| Table of Contents |  |
|
Clinical Image
|
| Recurrent evisceration from Mcburney's incision |
| Vinay S Gundlapalli1, Orville Domingo2 |
|
1Surgery Resident (PGY3), Mercy Fitzgerald Hospital, Darby, PA, USA.
2Attending Surgeon, Department of General Surgery, Mercy Fitzgerald Hospital, Darby, PA, USA. |
|
doi:10.5348/ijcri-2012-06-140-CR-13
|
|
Address correspondence to: Dr Vinay S Gundlapalli Department of Surgery 1500, Lansdowne Ave, Darby PA, 19023 USA Fax: 6105346209 Email: vinaygsagar@gmail.com |
|
[HTML Abstract]
[PDF Full Text]
|
| How to cite this article: |
| Gundlapalli VS. Recurrent evisceration from Mcburney's incision. International Journal of Case Reports and Images 2012;3(6):54–56. |
|
Case Report
| ||||||
|
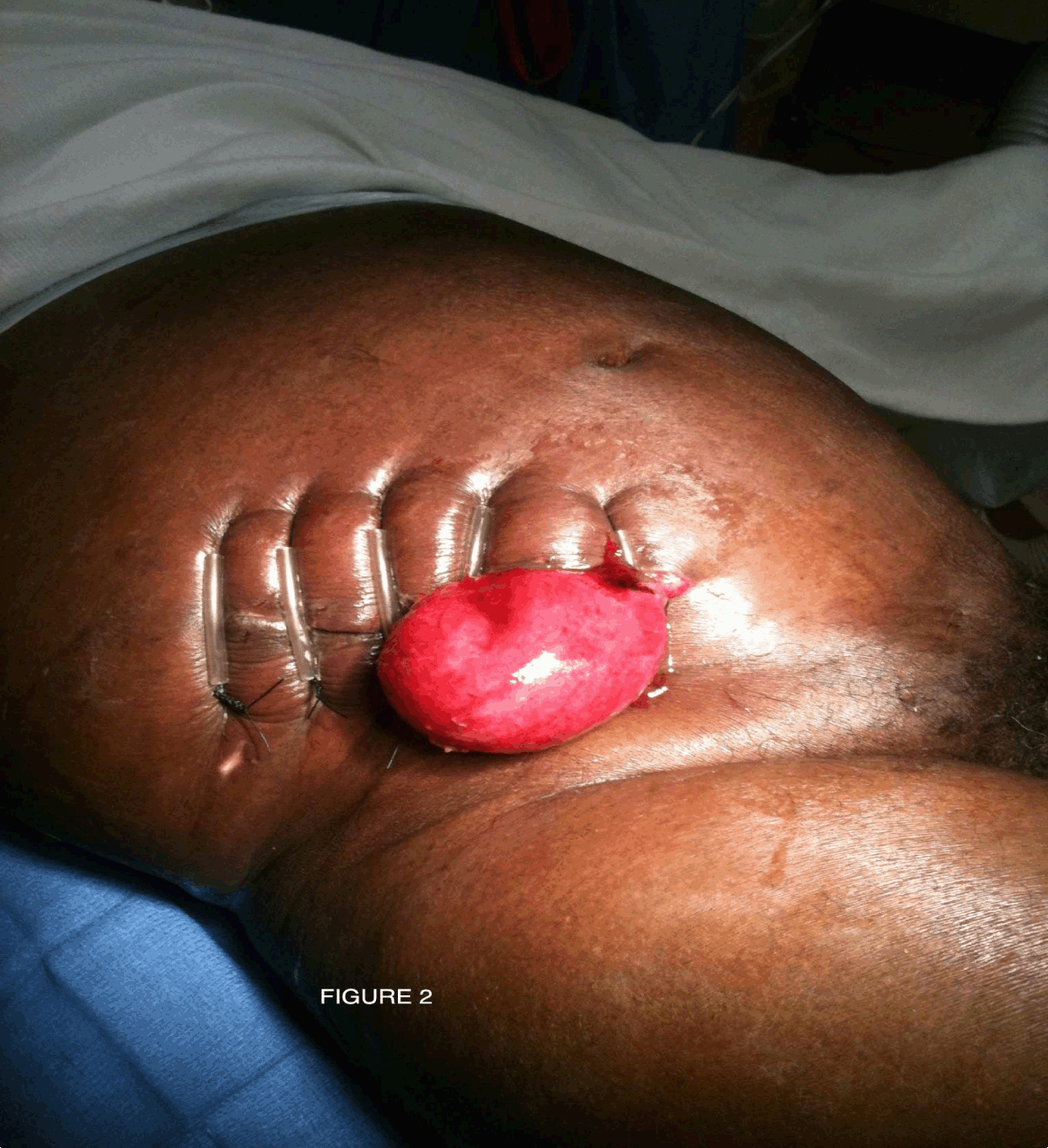
A 71-year-old, male presented to emergency room with 24 hr history of right lower quadrant (RLQ) pain, anorexia and low-grade fever. His past medical history included hypertension, asthma, COPD and cerebral palsy. Patient was disabled with severe flexion deformity at the hip joint. On physical examination he was tachycardic, hypotensive and had RLQ tenderness without peritonitis. Blood tests showed white cell count of 7.6x103 cells/mm3 and hemoglobin of 10.4 g/dl. Computed tomography (CT) scan (Figure 1) showed dilated fluid filled appendix (1.1 cm), with fat stranding confirming acute appendicitis (Figure 1). He was resuscitated, given antibiotics and an emergent open appendectomy performed. Post operatively patient was on the surgical floor but was transferred to the ICU for acute exacerbation of COPD and was started on short course steroids in addition to nebulizers. He recovered over the next few days and transferred to the surgical floor. While awaiting placement to a skilled nursing facility on post op day seven he eviscerated bowel through the Mcburney's incision while having a bowel movement (Figure 2). He was taken to the operating room emergently, bowel was reduced and incision primarily repaired with retention sutures. Patient remained in the hospital and he eviscerated again on the post op day eleven (Figure 3). This time after the bowel was reduced the defect was repaired with a biological mesh and wound approximated with closely placed retention sutures (Figure 4). The patient remained intubated for a week after which tracheostomy was performed due to inability to wean off ventilator. The patient was in the ICU for four days then transferred to a long-term acute care center where he improved over the next four weeks. On follow up his incision healed well. | ||||||
| ||||||
|
| ||||||
| ||||||
|
| ||||||
| ||||||
|
| ||||||
| ||||||
|
Discussion
| ||||||
|
Evisceration or Burst abdomen via laparotomy incisions is rare. [1] The incidence of evisceration after open appendectomy through a Mcburney's incision is not clearly known and the recurrence of such evisceration has never been documented in the recent literature. There are multiple layers of fascia and muscles with good blood supply which lead to good healing thus preventing eviseration. The major independent risk factors for evisceration through midline incision are old age, male gender, chronic pulmonary disease, ascites, jaundice, anemia, emergency surgery, type of surgery, postoperative coughing, sepsis, corticosteroid use and wound infection. [2] Our patient had six of the above risk factors (elderly male patient with COPD receiving steroids, who underwent an emergent operation and also had severe cough postoperatively), which predisposed him to have evisceration. It has to be noted that the risk factors mentioned were for evisceration through a midline incision but they should hold good for the Mcburney's incision as well. Other than the patient factors the surgeon can prevent or reduce incidence of evisceration by following good surgical principles. Well-done, large, prospective studies with the best follow-up found that a Suture Length (SL)-to-Wound Length (WL) ratio of approximately 4:1 minimized the incidence of fascial dehiscence and incisional hernia formation. [3] [4] The pathognomonic sign of evisceration or burst abdomen is the discharge of serosanguinous (salmon colored) fluid from the wound. [5] The diagnosis of evisceration is clinical with the identification of intra-abdominal contents through the incision. The preferred treatment of evisceration is an emergent reclosure. [5] Our patient had an emergent repair with reduction of bowel and primary closure with retention sutures on the first re-operation. On second re-operation he underwent primary closure reinforced with biological mesh and closely placed retention sutures. The mortality and morbidity of evisceration is high. [5] | ||||||
|
Conclusion
| ||||||
|
Evisceration is occasionally seen in midline laparotomy incisions in high-risk patients but exceedingly rare in Mcburney's incision. | ||||||
|
References
| ||||||
| ||||||
|
[HTML Abstract]
[PDF Full Text]
|
|
Author Contributions:
Vinay S Gundlapalli - Substantial contribution to the conception and design, acquisition of data, analysis and interpretation of data, drafting the article, revising it and final approval of the version to be published Orville Domingo - Substantial contribution to the conception and design, acquisition of data, analysis and interpretation of data, drafting the article, revising it and final approval of the version to be published |
|
Guarantor of submission:
The corresponding author is the guarantor of Submission. |
|
Source of support:
None |
|
Conflict of interest:
The authors declare no conflict of interest. |
|
Copyright:
© Vinay S Gundlapalli et al. 2012; This article is distributed the terms of Creative Commons Attribution License which permits unrestricted use, distribution and reproduction in any means provided the original authors and original publisher are properly credited. (Please see Copyright Policy for more information.) |
|
|