|

|
 |
|
Case Report
| ||||||
| Peritoneal encapsulation, left paraduodenal hernia with retroperitonealization of inferior mesenteric vein leading to triple obstruction | ||||||
| Imtiaz Wani1, Khursheed A Wani1, Muneer Wani1, Gulzar Bhat1, Mubashir Shah1 | ||||||
|
1Department of General Surgery, SKIMS, Srinagar, Kashmir, India.
| ||||||
| ||||||
|
[HTML Abstract]
[PDF Full Text]
[Print This Article]
[Similar article in Pumed] [Similar article in Google Scholar] 
|
| How to cite this article: |
| Wani I, Wani KA, Wani M, Bhat G, Shah M. Peritoneal encapsulation, left paraduodenal hernia with retroperitonealization of inferior mesenteric vein leading to triple obstruction. International Journal of Case Reports and Images 2013;4(3):169–174. |
|
Abstract
|
|
Introduction:
Encasing of small bowel in an anomalous accessory membrane results in peritoneal encapsulation and is a very rare cause of intestinal obstruction. It is believed to be caused by malrotation of the bowel during the 12th week of gestation and this causes the formation of an accessory sac from the peritoneum, covering the umbilicus. Left paraduodenal hernia is the most common form of congenital internal hernia. Paraduodenal hernia are caused by abnormal rotation of the midgut during embryonic development. This rarely presents as an intestinal obstruction. Congenital adhesions are rare in adults and these may lead to retroperitonealization of inferior mesenteric vein.
Case Report: A case of peritoneal encapsulation and left paraduodenal hernia with congenital adhesions leading to retroperitonealization of inferior mesenteric vein in the same patient is reported here. A 28-year-old male presented with recurrent small bowel obstruction and was diagnosed with an intestinal obstruction. Computed tomography confirmed peritoneal encapsulation and left paraduodenal hernia with features of intestinal obstruction. Excision of membrane and reduction of hernia with retroperitonealization of inferior mesenteric vein was done. Conclusion: This is the first case reported in literature where peritoneal encapsulation, paraduodenal hernia and retroperitonealization of inferior mesenteric vein occurred together and lead to bowel obstruction. In this case, the origin of three abnormal anatomical structures must have been congenital as there was no history of prior surgery. | |
|
Keywords:
Encapsulation, Paraduodenal, Inferior mesenteric vein (IMV)
| |
|
Introduction
| ||||||
|
The peritoneal encapsulation, first described by Cleland [1] in 1868, is a rare developmental abnormality in which part or the entire small bowel is encased in an accessory sac. It is believed to be caused by malrotation of the bowel during the 12th week of gestation and this causes the formation of an accessory sac from the peritoneum covering the umbilicus. [2] The incidence of this condition is not well known. There are not more than 50 to 60 cases described in literature. [3] [4] [5] Most of the cases remain asymptomatic; diagnosed usually as an incidental finding during surgery for unrelated conditions and only rarely present as bowel obstruction. [6] [7] [8] Paraduodenal hernia is the most common type of intestinal hernia, accounting for 30–53% of all cases and accounts for 0.2–0.9% of all bowel obstructions. [9] This hernia has a variable clinical manifestation and rarely may present as an acute abdomen. In adults, occurrence of congenital bands is an extremely rare condition. [10] [11] The entrapment of the intestine between the bands and the mesentery or by compression of the bowel leads to obstruction. Rarely a vessel with an abnormal position compressing on the gut could lead to bowel obstruction. [3] Clinical diagnosis of bowel obstruction is often difficult to make due to ambiguous presentation in peritoneal encapsulation, paraduodenal hernia, congenital bands and an abnormal vessel compressing the gut. [12] [13] [14] X-ray of abdomen, ultrasonography, barium study and computed tomography are contributory in diagnosis of each form of obstruction. The excision of membrane in peritoneal encapsulation is recommended even if this condition is diagnosed incidentally. All paraduodenal hernias must be repaired, including those that are asymptomatic. [15] Release of adhesions in congenital bands and the retroperitonealization of vessel leading to obstruction is recommended. | ||||||
|
Case Report
| ||||||
|
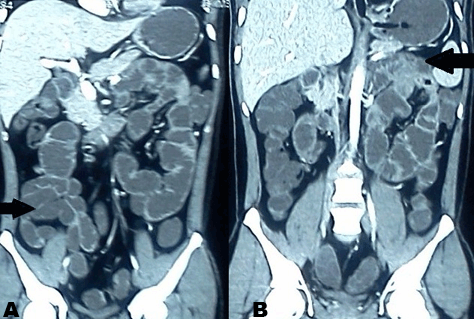
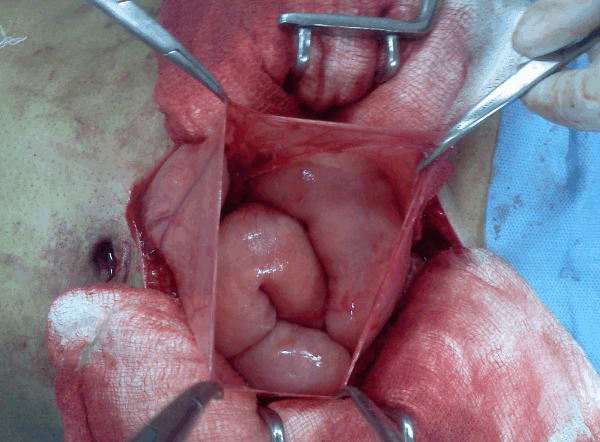
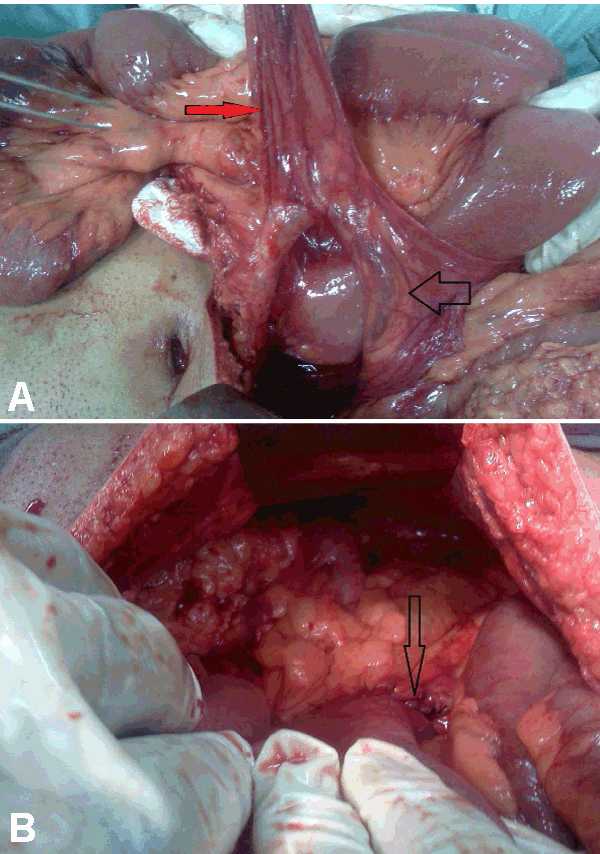
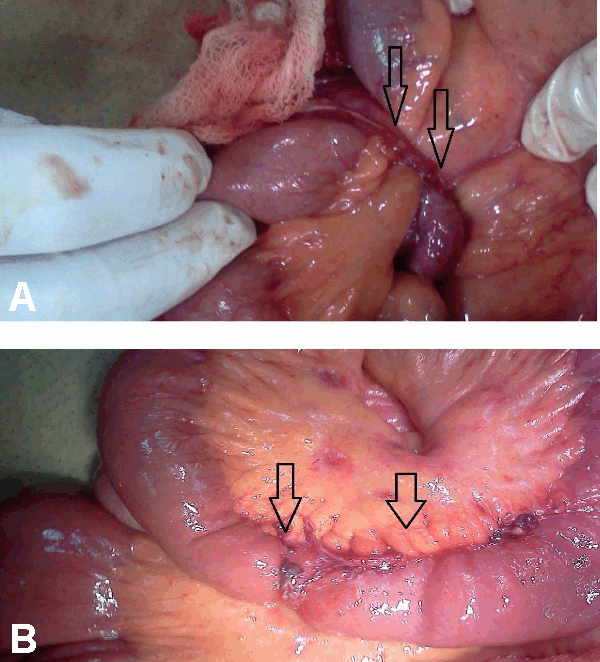
A 28-year-old male presented with generalized abdominal pain, fever and multiple episodes of vomiting. Abdominal pain was episodic and colicky and vomitus was bilious. There was no past history of trauma or surgery. Patient had a past history of three episodes of similar abdominal pain and vomiting three months back. Second episode occurred 12 days after the first episode and third episode occurred 21 days after first episode. Patient was diagnosed as a case of recurrent sub-acute intestinal obstruction by small gut stricture which was confirmed on the barium study at that time. During and after each episode the patient was managed conservatively without any surgical intervention. General physical examination during current episode showed dehydrated appearence, pulse 96/min, blood pressure 110/70 mmHg, and temperature of 99oC. Systemic examination was normal. Abdominal examination revealed distended abdomen, diffuse tenderness and a high pitch bowel sounds. Laboratory parameters were normal. X-ray of abdomen showed multiple air fluid levels. Computed tomography scan of the abdomen revealed conglomeration of gut in a thin sac suggestive of peritoneal encapsulation on the right side. There was displacement of inferior mesenteric vein and the entrapped bowel in left upper abdomen (left paraduodenal hernia). (Figure 1A–B) Gut loops were dilated and had thick walls. Exploratory laparotomy revealed encasement of bowel loops in membrane, typical of peritoneal encapsulation with inter-loop adhesions present in the bowel outside the peritoneal sac. (Figure 2) Gut inside peritoneal encapsulation was dilated, which was suggestive of obstruction. Malrotations of small gut loops was seen. After careful dissection of the membrane, adhesiolysis and release of omental adhesions, a vessel lying on ileal loops, outside the retroperitoneum, was seen which was identified as inferior mesenteric vein (IMV). (Figure 3A-B) The bowel proximal to the abnormally placed IMV was dilated with thickened wall which was suggestive of obstruction. This abnormally lying IMV was constrained by adhesions to small bowel. Peritoneal encapsulation and retroperitonealization of IMV were leading to sub-acute intestinal obstruction. Further exploration revealed a loop of intestine impacted in a left paraduodenal fossa. Diagnosis of the left paraduodenal hernia was confirmed. (Figure 4A- B) Incarcerated segment of bowel in left paraduodenal fossa had signs of strangulation with thickened walls leading to acute abdomen. Resection of incarcerated segment and the closure of hernial orifice was done. Retroperitonealization of anteriorly placed IMV was achieved. Postoperative period was uneventful and patient was discharged after one week. Patient is well on follow up for last 13 months. | ||||||
|
| ||||||
| ||||||
| ||||||
| ||||||
|
Discussion
| ||||||
|
Peritoneal encapsulation is a developmental abnormality encasing part or the entire small bowel in an accessory sac derived from the yolk sac. [16] The accessory peritoneal membrane is derived from the peritoneum of the yolk sac which withdraws into the abdominal cavity with the small bowel instead of remaining at the base of the umbilical cord. This is attached to the ascending and descending colon laterally, the transverse mesocolon superiorly and merges with posterior parietal peritoneum inferiorly. The membrane has two openings, one around the duodenojejunal flexure and the other at the ileocecal junction. [7] Peritoneal encapsulation seems to be predominant in males and is not always associated with abnormal intestinal rotation. [17] [18] The condition is largely asymptomatic but some cases may present as bowel obstruction. [19] [20] Peritoneal encapsulation very rarely leads to an acute iliac occlusion or to idiopathic sclerosing peritonitis. [21] [22] This congenital encapsulation can be diagnosed incidentally during laparotomy for other conditions and some cases are diagnosed at autopsy. [3] [8] It can occur with incomplete situs inversus and abnormal artery (both are congenital anomalies) or as an incidental findings at time of gastric surgery or during colon cancer surgery. [4] [23] Paraduodenal hernia is a rare condition in which the small bowel loops are trapped within a congenital paraduodenal fossa. [24] Males are three times more affected than females. [25] Paraduodenal hernia are divided into two subtypes: left or right paraduodenal hernia. About 75% are located on the left side. [9] A case of congenital pyloric stenosis associated with the presence of a paraduodenal hernia in an adult patient has been reported. [26] Paraduodenal hernia lacks a true hernial sac and is termed 'prolapse' or 'procidentia' rather than a hernia. [27] The left paraduodenal hernia is a result of anomalous rotation of midgut into the developing mesentery of the descending colon with mechanical forces of fluctuating intra-abdominal pressure leading to herniation in places where the peritoneum is yet incompletely fused. [27] [28] They originate at the fossa of Landzert which is just lateral to the fourth segment of the duodenum and behind the inferior mesenteric vein and ascending left colic artery. [29]The sac lies to left of the duodenum. Inferior mesenteric vessels constitute the anterior free margin of the sac. [30] Accurate anatomy is important surgically, as the inferior border of the hernia opening is safest place to widen the neck of the hernia. [27] Symptoms of paraduodenal hernia are non-specific, ranging from recurrent vague abdominal pain, nausea, vomiting and reversible obstruction leading to an acute abdomen. [31] About 50% cases follow an asymptomatic clinical course and are diagnosed incidentally; rest 50% patients with paraduodenal hernia have episodes of intestinal obstruction at some point of their lives. [32] The symptoms depend on patient's position, with symptoms aggravating while standing and relieved in a supine position. [33] Spontaneous reduction apparently causes the periodic presentation of abdominal pain with normal radiographic studies. [34] The herniated small bowel loops may become trapped within this mesenteric sac. Symptoms may also result from retroperitoneal mass effect. Adhesions are the cause of about 30–41% of all intestinal obstructions and for the small bowel obstruction, the proportion rises to 65–75%. [35] Only 3% of these are thought to be caused by congenital omental bands formed by abnormal adhesions of the peritoneal folds during embryogenesis. [10] [36] In our case, congenital adhesions might have led to constraining effect on IMV leading to its retroperitonealization which compressed the small bowel leading to obstruction. A congenital constraining of adhesions between the vein and the gut can also lead to bowel obstruction. In view of the diagnostic difficulty based on clinical findings, imaging studies often play an important role in the diagnosis. Radiographic studies are usually normal or show non-specific features of intestinal obstruction. Plain abdominal X-rays are suggestive of mechanical bowel obstruction which was present in our case. A paraduodenal hernia may be demonstrated by an upper gastrointestinal series performed during a period of acute symptoms. Barium contrast study demonstrates sac-like mass of mildly dilated jejunal loops, left of the ligament of Treitz with mass effect causing displacement of the greater curvature and posterior wall of the stomach. [37] Ultrasonography in internal hernia shows hetergenous echoic abdominal mass with presence of changing cystic or tubular internal components and a surrounding the membrane. [38] On computed tomography (CT) scan, the findings are very non-specific. Small bowel is seen enveloped in a thin membrane and may be suggestive of peritoneal encapsulation. [20] [23] [39] The following findings are seen on CT scan in left paraduodenal hernia: [27] [40] [41]
Congenital adhesions involve surgical release of adhesions and bands. Treatment of peritoneal encapsulation involves the total removal of the anomalous membrane and release of both openings. Bowel resection may be necessary if the membrane cannot be stripped atraumatically or if obvious gangrene of the bowel is present. There is no re-operation reported in literature after dividing the encasing membrane in peritoneal encapsulation. [4] Surgical treatment of left paraduodenal hernia follows the basic principles of hernia surgery: reduction of the contents, restoration of normal anatomy and repair of the defect. [33] [42] A retroperitonealization of inferior mesenteric vein involves retroperitonealization of vein after release of congenital adhesions. | ||||||
|
Conclusion
| ||||||
|
Occurrence of paraduodenal hernia, peritoneal encapsulation and congenital adhesions leading retroperitonealization of inferior mesenteric vein in the same patient is rare. Left paraduodenal hernia rarely presents as an acute abdomen. Occurring of three abnormal anatomical structures must have had a congenital origin as the patient had no predisposing factors for the development of these congenital anamolies. | ||||||
|
References
| ||||||
| ||||||
|
[HTML Abstract]
[PDF Full Text]
|
|
Author Contributions
Imtiaz Wani – Substantial contributions to conception and design, Acquisition of data, Analysis and interpretation of data, Drafting the article, Revising it critically for important intellectual content, Final approval of the version to be published Khursheed A Wani – Substantial contributions to conception and design, Acquisition of data, Analysis and interpretation of data, Drafting the article, Revising it critically for important intellectual content, Final approval of the version to be published Muneer Wani – Substantial contributions to conception and design, Acquisition of data, Analysis and interpretation of data, Drafting the article, Revising it critically for important intellectual content, Final approval of the version to be published Gulzar Bhat – Substantial contributions to conception and design, Acquisition of data, Analysis and interpretation of data, Drafting the article, Revising it critically for important intellectual content, Final approval of the version to be published Mubashir Shah – Substantial contributions to conception and design, Acquisition of data, Analysis and interpretation of data, Drafting the article, Revising it critically for important intellectual content, Final approval of the version to be published |
|
Guarantor of submission
The corresponding author is the guarantor of submission. |
|
Source of support
None |
|
Conflict of interest
Authors declare no conflict of interest. |
|
Copyright
© Imtiaz Wani et al. 2013; This article is distributed the terms of Creative Commons Attribution License which permits unrestricted use, distribution and reproduction in any means provided the original authors and original publisher are properly credited. (Please see Copyright Policy for more information.) |
|
|