|

|
 |
|
Case Report
| ||||||
| Fibrodysplasia ossificans progressiva diagnosed as ankylosing spondylitis: A case report | ||||||
| Sandesh S Thete1, Eknath D Pawar2, Gaurav Bafna3, Purushottam Pawar3 | ||||||
|
1MBBS, MS (Orthopedics), Assistant Professor, Department of Orthopedics, Government Medical College and Hospital, Aurangabad, Maharashtra, India.
2MBBS, MS (Orthopedics), Associate professor and head of Department, Department of Orthopedics, Government Medical College and Hospital, Aurangabad, Maharashtra, India. 3MBBS, MS (Orthopedics) Resident, Department of Orthopedics, Government Medical College and Hospital, Aurangabad, Maharashtra, India. | ||||||
| ||||||
|
[HTML Abstract]
[PDF Full Text]
[Print This Article]
[Similar article in Pumed] [Similar article in Google Scholar] 
|
| How to cite this article: |
| Thete SS, Pawar ED, Bafna G, Pawar P. Fibrodysplasia ossificans progressiva diagnosed as ankylosing spondylitis: A case report. International Journal of Case Reports and Images 2014;5(1):62–65. |
|
Abstract
|
|
Introduction:
Fibrodysplasia (myositis) ossificans progressiva is a rare and very crippling form of disease characterized by great toe malformation and heterotopic bone formation. We herein report a case of fibrodysplasia ossificans progressiva in whom the onset of complaints was after 20 years of age which led physicians to confuse this case with ankylosing spondylitis.
Case Report: A 35-year-old male was referred to us by a physician for operative management of multiple joint deformities secondary to ankylosing spondylitis. However, the history and radiological findings were not consistent with ankylosing spondylitis. Clinical finding of symmetrical valgus malformations of great toes and radiological findings of heterotopic ossifications at multiple sites clinched the diagnosis of fibrodysplasia ossificans progressiva. Plans of surgery were declined after discussion with patient. Conclusion: Fibrodysplasia ossificans progressiva is an exceedingly uncommon genetic disorder. Erroneous diagnoses are very frequent and are commonly associated with apparent iatrogenic harm because of invasive diagnostic or potentially harmful therapeutic interventions. The correct diagnosis of fibrodysplasia ossificans progressiva can be made clinically even before radiographic evidence of heterotopic ossification is seen. | |
|
Keywords:
Fibrodysplasia (myositis) ossificans progressiva (FOP), Ankylosing spondylitis, Heterotopic ossifications, Misdiagnoses
| |
|
Introduction
| ||||||
|
Fibrodysplasia (myositis) ossificans progressiva (FOP) is a rare and very crippling form of disease characterized by great toe malformation and heterotopic bone formation. [1] [2] It has an incidence of one in two million. Usual age of onset of symptoms and presentation is within first decade [1, 2]. We herein report a case of FOP in whom the onset of complaints was after 20 years of age. This wrongly led physicians to confuse this case with ankylosing spondylitis. We review the main clinical features, medical treatments and role of surgical management in FOP. | ||||||
|
Case Report
| ||||||
|
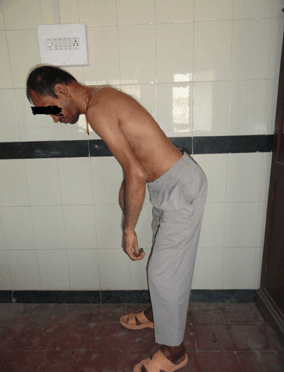
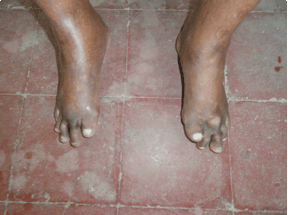
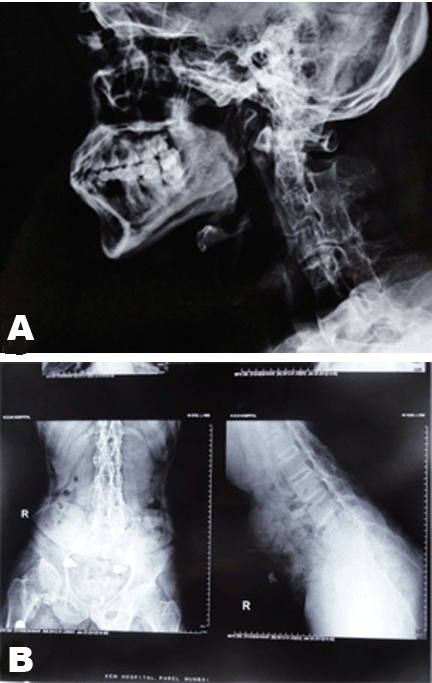
A 35-year-old male was referred to us by a physician for operative management of multiple joint deformities secondary to ankylosing spondylitis. When he first visited the outpatient department of our institute for consultation, one of the authors also made the same diagnosis. His history was suggestive of ankylosing spondylitis as he had gradual onset of pain and slowly progressive morning stiffness in his twenties. He had exaggerations and remissions over years till the disease progressed to its present status. But he never had the classic complain of morning stiffness seen in ankylosing spondylitis. Moreover both his daughters, aged 15 years and 11 years, were having similar complaints which did not fit into picture of ankylosing spondylitis. On examination he walked with the help of crutches with stooped posture. Lumbar lordosis was obliterated with generalized straightening of spinal curvatures but no obvious kyphosis was noted. (Figure 1) A hard swelling was palpable in left adductor group of muscle and several small swellings were palpable in para spinal muscles and around elbow and ankle. No movements were possible in spine while both hips and elbow were fused in flexion. Shoulder and knee joint had preserved functional range of motion. These examination findings and history were not classical of ankylosing spondylitis yet it could not be ruled out. However, the patient had bilateral malformation of both big toes which he said that were present since birth and they were hypoplastic, valgoid and stiff. (Figure 2) (Figure 3) Then the diagnosis of FOP was considered in this patient. On radiological examination with radiographs of lumbar and cervical spine, heterotopic bone formation was noted in paraspinal muscles. (Figure 4A) Disc spaces were normal and no marginal syndesmophytes were noted (Figure 4B). A more pronounced heterotopic mass was seen in left adductor group of muscle. Trabeculations were noted in heterotopic bone suggesting it was mature lamellar bone. Laboratory investigations of the patient were negative for HLA B27 and rest of biochemical markers were within normal limits. Supported with this clinical and investigational data, diagnosis of FOP was made. The patient declined the surgical intervention. | ||||||
| ||||||
| ||||||
| ||||||
| ||||||
|
Discussion
| ||||||
|
Fibrodysplasia ossificans progressiva is an exceedingly uncommon genetic disorder characterized by congenital bilateral malformation of big toe and progressive heterotopic ossification in mesodermal tissues such as muscles, aponeurosis, fascia, tendon and ligaments. [3] Affected individuals are normal at birth except for great toe malformations and average age of presentation is in first decade (range 1–25 years). [2] Kitterman et al. reported 90% of these patients received some wrong or hazardous treatment before proper diagnosis. [4] Misdiagnoses of cancer or fibromatosis, including aggressive juvenile fibromatosis and desmoid tumor, were given to 37% patients. Other misdiagnoses given, in order of frequency, are injuries attributable to trauma or overuse, myositis, rheumatoid arthritis, ankylosing spondylitis, neurofibromatosis and scleroderma. [8] Involvement usually progresses from axial to appendicular and cranial to caudal. [3] They usually present in flare ups following triggering events like trauma, immunizations, influenza like infections or muscle fatigue. Painful swellings appear in skeletal muscles during flare ups which subside in size and become hard as mature bone is formed. Histopathological examination of painful swellings during flare up shows various stages of mature bone formation and mature bone during quiescence. [5] However, invasive investigations, like biopsy, can lead to flare ups and hence avoided. Biochemical markers of bone formation and inflammation are normal, except during flare ups when their values are very high. [6] Radiographs reveal heterotopic bone formation at various sites. [3] Diagnosis is made clinically based on the findings of congenital symmetrical malformation of big toe and progressiva heterotopic bone formation. The genetic basis is traced to a recurrent heterozygous missense point mutation on chromosome 2q.23-24 region. It causes abnormality in ACVR1/ALK2 receptors in BMP signaling pathway. [7] This causes profound dysregulation of BMP signaling pathway, particularly over expression of BMP4, leading to uncontrolled heterotopic enchondral ossifications. [5] [8] Both sporadic and familial case have been reported with 90% of cases are new mutations and 10% familial cases with autosomal dominant mode of transmission. Average life expectancy of these individuals is 40 years with cause of death in most cases being thoracic insufficiency syndrome due to chest wall immobility [9]. To the date of writing this article no single effective treatment has been agreed upon and controversies continue. Generally, management needs a well-structured and individualized approach focusing on the following: [10]
Various drug classes can be used for management like steroids, NSAIDs, mast cell stabilizers, chemotherapy agents, radiotherapy, bone marrow transplantation are few to mention [10]. Definitive target for therapy is gene therapy with noggin, a BMP4 antagonist in BMP signaling pathway. Surgery is usually deferred in these individuals because risks, which start from anesthesia to flare ups away from operative site postoperatively, outweigh the benefits of any operative intervention. Hence adventurous interventions like surgery should be undertaken in clear indications and after thorough discussion with affected individuals and their relatives. [4] This case reinforces the importance of thorough history and clinical examination aiding in diagnosis, avoiding unnecessary investigations and potentially harmful interventions. | ||||||
|
Conclusion
| ||||||
|
Fibrodysplasia ossificans progressiva (FOP) is an exceedingly uncommon genetic disorder. Erroneous diagnoses are very frequent and are commonly associated with apparent iatrogenic harm to individuals affected with FOP. The correct diagnosis of fibrodysplasia ossificans progressiva can be made clinically even before radiographic evidence of heterotopic ossification is seen. Errors in diagnosis can lead to invasive diagnostic procedures (surgical or needle biopsies) or unnecessary therapeutic interventions (surgery, chemotherapy, or physical therapy) which can result in permanent disability, which can be avoided with correct diagnosis. | ||||||
|
References
| ||||||
| ||||||
|
[HTML Abstract]
[PDF Full Text]
|
|
Author Contributions
Sandesh S Thete – Substantial contributions to conception and design, Acquisition of data, Analysis and interpretation of data, Drafting the article, Revising it critically for important intellectual content, Final approval of the version to be published Eknath D Pawar – Acquisition of data, Drafting the article, Revising it critically for important intellectual content, Final approval of the version to be published Gaurav Bafna – cquisition of data, Drafting the article, Revising it critically for important intellectual content, Final approval of the version to be published PurushottamPawar – cquisition of data, Drafting the article, Revising it critically for important intellectual content, Final approval of the version to be published |
|
Guarantor of submission
The corresponding author is the guarantor of submission. |
|
Source of support
None |
|
Conflict of interest
Authors declare no conflict of interest. |
|
Copyright
© Sandesh S Thete et al. 2014; This article is distributed the terms of Creative Commons Attribution License which permits unrestricted use, distribution and reproduction in any means provided the original authors and original publisher are properly credited. (Please see Copyright Policy for more information.) |
|
|