|

|
 |
|
Case Report
| ||||||
| A variant common hepatic artery originating from the normal celiac trunk and passing behind the portal vein successfully treated with pancreaticoduodenectomy for middle bile duct cancer: A case Report | ||||||
| Yoshihito Ohta1, Michiki Narushima1, Adoru Okaue1, Hisashi Nakata2, Hisahiro Matsubara3 | ||||||
|
1Department of Surgery Shimizu Kousei Hospital, Shimizu-ku, Shizuoka, Japan.
2Department Internal Medicine, Shimizu Kousei Hospital, Shimizu-ku, Shizuoka, Japan. 3Department of Frontier Surgery, Graduate School of Medicine, Chiba University, Chuo-ku, Chiba, Japan. | ||||||
| ||||||
|
[HTML Abstract]
[PDF Full Text]
[Print This Article]
[Similar article in Pumed] [Similar article in Google Scholar] 
|
| How to cite this article: |
| Ohta Y, Narushima M, Okaue A, Nakata H, Matsubara H. A variant common hepatic artery originating from the normal celiac trunk and passing behind the portal vein successfully treated with pancreaticoduodenectomy for middle bile duct cancer: A case Report. International Journal of Case Reports and Images 2013;4(10):536–540. |
|
Abstract
|
|
Introduction:
Pancreaticoduodenectomy (PD) consists of multiple complex surgical procedures, including skeletonization of the hepatic artery for lymph node dissection. Variations in the hepatic artery can be observed in 25–45% of cases, so it is important for surgeons to have knowledge of the hepatic blood supply to avoid injury that may result in biliary fistula or hepatic ischemia after surgery.
Case Report: We encountered a 67-year-old male patient with a variant common hepatic artery which originated from the normal celiac trunk and passed behind the portal vein. This patient successfully underwent a subtotal-stomach-preserving PD for middle bile duct cancer. The frequency of this variant common hepatic artery is approximately 0.1%; according to two large-scale retrospective studies on the variations of the hepatic blood supply. Unlike the different branches or number variations, it is difficult to identify the course variations with conventional visceral angiography or three-dimensional computed tomography arteriography (CTA) (3D-CT angiography image in arterial phase). The variant course of the common hepatic artery in this patient was preoperatively identified by fused images from 3D-CTA and venography. Conclusion: Fusing images from 3D- CTA and venography should be recommended as part of the routine preoperative examination for depicting anatomical variations, such as in the variant course of the common hepatic artery in the patients planning to undergo PD. | |
|
Keywords:
Variant common hepatic artery, Pancreaticoduodenectomy, Bile duct cancer
| |
|
Introduction
| ||||||
|
Pancreaticoduodenectomy (PD) requires complex surgical procedures associated with high morbidity and even the risk of mortality. [1] [2] [3] [4] [5] [6] [7] [8] [9] Variant arterial anatomy in patients undergoing PD increases the risk of injury of the hepatic blood supply which may result in biliary fistula or hepatic ischemia after surgery.[1] [7] [8] [9] Meanwhile anatomical variations of the hepatic artery are not uncommon, which can be observed in 25–45% of the cases. [5] [6] [7] [8] [9] Therefore, it is extremely important to identify these anomalous vessels prior to surgery when planning therapeutic strategies for PD. Visceral angiography or three-dimensional computed tomography (CT) arteriography (the arterial phase of 3D-CT angiography) is usually performed as a routine diagnostic procedure. However, it is difficult to identify the course variations with these examinations. We encountered a patient with a variant common hepatic artery (CHA) originating from the normal celiac trunk and passing behind the portal vein suffering from middle bile duct cancer. According to two large-scale retrospective studies concerning the variations of the hepatic blood supply, this course variation of the CHA is very rare, approximately 0.1% of the cases. [10] [11] We identified this rare variation by fusing images from 3D- CT arteriography and venography (the venous phase of 3D-CT angiography) before performing PD and therefore were able to safely deal with this variant CHA at surgery. | ||||||
|
Case Report
| ||||||
|
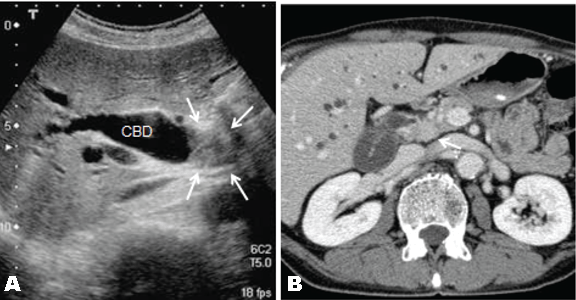
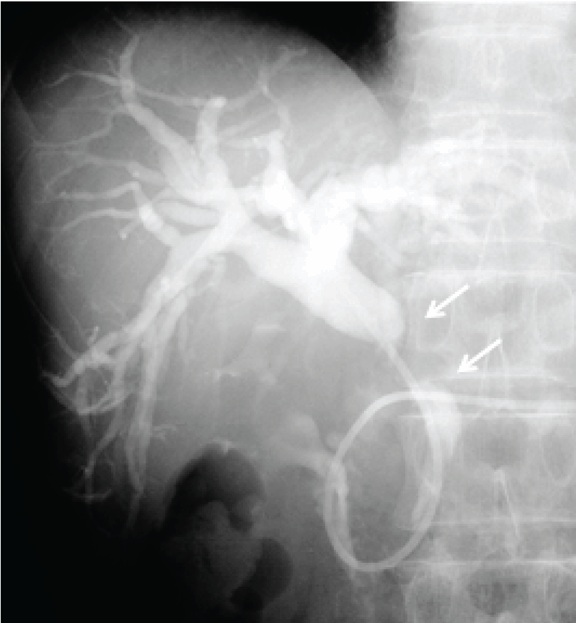
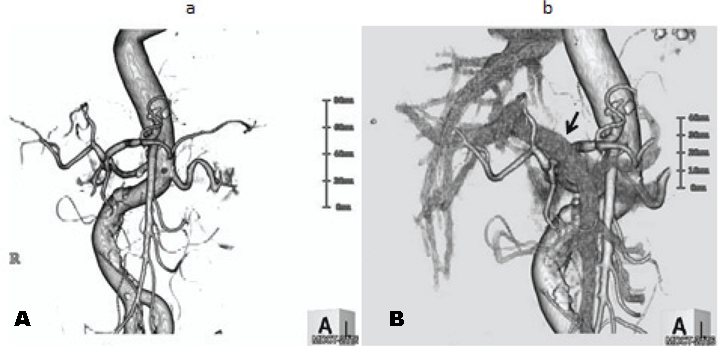
A 67-year-old male patient was referred to our hospital to investigate a case of jaundice on October 2010. He denied anorexia, abdominal pain, alcohol abuse and cigarette smoking. Physical examination revealed a mildly cachectic and icteric male with no acute distress. An abdominal examination revealed no palpable abdominal masses, organomegaly or evidence of ascites. He denied abdominal tenderness. On admission his total bilirubin level 7.52 mg/dL, alkaline phosphatase 1032 IU/L (normal range 105–320 IU/L), carcinoembryonic antigen 11.8 ng/dL (range, 0.0–5.0 ng/dL), carbohydrate antigen 19–9 was 765.1 Um/L (normal range 0.0-37.0 U/mL). Ultrasonography and contrast-enhanced computed tomography (CT) of the abdomen revealed a mass, approximately 2 cm in diameter, in the middle of the common bile duct (CBD), which caused the dilatation of the proximal biliary tract. (Figure 1A–B) Endoscopic retrograde naso-biliary drainage was successfully performed to improve the jaundice. Cholangiography and magnetic resonance cholangiopancreatography revealed a 2.5-cm filling defect in the middle of the CBD. (Figure 2) Based on these findings, the patient was diagnosed with middle bile duct cancer and a subtotal-stomach-preserving PD was planned. A 3D-CT angiography was performed prior to the PD procedure in order to identify the anatomy of the hepatic blood supply. The 3D-CT arteriography showed a normal trifurcation of the celiac trunk, CHA, left gastric artery and splenic artery. (Figure 3A) However, fused images from the 3D-CT arteriography and venography showed an unusual trajectory of the CHA, passing behind the portal vein, immediately running towards the ventral side between portal vein and CBD, and ascending to the hepatic hilum in front of the portal vein after giving off the gastroduodenal artery (Figure 3B). During surgery, we easily identified and safely dealt with the variant CHA and completed the complicated procedure including the skeletonization of this artery for lymph node dissection without any vascular injury. Pathological findings showed moderately differentiated tubular adenocarcinoma, T2, N1, M0, Stage IIB in terms of the UICC TNM classification. The patient had an uneventful postoperative course except for a grade B pancreatic fistula which was treated by percutaneous abdominal puncture. The patient was discharged on postoperative day-24 and remained disease-free for 16 months. | ||||||
|
| ||||||
| ||||||
|
| ||||||
|
Discussion
| ||||||
|
Pancreaticoduodenectomy requires complex surgical procedures associated with high morbidity and even the risk of mortality [1–9]. Variant arterial anatomy in patients undergoing PD increases the risk of injury of the hepatic blood supply which may result in the inadvertent bleeding, biliary fistula or hepatic ischemia after surgery. [1] [7] [8] [9] Traverso et al. [1] reported that accidental ligation of the replaced CHA can lead to ischemia of the bilioenteric anastomosis and a consequent leak. Biehl et al. [7] and Kim et al. [8] demonstrated poor clinical outcomes after PD in patients with variant vascular anatomy and recommended angiography in all patients preparing to undergo PD. After analyzing studies which compared imaging modalities, Shukla et al.[9] concluded that routine preoperative CT angiography for PD helps to identify the hepatic vascular anatomy and thereby prepares the surgeon to better deal with the vascular anomalies intraoperatively. [10] [11] [12] As mentioned above, the anatomical variations of the hepatic blood supply are not rare, which can be observed in 25–45% of the cases. [13] [14] [15] [16] [17] Variant left or right hepatic arteries are common anatomical variations of the hepatic blood supply. Common hepatic artery divided from the superior mesenteric artery can be observed in 1.5–4.5% of the cases. [13] [14] [15] [16] [17] An international classification of the variations in the vascular anatomy of the liver was proposed by Michels [13] in 1966 and modified by Hiatt et al. [14] in 1994. Additionally, anatomic, surgical and radiological studies have described other rare hepatic arterial variations. [16] [17] [18] [19] We encountered a male patient with a variant CHA originating from the normal celiac trunk and passing behind the portal vein who underwent PD for middle bile duct cancer. This variant course of the CHA has seldomly been previously identified or reported. After studying 932 dissections of the hepatic artery in liver transplantation, Abdullah et al. [18] identified one case with the same variant CHA. Based on the retrospective evaluation of the findings in 5002 patients who underwent spiral CT and digital subtraction angiography, Song et al. [19] found six CHAs which had a suprapancreatic retroportal course. To the best of our knowledge, this is the first case reported of a patient with this CHA variation who successfully underwent PD. It may be difficult to identify the course variations with conventional visceral angiography or 3D-CT arteriography, because these examinations cannot delineate the dimensional relationship between CHA and portal vein separately by themselves. In our case, fused images of 3D-CT arteriography and venography clearly showed the abnormal course of the CHA which passed behind the portal vein, although CT arteriography by itself showed a normal configuration of the CHA. | ||||||
|
Conclusion
| ||||||
|
We herein presented a patient with a variant common hepatic artery originating from the celiac artery and passing behind the portal vein which we identified by fusing images from three-dimensional computed tomography arteriography and venography prior to performing pancreaticoduodenectomy for middle bile duct cancer. Fused images from three-dimensional computed tomography arteriography and venography should be recommended as one of routine preoperative examinations for depiction of anatomical variations including the variant course of the common hepatic artery in patients planning to undergo pancreaticoduodenectomy. | ||||||
|
References
| ||||||
| ||||||
|
[HTML Abstract]
[PDF Full Text]
|
|
Author Contributions
Yoshihito Ohta – Substantial contributions to conception and design, Acquisition of data, Analysis and interpretation of data, Drafting the article, Revising it critically for important intellectual content , Final approval of the version to be published Michiki Narushima– Acquisition of data, Analysis and interpretation of data, Drafting the article, Revising it critically for important intellectual content, Final approval of the version to be published Adoru Okaue – Acquisition of data, Analysis and interpretation of data, Drafting the article, Revising it critically for important intellectual content, Final approval of the version to be published Hisashi Nakata – Acquisition of data, Analysis and interpretation of data, Drafting the article, Revising it critically for important intellectual content, Final approval of the version to be published Hisahiro Matsubara – Substantial contributions to conception and design, Analysis and interpretation of data, Drafting the article, Revising it critically for important intellectual content, Final approval of the version to be published |
|
Guarantor of submission
The corresponding author is the guarantor of submission. |
|
Source of support
None |
|
Conflict of interest
Authors declare no conflict of interest. |
|
Copyright
© Yoshihito Ohta et al. 2012; This article is distributed the terms of Creative Commons Attribution License which permits unrestricted use, distribution and reproduction in any means provided the original authors and original publisher are properly credited. (Please see Copyright Policy for more information.) |
|
|