if possible, should be the amputation. Alternatively, where amputation is not possible the alternative must be the largest and most radical excision possible [3]. According to Musculoskeletal Tumor Society, majority of the patients had Stage II (high grade but not metastasized) or Stage III (plus metastasis) tumors. The aim of this paper is to report a rare case of a sizeable low grade malignant schwannoma of the posterior tibial nerve and to underline the methods of treatment. | ||||||
|
Case Report
| ||||||
|
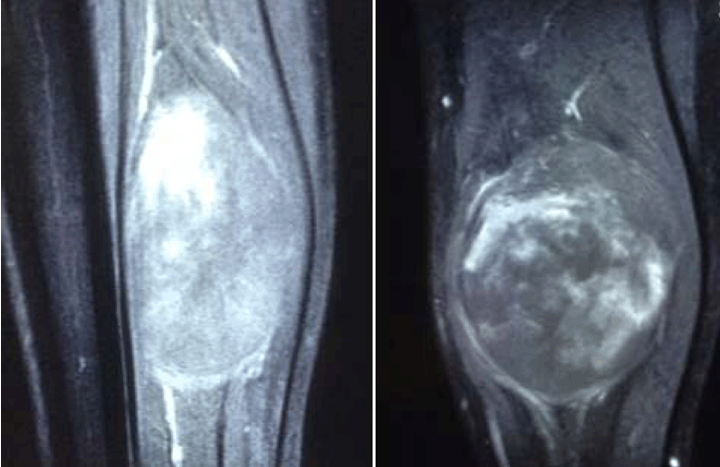
A 37-year-old white male presented himself with a slowly growing mass in his left calf. He was complaining of mild pain and paresthesia of 12 months duration. Loss of sensation in the sole of the foot was observed. On physical examination, a firm painful mass was palpable in the posterior compartment of the left calf. The tumor was relatively mobile in relation to adjacent structures. Also the pain was exacerbate by the motion and prolonged orthostatism. Laboratory testing showed no alteration of erythrocyte sedimentation rate (ESR), C-reactive protein (CRP), fibrinogen or alkaline phosphatase (ALP). The X-ray of lungs was normal. In magnetic resonance imaging (MRI) scan the lesion appeared to be ovalar and multinodular. It measured 90x71x46 mm occurring the distal third of calf posterior compartment. There was a high intensity signal in T2-weighted images and low intensity signal in T1-weighted images (Figure 1). No invasion of the surrounding bones was observed. According to the slower rate of growing and to the mobility of the tumor diagnosis was oriented to a benign lesion of posterior calf muscles. The decision was to perform a excisional biopsy of the tumor. Intraoperatively, we discovered that the tumor had a posterior tibial nerve sheath origin (Figure 2). We performed a marginal excision of this tumor and sent it for anatomopathological examination (Figure 3) and (Figure 4). The examined tumor consists of bundles of irregular spindle cells with moderate cellular density and atypias, mottled appearance, with hyperchromatic nuclei which vary in shape (ellipsoidal, strip-like or comma shape) and the absence of perivascular cluster of cells; predominant architecture closely resembling neurofibroma (1 point). The mitotic rate was low, with 2–4 mitoses/high power field (1 point) and the necrosis was absent (1 point). According to obtained score of 3 points, we classified the tumor as low-grade malignant peripheral nerve sheath tumor (MPNST) (Figure 5) . | ||||||
| ||||||
| ||||||
| ||||||
| ||||||
| ||||||
|
Discussion
| ||||||
|
As we mentioned before, most MPNSTs are high grade. These tumors have a highly aggressive clinical evolution. Ducatman reported in his study of 120 cases that 18% of MPNSTs were low grade. Although no significant correlation has been noted between survival and histological grade, 60% of patients with MPNST die. Survival rates at five and 10 years are 34% and 23%, respectively [4]. The diagnosis of low grade MPNST is not easy due to similarity with neurofibromatosis. Also the pathological features of low grade MPNST often overlap with those of other soft tissue tumors [5]. The diagnosis is particularly difficult when MPNST has multiple mesenchymal differentiations, and should be differentiated from rhabdomyosarcoma, osteosarcoma, chondrosarcoma or liposarcoma [6]. The MPNST with glandular differentiation must be differentiated from metastatic carcinoma. In metastatic carcinoma, spindle-shaped cells around the glandular structures are often reactive proliferating fibroblasts. Full physical examination should be performed for differential diagnosis [7]. The MPNSTs are histologically characterized by hypercellularity, cytological atypia and increased mitotic activity as our study found [8]. Kar et al. in their study showed that grade of the tumor was a significant prognostic factor for survival. Cellular differentiation emerged as a significant prognostic factor for disease free survival in both univariate and multivariate analysis. Mitosis and tumor necrosis had no impact on survival. The index of increasing proliferation was correlated with grade of the tumor and with prognosis of the disease [9]. Other studies also showed that grade of the tumor, necrosis vascular invasion, and presence of mitosis have significant influence on survival [8]. Scheithauer et al. have reported the divergent differentiation as a significant adverse prognostic marker for MPNST [10]. Regarding treatment attitude, Kar et al. performed, among the 15 patients with extremity MPNST, limb salvage surgery in 10 patients, and amputations or disarticulation in five patients, either for primary or recurrent tumor with neurovascular encasement and extensive soft tissue with bone involvement. The five-year overall and disease free survival was 58%. Fifty-four percent of the patients developed relapse of disease, including local, systemic, and second primary sarcomas of same histology (multifocal MPNST). Authors suggested that radical surgical resection is the treatment of choice in MPNST, and that amputations are indicated only when wide excision is not feasible and in patients with severely compromised limb function. The cut end of the nerve should be sent for frozen section to assess the tumor free margin of the resection [9]. Non-conservative surgery is associated with better local control but not with better survival in these patients, as studies previously reported [11]. Matejcik showed that good results were obtained in those patients who did not undergo any attempt for biopsy first, but who received radical excision from the beginning [12]. The only argument for performing a biopsy is suspicion of malignancy [13]. We did not have a suspicion of malignancy in our case due to the slowly growing rate, non-invasive tendency and to the mobility of the tumor. The treatment performed was surgical excision of the tumor with adequate exposure of normal nerve proximally and distally. | ||||||
|
Conclusion
| ||||||
|
This case is a rare low grade malignant schwannoma of the posterior tibial nerve. Clinical and radiological findings of this case suggested a benign tumor. According to this, the decision was to perform a excisional biopsy of the tumoral mass and not only a biopsy first. Despite the malignancy, cellular differentiation and tumoral low grade could be favorable prognostic factors for disease free and overall survival after marginal excision of the tumor. Further follow-up of this case is needed. | ||||||
|
References
| ||||||
| ||||||
|
[HTML Abstract]
[PDF Full Text]
|
|
Author Contributions
Horia Orban – Substantial contributions to conceptions and design, Acquisition of data,Analisys and interpretation of data, Drafting the article, Revising it critically for important intellectual content, Final approval of the version to be published Gabriel Stan – Substantial contributions to conceptions and design, Acquisition of data, Analisys and interpretation of data, Drafting the article, Revising it critically for important intellectual content, Final approval of the version to be published Boris Feghiu – Substantial contributions to conceptions and design, Acquisition of data, Drafting the article, Final approval of the version to be published Mihaela Dragusanu – Substantial contributions to conceptions and design, Acquisition of data, Drafting the article, Final approval of the version to be published George Simion – Substantial contributions to conceptions and design, Acquisition of data, Drafting the article, Final approval of the version to be published |
|
Guarantor of submission
The corresponding author is the guarantor of submission. |
|
Source of support
None |
|
Conflict of interest
Authors declare no conflict of interest. |
|
Copyright
© 2014 Horia Orban et al. This article is distributed under the terms of Creative Commons Attribution License which permits unrestricted use, distribution and reproduction in any medium provided the original author(s) and original publisher are properly credited. Please see the copyright policy on the journal website for more information. |
|
|