|

|
 |
|
Case Report
| ||||||
| Rural medicine in a developing economy: Does the presence of orthodox practice guarantee safe patient care? | ||||||
| Ikpeme A Ikpeme1, Anthonia A Ikpeme2, Emmanuel Efa3, Elijah Udoh1 | ||||||
|
1Department of Surgery, University of Calabar Teaching Hospital, P.M.B 1278, Calabar, Nigeria.
2Department of Radiology, University of Calabar Teaching Hospital, P.M.B 1278, Calabar, Nigeria. 3Department of Medicine, University of Calabar Teaching Hospital, P.M.B 1278, Calabar, Nigeria. | ||||||
| ||||||
|
[HTML Abstract]
[PDF Full Text]
[Print This Article]
[Similar article in Pumed] [Similar article in Google Scholar] 
|
| How to cite this article: |
| Ikpeme IA, Ikpeme AA, Efa E, Udoh E. Rural medicine in a developing economy: Does the presence of orthodox practice guarantee safe patient care? International Journal of Case Reports and Images 2012;3(12):53–57. |
|
Abstract
|
|
Introduction:
Medical practice in the developing world presents challenges which are more marked in the rural communities. A low doctor-patient ratio combined with a firm belief in traditional and unorthodox practices challenges the role of orthodox medicine in these communities. Despite the documented complications of unorthodox practices, injudicious orthodox care plays a significant role in the development of preventable complications and potential poor outcomes in the healthcare of rural dwellers in resource challenged societies. This article presents a case of severe preventable complications following injudicious orthodox care in a rural African region.
Case Report: An 80-year-old rural dweller presented with a three-week history of lower urinary obstructive symptoms complicated by sepsis, hydronephrosis and renal parenchymal damage. He had spent three weeks in an orthodox medical practice in a rural community. Urinary catheterization produced 1700 mL of frank pus. He was managed by warm lavage, broad spectrum antibiotics and a referral to urological care. He made a full recovery from the complications and was offered elective prostatectomy. Conclusion: This case report highlights the potential for preventable complications in orthodox medical care in the rural areas of the developing world. Whereas orthodox practitioners are quick to highlight the complications that attend unorthodox medical practices, there is a need for appropriate audit and continuing medical education of orthodox rural practitioners. | |
|
Keywords:
Rural medicine, Developing economy, Safe patient care
| |
|
Introduction
| ||||||
|
Medical practice in many developing countries presents unique challenges. These challenges are even more marked in the rural communities of the developing countries. With a doctor-patient ratio below the standard by World Health Organization (WHO), recommend, the role of customs, taboos and age long belief systems coupled with attendant poverty ensures that orthodox medicine faces a stiff challenge from unorthodox and traditional practices in these communities. [1] While the WHO works towards institutionalizing traditional medicine in the health systems of the African region, many reports have documented the complications that follow unorthodox and traditional practices in many of the world's poor regions. [2] [3] [4] [5] Orthodox medicine has evolved based on scientific advances. One of the challenges we face today is the availability of high quality medical and health care to everyone at reasonable cost and with easy access. [6] A worldwide shortage of rural family physicians has been identified as contributing to difficulties in providing appropriate medical care in the rural areas of both developed and developing countries. [7] [8] In the rural areas of West Africa, the picture of medical practice has not changed much over the last 30 years. [9] Medical colleges producing an increasing number of orthodox physicians and with some of them setting-up practices in the rural areas it should be expected that the standard of care available to rural dwellers would improve. Our report shows that this may not be the case. Trained in rigorous and structured training programs, orthodox physicians should bring the advantages of their training to bear on the healthcare status of the communities they work in. This must include safe practices, a recognition of the finiteness of their skills and early referral. [9] Access to safe healthcare presents an acute problem in the rural communities of many African countries. Despite huge investments in healthcare, there still exists significant urban-rural inequalities in healthcare in these communities. The index case demonstrates that among the indices that influence the healthcare of rural dwellers in Nigeria, the skills and knowledge base of orthodox practitioners are major contributors to outcomes. There needs to be a conscientious effort on the part of medical schools to develop curriculum to address rural practices and for regulators to encourage and enforce continuing medical education in these communities. This index case shows that beyond the often over flogged arguments for illiteracy, poverty, late presentation and injudicious unorthodox interventions as the underlying factors for poor health outcomes in the rural African communities, orthodox physicians need to examine their roles and the audit of their practices and interventions as a significant underlying factor in fostering poor outcomes. This report presents a case of severe preventable complications following injudicious orthodox care in a rural African region, and draw attention to the need for orthodox practitioners to focus on their practices as an important determinant of potential poor clinical outcomes in the developing countries. | ||||||
|
Case Report
| ||||||
|
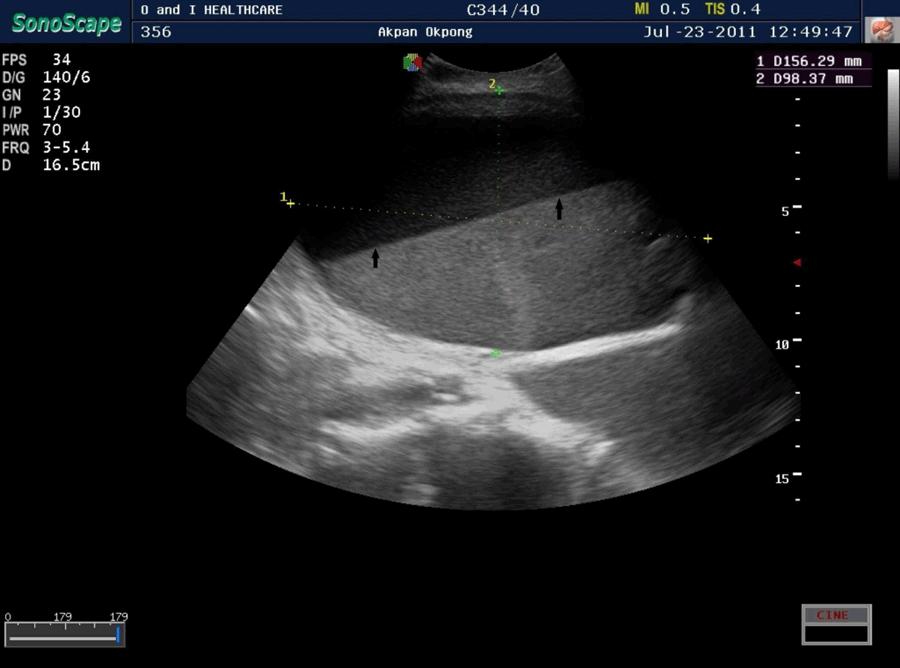
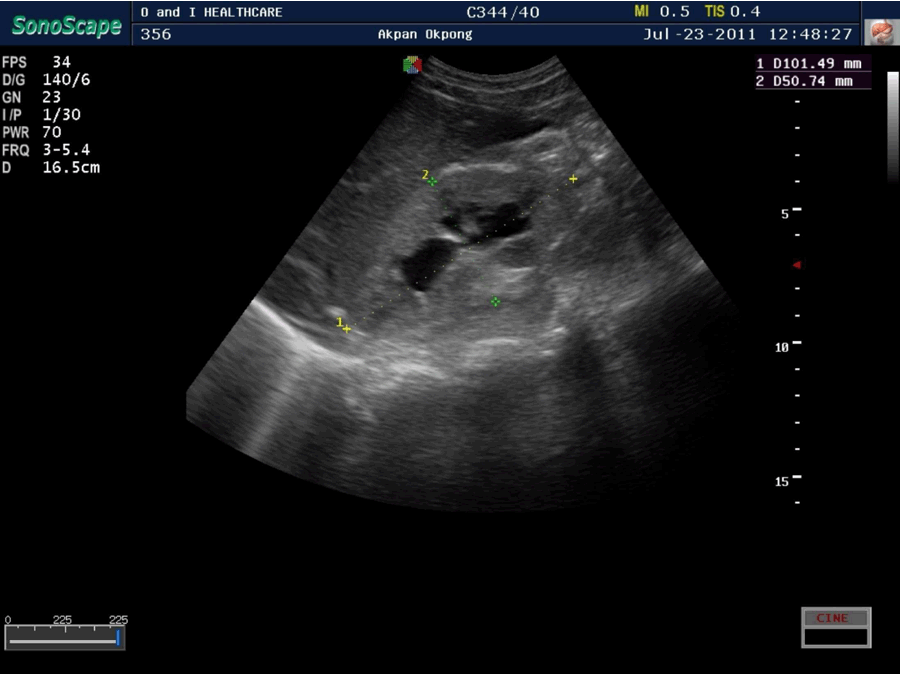
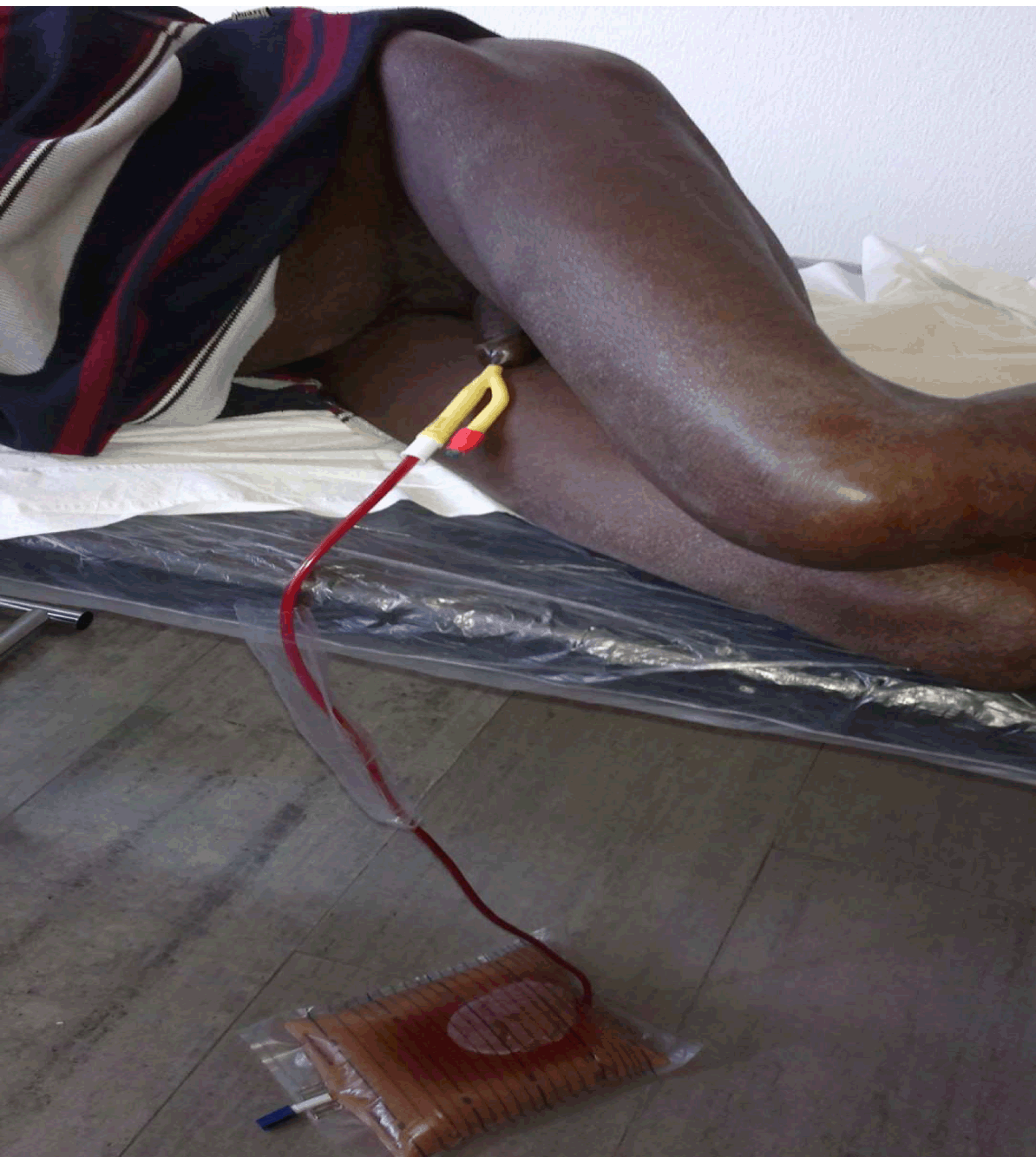
AO, An 80-year-old rural dweller was presented to our practice with a three-week history of complete inability to pass urine, lower abdominal swelling and a general feeling of ill-health. Past medical history revealed features of lower urinary tract obstruction with straining, poor stream (not improved by straining) and a feeling of incomplete voiding lasting for about two years. There was no history of hematuria. The patient had presented in a rural private practice where he had spent the preceding three weeks. After one failed attempt at catheterization, he was managed by repeated supra-pubic bladder aspirations for three weeks. He received no antibiotics and was only referred when he became obtunded. Clinical examination showed a weak, elderly man, with low body temperature (35°C), a respiratory rate of 30/min and an obtunded sensorium. There was bilateral pitting pedal oedema, generalized lower abdominal tenderness and the bladder size was 24 weeks. Abdomino-pelvic and transrectal ultrasonographic examination showed uniformly enlarged prostate (prostatic volume 85 cc) with no calcifications or suspicious foci, an enlarged bladder containing an estimated 1000 mL of fluid with fluid-fluid level, bilateral hydronephrosis and grade 3 renal parenchymal disease (Figures 1 and 2). An impression of mismanaged bladder outlet obstruction with sepsis and reno-pelvic complications was made. The patient was managed by urethral catheterization which yielded 1700 mL of frank pus (subsequently becoming blood stained) (Figure 3), warm bladder lavage with 2000 mL normal saline, continuous bladder drainage with an in-dwelling catheter and intravenous broad spectrum antibiotics. A sepsis work up and serum electrolytes, urea and creatinine were requested and the patient was referred to the urologists. He subsequently made a full recovery from the immediate complications and was scheduled for elective prostatectomy. | ||||||
| ||||||
| ||||||
| ||||||
| ||||||
|
Discussion
| ||||||
|
Access to healthcare is a major problem in rural communities. [10] The World Bank group argues that despite major investments in health in Africa, populations in the poorer rural communities in Sub- Saharan Africa lose out in health service coverage. [11] One of the identified denominators of this position is the shortage of appropriate healthworkers in the rural communities leading to urban-rural inequalities of healthcare. [11] [12] Access to an orthodox healthcare practitioner may not be the only challenge that rural dwellers face. The quality of healthcare available to rural dwellers is a function of many indices including the skills and knowledge base of the practitioners. The index case aptly demonstrates these issues. Whereas there are arguments for medical schools to help in the recruitment, training and retention of rural practitioners, [13] [14] [15] [16] emphasis has to be laid on the quality of training available in medical colleges in the developing world. Graduating clinicians must be taught repeatedly that prompt and appropriate referral is a critical component of safe healthcare practices. Like most other developing countries, the major proportion of Nigerians live in the rural areas. Patients also have a strong positive perception of traditional health practices but will accept orthodox care. [17] [18] While orthodox practitioners have documented the complications that follow traditional medical practices, [1] [3] [17] orthodox medicine can only win the hearts of the majority of rural dwellers if consistent and proven safe outcomes are achieved. Medical schools, therefore, need to target the development of rural practices in their curricular. [12] [13] [14] [19] There is available evidence that medical schools can maintain competitive admission criteria while attracting and graduating students who will likely enter rural practice. [19] Continuing medical education aims to foster lifelong learning in a physician. This ultimately translates to the maintenance and increase in knowledge, skillbase and professional competence of physicians. This is well established in the developed world and only becoming implemented in Nigeria. Besides targeting the development of rural practice curricular, continuing medical education when enforced will help in the reduction of avoidable complications in orthodox care and argurably improve the quality of healthcare available to rural dwellers in the developing world. | ||||||
|
Conclusion
| ||||||
|
Our report highlights the potential for preventable complications in orthodox medical care in the rural areas of the developing world. While orthodox practitioners highlight the complications that follow traditional medical and other unorthodox interventions, there is the need to encourage continuing medical education, early and appropriate referral and regular audit of orthodox medical practices in the developing countries. The inequalities in urban-rural healthcare should be addressed in ways that ensure consistently safe outcomes for rural dwellers. | ||||||
|
References
| ||||||
| ||||||
|
[HTML Abstract]
[PDF Full Text]
|
|
Author Contributions
Ikpeme A Ikpeme – Substantial contributions to conception and design, Acquisition of data, Drafting the article, revising it critically for important intellectual content, Final approval of the version to be published Anthonia A Ikpeme – Substantial contributions to conception and design, analysis and interpretation of data, Drafting the article, Final approval of the version to be published Emmanuel Efa – Substantial contributions to conception and design, Drafting the article, revising it critically for important intellectual content, Final approval of the version to be published Elijah Udoh – Substantial contributions to conception and design, Drafting the article, revising it critically for important intellectual content, Final approval of the version to be published |
|
Guarantor of submission
The corresponding author is the guarantor of submission. |
|
Source of support
None |
|
Conflict of interest
Authors declare no conflict of interest. |
|
Copyright
© Ikpeme A Ikpeme et al. 2012; This article is distributed the terms of Creative Commons Attribution License which permits unrestricted use, distribution and reproduction in any means provided the original authors and original publisher are properly credited. (Please see Copyright Policy for more information.) |
|
|