|

|
 |
|
Case Report
| ||||||
| Primary posterior mediastinal hydatid cyst mimicking malignant mediastinal neurogenic tumor | ||||||
| Aram Baram1, Fahmi H Kakamad2, Ali A Alwan3 | ||||||
|
1MD, MRCS, FACS, University of Sulaimani /Faculty of Medical Sciences, School of Medicine/Department of Thoracic and Cardiovascular Surgery, François Mitterrand Street, Sulaymaniyah, IRAQ.
2MD, University of Sulaimani/Faculty of Medical Sciences, School of Medicine/Department of Thoracic and Cardiovascular Surgery/ François Mitterrand Street, Sulaymaniyah, IRAQ. 3MD, FICMS, University of Sulaimani/Faculty of Medical Sciences, School of Medicine/Department of Orthopedics and Trauma/François Mitterrand Street, Sulaymaniyah, IRAQ. | ||||||
| ||||||
|
[HTML Abstract]
[PDF Full Text]
[Print This Article]
[Similar article in Pumed] [Similar article in Google Scholar] 
|
| How to cite this article |
| Baram A, Kakamad FH, Alwan AA. Primary posterior mediastinal hydatid cyst mimicking malignant mediastinal neurogenic tumor. International Journal of Case Reports and Images 2014;5(1):54–57. |
|
Abstract
|
|
Introduction:
Hydatid disease is caused by Echinococcus granulosus parasite. It is an endemic disease; particularly in many Mediterranean countries. Bone involvement is reported in 1–2% of the cases and about 50% of those are seen in the spine. Herein we report a case of primary spinal extradural hydatid cyst that caused paraplegia due to compression of the dorsal spinal cord and was diagnosed initially as case of lumbar prolapsed intervertebral disc.
Case Report: A 40-year-old female referred to us suffering from painful spastic weakness of lower limbs, her condition started six months earlier to admission and she became paraplegic for last four months with loss of bladder and bowel control. She had L4, L5 lumbar laminectomy four months earlier as she was diagnosed as lumbar prolapsed intervertebral disc. After a thorough diagnostic workup, it was provisionally found that she has a malignant posterior mediastinal mass, but surprisingly only intraoperatively we discovered that she had only a posterior mediastinal hydatid cyst, which had been treated accordingly. Conclusion: Hydatid cyst may speculate all types of thoracic tumors so high index of suspension should be considered in treating thoracic tumors in an endemic area. | |
|
Keywords:
Mediastinal hydatid cyst, Neurogenic tumor, Paraplegia
| |
|
Introduction
| ||||||
|
Hydatid disease is caused by Echinococcus granulosus parasite. It is an endemic disease; particularly in many Mediterranean countries. The liver and the lungs are most frequently involved. [1] Bone involvement is reported in 1–2% of the cases and about 50% of those are seen in the spine. [2] The first hydatid disease in spine was reported in 1807 by Chaussier [3]. Its clinical characteristics, diagnosis and therapy are still not definitive. [3] Spinal hydatid disease manifests itself through symptoms and signs related to compression of the cysts on other structures it has no specific pathognomonic symptoms or signs. The disease presents with radiculopathy, myelopathy and/or localized pain and tenderness owing to destructive bone lesions, pathological fracture and consequent cord compression. [4] X-ray appearance and computed tomography (CT) scan findings of spinal echinococcosis are non-specific and sometime misleading. Magnetic resonance imaging (MRI) is very sensitive diagnostic tool for hydatid cyst of spine. [3] | ||||||
|
Case Report
| ||||||
|
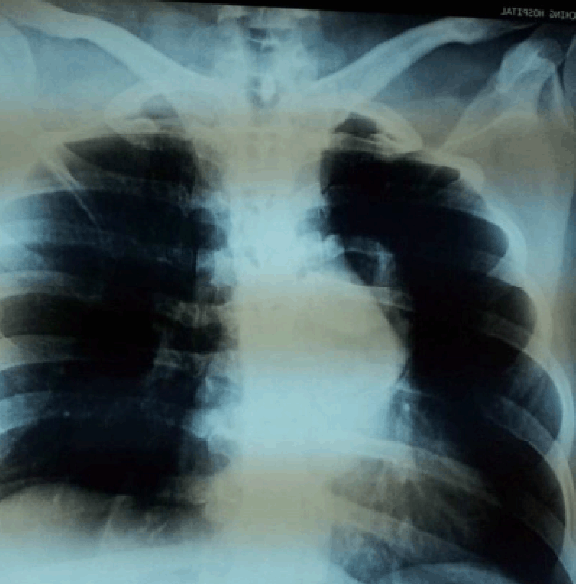
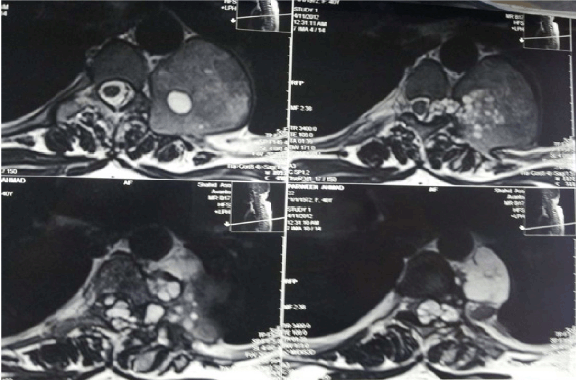
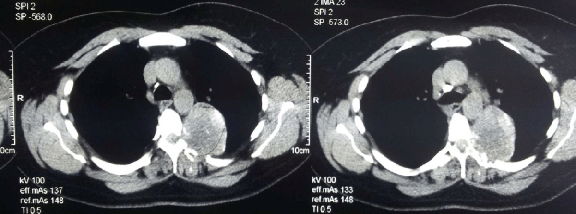
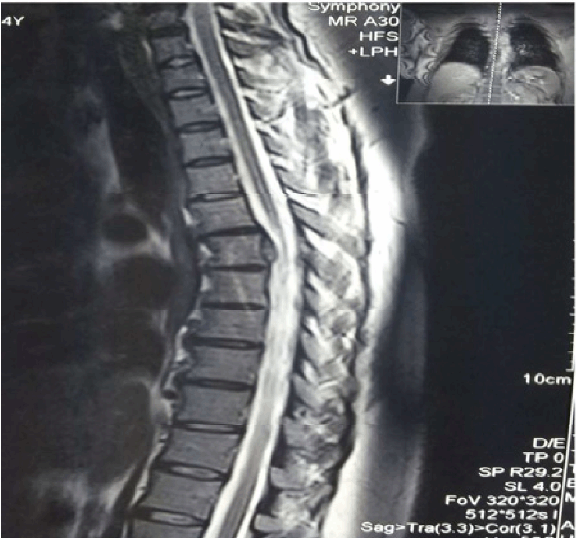
A 40-year-old female referred to us suffering from painful spastic weakness of lower limbs, her condition started six months earlier to admission and she became paraplegic for last four months with loss of bladder and bowel control. She had L4, L5 lumbar laminectomy four months earlier as she was diagnosed as lumbar prolapsed intervertebral disc. Physical examination revealed bilateral lower limb weakness; power grade was zero, sensory loss from the level of D10, absence of all lower limb reflexes, distal pulses were positive. Per-rectal examination showed decreased anal tone. Chest X-ray showed left hilar shadow, (Figure 1) CT scan revealed posterior mediastinal dumbbell tumor extended to the spinal canal at the level of D5, with destruction of left transverse process, pedicle, and fifth rib, (Figure 2) MRI scan showed posterior mediastinal cystic lesion, (Figure 3) Through mini-thoracotomy incision, exploration of the pleural cavity was done, cystic lesion was found in the left para- vertebral gutter with features of hydatid cyst, after isolation by Povidone-iodine soaked packs aspiration of the cyst was done which revealed caseating material and large number of small daughter cysts. Intraoperative orthopedic surgeon performed decompression of the canal anteriorly with partial anterolateral corpectomy. Histopathological examination of the specimen confirmed hydatidosis. She was treated by 800 mg Albendazole daily and program of physiotherapy. Full power movements appeared in four months post-operatively and her last MRI showed normal dorsal spinal cord with partial distortion of the body of D8-9. (Figure 4) | ||||||
| ||||||
| ||||||
| ||||||
| ||||||
|
Discussion
| ||||||
|
Vertebral hydatidosis is a silent, slowly progressive disease. Pain is an important presenting symptom. Neurological disorders occur after a latent period of several years. [6] [7] The diagnosis is considered if the patient lives in a geographic region where the infestation is known to occur. [7] Our case did not show any sign of chest involvement clinically and posterior mediastinal mass was an accidental finding on chest radiography during diagnostic workup for her paraplegia. In bone tissue the larva behaves differently from soft tissue. It grows in direction of least resistance, infiltrating and damaging the bone like a tumor by exogenous vesiculation, then enlarged by endogenous vesiculation resulting in formation of daughter cyst. [8] Braithwaite and Lees classified the spinal hydatid as follows: [9]
The first three groups of hydatidosis are rare, and only sporadic cases have been reported [9]. We can classify our case as type (III) who recovered from paraplegia and to our knowledge only a few cases have been reported to regain full power [4, 6, 8]. Spinal involvement is believed to occur through vertebral–portal venous anastomosis or might be caused by encroaching pulmonary lesions. Rarely the disease begins from the extradural region. [9] Most spinal hydatid cysts are thoracic (52%), lumbar (37%) and then the cervical and sacral levels. [4] The surgical treatment consists of removal of cyst contents without contamination followed by appropriate management of any remaining cavity. The surgical area might be irrigated with chemical agents in an attempt to kill scoleces. [7] Indications for chemotherapy include inoperable lesions unless it is not a harmful lesion, unwillingness of the patient to undergo surgery, and use as an adjunct to surgery. The combination of chemotherapy and surgical treatment has been found to be more efficient than surgical treatment alone. [9] Albendazole has been found to be better absorbed than Mebendazole and exhibits superior efficacy against helminthes. [7] | ||||||
|
Conclusion
| ||||||
|
lthough extremely rare, intraspinal extradural thoracic hydatid cyst might be a reversible cause of paraplegia, sphincter dysfunction and sensory loss. Surgical decompression is the treatment of choice followed by postoperative chemotherapy and program of physiotherapy. Hydatid cyst may speculate all types of thoracic tumors so high index of suspension should be considered in treating thoracic tumors in an endemic area. | ||||||
|
References
| ||||||
| ||||||
|
[HTML Abstract]
[PDF Full Text]
|
|
Author Contributions
Aram Baram – Substantial contributions to conception and design, Acquisition of data, Analysis and interpretation of data, Drafting the article, Revising it critically for important intellectual content, Final approval of the version to be published Fahmi H Kakamad – Acquisition of data, Drafting the article, Revising it critically for important intellectual content, Final approval of the version to be published Ali A Alwan – Acquisition of data, Drafting the article, Revising it critically for important intellectual content, Final approval of the version to be published |
|
Guarantor of submission
The corresponding author is the guarantor of submission. |
|
Source of support
None |
|
Conflict of interest
Authors declare no conflict of interest. |
|
Copyright
© Aram Baram et al. 2014; This article is distributed the terms of Creative Commons Attribution License which permits unrestricted use, distribution and reproduction in any means provided the original authors and original publisher are properly credited. (Please see Copyright Policy for more information.) |
|
|